* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 18: Blood
Molecular mimicry wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Adaptive immune system wikipedia , lookup
Atherosclerosis wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
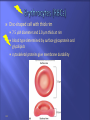
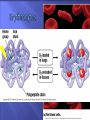
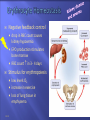
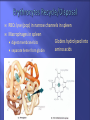
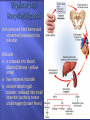
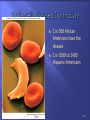
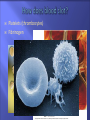
Transport Protection WBCs, antibodies, and platelets Regulation 18-2 O2, CO2, nutrients, wastes, hormones, and heat fluid regulation and buffering You have about 11 pints of blood (4 to 6 liters) The plasma portion (fluid portion) is mostly water Cells float in the plasma Red cells are also called erythrocytes White cells are also called leukocytes Platelets are pieces of cells also called thrombocytes Viscosity - resistance to flow whole blood 5 times as viscous as water Osmolarity total molarity of dissolved particles sodium ions, protein, and RBCs high osmolarity causes fluid absorption into blood, raises BP low osmolarity causes fluid to remain in tissues, may result in edema 18-4 18-5 Plasma – liquid portion of blood serum remains after plasma clots 3 major categories of plasma proteins albumins - most abundant contributes to viscosity and osmolarity globulins (antibodies) provide immune system functions alpha, beta and gamma globulins fibrinogen precursor of fibrin threads that help form blood clots Plasma proteins formed by liver 18-6 except globulins (produced by plasma cells) Nitrogenous compounds amino acids from dietary protein or tissue breakdown nitrogenous wastes (urea) toxic end products of catabolism normally removed by the kidneys Nutrients O2 and CO2 Electrolytes 18-7 glucose, vitamins, fats, minerals, etc Na+ makes up 90% of plasma cations BUN Creatinine Iron ferric (Fe3+) and ferrous (Fe2+) stomach acid converts Fe3+ to absorbable Fe2+ gastroferritin binds Fe2+ and transports it to intestine absorbed into blood and binds to transferrin for transport bone marrow for hemoglobin, muscle for myoglobin and all cells use for cytochromes in mitochondria Vitamin B12 and folic acid Vitamin C and copper 18-8 rapid cell division cofactors for enzymes synthesizing RBCs Disc-shaped cell with thick rim 18-9 7.5 M diameter and 2.0 m thick at rim blood type determined by surface glycoprotein and glycolipids cytoskeletal proteins give membrane durability 18-10 Gas transport - major function increased surface area/volume ratio due to loss of organelles during maturation increases diffusion rate of substances 33% of cytoplasm is hemoglobin (Hb) O2 delivery to tissue and CO2 transport to lungs Carbonic anhydrase (CAH) produces carbonic acid from CO2 and water important role in gas transport and pH balance 18-11 Are your red blood cells Carry oxygen from the lungs to your tissues Contain hemoglobin, a protein molecule that actually carries the O2 Anemia is a low amount of hemoglobin in the blood, sometimes caused by too few RBCs. Symptoms: Pallor Weakness Tiredness Unable to exercise without getting out of breath RBC count and hemoglobin concentration indicate amount of O2 blood can carry hematocrit (packed cell volume) - % of blood composed of cells men 42- 52% cells; women 37- 48% cells hemoglobin concentration of whole blood men 13-18g/dL; women 12-16g/dL RBC count men 4.6-6.2 million/L; women 4-2-5.4 million/L 18-14 Adult produces 400 billion platelets, 200 billion RBCs and 10 billion WBCs every day Hemopoietic tissues produce blood cells yolk sac produces stem cells liver stops producing blood cells at birth spleen remains involved with WBC production red bone marrow pluripotent stem cells hemopoiesis produces RBCs, WBCs and platelets 18-17 Negative feedback control drop in RBC count causes kidney hypoxemia EPO production stimulates bone marrow RBC count in 3 - 4 days Stimulus for erythropoiesis 18-18 low levels O2 increase in exercise loss of lung tissue in emphysema 2.5 million RBCs/sec Development takes 3-5 days First committed cell - erythrocyte colony forming unit has receptors for erythropoietin (EPO) from kidneys Erythroblasts multiply and synthesize hemoglobin Discard nucleus to form a reticulocyte 18-19 reduction in cell size, increase in cell number, synthesis of hemoglobin and loss of nucleus named for fine network of endoplasmic reticulum 0.5 to 1.5% of circulating RBCs RBCs lyse (pop) in narrow channels in spleen Macrophages in spleen Globins hydrolyzed into digest membrane bits amino acids separate heme from globin 18-20 Iron removed from heme and converted (stepwise) into bilirubin Bilirubin is released into blood plasma (kidneys - yellow urine) liver secretes into bile concentrated in gall bladder: released into small intestine; bacteria create urobilinogen (brown feces) 18-21 Polycythemia - an excess of RBCs primary polycythemia myeloproliferative disorder erythropoietic cell line in red bone marrow hematocrit as high as 80%!! secondary polycythemia from dehydration, emphysema, high altitude, or physical