* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Hormone
Hormone replacement therapy (menopause) wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Signs and symptoms of Graves' disease wikipedia , lookup
Hormonal breast enhancement wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Hypothalamus wikipedia , lookup
Hypothyroidism wikipedia , lookup
Growth hormone therapy wikipedia , lookup
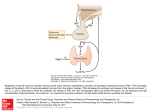
DEVELOPMENT OF THE ENDOCRINE SYSTEM Prof. Dr. Olcay Evliyaoğlu Steroid hormones: are not stored rate of synthesis = rate of secretion Adrenal, gonadal steroids: Synthesis is controlled by trophic hormones. Stimulating hormone -------> receptor --------> activation of adenylate cyclase ------> cAMP increases McCune Albright Syndrome: Activating mutation in the alpha subunit of G protein. Testotoxicosis: Activating mutation of LH receptor ( transmembrane domain - interaction with G protein.) Disorders of hormone resistance Insulin resistance Testicular feminization Certain types of dwarfism Diabeted insipidus (nephrogenic) Pseudohypoparathyroidism Hormone ↑ --> receptor number decreases “down regulation” or “desensitization” obesity - insulin precocious puberty - GnRH analogues Hormone ↑ --> receptor number increases “up regulation” estrogen - FSH ↑ ---> LH receptors increase Distinguishing characteristic of endocrine systems: feedback control & hormone production. The paradigm for feedback control is the interaction of the pituitary gland with the thyroid, adrenals and gonads. Hormones produced in peripheral endocrine organs feedback on the hypothalamic-pituitary system ------> regulate the production of the trophic hormones that control peripheral endocrine glands. Negative Feedback Metabolite Cortisol --> ACTH/ CRH Thyroid hormones --> TSH /TRH Short Feedback TSH --> TRH ACTH --> CRH Positive Feedback Hypophysogonadal (only example) : Estrogen --> LH, FSH Adrenal gland develpment Embryology Mesoderm........adrenal cortex Ectoderm.........adrenal medulla 5-6 wk fetal adrenal cortex Outer definitive zone (glucokortikoids and mineralocorticoids) Inner fetal zone (androgenic precursors) At birth AG is 0,5 % of total BW Glomerulosa 15 % Fasiculata 75 % Reticularis 10 % Fetal zone disappears around 1 years of age Glomerularis and fasiculata development is completed in 3 years. Reticularis development is completed in 15 years Fetal cortisol --> cortisone (Midgestation: cortisone (x4-5 cortisol)) Cortisone: relatively inactive glucocorticoid; it protects the anabolic milieu of the fetus: cortisol can retard placental and fetal growth. As term approaches; liver, lung express 11-beta hydroxy steroid dehydrogenase I activity: cortisone --> cortisol Cortisol: an important stimulus for preparing the fetus for extrauterine survival. Development of pituitary gland Growth hormone The most produced hormone in the pituitary. Single chain alpha-helical nonglukolized polypeptide. Consists of 191 aminoacids and two intramolecular disulfide bounding. 22kDa molecüler weight 75% 20kDa 10-25% N-asetile ve desamine forms veya oligomers GH GH-BHBP Extracellular part of GH rec Growth hormone Encoded by GH-1 gene. Locolized on 17q 22-24 chromosome. GH secretion Under control of 2 hypothalamic hormones Growth hormone releasing hormone(GHRH) Somatotropin release-inhibiting factor (SRIF, somatostatin) GHRH Protein with 44 aminoacids Vazoactive intestinal polypeptide/ glukagon family GH secretion Human growth hormone (hGH) Nonpulsatile GH secretion in infants. During childhood 24 hour integrated GH secretion increase progressively. In puberty GH secretion amplitude increase to peak levels ( effect of gonadal steroids on GHRH). GH secretion decrease with age but secreted life long. GH-releasing peptides (GHRP)or secretagogues (GHS) Ligands that increase GH produced by humans Do not use GHRH or SRIF receptors GHS-R G-protein associated rec protein kinase C hypothalamus, pituitary somatotrophs Ghrelin Endogen ligand for GHS-R. Increase GH secretion in rats (intracellular Ca increase). Physiologic mediator of nutrition GH effect Bound to GH-binding protein (GHBP) (at least 50 %) GHBP, is the extra cellular component of GH-R GH-R member of cytokine rec family 620 aa protein On plasma