* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Hx - Palliative Care
Polysubstance dependence wikipedia , lookup
Toxicodynamics wikipedia , lookup
NMDA receptor wikipedia , lookup
Drug interaction wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Oral rehydration therapy wikipedia , lookup
Theralizumab wikipedia , lookup
Methylphenidate wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Psychopharmacology wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
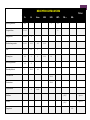
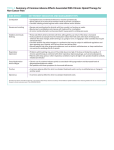
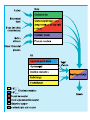
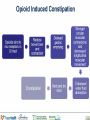
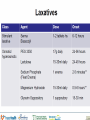
A mechanistic approach to Nausea Vomiting and Constipation in the ED Emergency/Palliative Medicine Workshop for UBC Emergency Medicine Residents Susanne Moadebi PharmD BCPS July 27th, 2016 HOPE Centre Outline List common mechanisms which cause nausea and vomiting Classify antiemetic agents based on major neurotransmitters and receptor targets Review antiemetic use and new agents for treatment of constipation in the emergency department Outline treatment principles for Malignant Bowel Obstruction Cases 2 RECEPTOR ANTAGONISM D2 Metoclopramide H1 AchM 5HT2 +++ Domperidone ++++ Haloperidol ++++ + Methotrimeprazine ++++ +++ ++ CPZ ++++ ++ + Olanzapine ++ + + Prochlorperazine ++ + Dimenhydrinate + ++++ 5HT3 5HT4 + ++ NK1 +++ +++ ++ ++ ++++ Granisetron ++++ + CB1 + 2 + Ondansetron Scopolamine Notes + ++++ Nabilone (++)* *Agonist Sativex (++)* *Agonist Aprepitant +++ Case 1 17 y/o female Presents to ED with Mother due to crampy dull generalized abdominal pain 6/10 for 2 weeks Having difficulty keeping water down, 3 episodes of emesis in 24 hours Last BM 12 hours ago was loose no blood Travel to France with school 3 weeks ago Hx Bipolar depression/ADHD/ no eating disorder no drug allergies no gluten allergies, reviewed sexual history Meds Lithium carbonate LA 600mg/day Methylphenidate LA 54 mg/day increased from 36mg/day 2 weeks ago during midterm exams PE BP 124/80 HR 95 T37C oral Pain 6/10 Mild tenderness, no peritoneal signs, no guarding no rebound no acute appendicitis Labs Lipase WNL Hcg negative Lithium WNL CBC (WBC normal) urinalysis normal ERP contacted Pharmacist to review her home medications What add? anti-emetic would you think to Case 1 continued methylphenidate acts as a dopamine and norepinephrine reuptake inhibitor resulting in a prolongation of dopamine (D1/D2) receptor effects. It is believed that methylphenidate activates the brain stem arousal system and cortex. The most common side effects associated with methylphenidate include headache, nausea, vomiting, anorexia, dizziness, and insomnia. Case 1 Resolution Optimizing Therapy The Dopamine Dilemma Treating side effects of a stimulant with an antipsychotic, may mask symptoms temporarily while worsening the underlying chemical imbalance over the long term Lithium or MPH can provide visceral stimulation mediated nausea involves using the D2 and 5HT3 antagonist which are effective with IV rehydration Intervention Metoclopramide 10 mg iv dose then switch to po at home. Iv fluid rehydration Temporary stop lithium. Concern about level trending up and renally accumilation Pharmacist contacted Psychiatrist to review her home medications – return to previous dose methylphenidate 36 mg daily Monitoring and Evaluation What options could we consider for further management of her nausea? What happens if her nausea worsens and is accompanied by intermittent vomiting and retching? + Cannabis and cannabinoids Plant derived cannabinoids THC – has psychotropic effect that produces “high” CBD cannabidiol & CBN Cannabinol have anti-seizure anti-nauseant anti-anxiety Tolerance may occur with chronic use. Hyperemesis may be observed with larger doses or chronic use Synthetic cannabinoids Nabilone Cesamet® Endocannabinoids anandamide -2-arachidonolglycerol 2_AG The body produces stimulate cannabinoid receptors naturally. There are at least two different types of cannabinoid receptors in the body: CB1 receptors in the brain and nervous system, and CB2 receptors in the immune system. Case 2 Hx HR+ HER2-mBC mets to lung/spine no known drug allergies. Followed by GP for palliative services Meds 64 y/o female Presents to ED with declining oral intake due to intractable nausea. Complains of hard stools, incomplete evacuation, bloating, abdo pain. No BM x 10 days She has tried PEG 3350 17g x 2 doses, glycerine suppositories, magnesium citrate, docusate