* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Understanding Genetic Cancer Risk: BRCA1 and 2
Survey
Document related concepts
Gene expression profiling wikipedia , lookup
Biology and consumer behaviour wikipedia , lookup
Genetic testing wikipedia , lookup
Gene expression programming wikipedia , lookup
Polycomb Group Proteins and Cancer wikipedia , lookup
Population genetics wikipedia , lookup
Genome evolution wikipedia , lookup
Designer baby wikipedia , lookup
Frameshift mutation wikipedia , lookup
Cancer epigenetics wikipedia , lookup
Public health genomics wikipedia , lookup
Point mutation wikipedia , lookup
Nutriepigenomics wikipedia , lookup
Microevolution wikipedia , lookup
Genome (book) wikipedia , lookup
Transcript
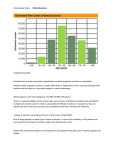
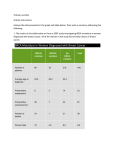
Page 1 of 4 Understanding Genetic Cancer Risk: BRCA1 and 2 Genetic cancer risk BRCA1 and BRCA2 genes About 5 to 10 out of 100 cancers are due to an inherited gene. A family with these genes often has: • The same type of cancer in more than one person. • Cancers found at a young age (before age 50). • People with more than one cancer. • Cancer in two or more generations. The tables show the chance of getting cancer over a lifetime. It compares a group with normal BRCA genes and a group with a BRCA mutation. Having a mutation does not mean you will develop cancer. But your risk is much greater. For example, out of 100 women with a BRCA mutation, 40 to 80 will get breast cancer. We each inherit two copies of every gene in our bodies: one from our mother and one from our father. Each gene has a specific job to do. When a gene has a mistake or “mutation,” it does not work like it should. Everyone has two copies of BRCA1 and two copies of BRCA2. A single mistake in one of the copies increases the risk for cancer of the breast and ovaries. The risk for pancreatic cancer and melanoma may also increase slightly in some families. A person’s ethnic background also plays a role. For example, people of Ashkenazi Jewish origins have a higher chance of having a BRCA gene mutation. Women In general with BRCA mutation Breast cancer 12 out of 100 40-80 out of 100 Ovarian cancer 1-2 out of 100 10-40 out of 100 Men In general with BRCA mutation Breast cancer less than 1 in 100 7 out of 100 Prostate cancer 16 out of 100 20 out of 100 If you are deaf or hard of hearing, please let us know. We provide many free services including sign language interpreters, oral interpreters, TTYs, telephone amplifiers, note takers and written materials. Page 2 of 4 Inheritance Advantages to testing When a parent has a BRCA mutation, each child has a 1 in 2 chance they will inherit the mutation. Therefore, each child has a 1 in 2 chance of being at increased risk for having cancer. The results may • clarify your cancer risk. • help you make medical decisions. • explain the cancers in your family. • give useful information to your family (if you share your results). Disadvantages to testing Dad = affected 1 gene mutation Mom = not affected normal genes The results may • cause you to feel sad, angry or upset on learning about a cancer risk. Affected 1 gene mutation Not affected normal genes Not affected normal genes Affected 1 gene mutation Genetic testing Genetic testing involves a simple blood test. The test looks in the BRCA1 and BRCA2 genes for any changes that are linked to cancer risk. If possible, the person who has had cancer should be tested before other family members. This helps us see whether or not a gene is linked with the cancer in the family. Results There are three possible results of testing: • We may find a harmful mutation (positive). • We may find no mutation (negative). • We may find a change in one of the genes, but it is unclear how this affects family cancer risk (change of unknown importance). • leave you confused about the meaning of a test result. • lead to concerns about discrimination (see below). Genetic Information Nondiscrimination Act (GINA) GINA is a federal law that protects people from discrimination based on a genetic test result. The law protects your rights to health insurance and employment. To learn more, visit the National Human Genome Research Institute at: www. genome.gov/10002077. Page 3 of 4 Reducing inherited cancer risk Screenings for women with a BRCA mutation: Breast • Age 18: Begin breast self-exams monthly. • Age 25: Begin breast exams in clinic every 6 to 12 months. • Age 25 (or younger): Begin yearly breast MRI. • Age 30: Begin yearly mammogram in addition to breast MRI. Alternate these exams every 6 months. • Consider preventive chemotherapy or preventative mastectomy. Questions to ask yourself • If I have a gene mutation, how will the test result affect me and my family? If I don’t have a gene mutation? • Should I share my test results? How will my family react to this news, which may also affect them? • Are my children ready to learn new information that may one day affect their own health? Resources FORCE: Facing Our Risk of Cancer Empowered www.facingourrisk.org Bright Pink: www.bebrightpink.org Ovarian American Cancer Society (ACS): www.cancer.org • At age 30 (or younger): Consider ultrasound and CA-125 blood test every 6 months. National Cancer Institute (NCI): www.cancer.gov • By ages 35-40 (or after child bearing): Consider removing the ovaries and fallopian tubes. Screenings for men with a BRCA mutation: • Age 35: Self-breast exams training and education • Age 35: Start breast exams in clinic, every 12 months. • Age 40: BRCA2 carriers begin prostate cancer screening • Age 40: BRCA1 carriers consider prostate cancer screening Both men and women should talk to their doctor or genetic counselor about screening for pancreatic cancer and melanoma. Please call us if you have any questions or concerns. Cancer Risk Management Program 612-626-9898 Appointment Scheduling 1-855-4-UMP-CANCER (1-855-486-7226) Page 4 of 4 www.fairview.org For informational purposes only. Not to replace the advice of your health care provider. Copyright © 2014 Fairview Health Services. All rights reserved. SMARTworks 521837– REV 04/15.