* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Systemic Inflammatory Response to Cardiac Surgery
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
DNA vaccination wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Complement system wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
Atherosclerosis wikipedia , lookup
Innate immune system wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Inflammatory bowel disease wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Inflammation wikipedia , lookup
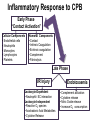
The Systemic Inflammatory Response to Cardiac Surgery Aims and Objectives To provide an overview of: • Pathophysiology of the inflammatory response in cardiac surgery. • Factors influencing the extent of the inflammatory response . • Clinical implications . • Therapeutic strategies. SIRS: Systemic Inflammatory Response Syndrome • A nonspecific, generalised inflammatory response, independent of causative factors but an indicator of injury. • Symptoms of “sepsis” can arise in the absence of an infection. • A frequent complication of SIRS is the development of organ dysfunction. • Long term survival of patients developing SIRS may be adversely affected. Clinical Implications of the Inflammatory Response to Cardiac Surgery • Beneficial? : Immune system priming may help prevent perioperative infection and promote wound healing. However……. • An uncontrolled inflammatory response contributes to the pathogenesis of: * Acute pulmonary dysfunction * Cardiovascular dysfunction * Neurologic dysfunction * Renal dysfunction * Splanchnic dysfunction * Hematologic dysfunction Factors That Activate the Inflammatory Response • Surgical trauma. • Blood loss, haemodilution and transfusion. • Hypothermia. • Anaesthetic drugs • CPB. CPB and The Activation of the Inflammatory Response • Contact activation: exposure of blood to foreign surfaces of the circuit. • Ischemia, hypoperfusion / reperfusion injury to all organs. • Endotoxemia: Splanchnic hypoperfusion may damage mucosal barrier allowing translocation of endotoxin. (Other sources of endotoxin include priming fluid and cardioplegia) Complement Activation and Cardiac Surgery • Contact activation: exposure of blood to foreign surfaces of the circuit. (Blood-gas interface may play a part). (Alternative pathway) • Ischemia, hypoperfusion / reperfusion injury to all organs. (Alternative pathway) • Heparin neutralisation with protamine. Delayed activation of complement appears to be mediated by CRP in response to large heparin-protamine complexes. (Classical pathway) Cytokines and Cardiac Surgery • Proinflammatory cytokines stimulate the inflammatory response; plasma concentrations of specific cytokines are predictive of outcome in critically ill patients. • Tumour necrosis factor α (TNF α) and Interleukin 1β (IL-1 β) are elevated early following cardiac surgery, with IL-6 and IL-8 peaking later. • Direct cause and effect are not fully understood however elevations of proinflammatory cytokines are associated with adverse events. Patients who develop SIRS have significant elevations in cytokine levels compared to patients who have an uncomplicated recovery following surgery. Coagulation-Fibrinolytic Cascades • The coagulation-fibrinolytic cascades and the inflammatory response are separate processes however they are closely interconnected. • Haemostasis is mediated by a balance of procoagulant and anticoagulant properties which are tightly controlled. • Coagulation factors including the activation of tissue factor are initiated in response to inflammatory stimulus, oxidative or shear stress during CPB. • The endothelium is intricately involved in both processes. Heparin and Protamine • Drugs used to modulate coagulation during cardiac surgery. • Heparin appears to possess important anti-inflammatory effects however protamine neutralisation results in significant cardiovascular effects. (Note caution and speed of delivery of protamine during surgery). • Although protamine itself has adverse effects, it is the heparin protamine interaction that activates the inflammatory response. * Complement activation * Histamine release * Thromboxane, nitric acid production and antibody formation In a minority of patients severe anaphylactic reactions may result from the heparin-protamine interaction. The Endothelium • The vascular endothelium is a dynamic participant in cellular and organ function rather than a static barrier. • The inflammatory response to CPB is characterised by a state of widespread endothelial activation and injury. • The endothelium controls vascular tone and permeability, regulates coagulation and thrombosis and directs the passage of leukocytes into areas of inflammation. • Inflammatory mediators including TNFα and IL-1β bind to specific receptors on the endothelium. This schematic diagram depicts the role of the endothelium in the regulation of vascular tone and illustrates important early events known to occur in systemic inflammatory response syndrome (SIRS). The endothelium regulates local vascular tone and adapts organ blood flow to metabolic needs, by altering the balance of 4 key mediators: nitric oxide (NO), prostacyclin (PGI2), thromboxane (TXA2), and endothelin (ET) Endothelial Damage • Vascular endothelium damage plays a central role in the pathogenesis of microcirculatory derangement following CPB. • An increased pulmonary vascular resistance (PVR) following CPB is attributed to reduced Nitric Oxide (NO) release from dysfunctional pulmonary endothelium. (Reversed by NO supplementation). • Loss of vasodilator and antithrombotic effects of NO may alter myocardial perfusion. • Endothelial