* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The b-oxidation pathway as an energy source
Amino acid synthesis wikipedia , lookup
Adenosine triphosphate wikipedia , lookup
Photosynthetic reaction centre wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Microbial metabolism wikipedia , lookup
Light-dependent reactions wikipedia , lookup
Biosynthesis wikipedia , lookup
Mitochondrial replacement therapy wikipedia , lookup
Nicotinamide adenine dinucleotide wikipedia , lookup
Specialized pro-resolving mediators wikipedia , lookup
Butyric acid wikipedia , lookup
Mitochondrion wikipedia , lookup
Electron transport chain wikipedia , lookup
NADH:ubiquinone oxidoreductase (H+-translocating) wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Biochemistry wikipedia , lookup
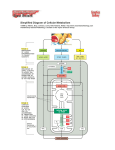
Oxidative phosphorylation wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
IV: Mitochondrial function (e.g. hepatocytes) 1) citric acid cycle as an energy source a) pyruvate or a-ketoglutarate dehydrogenase b) lipoic acid therapy 2) the respiratory chain as an energy source 3) oxidative phosphorylation and uncouplers 4) membrane transporters and shuttles a) cytosolic NADH oxidation b) acetyl CoA (NADPH export) c) transport systems in the mitochondria d) gluconeogenesis and glucose transport 5) mitochondrial diseases and treatment a) creatine therapy b) coenzyme Q10 therapy 6) b-oxidation of fatty acids as an energy source a) starvation/diabetes/endstage renal disease b) carnitine therapy c) ketogenic diet therapy d) drug induced fatty liver and NASH e) alcohol induced fatty liver and ASH 7) hepatic detoxification of a) monoamines b) alcohols c) toluene 8) hemoprotein mediated diseases a) rhabdomyolysis b) kernicterus 9) Heme biosynthesis & porphyria a) Heme biosynthesis b) Porphyria c) Oxidative degradation of heme to bilirubin 1 CITRIC ACID CYCLE AS AN ENERGY SOURCE An overview of the citric acid cycle Stryer 2 Acetyl CoA + 3 NAD+ + FAD + GDP + Pi + 2 H2O 2 CO2 + 3 NADH + FADH2 + GTP + 2H+ + CoA toxic! 120uM plasma citrate complexes Fe 3 The citric acid cycle is a source of biosynthetic precursors Glucose Pyruvate ATP, CO2 Phosphoenolpyruvate Acetyl CoA ADP, Pi Amino acids Oxaloacetate Succinyl CoA Porphyrins Citrate Stryer Fig. 20-17. Biosynthetic roles of the citric acid cycle. Intermediates drawn off for biosyntheses are replenished by the formation of oxaloacetate from pyruvate. (Anaplerotic) aketoglutarate Amino acids 4 Control of the citric acid cycle Stryer Fig. 20-22. Control of the citric acid cycle and the oxidative decarboxylation of pyruvate: * indicates steps that require an electron acceptor (NAD+ or FAD) that is regenerated by the respiratory chain. 5 2. THE RESPIRATORY CHAIN AS AN ENERGY SOURCE 6 The mitochondrial respiratory chain NADH Diagram of a mitochondrion FMNH2 complex I NADH-Q reductase 2Fe-2S 4Fe-4S Q FADH2 in flavoproteins succinate:Q reductase (complex II) complex III Cytochrome reductase Chemiosmotic theory of oxidative phosphorylation cyt c complex IV Cytochrome oxidase O2 Sequence of electron carriers in the respiratory chain 7 NADH coenzyme Q reductase: complex I M N N A D H F + N A D O O F M N H 2 H C OC 3 H C OC 3 C C H 3 C H 3 N C (C H C C C H )10 H 2 2 C H O Q H 2x O C e- Q e R + H C OC 3 H C OC 3 C O H eC C H 3 C R C O H + + A H OC 3C H OC 3C C C C H 3 C R C O H C o eR e 1 0S I n ( U B The reduction of ubiquinone to ubiquinol proceeds through a semiquinone anion intermediate. 