* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Myocardial infarction wikipedia , lookup
Artificial heart valve wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Atrial septal defect wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
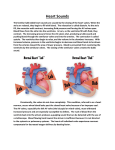
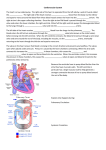
The Cardiovascular System Name____________________ per___ I. Vessels A. Artery Strong elastic vessel that takes blood ________ form heart Under __________________ 3 layers: 1.________________endothelium, 2.________________smooth muscle, 3.________________connective tissue B. Arteriole Smaller arteries with smooth muscle Help control flow of blood by _______________&______________ Layers of vessel get _________ as they approach ____________ C. Capillary Smallest diameter ~_____________ Diffusion of ___________, gases& waste between blood system & cells Can _______ or __________ depending on blood flow needed to area D. Venule Merge to form________________ Start path back to ______________ E. Vein Returns blood to heart _______________ pressure ___________ walls, __________ muscle but ___________ diameter than arteries Valves ___________ back flow of blood Skeletal muscles help blood flow toward ______________ Blood reservoir: 1.veins ______________ to increase blood pressure in times of blood loss 2.Can maintain normal pressure with up to _____% loss of blood volume. II. The Heart A. General characteristics Involuntary, _______________ muscle Located between the lungs, behind sternum in ________________ 14cm x 9cm ( about the size of your ________) Specialized muscular pump( 2 in 1) Right side is “____________________” Left side is “ ____________________” The _________ is located at second rib(top) The___________ is located at the 5th intercostals space, left of sternum heart extends down and to the left ( base to apex) B. Heart coverings pericardium has _________ layers 1. ______________pericardium- outermost sac around heart; tough/dense tissue 2. ______________ pericardium: inner lining of fibrous pericardium 3. _______________pericardium: inner most layer; directly attached to heart. C. Heart Wall _______________: outmost layer of the heart( AKA visceral pericardium) ________________: middle layer: actual cardiac muscle ________________: inner most layer; lines chambers, covers all internal structures. D. Heart Chambers Atria: 1. _____________________ 2. thin walls 3.______________blood returning to the heart from body 4. pushes blood into __________________ 5._____________: small earlike appendages attached to atria 6.interatrial septum:_______________ atria 7.________________: remains of old foramen in fetal heart. Ventricles 8. 2 lower chambers 9. thick, muscle wall 10. force blood out of heart to lungs or body 11. papillary muscles attach to valves 12. interventricular septum: divides ventricles E. Valves i. Atrioventricular valves( AV) 1. Have cusps that point downward into ventricle. 2. force blood 1 direction 3. close to stop backflow of blood 4. closing of valves give “lubb-dubb” sound to heart 5. attached by Chordae tendonae to papillary muscles a. Tricuspid valve( 3 cusps) i. between R. Atrium & R. ventricle b.Bicuspid valve( 2 cusps) i. ( mitral valve) ii. between L. Atria & L. ventricle ii. Semilunar ( SL) Valves 1.. pulmonary valve: between R. ventricle & pulmonary artery 2. Aortic( semilunar) valve: between L. Ventricle & Aorta F. Blood flow through heart i. Deoxygenated side 1.from body via inferior & superior vena cava 2. Right atrium 3.tricuspid valve 4.right ventricle 5.pulmonary semilunar valve 6.pulmonary trunk 7.right & left pulmonary arteries 8.to lungs H. ii. Oxygenated side 1.from lungs via right & left pulmonary veins 2.left atrium 3.bicuspid valve 4.left ventricle 5.aortic semilunar valve 6.aorta 7.out to body iii. Coronary circulation 1.coronary arteries branch off aorta a. give oxygenated blood to heart 2.coronary sinus (vein) a. divides apex & base b.lies in coronary sulcus c. empties into right atrium G. Cardiac cycle i. Complete cycle of atrial & ventricular contractions 1. Atrial pressure> ventricular: A-V valves open a. Blood flows into ventricles 