* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download endocrine system - Crestwood Local Schools
Immunocontraception wikipedia , lookup
Rheumatic fever wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Social immunity wikipedia , lookup
Gluten immunochemistry wikipedia , lookup
Monoclonal antibody wikipedia , lookup
DNA vaccination wikipedia , lookup
Herd immunity wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Vaccination wikipedia , lookup
Schistosoma mansoni wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Globalization and disease wikipedia , lookup
Autoimmunity wikipedia , lookup
Germ theory of disease wikipedia , lookup
Immune system wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Adaptive immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Innate immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
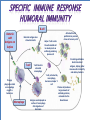
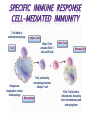
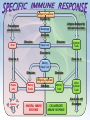
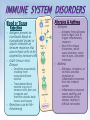
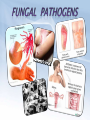
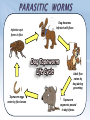
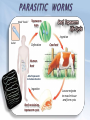
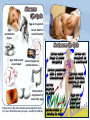
• Protection against infection & disease SELF vs. NONSELF • Self • Body recognizes molecules (MHC proteins) in plasma membrane as a label of “self” • Non-self • Unfamiliar antigens are not recognized and stimulate reaction from immune system Second Line of Defense • • Non-specific Defensive cells • • • • Proteins • • • Phagocytes (Neutrophils & Macrophages) Eosinophils Natural Killer Cells Interferons Complement system Inflammatory Response Inflammatory Response • • • • Non-specific! Small, mobile connective tissue cells called Mast Cells release histamines in response to chemicals from damaged cells, causing “inflamed” look beneath skin Histamines make blood vessels dilate, causing redness, swelling, heat & pain If infection is severe or spreads, fever & stronger immune response can result Humoral (Antibody-Mediated) Immunity • Primarily defends against extracellular pathogens or toxins B-cell Bacteria with Antigens on Surface Bacterial antigens also stimulate B-cells T-cell A large phagocyte called a macrophage engulfs a bacterium Macrophage T-cell binds to activated macrophage Helper T-cell assists the activated B-cell to develop into an antibody-producing plasma cell Activated B-cells proliferate to produce clones of memory cells Circulating antibodies bind to bacterial antigens, helping other immune cells to identify and destroy bacteria T-cell, activated by macrophage, becomes a Helper Tcell Plasma cell produces large amounts of antibody proteins, released into the bloodstream Antigens are displayed on surface of macrophage after digestion of bacterium T-cell binds to activated macrophage Helper T-cell Helper T-cell activates Killer Tcells and B-cells T-cell Antigens are displayed on surface of macrophage Killer T-cell Infected Cell T-cell, activated by macrophage becomes a Helper T-cell Macrophage Killer T-cells bind to infected cells, disrupting their cell membranes and destroying them Artificial Immunity • • Antibodies are introduced into the body by nonnatural processes (i.e. injections) Requires intentional actions ACTIVE • NATURAL • • ARTIFICIAL • Due to a specific immune response in the body, a survivor of a disease is permanently immune to a recurrence of that disease. Example: Measles Vaccination for a disease causes a specific immune response in the body, resulting in permanent immunity to that disease. Example: Polio PASSIVE • Newborn infant gets antibodies from its mother, providing temporary immunity to diseases that the mother had an active immunity to. • Injection of antibodies for a disease (produced by another source) provides temporary immunity to the disease Example: Rabies • ACTIVE • NATURAL • • ARTIFICIAL • Due to a specific immune response in the body, a survivor of a disease is permanently immune to a recurrence of that disease. Example: Measles Vaccination for a disease causes a specific immune response in the body, resulting in permanent immunity to that disease. Example: Polio PASSIVE • Newborn infant gets antibodies from its mother, providing temporary immunity to diseases that the mother had an active immunity to. • Injection of antibodies for a disease (produced by another source) provides temporary immunity to the disease Example: Rabies • Antigen (1st exposure) Engulfed by Free antigens directly activate Antigens displayed by infected cells activate Macrophage Stimulates B-cell Stimulates Helper T-cell Stimulates Cytotoxic T-cells Gives rise to Gives rise to Gives rise to Memory Helper T-cell Stimulates Stimulates Antigen (2nd exposure) Plasma cells Antibodies Memory B-cells Stimulates HUMORAL IMMUNE RESPONSE Memory T-cells CELL-MEDIATED IMMUNE RESPONSE Active Cytotoxic T-cells Attack cells with this antigen Blood or Tissue Rejection – Antigens