1 8 Model of NADH-Q reductase Stryer Fig 21-9 9 Q:Cytochrome c reductase (Complex III) Q cyt b (+2) QH Fe-S(+2) cyt c1(+3) cyt c(Fe+2) QH cyt b (+3) QH2 Fe-S(+3) cyt c1(+2) cyt c(Fe+3) Stryer p. 537 cytochrome c reductase Stryer Fig. 21-11 Model of a portion of Q: cytochrome c reductase 10 Cytochrome oxidase (Complex IV) Lodish Fig. 17-30 11 Electron transport can be blocked by specific inhibitor poisons NADH NADH-Q Reductase QH2 Blocked by rotenone and amytal Cytochrome b Blocked by antimycin Cytochrome c1 Sites of action of some inhibitors of electron transport Cytochrome c Cytochrome Oxidase Blocked by CN- , N3 -, and CO O2 12 Cytochrome C - catalytic site RC C H 2 H V i o f + n C H 3 H SC H C 2 y o t R y l f h The heme in cytochromes c and c1 is covalently attached to 2 cysteine side chains by thioether linkages ' s e RC S C H t e iH 2 g Tr o h t h e h e R ' n e u i opp m The iron atom of the heme group in cytochrome c is bonded to a methionine 13 sulfur atom and a histidine nitrogen atom Cytochrome C - soluble NOT membrane bound 1. 26/104 amino acids residues have been invariant for > 1.5 x 109 years. 2. Met 80 and His 18 - coordinate Fe. 3. 11 residues from number 70 - 80 lining a hydrophobic crevice have remained virtually unchanged throughout all cytochrome c regardless of species or even kingdom. 4. A number of invariant arginine and lysine clusters can be found on the surface of the molecule. Cytochrome c has a dual function in the cell. Electron transport for ATP production AND the major cause of most programmed cell death (apoptosis) is initiated by the release of cytochrome c into the cytosol! 14 Origin of mitochondria: the endosymbiont hypothesis The endosymbiont hypothesis suggests that mitochondria have evolved from anaerobic bacteria which were phagocytosed by eukaryote cells at the time oxygen appeared on earth, Similarities between mitochondria and bacteria include the presence of: • cardiolipin •transporters • ribosomes • circular RNA and DNA Therefore mitochondria protein synthesis should be inhibited by: • TETRACYCLINE • CHLORAMPHENICOL. E.g. The extensive use of these drugs can inhibit 1. Bone marrow mitochondrial protein synthesis leading to a decline in the production of white or red cells. 2. Intestinal epithelial cells causing them to cease dividing. 15 3. OXIDATIVE PHOSPHORYLATION AND UNCOUPLERS 16 Oxidative phosphorylation 17 4.Mitochondrial MEMBRANE TRANSPORTERS A) Cytosolic NADH oxidation B) Acetyl CoA (NADPH export) C) Transport systems in the mitochondria D) Gluconeogenesis and glucose transport 18 Compartmentalization of the major pathways of metabolism 19 a) Cytosolic NADH oxidation: membrane transporters glycerol phosphate shuttle (Bucher shuttle) 20 b) Acetyl CoA/NADPH export to cytosol for fatty acid synthesis/ drug metabolism Gl uc o s e Cyt osol Py r uv a t e Ac e t y l CoA at hi gh c on c e n t r a t i o n Ci t r a t e Ci t r a t e Ac e t y l CoA Sy nt h as e Ci t r a t e +ATP +CoA f a t t y a c i d s yn t he or dr ug m e t a b ol i ( N- a c e t y l a t i on ) ATP c i t r at e l y as e Ox a l o a c e t a t e NADH Mi t ochondr i al Mat r i x ma l at e d e hy dr o ge n as e Ox a l o a c e t a t e NAD+ ADP M al a t e NADP+ ma l i c e n z y me CO2 Py r uv a t e Py r uv a t e ATP NADPH CO2 f a t t y a c i d s yn t he s i s or P4 50 c a t a l y z e d dr ug m e t a bol i s m Th e r e f or e m a l i c e nz ym e s u ppl i e s NADPH Ci t r a