* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Title: Author - Department of Biochemistry and Molecular Biology
Survey
Document related concepts
Metabolic network modelling wikipedia , lookup
Point mutation wikipedia , lookup
Catalytic triad wikipedia , lookup
NADH:ubiquinone oxidoreductase (H+-translocating) wikipedia , lookup
Proteolysis wikipedia , lookup
Oxidative phosphorylation wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Photosynthetic reaction centre wikipedia , lookup
Nicotinamide adenine dinucleotide wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Metalloprotein wikipedia , lookup
Peptide synthesis wikipedia , lookup
Genetic code wikipedia , lookup
Citric acid cycle wikipedia , lookup
Biochemistry wikipedia , lookup
Transcript
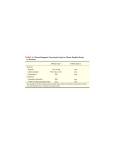
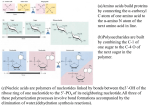
Title: Study of transaminases Author: János András Mótyán, Ph.D. assistant lecturer Department of Biochemistry and Molecular Biology Faculty of Medicine, University of Debrecen 2015 Date: 2014.12.01-2015.01.31. The development of this curriculum was sponsored by TÁMOP 4.1.1.C-13/1/KONV-2014-0001. The project is supported by the European Union and co-financed by the European Social Fund. 1 THEORETICAL BACKGROUND 1. TRANSAMINASES The Study of transaminases practice includes the study of the reversibility of transaminase reaction, the determination of serum glutamate-oxaloacetate-transaminase (GOT) and glutamatepyruvate-transaminase (GPT) activities by optical test and the determination amino acid composition of serum and urine in case of a metabolic disease (phenylketonuria). Therefore, here we are focusing on the transamination reactions and the degradation of phenylalanine and tyrosine, and we describe the theoretical background of the experiments. 1.1 Introduction Human proteins are built up by 20 different amino acids (Figure 1). These amino acids commonly found in proteins as residues have L-configuration (except glycine) and are α-amino acids (except proline, which is imino acid). All of these amino acid contains a carboxyl-group and an amino group attached to the α-carbon atom (α-amino acids), furthermore, a distinctive side chain. Amino acids can be differentiated based on the characteristics of the side chains: they can be classified into nonpolar, aromatic, polar and uncharged, negatively or positively charged groups. 2 Figure 1. Building blocks of amino acids. Several common types of reactions are involved in the metabolism of the amino acids, which have key role both in their degradation and in their synthesis. Such reactions are the transamination, deamination (oxidative and non-oxidative), decarboxylation (oxidative and nonoxidative), monooxigenation, dioxigenations and the transfer reactions of one-carbon units. Enzymes are classified into 6 classes by the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology (NC-IUBMB) based on the type of reaction catalyzed: 1. oxidoreductases 2. transferases 3. hydrolases 4. lyases 5. isomerases 6. ligases The transferases belong to the 2nd enzyme class (EC 2) and catalyze the transfer of a functional group between the donor and the acceptor molecule. The group of enzymes transferring nitrogenous groups (EC 2.6) contains the group of aminotransferases, also referred as transaminases (EC 2.6.1), which enzymes catalyze the transfer of an amino group from an amino acid to a keto acid. In this reaction a new amino acid and a new keto acid is released. 1.2 The transamination reactions 3 The role of transamination reactions is the elimination of the amino nitrogen from the amino acids. While in case of the deamination reaction the nitrogen is removed from the amino acid pool, the transamination reactions do not eliminate nitrogen from the pool. Quantitatively transamination it is the most important reaction type of the amino acid metabolsim. Transaminases exist for all amino acids except Lys and Thr. Usually the transamination is the starting reaction during the degradation of amino acids. Transaminases can be classified based on their cellular localization (cytoplasmic or mitochondrial), the position of the amino group (α, β, etc.) or the substrate partner molecule. In the transamination reaction the amino group of the amino acid substrate is transferred to pyridoxale phosphate cofactor of transaminase enzyme followed by its transfer to the keto acid substrate. Keto acid and amino acid products are produced in the reaction. Transaminase catalyzed reaction is reversible. Pyridoxale phosphate cofactor is regenerated in the reciprocal reaction, in which keto acid is used as substrate and amino acid product is released (Figure 2). Figure 2. General scheme of transamination. PLP = pyridoxale phosphate, PMP = pyridoxamine phosphate. Pyridoxale phosphate (PLP) is used as cofactor (Figure 3) by all transaminases. Pyridoxale phosphate is a derivative of Vitamin B6. 