conditioning Dangers of polycythemia increased blood volume, pressure, viscosity can lead to embolism, stroke or heart failure 18-22 Inadequate erythropoiesis or hemoglobin synthesis inadequate vitamin B12 from poor nutrition or lack of intrinsic factor (pernicious anemia) Don’t make iron-deficiency anemia enough kidney failure and insufficient erythropoietin aplastic anemia - complete cessation Hemorrhagic anemias Hemolytic anemias 18-23 Lose cells faster than you can make them Tissue hypoxia and necrosis (short of breath and lethargic) Low blood osmolarity (tissue edema) Low blood viscosity (heart races and pressure drops) 18-24 Hereditary Hb ‘defect’ of African Americans recessive allele modifies hemoglobin structure sickle-cell trait - heterozygous for HbS individual has resistance to malaria HbS indigestible to malaria parasites sickle-cell disease - homozygous for HbS individual has shortened life 18-25 in low O2 concentrations HbS causes cell elongation and sickle shape cell stickiness causes agglutination and blocked vessels intense pain; kidney and heart failure; paralysis; stroke chronic hypoxemia reactivates hemopoietic tissue enlarging spleen and bones of cranium 1 in 500 African Americans have the disease 1 in 1000 to 1400 Hispanic-Americans 18-26 Platelets (thrombocytes) Fibrinogen Small fragments of megakaryocyte cytoplasm Functions 18-28 2-4 m diameter; contain “granules” amoeboid movement and phagocytosis secrete vasoconstrictors stick together to form temporaryplatelet plugs secrete clotting factors initiate formation of clot-dissolving enzyme phagocytize bacteria chemically attract neutrophils and monocytes to sites of inflammation All 3 steps involve platelets 18-29 pain receptors smooth muscle injury platelets release serotonin (vasoconstrictor) 18-30 broken vessel exposes collagen platelet pseudopods stick to damaged vessel and other platelets pseudopods contract and draw walls of vessel together forming a platelet plug 18-31 Platelets degranulate releasing substances that initiate fibrin clot Fibrinogen (in plasma) is converted into fibrin threads which form the clot 18-32 Most of the clotting factors are made in the liver Liver diseases compromise clotting Clot retraction occurs within 30 minutes Platelet-derived growth factor secreted by platelets and endothelial cells Fibrinolysis (dissolution of a clot) 18-34 repair damaged vessel plasmin, a fibrin-dissolving enzyme (clot buster) Genetic lack of any clotting factor affects coagulation Sex-linked recessive (on X chromosome) hemophilia A missing factor VIII (83% of cases) hemophilia B missing factor IX (15% of cases) note: hemophilia C missing factor XI (autosomal) Physical exertion causes bleeding and excruciating pain 18-35 transfusion of plasma or purified clotting factors factor VIII produced by transgenic bacteria Embolism - clot traveling in a vessel Thrombosis - abnormal clotting in unbroken vessel most likely to occur in leg veins of inactive people pulmonary embolism - clot may break free, travel from veins to lungs Infarction may occur if clot blocks blood supply to an organ (MI or stroke) 18-36 650,000 Americans die annually of thromboembolism 18-38 Conspicuous nucleus Travel in blood before migrating to connective tissue Protect against pathogens Granulocytes neutrophils (60-70%) fine granules in cytoplasm; 3 to 5 lobed nucleus eosinophils (2-4%) large rosy-orange granules; bilobed nucleus basophils (<1%) large, abundant, violet granules (obscure a large S-shaped nucleus) Agranulocytes lymphocytes (25-33%) variable amounts of bluish cytoplasm (scanty to abundant); ovoid/round, uniform dark violet nucleus monocytes (3-8%) largest WBC; ovoid, kidney-, or horseshoe- shaped nucleus 18-39 Neutrophils ( in bacterial infections) Eosinophils ( in parasitic infections or allergies) phagocytosis of antigen-antibody complexes, allergens and inflammatory chemicals release enzymes to destroy parasites Basophils ( in chicken pox, sinusitis, diabetes) 18-40 phagocytosis of bacteria release antimicrobial chemicals secrete histamine (vasodilator) secrete heparin (anticoagulant) Lymphocytes ( in diverse infections and immune responses) destroy cells (cancer, foreign, and virally infected cells) “present” antigens to activate other immune cells coordinate actions of other immune cells secrete antibodies and provide immune memory Monocytes ( in viral infections and inflammation) differentiate into macrophages phagocytize pathogens and debris “present” antigens to activate other immune cells 18-41 Hematocrit Hemoglobin concentration Total count for RBCs, reticulocytes, WBCs, and platelets Differential WBC count RBC size and hemoglobin concentration per RBC 18-42 Leukopoiesis pluripotent stem cells – most WBCs develop in the bone marrow T lymphocytes complete development in thymus Red bone marrow stores and releases granulocytes and monocytes Circulating WBCs do not stay in bloodstream granulocytes leave in 8 hours and live 5 days longer monocytes leave in 20 hours, transform into macrophages and live for several years WBCs provide long-term immunity (decades) 18-43 Fig. 18.18 18-44