t e Lya s e s up pl i e s a c e t yl CoA. Pe nt o s e Pho s ph a t e Pa t hwa y NADPH 21 Isocitrate as an NADPH shuttle for drug metabolism Gl uc os e Py r u va t e Ac e t yl CoA CYTO SO L M I TO CH O NDRI AL M ATRI X Ci t r a t e Ox a l oa c e t a t e NADH M al at e Fu m a r a t e NAD+ CI TRI C ACI D CYCLE I s oc i t r a t e NAD+ NADH Su c c i n a t e i s oc i t r a t e de hy dr og e n as e NADP+ i s oc i t r a t e de hy dr og e n as e NADPH CO 2 a- k e t og l u t a r a t e NADH I s oc i t r a t e a- k e t og l u t a r a t e NAD+ P4 50 c at al yz e d DRUG M ETABO LI S M Su c c i n yl CoA CO2 22 d) Gluconeogenesis and glucose export by the liver ! 3 irreversible steps Major antidiabetic drug METFORMIN Inhibits gluconeogenesis Decr Hepatic Glucose Synth. 23 Glucagon 51aa & Insulin 29aa • Pancreas synthesises both peptide hormones • Glucagon hepatocyte receptors signals glycogenolysis (glycogen breakdown to glucose then increases gluconeogenesis pyruvate -- glucose) • Drugs. Dipeptidyl peptidase-4 inhibitor (Januvia, new anti type 2 diabetes) increases incretin , a GI hormonal peptide inhibitor of glucagon which lowers plasma glucose. • Metformin, antidiabetic drug inhibits gluconeogenesis but also can inhibit mitoch.complex I causing lactic acidosis. • Insulin required for cells (e.g.liver,muscle,fat) to take up glucose and synthesise glycogen. 24 5. MITOCHONDRIAL DISEASES (e.g. DEFECTIVE ELECTRON TRANSPORT) AND TREATMENT A) Creatine therapy B) Coenzyme Q10 therapy 25 Mitochondrial Myopathies • Genetic defects in mitochondrial structure & function leading to defective aerobic energy transduction and resulting in: exercise intolerance, lactic acidosis, stroke/seizure, headaches. 26 CREATINE THERAPY (an ergogenic aid effective against mitochondrial myopathies?) stored in muscles (makes ATP) • daily intake is 2g including1g (meat, fish, animal products) • 1g formed in liver, kidneys, pancreas from glycine,arginine,methionine • plasma levels incr. in kidney,heart,liver damage or rhabdomyolysis • 5-7g x 4 per day for 5-7 days increases muscle creatine stores by 18% (bigger increase in vegetarians); enhances performance in certain repetitive, high intensity, short-term exercise tasks in healthy individuals, offsets fatigue in mitochondrial myopathy patients and improves the mobility of the elderly. J. Amer. Coll. Nutr. 17, 216-234 (1998). 27 b) Ubiquinone (Coenzyme Q10) as a Food Supplement or Therapy • An essential electron and proton carrier in the mitochondrial respiratory chain. • Found in all intracellular membranes (acts as a mobile lipid soluble antioxidant that prevents membrane lipid peroxidation) • Better antioxidant if reduced to ubiquinol (UQH2) by NADH dehydrogenase of the respiratory chain. • Synthesised in mitochondria • Contributes to the fluidity of the phospholipid bilayer in membranes • Prevents plasma lipoprotein oxidation • Is a dietary supplement that protects liver from hepatotoxins (e.g. ethanol) and partly prevents mitochondrial myopathies (J. Neurol. Neurosurg. Psych. 50,1475-81) • Deficiency may occur in patients taking cholesterol lowering drugs (the statins) which act by inhibiting HMG-CoA reductase (e.g. lovastatin) Proc. Nat. Acad. Sci. 87, 8931 (1990) 28 6. b-OXIDATION OF FATTY ACIDS AS THE BEST ENERGY SOURCE a) Starvation/diabetes/endstage renal disease b) Carnitine therapy c) Ketogenic diet therapy d) Drug induced non alcoholic steatohepatitis , NASH e) Alcohol induced steatohepatitis , ASH 29 Stages in the extraction of energy from food stuffs. 