4 Figure 3. Structure of pyridoxine and pyridoxale phosphate cofactors. 1.2.1. Mechanism of transamination The pyridoxale phosphate is attached to a lysil sidechain of the enzyme via a Schiff base (imine) linkage, which could be substituted by an amino acid. The pyridoxale phosphate cofactor is covalently attached to the enzyme. After the binding of a substrate the cofactor will be attached to the amino acid, the covalent linkage will be disrupted between the cofactor and the enzyme. There are non-covalent interactions between the enzyme and the amino acid-bound cofactor. In the first step of the transamination reaction the amino group of the amino acid substrate attacks the enzyme-cofactor Schiff base, which step is resulted in the formation of an amino acidPLP aldimine. Through a quinonoid intermediate state the Schiff base is hydrolyzed, a pyridoxamine phosphate and a keto acid product is released (Figure 4). Figure 4. shows the first part of the overall catalytic process catalyzed by aminotransferases, in which amino acid substrate enters the catalytic cycle and keto acid product is released (left to right). To regenerate the PLPenzyme, the “first” keto acid (released as product) is replaced by a “second” keto acid which is used as substrate in the reversal steps (right to left). The amino acid is transferred from the pyridoxal phosphate to the “second” keto acid, leading to the release of an amino acid product. Figure 4. Mechanism of transamination. 1.2.2. Relevance of transamination 1.2.2.1 Transport of reduced electron carriers into the mitochondria from the cytosol 5 Reduced electron carriers are oxidized in the terminal oxidation. The reduced carriers which were produced by the pyruvate dehydrogenase or by reactions of citric acid cycle could be oxidized within mitochondria. The NADH released in a glycolytic reaction (catalyzed by glyceraldehide-3-phosphate-dehidrogenase) requires a transport mechanism, because the inner mitochondrial membrane is not permeable for NAD+ and NADH+H+. There are two main transport mechanisms which are responsible for the mitochondrial transport of NADH produced in the cytosol. These are the malate-aspartate and the glicerophosphate shuttles. Both shuttles are able for the transport of the reduced electron. While the malate-aspartate shuttle is reversible and works in case of high cytosolic NADH concentration, the glycerophosphate shuttle is irreversible and is independent from the NADH concentration. In case of the glycerophosphate shuttle the glycerol-3-phosphate-dehidrogenase converts the dihydroxiacetone-phosphate to glycerol-3-phosphate in the cytosol, along with the oxidation of NADH. After entering the mitochondrial matrix, the mitochondrial isoform of the enzyme converts the glycerol-3-phosphate back to dihydroxiacetone-phosphate along with the reduction of its FAD cofactor. By the help of this shuttle mechanism, the NADH released in the cytosol reaches the mitochondrial respiratory chain as FADH2. The malate-aspartate shuttle is also responsible for the transport of reduced electron carriers through the inner mitochondrial membrane. By the help of this shuttle mechanism, the NADH released in the cytosol reaches the mitochondrial respiratory chain as NADH. In the first step of the transport mechanism the NADH reduces the oxaloacetate to malate in the intermembrane space, which reaction is catalyzed by the malate-dehydrogenase enzyme. Malate enters the matrix by the malate-α-ketoglutarate transporter, where it is converted back to oxaloacetate, along with the reduction of NAD cofactor of malate-dehydrogenase and the release of NADH. In a transamination reaction the oxaloacetate is converted to aspartate (while glutamate is converted to α-ketoglutarate) by the aspartate-aminotransferase (glutamate-oxaloacetate transaminase). Aspartate is transported into the intermembrane space by the glutamate-aspartate transporter, where α-ketoglutarate is converted to oxaloacetate in a repeated transamination reaction. Oxaloacetate could be reduced by the malate dehydrogenase and enter the cycle again to transport NADH into the mitochondrial matrix (Figure 5). 6 Figure 5. The malate-aspartate shuttle. 