dysfunction and associated inflammatory response may alter long term survival; patency of grafts, progression of atherosclerosis. (Recruits leukocytes and platelets to the arterial wall). Illustration of Neutrophil-Endothelium Interaction Each neutrophil represents a key event within the capillary, from right to left. * Initially the freely moving neutrophil is converted to the “rolling” state. * The neutrophil loosely interacts with the endothelium via the expression of selectins (adhesion molecules) on both membranes. * The expression of integrin receptors result in tighter binding to the capillary wall. * In the third stage the neutrophil becomes tightly bound to the endothelium and transmigrates out of the circulation, triggering activation, degranulation and further endothelial injury. Factors Influencing the Extent of the Inflammatory Response • Preoperative: * Disorders of cytokine balance. * Diabetic patients- impaired micro circulation may effect immune response. • Anaesthetic Techniques: * Anaesthetic drugs- Many of the drugs used possess immunomodulatory effects. * Lung management –Apnea is associated with enzyme production and Acute Lung Injury (ALI). • Surgical Factors: * Type of operation ( length of ischemic time) * Inflammation appears to correlate with severity of illness; ventricular dysfunction increases cytokine concentrations. CPB and Immunological Response • • • • • • • • • • The composition of the priming solution Cardioplegia Pulsatile or nonpulsatile flow Hemofiltration Roller or centrifugal pump Type of circuit (biocompatible) Temperature Blood transfusion Cardiotomy suction Hypoperfusion Inflammatory Response to CPB Early Phase “Contact Activation” Cellular Components • Endothelial cells • Neutrophils • Monocytes • Lymphocytes • Platelets Humoral Components • Contact • Intrinsic Coagulation • Extrinsic coagulation • Complement • Fibrinolysis Late Phase I/R Injury Leukocyte-Dependent • Neutrophil- EC interaction Leukocyte-Independent • Reactive O2 species • Arachadonic Acid Metabolites • Cytokine Release Endotoxaemia • Complement activation • Cytokine release • Nitric Oxide release • Increase O2 consumption CPB and Immunological Response Temperature: • The release of inflammatory mediators appears to be temperature dependent. Warm CPB is associated with an increased inflammatory response compared to hypothermic CPB. However hypothermic CPB may simply delay cytokine release and neutrophil activation. • Evidence suggests tepid CPB (32-34°C) most effectively attenuates the inflammatory response. CPB and Immunological Response Circuit adaptation: • Heparin-coated circuits reduce complement and proinflammatory cytokine release. More evidence is required to analyse clinical significance. • Some studies demonstrate that centrifugal pumps result in less activation of the inflammatory response. CPB and Immunological Response Shear Stress: • Excessive shear stress may develop during CPB as a result of pressure changes across the circuit. Damage to blood constituents activates the inflammatory response. • Shear stress appears to be particularly significant at the tip of the arterial cannula and is associated with haemolysis. • Leukocyte adhesiveness is increased, with neutrophil degranulation and release of cytotoxic products further inducing endothelial damage and immune response. Blood Transfusion • Restrictive Transfusion Strategies?! • Do we know the exact content of a bag of packed cells? CPB and Immunological Response Blood Transfusions: • Blood transfusions are associated with an increased morbidity and mortality in cardiac surgery patients. • The immunomodulatory effects of blood transfusions are increasingly recognised. • Packed red cells directly increase the concentration of inflammatory mediators and indirectly stimulate the inflammatory response. • Aged packed cells contain a high proportion of deformed erythrocytes and debris which cause microcirculation occlusion, damage and tissue ischemia in some organs. CPB and Immunological Response Hemofiltration: • Why do we use hemofiltration therapy? Modify immune response? • Hemofiltration appears to remove TNF α and IL-1β and their inhibitors from the plasma of patients with SIRS. • The advantage that comes with the removal of inflammatory mediators must be balanced against the removal of clotting factors and other useful metabolites. It is critical to always treat the patient as a whole and not to focus on one aspect. CPB and Immunological Response Cardiotomy Suction: • Do all surgeons use them? • Shear stress and negative pressure in conjunction with air/blood interface activation leads to immunologically activated blood. • Separate reservoir. • Cell salvage • Sucker bypass scenario? CPB and Immunological Response Endotoxins: • Hypoperfusion and inflammation effect the permeability of the mucus membrane within the gut. • Translocation of Endotoxins from the gut increases the immune response. Endotoxins are present elsewhere. • Strategies to reduce endotoxemia are done routinely for gastric surgery; Selective Digestive Decontamination (SDD): Oral nonabsorbable antibiotics reduce the gut content of enterobacteria. Schematic diagram of potentially useful strategies and therapies to control the inflammatory response in cardiac surgery. Conclusion • Cardiac surgery evokes a generalised inflammatory response in all patients, with serious clinical consequences in a minority. • A balanced, controlled inflammatory response is potentially beneficial however a loss of control may lead to SIRS and consequently organ dysfunction. • We can make a difference! • Research is on going into strategies and therapies to reduce the immune response