sodium and psyllium powder Exemestane 25mg po daily Morphine Long-acting capsules 120mg po BID recently increased 2 weeks ago PE BP 178/89 HR 108 T37.6C oral Pain 8/10 Labs CHEM7/CBC (WBC normal) urinalysis normal, lipase, liver panel normal Abdominal XR – no obstruction but faecal loading shown on x-ray ERP contacted Pharmacist to review her home medications What would you treatment would you consider? Case 2 Resolution Opioid induced constipation – how would you treat? Intervention – use a peripherally acting mu-opioid receptor antagonist- 62 kg give Methylnaltrexone 8mg sc T1/2 8 hours and T peak 30 minutes with no withdrawal of analagesia Time to first laxation is 4 hours & will see appetite improve Monitoring Watch for dizziness, abdo pain cramping start regular PEG and sennosides PEG is more effective than lactulose for prevention Drug name Indication Class/Mech. of Action Onset of Action Methylnaltrexone (Relistor) Adjunct in refractory opioid induced constipation for palliative care patients Mu opioid receptor antagonist 30-60m Naloxegol (Movantik) Opioid induced constipation Mu opioid receptor antagonist Lubiprostone (Amitiza) Opioid induced constipation Prucalopride (Resotran) Linaclotide (Constella) Drug Dosing/Dosage Form Metabolism/Cle arance Adverse Effects Administered subQ q48 hours PRN Weight and Renal Fxn: 8mg / 12mg /‘0.15mg/kg CrCl <30mL/min: ↓ dose by 50% Dosage Form: Subcutaneous injection Substrate of CYP2D6 (minor); Urine (54% as unchanged drug) T1/2 = 8h Abdominal pain, diarrhea, flatulence, nausea, dizziness. Risk of GI perforation in patients with cancer, GI malignancy, GI ulcer, Ogilvie’s syndrome Time to peak: <2h 25mg PO daily CrCl <60ml/min - start at 12.5mg daily and may increase to 25mg daily if well tolerated Dosage Form: Tablets (12.5mg, 25mg) Substrate of CYP3A4 Urine (16% as unchanged drug); Primarily hepatic T1/2 = 6-11h Headache, nausea, diarrhea, vomiting, hyperhidrosis Type 2 Chloride Channel Activator Time to peak: ~1h 24mcg PO BID Dosage Form: Capsule (8mcg, 24mcg) Rapid and extensive within stomach and jejunum by carbonyl reductase T1/2 = 0.9-1.4h Headache, nausea, diarrhea, edema, dizziness, abdominal pain, dyspnea Refractory opioid induced constipation in females 5HT4 Recepto r Agonist 2-3h 2mg PO daily CrCl <30mL/min = 1mg PO daily Dosage Form: Tablet (1mg, 2mg) Substrate of Pglycoprotein Minor route of elimination T1/2 = ~24h Nausea, diarrhea, abdominal pain, headache Refractory opioid induced constipation Guanylyl cyclase C agonist Not available Metabolized within GI tract to active metabolite T1/2 = Diarrhea, headache, abdominal pain, flatulence, URTI 145mcg PO daily Dosage Form: Capsule (145mg, 290mg) Case 3 Hx Stage IV gastric CA dx 1 year ago; anxiety and depression. Multiple cycles of chemo (last one month ago) with progressive carcinomatosis. Has tried TPN several times but failed J-tubes in the past. Meds oxycodone 10 mg TID 56 y/o male Presents to ED with recurrent nausea seen here yesterday – recalcitrant nausea NYD. No emesis, no diarrhea, loose stools last few days; covering eyes states makes it better for his nausea He has tried ondansetron and metoclopramide; admit for symptom management clonazepam 0.5mg TID paroxetine 60 mg once daily PE BP 178/89 HR 108 T37.6C oral Pain 8/10 Mild Labs CHEM7/CBC (WBC normal) urinalysis normal, lipase, liver panel normal Abdominal CT –found malignant intestinal obstruction due to carcinomatosis ERP contacted Pharmacist to review his home medications What would you treatment would you consider? Dx Malignant Bowel Obstruction Metoclopramide Haloperidol (5–15 mg/day) Methotrimeprazine (50–150 mg/day) Hyoscine butylbromide (Buscopan®) (60-120mg/day) Octreotide (200 - 900 mcg/day) Steriods Case 3 Resolution Decadron 8mg SQ BID, metoclopramide10mg SQ q6h, octreotide 100mcg SQ q8h Corticosteroids also are used to reduce inflammatory edema and decrease water and salt secretion in bowel. They are relatively inexpensive and well tolerated. First line involves steroids, antiemetics, anti-cholinergics, analgesics and parental rehydration. If it fails, somatostatin analogues supersede steroid and anticholinergics. Take home points 1) 2) 3) 4) VOMIT acronym Better to use metoclopramide consider D2 antagonism which may offset decreased persistalsis caused by the opioids For palliative/frail patients with constipation add an osmotic laxative (e.g PEG 3350) Don’t use docusate insufficient evidence to support its use. Use octreotide for malignant bowel obstruction Questions?