1.2.2.2 Funneling nitrogen into glutamate The role of transamination is the funneling of amino nitrogens from amino acids to glutamate. The glutamate could be deaminated (see point 3) and the nitrogen funnelled into glutamate could be used to convert it to urea and eliminate from the amino acid pool (see point 5). The glutamate dehydrogenase catalyzed reaction has the highest relevance in the deamination. Deaminated amino acids can be used to produce energy by their fully oxidation. The glutamate has great relevance in transamination reactions, because the glutamate-αketoglutarate amino acid-keto acid pair, which are involved in several transamination reactions. 1.2.2.3 Trans-deaminastion In case of trans-deaminastion the common intermediate is glutamate, which is further converted by oxidative deamination after a transamination reaction. α-Ketoglutarate and ammonia is released in the reaction catalyzed by glutamate dehydrogenase (GDH) (Figure 6). This oxidative step uses NAD cofactor and due to the release of ammonia the nitrogen is eliminated from the amino acid pool. The glutamate dehydrogenase catalyzed reaction is reversible in vitro and is shifted towards the production of ammonia in vivo. In the reversed reaction glutamate is released and NADPH is used as cofactor. 7 Figure 6. Trans-deamination. 1.2.2.4 The glucose-alanine cycle Glucose-alanine cycle has key role in the amino acid transport between different tissues. This cycle works between the liver and the muscle. The glucose-alanine cycle provides substrate for the muscle by the help of gluconeogenesis. Muscle has high transamination capacity, because the pyruvate (produced by the glycolysis) is converted to alanine by transamination. Produced alanine is transported to the liver by the bloodstream, where it is converted back to pyruvate by a repeated transamination reaction. Pyruvate is a substrate for gluconeogenesis, and its conversion to glucose provides energy source for the muscle, it is transported to the muscle by the bloodstream (Figure 7). However, NADH is released during the conversion of glucose to pyruvate, this NADH is not used for the conversion of pyruvate to lactate (in case of normoxia), because this reaction would deplete the pyruvate and the pyruvate would not be able to enter the transamination reaction and would not be converted alanine. In case of relative hypoxia (for example in case of extensive physical activity) the tissue does not completely oxidize glucose to water and CO2, therefore, elevated amount of lactate is produced due to the anaerob glycolysis. 8 Figure 7. The glucose-alanine cycle. 1.2.2.5 Urea synthesis Nitrogen is provided for the urea synthesis not only by deamination reactions but by transamination reactions. In this way both nitrogens of urea could come from glutamate amino nitrogen. The aspartate required for urea synthesis is released by a transamination reaction. The ammonia released in the glutamate dehydrogenase (GDH) catalyzed reaction is used in the preparatory step of urea cycle by carbamoyl phosphate synthase I (CPS I) for the synthesis of carbamoyl-phosphate. The aspartate entering the urea cycle is produced by the conversion of oxaloacetate to glutamate (transaminase reaction), therefore, there is a strong connection between the urea cycle and citric acid cycle (Figure 8). Figure 8. Connection between urea cycle and citric acid cycle. 9 1.2.2.6 Conversions of amino acids Commonly the degradation of amino acids is started with transamination, in which reaction the glutamate-α-ketoglutarate amino acid-keto acid pair is involved. With the exception of lysine and threonine transaminases exists for all amino acids. If it is necessary, the synthesis of non-essential amino acids can be carried out by aminotransferase catalyzed reactions. In this case an α-keto acid is used as precursor and an amino group is transferred. The transaminase reactions of essential amino acids have only one direction, because the equivalent α-keto acids cannot be synthesized in humans. 1.2.3 Clinical correlations The number of metabolic diseases caused by of transaminase deficiencies is small, possibly beause the complete lack of transaminase activity is not compatible with life. For example, degradation of valine and isoleucine starts with transamination. Enzymopathies of these enzymes are known and lead to hypervalinaemia, hyperleucine-isoleucinaemia. Transaminases have high diagnostic value, because the serum level of transaminases gives important information from the viewpoint of diagnosis. Transaminases are intracellular enzymes, therefore, their concentration in serum is low. Normal value of glutamate-oxaloacetate-transaminase (GOT) enzyme in serum is 60-260 nkat/l (3.8-15.8 U/l), while normal value of glutamate-pyruvate-transaminase (GPT) is 8-290 nkat/l (0.5-17.3 U/l). Tissue lesions (e.g. cell necrosis, changes of membrame permeability, etc.) lead to increase in serum concentration of the enzymes. Heart muscle tissue contains highest amount of GOT, while liver contains highest amount of GPT. Measurement of transaminases is important in the diagnosis of injury of heart muscle or liver. Serum GOT activity increases 4-6 hours after heart infraction, reaches the maximum after ~24 hours (could reach 1700 nkat/l). This value decreases until it reaches the normal value, which takes approximately 7 days. During this period the GPT activity is constant. Serum GPT activity increases mainly after the damage of liver cells, high serum level can be measured in case of infectious liver lesions. Increased GPT activity can be measured after heart infraction due to the impaired blood supply and damage of liver cells. 1.3 Reactions of amino acids: phenylalanine and tyrosine Degradation of phenylalanine and tyrosine occurs mainly in the liver. The major pathway of the degradation is started with a monooxigenase reaction leading to the conversion of phenylalanine to tyrosine (Figure 9). 10 There is a minor pathway of the phenylalanine degradation starting with a transamination reaction, but the capacity of this enzyme is low. Minor pathways have relevance in case of high phenylalanine concentration. In this case the phenylalanine is converted to phenylpyruvate by transamination. Further minor pathway is the conversion to phenyllactate or phenylacetate (see later) (Figure 11). Phenylalanine hydroxylase catalyzed reaction is monooxigenation, where one atom of molecular oxygen forms hydroxyl group of the substrate while the other forms water with the hydrogens of the cofactor. This reaction releases tyrosine. From this step the phenylalanine and tyrosine has the same metabolism (Figure 9). Figure 9. Conversion of phenylalanine and tyrosine to homogentisate. The phenylalanine hydroxylase catalyzed monooxigenation requires oxigent and tetrahydrobiopterin (BH4) as cofactor. Tetrahydrobiopterin is synthesized from GTP precursor by GTP cyclohydrolase I. BH4 is oxidized to dihydrobiopterin (BH2) in the phenylalanine hydroxylase catalyzed reaction. BH2 could be reduced to BH4 by dihydrobiopterin reductase (Figure 10). Figure 10. Reaction catalyzed by dihydrobiopterin reductase. Second step of the major phenylalanine and tyrosine degradation pathway is the conversion of tyrosine to p-hydroxyphenylpyruvate, together with the conversion of α-ketoglutarate to glutamate (Figure 9). The p-hydroxyphenylpyruvate is converted to homogentisate by the dyoxigenase enzyme. In the following steps acetoacetate and fumarate is produced from homogentisate. 1.3.1 Phenylketonuria and possible causes 11 Phenylalanine and tyrosine have several precursor functions. They are important precursors of the neurotransmitter (catecholamines: dopamine, norepinephrine, epinephrine) and thyroxine synthesis. Tyrosinase converts tyrosine to dopa, which product is used in melanine (pigment) synthesis. The most common disease which affects the amino acid metabolism is phenylketonuria. Deficiencies affecting the metabolism of phenylalanine and tyrosine lead to the development of different metabolic disorders, for example the impaired tyrosine synthesis leads to reduced catecholamine synthesis and melanine production. 1.3.1.1 Classical phenylketonuria - phenylalanine hydroxylase deficiency The consequence of mutation of the phenylalanine hydroxylase gene is the phenylketonuria (PKU). It is an inherited autosomal recessive disorder in which phenylalanine-tyrosine conversion is impaired. The consequence of the enzyme deficiency is the accumulation of the phenylalanine, because it cannot be converted tyrosine. Deficiency of phenylalanine hydroxylase enzyme leads classical phenylketonuria. PKU can be characterized by high serum concentration of phenylalanine. Main symptom of the disease is the lighter skin color due to the impaired melanine synthesis and mental retardation. Early diagnosis of PKU is very important, because in case of the recognized PKU a strict diet could be applied, which contains sufficient amount of essential amino acids and very low concentration of phenylalanine. This therapy can be applied efficiently, and in this way the development of serious symptoms (including mental retardation) can be avoided. Phenylketonuria screening of newborn babies is compulsory in Hungary. 