membrane. Extracellular part is transport protein Single transmembrans helix Intracellular part GH IGF’s (somatomedins) Similliar to proinsuline Effect on extrauterine growth via IGF-1ile (70aa polypeptide) Disorders associated with low IGF-1 levels GH deficiency Hypothyroidism Malnutrition Chronic diseases Fetal IGF-1 is correlated with gestastional age Newborn IGF-1 levels are 30-50 % of adult values Increase through out childhood and reach adult levels in puberty Gonadal steroids increase IGF-1 production. In puberty levels are 2-3 fold higher than adult values Increase osteoblastic activity and collagen synthesis stimulate long bone growth IGF’ s are bound to IGF binding proteins (IGFBP) t½ Transport to target tissue. Modulate the relation with IGF rec 6 different IGFBP are cloned IGFBP-3, 90 % related to GH IGF-1 rec Structure resembles insulin rec (2 alpha,2beta subunits) GH increase GHRH Arginin,leucine Alpha adrenergic agonists (alpha 2 adrenergic) Beta adrenergic antagonists Dopamine, acetylcholine Hypoglycemia Sleeping Exercise GH decrease Hypergylcemia Obesity İncrease in free FA Glucocortikoid excess Hypothyroidism Incresed adrenergic tonus Psychosocial deprivition Thyroid gland development Is derived from primitive pharynx-precursor of T4 producing cells And fourth pharengeal pouchprecursor of calcitonin(C) cells For development and descent of thyroid several transcription factors such asTITF1/NKX2, FOXE1 and PAX 8 are needed to work on time and coordinated Embryogenesis After 1st month it is visable. At ıntrauterin 8 wk Tg synthesis begins shows thyroid activity 10. wk iodine trapping 12. wk colloid formation begins and withTSH sec from pituitary T4 synthesis begins This synthesis increase progresively with hypothalamic maturation after 18 wk of gestation Thyroid hormone biosynthesis Tiroid kolloidi tiroglobulin Protein sentezi Çekirdek DNA/RNA sentezi G proteini Damar Thyroid hormone synthesis Uptake I uptake actively with Na-iodine pump Thyroid hormone synthesis Organification İyodine + thyroglobulin MIT DIT Thyroid hormone synthesis Conjugation MIT + DIT DIT +DIT Thyroid peroksidase(TPO) T3 T4 TİROKSİN (T4) (fenol halkası) (tirozil halkası) I I 5’ HO 6’ 1’ b 4’ 3’ 5 O a 4 3 2’ I 1 CH2 CH NH2 2 I Tip I-II monodeyiodinaz 5’ - monodeyidinasyon Tip III monodeyiodinaz I R COOH 6 I R O I I T3 5 - monodeyidinasyon R R O I I rT3 Serum thyroid hormone concentrations TT3 TT4 TBG rT3/T4 Effects of thyroid hormones Growth O2 usage Heat production Nerve functions Lipids Proteins Nucleic acids Vitamins Inorganic ions Other hormones Effect metabolism Actions of thyroid hormones Regulation of thyroid hormones Regulation of thyroid hormones G Protein TSH CAMP Adenilate cyclase ATP Iodine uptake İodothyrosine synthesis Tg synthesis Glucose oxidation Colloid pinositosis Hormone secretion Thyroid growth Regulation of thyroid hormones Physiologic limits Thyroid membrane iyodine uptake Iodine intake Pharmachologic doses TPO activity Iodine organification (Wolf Chaikoff effect) TSH induced CAMP stimulation inhibitted • Tg synthesis • Hormone secretion • Thyroid growth Iodine needs in different times of age Age and stages of life Daily idoine recommendation(g) 6< 30 6-12 months 40 1< years in iodine deficient regions 1-10 years Adoles and adults Pregnant and lactating women 90 60-100 100 150 İYOT KLİRENSİ TSH (+) dolaşım Follikül hücresi ATPaz bağımlı Na-I simporter I2 I I %20 Pasif reabsorbsiyon %80 + GFR Daily iodine excretion gives intake İdrarla iyot atılımı Iodine induced hyperthyoridism (Jodbasedow effect) Nodular thyroid disease with otonomy and with out antibodies Diffuse goitre with thyroid stimulating antibodies Jodbasedow effect only in thyroids independent from TSH Iodine deficiency Iodine deficiency disorders (IDD) global heath problem World’s most common endocrine disorder Most frequent reseason for goitre and hypothyroidism IDD Goitre Hypothyroxinemia Neurodevelopmental disorders Cretinism Decreased fertility Still birth Increased perinatal mortality IDD indicators Decreased urinary iodine concentration Increased serum hTg concentration Increased newborn and cord blood TSH concentration There is a U type relation between Iodine intake and thyroid disease Thyroid disease risk