2.Atria Contracts: pushes blood into ventricles 3.Increase pressure in ventricles > atrium, contraction a. A-V valve close b. Papillary muscles contract to hold valves open 4. Atria relaxation: blood flows into chamber a. Semilunar valves (SLV)open: blood forced into arteries 5. ventricles relax : SLV close a. When ventricular pressure< atrial pressure: A-V open b.Brief time when both atria & ventricles are resting Electrocardiogram(ECG) i. Record of electrical change in myocardium during cardiac cycle 1.P-Wave: depolarization of ventricles a. Leads to atrial contraction b.S-A node triggered 2.Q-R-S Complex: depolarization of ventricles a. Leads to ventricular contraction b.Atria repolarized 3.T-Wave: repolarization of ventricles 4.P-Q interval: time for cardiac impulse to travel from SA node through AV node 5.A-V bundle injury: Increase QRS complex a. Takes longer to spread impulse through ventricles b.May be caused by decrease blood flow c. Artificial pacemaker can restore I. Heart Sounds i. Lubb-Dupp J. L. 1.Lubb- ventricular contraction; A-V valves close a. 5th intercostals space @ nipple line i. Left side=bicuspid ii. Right side= tricuspid 2.Dupp- Ventricular relaxation; SL Valves close a. 2nd intercostals space Heart Conduction system i. Muscle has inherent ability to contract ii. Muscle cells together contract to cell with the fastest rhythm iii. Initialed by “pace-setting” cells iv. Coordinates contraction so atria go 1st then ventricles 1.Sinoatrial node (SA) a. “pacemaker” b.Wall of right atrium c. Atrail contraction or systole d.Stimulates AV node 2.Atrioventricular node a. Relays signals to ventricles b.Bundle of His( AV bundle) to Purkinje fibers c. Ventricle contraction or systole K. Heart Action i. Cardiac output (CO): blood pushed / minute ~5,250ml/min or 5.25 L/min. ii. Stroke Volume(SV): how much blood pushed /beat ~70ml/min iii. Heart rate( HR): how fast heart beats/min ~ 75 bpm 1. CO = SV x HR 2.Starling’s law of the heart: explains how CO changes with levels of exercise & blood flow Blood Pressure i. Force against walls of blood vessels 1.Systolic Pressure: Ventricular systole a. Forced blood into pulmonary trunk & aorta increase arterial pressure b.Normal ~120mmHg 2.Diastolic Pressure: ventricular diastole a. Ventricles relax, pressure decreases b.Normal ~80 mmHg 3.Measuring Pressure a. Systolic over diastolic b.Normal 120/80 mmHg c. Use Sphyg/mo/ma/no/meter ( BP cuff) & stethoscope to hear Korotkoff sounds 4.Pulse a. Distention & recoil of arterial wall near surface b.Normal ~ 70-90 in adults, 80-140 in children c. Adult above 100 bpm : tachycardia d.Adult below 60bpm: bradycardia ii. Influences on Pressure 1.Blood viscosity: increased viscosity= increased pressure a. Dehydration/ anemia 2. Blood volume_ ~5L or 8% of body weight a. Hemorrhage/ dehydration= decrease volume 3. Resistance to flow: dilation/ constriction of vessels, M. a. peripheral resistance( PR) is friction of blood cells against wall of vessel b.change in diameter of vessels 4.Heart action: a. Co = SV x HR b.BP= CO x PR iii. Regulation of BP 1. Nervous system a. Adjusts CO & PR b. Autonomic control over SA node c. Vasomotor reflex center: constricts/ dilates vessels d. Baroreceptors: changes in pressure e. Chemoreceptors: changes in gases/ions 2.Hormonal controls a. Epinepherine/Norepinepherine i. Increase CO & PR ii. Arteriole vasoconstriction b. Atrial natriuretic factor i. Secreted by atria ii. Reduce blood volume, decrease BP iii. Does so via dehydration c. Antidiuretic hormone i. Increase blood volume, increasing BP ii. Kidneys conserve water 3. Kidney’s a. Maintain long term BP controls i. Regulate water excretion rate b. Release of Renin i. Triggers angiotensin: vasoconstrictor ii. Triggers aldosterone: reabsorb Na+/water follows iii. Increases BP by increasing BV & PR Capillary exchange i. Movement of fluid is caused by 2 forces 1. hydrostatic pressure a. pushes fluid out of vessel b. higher at artery end 2. osmotic pressure a. movement of fluid into vessel b. higher at venous end 3. some fluid goes into lymph system N. Circulation i. Pulmonary circulation 1. to/from lungs ii. Systemic circulation 1. to/from body