1.3.1.2 Cofactor deficiency - dihydrobiopterin reductase deficiency In contrast with classical phenylketonuria, 3% of PKU cases is caused by cofactor deficiency. In the case of cofactor deficiency the phenylalanine hydroxylase reaction is affected, and phenylalanine cannot be converted to tyrosine, because this monooxigenation reaction requires tetrahydrobiopterin cofactor. The accumulated phenylalanine is converted phenylpyruvate by a transaminase (along with the conversion of pyruvate to alanine) (Figure 11). 12 Figure 11. Production of phenylpyruvate, phenyllactate and phenylacetate. Phenylpyruvate can be further converted to phenyllactate ot phenylacetate (Figure 11), their accumulation could affect the central nervous system and causes severe symptoms. These molecules lead to the loss of the myelin coat of neurons causing mental retardation in case of cofactor deficiency, as well. The cofactor deficiency could affect not only the phenylalanine degradation but other synthetic pathways (e.g. dopamine). Urine sample of healthy persons contain only small amount of these metabolites, but high concentration can be detected in the urine of PKU patients. Characteristic symptom of this disease is the mousy odor of urine. Phenylalanine is toxic for neurons and this effect is responsible for the mental retardation, furthermore, the aromatic amino acid uptake of neurons is inhibited due to the high phenylalanine concentration. In the case of cofactor deficiency the therapy also involves synthetic diet low in phenylalanine. In case of biopterin deficiency treatment includes the administration of biopterin. Deficiency of reductase causes more severe symptoms, the impaired catecholamine and serotonin synthesis is responsible for the neurological symptoms. 1.3.1.3 Maternal phenylketonuria Even if the neonate is a heterozygote, high phenylalanine concentration in the mother's blood causes severe mental retardation and heart problems of the fetus. 1.3.1.4 Tyrosine aminotransferase deficiency 13 Rare but severe disease. Tyrosinaemia and mental retardation. Besides the neurological symptoms the eye is also affected, skin lesions also develop. The “cabbage" odor smell is characteristic for this disease. 1.3.1.5 Enzyme deficiencies of the BH4 synthesis In very rare cases the synthesis of the cofactor from GTP may also be affected due to the deficiency of one of the enzymes catalyzing the process. 1.4. Theoretical background of practices: 1.4.1 Study of reversibility of transaminase-reaction Amino acids are detected using ninhydrin reaction. Ninhydrin reaction is positive for every αamino acid. Ninhydrin reagent reacts with the terminal amino group, followed by the condensation of the ammonia (released from α-amino acids) with the ninhydrin, and a purple coloured product is formed (Figure 12). Figure 12. Detection of amino acids by ninhydrin reaction. 1.4.2 Determination of serum GOT and GPT activity by optical test Wartburg optical test is used in the practice to determine the serum activity of glutamateoxaloacetate-transaminase (GOT) and glutamate-pyruvate-transaminase (GPT) aktivitásának (Figure 13). 14 Figure 13. GOT and GPT catalyzed reactions. The Warburg optical test was described by Warburg at 1936. This colorimetric measurement is based on the different absorption properties of NAD+ (NADP+) and NADH (NADPH). The change of the NADH or NADPH concentration can be measured at 366 nm wavelength by this colorimetric method, because only the reduced forms of the cofactors absorb, the oxidized forms hardly show any absorbance around this wavelength (Figure 14). Change of the absorbance is measured in a 340-366 nm wavelength range, therefore, the test is referred as UV-test. This test is a useful method for enzyme activity measurements. Figure 14. Absorption of NAD+ (NADP+) and NADH (NADPH) at different wavelengths. This UV-test is used in the practice to determine GOT and GPT activities. But the activities of these enzymes cannot be determined directly, because there is no net NAD+ or NADH release or production in the catalyzed reaction. A coupled optical test must to be applied for the activity 15 measurement, which means that the transaminase reaction (reaction of interest) must to be completed with a second reaction (indicator reaction), in which NADH (or NADPH) is used or released by an auxiliary enzyme. In the GOT catalyzed reaction aspartate and α-ketoglutarate substrates are converted to glutamate and oxaloacetate products. This reaction is followed by the conversion of oxaloacetate to malate in the malate dehydrogenase (MDH) auxiliary enzyme catalyzed indicator reaction, followed by the release of NAD+ (Figure 15). The decrease