* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 37
Cardiovascular disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Infective endocarditis wikipedia , lookup
Heart failure wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Coronary artery disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Rheumatic fever wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Aortic stenosis wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
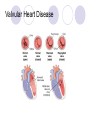
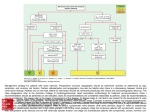
Chapter 37 Inflammatory and Structural Heart Disorders Valvular Heart Disease Valvular Heart Disease Stenosis Valve orifice is restricted Impending forward blood flow Creates a pressure gradient across open valve Degree of stenosis reflected in pressure gradient differences Regurgitation Incomplete closure of valve leaflets Results in backward flow of blood Mitral Stenosis Most adult cases result from rhematic heart disease Other causes Mitral valve becomes scarred and narrowed Left atrial overload eventually leads to right ventricular failure Mitral Stenosis Manifestations include fatigue, palpitations, dysrhythmias, low pitched diastolic murmur Mitral Regurgitation Mitral valve fails to close properly Usually chronic Blood flows back into left ventricle, elading to LA and LV dilation Manifestations include symptoms of LV failure, holosystolic murmur Mitral Valve Prolapse One or more of the mitral valve leaflets prolapses back into the left atrium during systole Usually congenital Usually benign, but can be problematic if it progresses to mitral regurgitation Most people asymptomatic, but manifestations may include CP, dyspnea and palpitations Aortic Stenosis Narrowing of the aortic valve causes obstruction of blood flow form the LV to the aorta during systole Common causes include congenital, rheumatic heart disease and senile or degenerative stenosis Manifestations: classic triad; systolic ejection murmur Aortic Regurgitation Aortic valve fails to close properly Blood flow back from the aorta into the LV during diastole-->volume overload of LV Cause may be acute or chronic (rheumatic disease, bicuspid AV, autommune conditions) Manifestations include signs and symptoms of LV failure (late), waterhammer pulse, high pitched diastolic murmur Tricuspid and Pulmonic disease Uncommon Will manifest as RV failure Diagnosis of valvular heart disease History and physical CXR ECG Echocardiogram Cardiac catheterization Collaborative Care Prophylactic antibiotic therapy Rheumatic fever, infective endocarditis Management of associated heart failure Vasodilators (except aortic stenosis) Inotropes (digoxin) Diuretics Beta blockers Anticoagulant therapy as indicated Surgical Treatment Percutaneous transluminal balloon valvuloplasty For stenotic disease Valve repair Eg, valvuloplasty, annuloplasty Valve replacement (prosthetic valves) Mechanical valves Biological valves Choice of valve depends on variety of factors Surgical Treatment Valve replacement Teaching Prophylaxis Anticoagulation Nursing Diagnoses and Interventions Activity intolerance Excess fluid volume Decreased cardiac output Deficient knowledge Chapter 37 Cardiomyopathies Cardiomyopathy Constitutes a group of diseases that directly affect the structural or functional ability of the myocardium Three major types Dilated Cardiomyopathy Characterized by diffuse inflammation and rapid degeneration of the myocardium that results in ventricular and atrial dilation and impaired systolic function May develop acutely or insidiously Manifest as heart failure, often biventricular Causes (table 37-18) Dilated Cardiomyopathy Interventions focused on improving heart failure Enhance contractility, decrease afterload Drugs Nitrates, diuretics, ACE inhibitors, beta blockers, aldosterone antagonists, anticoagulation Treat underlying disease process (as able) Cardiac resychronization therapy May require VAD or transplant Hypertrophic Cardiomyopathy Asymmetical left ventricular hypertrophy without ventricular dilation Primary defect is diastolic dysfunction May be idiopathic, often genetic Usually seen in young adults High risk of SCD Manifestations include dyspnea, fatigue, angina, syncope Hypertrophic Cardiomyopathy Collaborative management Reduce contractility and relieve outflow obstruction Drugs Beta blockers, calcium channel blockers Nitrates, digoxin contraindicated Avoid diuretics ICD placement Surgical treatment Teaching Avoid strenous activity Avoid dehydration Symptoms - elevate feet Restrictive Cardiomyopathy Impaired ventricular filling Manifestations include signs and symptoms of heart failure Treat to maintain cardiac output and manage symptoms Patient and Family Teaching for Cardiomyopathy Meds as prescribed Low sodium diet Hydration Avoid ETOH, tobacco and stimulants Balace activity and rest Avoid heavy lifting, discuss exercise with health care provider Stress reduction Report signs/symptoms of heart failure promptly May require IE prophylaxis