* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PowerPoint 簡報
Rheumatic fever wikipedia , lookup
Atherosclerosis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Complement system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Inflammation wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
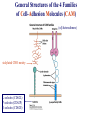
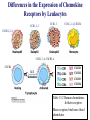
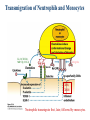
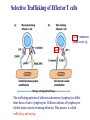
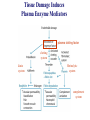
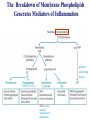
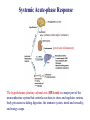
Chapter 15 Leukocyte Activation and Migration Lymphocytes bind to the surface of a high endothelial venule (HEV) Dec 26, 2006 When an infection is detected, the cells of the immune system cross the blood barrier and travel to the site of infection. How do leukocytes migrate to the tissue? 本章內容: 1. 參與白血球移動的分子及過程 2. 參與發炎反應的分子及生理變化 - For circulating leukocytes to enter inflamed tissue or peripheral lymphoid organs, the cells must adhere to and pass between the endothelial cells lining the walls of blood vessels, a process called extravasation. - Endothelial cells express leukocyte-specific celladhesion molecules (CAM) - CAMs on leukocytes serve to adhere to vascular endothelial cells and to increase the strength of the interactions between cells of the immune system, e.g., TH – APC, TH – B, CTL – target cells. General Structures of the 4 Families of Cell-Adhesion Molecules (CAM) (ab heterodimers) sialylated CHO moiety L-selectin (CD62L) P-selectin (CD62P) E-selectin (CD62E) Cell Adhesion Molecules (CAM) (on endothelium) (on endothelium) (on neutrophil) (on leukocyte) (on inflamed endothelium) (CD54, CD102, CD50) (CD106) (on mucosal endothelium, has both mucin-like and Ig-like domains) (lymphocyte Peyer's patch adhesion molecule-1) Chemokines 1. Small polypeptides, most of which contain 90 – 130 a. a. residues 2. Control the adhesion, chemotaxis, and activation of leukocytes – major regulators of leukocyte traffic. 3. Some are primarily involved in inflammatory processes, others are constitutively expressed and play important homeostatic or developmental roles. 4. Chemokine-mediated effects are not limited to the immune system. 5. The inflammatory chemokines are induced in response to infection and recruit phagocytes and lymphocytes to inflammatory sites. 6. Four classes: CXC, CC, C, CXXXC (or CX3C) 7. Ligands: e.g., CXCL8, Receptors: e.g., CXCR1 Chemokines Signal through Receptors Coupled with Large G Proteins (polypeptide chains traverse the membrane 7 times) Effects of Chemokines 1. Cell movement 2. Changes in cell shape 3. Promotion of adhesiveness to endothelial wall 4. Generation of microbicidal ·O - (superoxide anion) 2 in phagocytes 5. Release of proteases from neutrophils & macrophages 6. Release of histamine from basophils 7. Release of cytotoxic proteins from eosinophils Differences in the Expression of Chemokine Receptors by Leukocytes CCR1, 2, 3 CCR1, 3 CCR1, 2, 4, CXCR4 CXCR1, 2, 4 CCR2, 3, 4, CXCR3, 4 CXCR4 CXCR1 CXCR2 CXCR3 CXCR4 Table 13-2 Human chemokines & their receptors Most receptors bind more than 1 chemokine. Four Sequential But Overlapping Steps in Neutrophil Extravasation (by chemoattractant stimulus*) * * ** ** * * activated (inflamed) endothelium * Chemoattractant stimuli: chemokines platelet-activating factor (PAF) C5a, C3a, C5b67 N-formyl peptides (from microbes) * * Transmigration of Neutrophils and Monocytes IL-8 (CXCL8), MIP-1b (CCL4) integrins mucin CD31, CD321 Neutrophils transmigrate first, later, followed by monocytes. Lymphocyte Recirculation Routes Lymphocyte Extravasation Occurs in High-endothelial Venules (HEVs) - cuboidal (“high”) shape, - present in lymph nodes, Peyer’s patches, or tonsils, - express CAMs of the selectin, the mucin-like, and the Ig superfamilies. Extravasation of Naïve T lymphocytes The general process of lymphocyte extravasation is similar to neutrophil extravasation. Naïve T-cells circulate indiscriminately to secondary lymphoid tissue throughout the body. Selective Trafficking of Effector T cells CLA :cutaneous lymphocyte Ag The trafficking patterns of effector and memory lymphocytes differ from those of naïve lymphocytes. Different subsets of lymphocytes exhibit tissue-selective homing behavior. This process is called trafficking, or homing. Mediators of Inflammation 1. Chemokines – key mediators of inflammation 2. Plasma Enzyme Mediators a. kinin system b. clotting system c. fibrinolytic system d. complement system 3. Lipid Inflammatory Mediators 4. Cytokine Inflammatory mediators – IL-1, IL-6, TNF-, IL-12, IFN- Tissue Damage Induces Plasma Enzyme Mediators plasma clotting factor clotting system kinin system fibrinolytic system complement system The Breakdown of Membrane Phospholipids Generates Mediators of Inflammation platelet activating factor (PGE2, F2, D2…) SRS-A: slowreacting substances of anaphylaxis Inflammatory Response Acute inflammatory responses: 1. Local responses – swelling, redness, heat, pain, and loss of function 2. Systemic responses – due to combined effects of IL-1, IL-6, and TNF-a induction of fever, increased synthesis of hormones, e.g., ACTH and hydrocortisone, increased production of WBC, and production of acute-phase proteins in the liver Chronic Inflammation – accumulation and activation of macrophages, IFN-, TNF-a Systemic Acute-phase Response (adrenocorticotropic hormone) (potent anti-inflammatory) The hypothalamus-pituitary-adrenal axis (HPA axis) is a major part of the neuroendocrine system that controls reactions to stress and regulates various body processes including digestion, the immune system, mood and sexuality, and energy usage. Anti-inflammatory Effects of Corticosteroids 1. Decrease in the number of circulating lymphocytes 2. Alterations in lymphocyte circulation patterns 3. Induction of NF-kB inhibitor, IkB 4. Reduction in the phagocytic and the killing ability of macrophages and neutrophils 5. Reduction in chemotaxis 6. Decrease in the expression of class II MHC molecules and IL-1 production by macrophages 7. Reduction in TH-cell activation 8. Decrease in the released lysosomal enzymes at the site of inflammation IFN- and TNF-a Play a Central Role in the Development of Chronic Inflammation ↑ cytokine production ↑ Ag presentation ↑ hydrolytic enzymes ↑ ROS, RNS → tissue damage Activated macrophages → TNF-a IFN- & TNF-a act synergistically to induce ICAM-1, E-selectin, class I MHC molecules, and recruit large numbers of cells.