of the absorbance is measured, because the MDH uses NADH, therefore, decrease of NADH concentration leads to decrease of absorbance measured at 366 nm. Based on the Lambert-Beer law the absorbance can be used to calculate the concentration of molecule absorbing light. A=Ɛ*c*l A Ɛ c l - absorbance - molar extinction coefficient - concentration of molecule absorbing light - length of way of light Figure 15. Reactions of coupled optical test used for GOT activity measurement. In the GPT catalyzed reaction alanine and α-ketoglutarate substrates are converted to glutamate and pyruvate products. This reaction is followed by the conversion of pyruvate to lactate in the lactate dehydrogenase (MDH) catalyzed indicator reaction, followed by the release of NAD+ (Figure 16). 16 Figure 16. Reactions of coupled optical test used for GPT activity measurement. To make the reaction of interest to be the rate-limiting step of the coupled reaction, the excess of MDH and LDH auxiliary enzymes must to applied. The enzyme activities can be calculated based on the change of the absorbance. One katal is the amount of enzyme that converts 1 mol substrate per second, while one unit (U) is the amount of enzyme that catalyzes the reaction of 1 µmol substrate per minute. 1.4.3 Study of reactions of amino acid: phenylketonuria. Determination of amino acid composition of serum and urine by thin-layer ion-exchange chromatography Thin-layer chromatography is a simple and fast analytical method, which is useful to examine amino acids, short peptides, antibiotics, etc. Therefore, this method can be applied to determine the amino acid composition of serum and urine. Thin-layer chromatography is used in the laboratory practice to study a metabolic disease. The Polygram (Ionex-25 SA-Na) is a cation-exchanger thin-layer carried by plastic foil. The ion exchange resin is prepared from polyacrylamide carrying sulfate groups, the counter ions are Na+. The effectiveness of the separation of amino acids depends on the pH and ionic strength of the buffer system. We use sodium citrate buffer, pH 5.28, which separates basic and aromatic amino acids effectively. The amino acids are separated according to their positive charges depending on the number and pK value of their -NH groups. Use micropipette to apply the samples onto the thin-layer plate. Use pencil to indicate a start-line approximately 1 cm from the bottom of the plate. Apply the samples onto the start line. Use hair dryer during this process, to make as small sample spots as it is possible to avoid the contact of the spots and the mixture of samples. After drying the spots place the thin-layer plate into the chromatography tank containing developing buffer. Do not let the sample spots to sink into the 17 buffer! The buffer will run on the plate due to the capillary effect. Let the buffer run to 1 cm from the top of the plate, after it the plate need to be dried again by hair dryer. To develop the colors, the plate need to be sprayed by the ninhydrin reagents and dried again by hair dryer. Results can be evaluated based on the running distance of the sample spot, if it is necessary, the diameter of spots can be also determined. 18 Self-control questions 1. How transamination reactions are involved in the mitochondrial transport of reduced electron carriers produced in the cytosol? 2. How transamination reactions are involved in the glucose-alanine cycle? 3. What would be your diagnosis if the serum concentration of GOT (glutamate-oxaloacetatetransaminase) would be higher then 260 nkat/l? 4. What would be your diagnosis if the serum concentration of GPT (glutamate-oxaloacetatetransaminase) would be higher then 290 nkat/l? 5. What is the difference between the classical phenylketonuria and the cofactor deficiency? 19 REFERENCES 1. Biochemistry and molecular biology. II. Metabolism. Third edition. Debrecen, 2001.Edited by László Fésüs. Written by: János Aradi, László Fésüs, Mária Punyiczki, Balázs Sümegi, Zsuzsa Szondy and Tőzsér József. 2. Orvosi biokémia. Edited by: Ádám Veronika. Second edition. Budapest, 2002. Medicina Könyvkiadó Rt. 3. Textbook of Biochemistry with clinical correlations. Fifth edition. Edited by: Thomas M. Devlin, Wiley-Liss, 2002. 4. Biochemistry practical guide. Reprint of edition of 2010. Edited by Farkas Teichmann. University of Debrecen, Faculty of Medicine, Department of Biochemistry and Molecular Biology. Debrecen University Press, 2014. 5. Homepage of the Nomenclature Committee of the International Union of Biochemistry and Molecular Biology (NC-IUBMB) URL: http://www.chem.qmul.ac.uk/iubmb/enzyme 20