* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Adaptive immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Innate immune system wikipedia , lookup
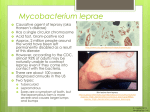
Cellular and Molecular Immunology: Peripheral B and T cell differentiation Christoph Mueller; Institute of Pathology [email protected] • General principles: - functional subsets - plasticity vs. stability of phenotype • Molecular basis of lymphocyte differentiation: transcription factors • Soluble factors and cognate interactions involved in the differentiation of lymphoid cells • Experimental approaches to study B/T cell differentiation • Consequences of impaired T and B cell differentiation RAG-1, 2 • RAG1 and RAG2 (“Recombination Activation Genes”) are essential for the rearrangement of the Ig and TCR genes • Mice deficient for either RAG1 and/or RAG2 are deficient for both T and B cells (but may still have some NK cells) • to prevent the later generation of autoreactive T and B cells, the expression of these two genes needs to be tightly regulated Regulation of T cell receptor gene rearrangement Experimental approach for determining the regulation of RAG gene expression Experimental set-up Mouse, transgenic for TCRab, recognizing the LCMV peptide gp33 in the context of H-2 Db - In a C57BL/6 (H-2b) genetic background: positive selection of TCRab tg T cells, tg TCRab expressed on thymocytes) - In a BALB/c (H-2d) background (no positive selection of TCRab tg T cells; no tg TCRab expressed on thymocytes) Working hypothesis: recognition of a MHC/Ag complex via a positively selecting TCRab down-regulates RAG expression in the differentiating T cells, and thus, terminates TCRab rearrangements Cortex Medulla In situ hybridisation for the detection of RAG-1 mRNA Thymus, wild type mouse (C57Bl/6 mouse) Medulla Cortex Murine Thymus, TCRab tg mouse with a positively selecting MHC haplotype: transcription of RAG1 gene is suppressed Cortex Medulla Murine Thymus, TCRab tg mouse with a non - selecting MHC haplotype: transcription of RAG1 gene is still active in the cortex CD8 T cell differentiation Functional Heterogeneity of CD4 T Lymphocytes naive CD4 T Cell Th1 Th0 ThO: IL2, IL3, IL4, IL5, IL6, IL9, IL10, IFN Th1: IL2, IFN , TNFalymphotoxin Th2: IL4, IL5, IL6, IL9, IL10 Th2 Naïve CD4 IL 4 IL 12 IFN Th 2 Th 1 Grogan & Locksley Curr Opinion Immunol 14: 366-72; 2002 Leprosy • Chronic - progressive infectious disease, affecting the skin, peripheral nerves and occasionally the respiratory tract • Infectious agent: Mycobacterium leprae • Globally, approx. 10-20 million patients infected, endemic in tropical areas (e.g. Southeast Asia; India, South America, Subsaharan Africa) Leprosy: Prevalence Leprosy: different clinical forms of the disease Lepromatous Leprosy: • Multiple, nodular lesions of the skin, in particular, of the face (”lion face"). • Persistent bacteriemia, foamy cell-like lesions with numerous M. leprae present Tuberculoid Leprosy: • Singular, small macular lesions of the skin. • Peripheral nerves (e.g. N. ulnaris, peronealis, N. auricularis) are often affected sensory neuropathy. • Granuloma are frequent (with only low numbers of M. leprae present) Immunological Spectrum of Leprosy naïve CD4 T cells Th1 Th0 Th2 cellular immunity humoral immunity Tuberculoid leprosy Lepromatous leprosy Granuloma formation Persistence of M. leprae Tissue damage may ensue Disfiguring disorder Lepromatous leprosy Tuberkuloid leprosy Type IV Hypersensitivity reactions Fig. 5-11 Kumar 6th edition Pathogens may influence the resulting adaptive immune response Science 302: 993-4; 2003 Figure 1 Stimulating the Th1 or Th2 response. In both pathways, dendritic cells internalize the pathogen. They present its antigens to T cells, which recognize antigens through their T-cell receptors (TCR). a, Organisms such as intracellular bacteria or viruses are recognized by the Toll-like receptors on dendritic cells; the resulting signals induce the secretion of interleukin-12 (IL-12) and differentiation of CD4 T cells into the Th1 lineage that produces gamma interferon (IFN-). b, How dendritic cells recognize larger pathogens, such as parasitic worms, is not known. But the end result is differentiation of Th2 effector cells regulated by T-cell-produced interleukin-4 (IL-4). Information1, 2 on the link between dendritic cells and T cells suggests that the former express different Notch ligands — Delta or Jagged — under different conditions. Jagged is specifically induced by stimuli known to induce Th2 differentiation. Notch signals (Notch-IC) can induce transcription of IL-4 through direct binding of RBPJ to the IL-4 promoter1 Nature 430, 150 - 151 (08 July 2004) # Publications per Year (PubMed) Publications on Suppressor T cells and Regulatory T cells 300 Suppressor T cells 250 Regulatory T cells 200 150 100 50 0 Rregulatory T cell subsets Natural regulatory T cells express the cell-surface marker CD25 and the transcriptional repressor FOXP3 (forkhead box P3). These cells mature and migrate from the thymus and constitute 5–10% of peripheral T cells in normal mice. Other populations of antigen-specific regulatory T cells can be induced from naive CD4+CD25- or CD8+CD25- T cells in the periphery under the influence of semimature dendritic cells, interleukin-10 (IL-10), transforming growth factor- (TGF-) and possibly interferon- (IFN-). The inducible populations of regulatory T cells include distinct subtypes of CD4+ T cell: T regulatory 1 (TR1) cells, which secrete high levels of IL-10, no IL-4 and no or low levels of IFN-; and T helper 3 (TH3) cells, which secrete high levels of TGF-. Although CD8+ T cells are normally associated with cytotoxic T-lymphocyte function and IFN- production, these cells or a subtype of these cells can secrete IL-10 and have been called CD8+ regulatory T cells. Mechanism(s) of suppression. Various molecular and cellular events have been described to explain how Treg can suppress immune responses. They include: IL-2 gene expression inhibition, modulation of costimulatory molecules on APCs and interaction of LAG3 with MHC class II molecules (a), immunosuppressive cytokine secretion (b), induction of tryptophan catabolism through CTLA-4 (c) and cytotoxicity (d). However, none of those mechanisms can explain all aspects of suppression. It is probable that various combinations of several mechanisms are operating, depending on the milieu and the type of immune responses. It is also possible that there might be a single key mechanism that has not been found yet (e). Abbreviations: APC, antigen presenting cell; TCR, T cell receptor. CD4 T cell differentiation (for beginners) CD4 T cell differentiation (for specialists) (Keiji Hirota, Bruno Martin and Marc Veldhoen, 2010): B cells …. CD4 T-Zelle CD40L 2.Signal: Quervernetzung der Ig durch Antigen oder Aktivierung durch CD40L T-Zell-Hilfe durch Zytokine CD40 1. Signal: Bindung des Antigen an Ig 2. Signal kein 2. Signal naive B - Zelle B-Gedächtniszelle a B-Zellen (CD19) b Mantelzone T-Zellen (CD3) c d „dark zone“ „light zone“ FDZ (CD21) e Mantelzone proliferierende Zellen (Ki-67) f Keimzentrum Mantelzone Plasmazellen k l Makrophagen (CD68) Keimzentrum Program of my next lectures: • Molecular mechanisms of immune tolerance • Central tolerance induction in the B cell and T cell compartment • Immune tolerance in the periphery • Immunopathology vs. Autoimmunity • Immune tolerance vs. Immune privilege vs. Immune ignorance