30 b-Oxidation of fatty acids - transport of acyl carnitine into the mitochondrial matrix Stryer Fig 24-4 31 The b-oxidation pathway as an energy source O O R C C C C S CoA H2 H2 H2 Acyl CoA oxida tion R C C C C S CoA H2 H H trans- -Enoyl CoA FAD FADH2 H2O O H O R C C C C S CoA H2 H b-Ketoacyl CoA H + + NADH NAD+ oxida tion Hydration OHH O R C C C C S CoA H2 H H 3-L-hydroxyacyl CoA CoA-SH Thiolysis O + R C C S CoA H2 Acyl CoA shortened by 2 carbon atoms O H3C C S CoA Acetyl CoA Citric acid cycle 32 Fatty acid Metabolism • Fatty acids are linked to coenzyme A (CoA) before they are oxidised Ou t e r M i t o c h o n d r i a l e m b r O O R M + C ATP + HS-CoA a s ( a O c y a c R y l Co n t h e t k a f a i d t h C S CoA AMP + PPi + A a s e t t y i o k i n a s e ) • Carnitine carries long-chain activated fatty acids into the mitochondrial matrix Carnitine therapy for mitochondrial diseases A c y CH 3 O R C C l S Co A + H3C aC H ro nA i t i a N c t a r HS-CoA r a + n n H3C y H N i s e c CH 3 O C C C C H2 H2 O CH 3 OH n C C H2 CH 3 t O f C R O C C H2 i O O e 33 The b-oxidation pathway as an energy source O O R C C C C S CoA H2 H2 H2 Acyl CoA oxida tion R C C C C S CoA H2 H H trans- -Enoyl CoA FAD FADH2 H2O O H O R C C C C S CoA H2 H b-Ketoacyl CoA H + + NADH NAD+ oxida tion Hydration OHH O R C C C C S CoA H2 H H 3-L-hydroxyacyl CoA CoA-SH Thiolysis O + R C C S CoA H2 Acyl CoA shortened by 2 carbon atoms O H3C C S CoA Acetyl CoA Citric acid cycle 34 a) Starvation/Diabetes/Endstage renal disease Fat breaks down to acetyl CoA which form ketone bodies • Under low carbohydrate condition, oxaloacetate is converted to glucose (gluconeogenesis). CoA O C S CH2 2 Acet y l Co A C th i o la se O CH3 Acety l Co A + H2O CoA CoA O C HC HM G-Co A syn th a se HO CH NAD+ H+ + NADH Acety l Co A S CoA CH3 C HM G Co A lya se CH2 COO b-Hy d ro x y H+ b-meth y l g lu t ary l Co A su cci n at e OH CH2 COO CH2 Aceto acety l Co A ci tric aci d cy cle D-b-Hy d ro x y b u ty rat e CH3 O CO2 CH3 Co A t ran sferase C su cci n y l Co A O CH3 KETOGENESIS Aceto acetate Aceto acetate CH2 COO b-h y d ro x y b u ty rat e (M E T ABOL IS M o f k eto n e b o d i es) i. e. , act as fu el an d sp ares g l u co se Aceto n e 35 Diabetic ketoacidosis weakness, dehydration, thirst, drowsiness,coma • Usually precipitated by infection • lipolysis is the major energy source increases acetyl CoA levels which increases ketone body formation.Acetone excreted by the lungs/kidney. e.g. by starvation or diabetes mellitus (insulin-stimulated glucose entry into cells is impaired fatty acids are oxidised to maintain ATP levels. • if citric acid cycle is slowed by thiamine deficiency. • disease state plasma ketone levels: 10-25 mM (normal <0.5mM) and acetone breath smell( rotten apples or pear-drop smell) • LIFE THREATENING: ketogenesis faster than ketone body metabolism b-hydroxybutyric acid ↑↑> acetoacetic acid ↑& causes severe ACIDOSIS. Antidote – insulin , water, base therapy (bicarbonate), carnitine • urinary excretion of Na+, K+, Pi, H2O, H+ dehydration, blood volume 36 b) Carnitine Therapy Carnitine alleviates acetyl-CoA mediated inhibition of pyruvate dehydrogenase. • Both glycolysis and fatty acid metabolism produce acetyl CoA • Accumulation of acetyl CoA can inhibit pyruvate dehydrogenase, the enzyme responsible for producing acetyl CoA from pyruvate. • Pyruvate will then be converted to lactic acid • Carnitine can temporarily scavenge acetyl CoA to form acetylcarnitine thus alleviating lactic acidosis in the muscle. C H3 H 3C N G L Y F O L A P C C + H C H2 C H3 C OH O C H2 O C A O- c L e Y A X C T I a T D r Y A T p d y e r h u y v d Y T A R A C U T T E V n E C T A C 37 Carnitine supplement Uses 1. Improves quality of life and walking performance in patients with limited walking capacity e.g., from end-stage renal disease and peripheral arterial disease. 2. Neurodegenerative diseases and recovery from cerebral ischemia. 3. Possible ergogenic aid but can cause an unpleasant body odour likened to rotting fish. 4. Improves memory of old rats (PNAS 99, 1876-81 (2002)) Biochemistry 1. Increases carnitine content, carries activated fatty acids across mitochondrial membrane and required for mitochondrial fatty acid oxidation. 2. Prevents acetyl CoA accumulation which inhibits pyruvate dehydrogenase. 3. Chelates iron and stabilizes membranes (antioxidant properties) 38 Carnitine supplement (cont) Sources Meat and dairy products exported and synthesized by liver > kidney from lysine + methionine. Highest levels in skeletal muscle, heart, adrenal gland but can’t synthesise it so take it up from the plasma. - total body store = 20-25gms. Oral Bioavailability 5-15% But over-the-counter formulations have low carnitine content and poor dissolution. - plasma acylcarnitines accumulate Journal of the American College of Nutrition, 17, 207-215 (1998) Progress in Cardiovascular Diseases, 40, 265-286 (1997) 39 c) Ketogenic diet therapy (results 10-25% seizure free & 60% better) for epileptic children resistant to phenytoin or valproate Energy Source Normal Diet Ketogenic Diet Protein 27% 10.4% adequate Carbohydrate 56% Fat 17% 89.6% Ketogenic diet consists of an egg nog that tastes like a mild shake (or frozen like ice cream) Supplying the body with fuel in the form of fat and proteins but not carbohydrates. fasting, diabeties Ketogenic diet Ketone Bodies Brain uses either glucose or ketone bodies as fuel Liver produces ketone bodies 40 d) Drug induced Fatty liver by inhibiting fatty acid oxidation. Liver (steatosis) and NASH (nonalcoholic steatohepatitis & whilst 5% of these get liver cancer) Steatosis (fatty liver) in 33% population & 80% of obese patients. Higher also in diabetes , high plasma triglycerides. NASH in 2-9% patients undergoing routine liver biopsy. Hepatocellular carcinoma rarely. Drugs that inhibit mitochondrial β-fatty acid oxidation 1)Tetracycline, valproic acid,oestrogens,glucocorticoids 2) Amiodarone,perhexiline are charged lipophilic drugs concentrate in liver mitochondria & inhib. β-fatty acid oxidn & respiration, cause lipid peroxidn. & reactive oxygen species (ROS). Steatosis and steatohepatitis are independent. Fibrosis occurs. 3) Drugs induce sporadic events of both e.g. carbamazepine 4) Latent NASH e.g. tamoxifen 41 e) Ethanol induced steatohepatitis (ASH) proposed endotoxin fatty liver mechanism 1) Ethanol causes lipogenesis and fatty liver (caused by inhibition of LDL synth. & export). 2) Ethanol oxidised by CYP2E1 to form hydroxyethyl radicals AND ethanol oxidised by ADH to form acetaldehyde which cause oxidative stress and hepatocyte/gut cytotoxicity. 3) Oxidative stress disrupts intestinal mucosal cell actin cytoskeleton (prev. by oats supplement). 4) Intestine becomes leaky & endotoxin enters blood & liver which causes liver inflammation and ASH. JPET 329,952-8(2009) 42