present on transfused blood or transplanted tissues or organs stimulate an immune response that causes those cells to be targeted by immune cells – Graft-Versus-Host Disease – Condition occasionally resulting from transplanted bone marrow – Transplanted bone marrow (source of immune cells) does not recognize and therefore attacks body tissues and organs – Rejections can be life- threatening Allergies & Asthma – Allergies – Antigens from allergens bind to Mast Cells & trigger inflammatory response – Mast Cells release histamines, which cause sneezing, runny nose & eyes, and other irritations – Asthma – Allergens, irritations, or stressful activities stimulate an inflammatory response from the immune system – Inflammatory response causes swelling and constriction of the airways, making it difficult to breathe Immune Deficiency Diseases • Primary • Secondary – A genetic (inherited) condition that compromises the immune system’s ability to fight off infection – Example: Severe Combined Immunodeficiency • Aka “Bubble Boy” disease • Genetic mutation disables immune system and leaves child susceptible to any infection • Bone marrow transplant is the only known cure • Without treatment, patients die in early childhood – Aka “Acquired” – Compromised immune function due to infection or disease – Not genetic – Example: HIV/AIDS What is a microbe? – Tiny! – Cannot be seen with the naked eye. – Domain Archaea – Domain Eubacteria – Domain Eukarya – – – – Protists Fungi Plants Animals Shapes • • • Cocci: sphere-shaped Bacilli: rod-shaped Spirilla: spiral-shaped Autotrophs • Photoautotrophic • • • Photosynthetic (energy from sun & carbon from CO2) Often found on surface of water Cyanobacteria (formerly known as “bluegreen algae”) • • • Found in fresh and salt water and on land Some can survive in extreme environments Often the first species to recolonize natural disaster sites (i.e. volcanic eruption) • Chemoautotrophic • • • Obtain energy directly from inorganic molecules, such as iron-, sulfur- or nitrogen-based compounds Basis of the only known ecosystems that are not dependent on sunlight Example – Deep ocean vents Bacteria as Pathogens – Bacteria can cause disease in two ways – Directly infecting body tissues (i.e. H. pylori) – Producing toxins (i.e. Clostridium botulinum) Terminology – Disease – Any change, other than an injury, which interferes with the normal functioning of the body – Pathogen – Disease-causing microorganism – Infection – Disease caused by a pathogen Specificity – Viruses only infect particular cell types – May infect multiple species – May only infect one particular species – May only infect one cell type within that species Characteristics – Non-cellular particle made up of genetic material inside a protein coat – Obligate intracellular parasite – activities associated with life only occur when virus invades a host organism’s cell – ARE VIRUSES ALIVE???? Structure & Shape • • • Nucleic acid core composed of either DNA or RNA Protein coat (capsid) surrounds genetic material Viruses come in many shapes & sizes Entry Attachment Replication Assembly Lysis Prion Diseases Creutzfeldt-Jakob disease – “Mad Cow” disease – Infection from eating contaminated food Fatal Familial Insomnia – Autosomal dominant – Onset between 35 & 60 Kuru – Infection caused by eating infected human brain tissue – Found almost exclusively in New Guinea among people who practice a form of cannibalism as part of a funeral ritual. Gerstmann-Straussler syndrome – Almost always inherited (autosomal dominant) – Onset between 20 & 55 Prion Diseases Creutzfeldt-Jakob disease – “Mad Cow” disease – Infection from eating contaminated food Fatal Familial Insomnia – Autosomal dominant – Onset between 35 & 60 Kuru – Infection caused by eating infected human brain tissue – Found almost exclusively in New Guinea among people who practice a form of cannibalism as part of a funeral ritual. Gerstmann-Straussler syndrome – Almost always inherited Normal (autosomal dominant) – Onset between 20 & 55 Protein Fungi • Single or multicellular • Eukaryotic • Cause disease by “digesting” host cells Parasitic Protists – Often have complex life-cycles involving more than one host – Examples: – Trypanosoma (African Sleeping Sickness) – Giardia (intestinal parasite) – Entamoeba histolytica (Amoebic Dysentery) – Certain diatoms (“Red tides”) Parasitic Protists – Often have complex life-cycles involving more than one host – Examples: – Trypanosoma (African Sleeping Sickness) – Giardia (intestinal parasite) – Entamoeba histolytica (Amoebic Dysentery) – Certain diatoms (“Red tides”) – Toxoplasma gondii (toxoplasmosis) – Plasmodium falciparum (malaria) Flatworms Flukes (parasitic) Tapeworms (parasitic) Infective cyst forms in flea Dog becomes infested with fleas Adult flea eaten by dog during grooming Tapeworm eggs eaten by flea larvae Tapeworm segments passed in dog’s feces. Head “hooks” Tapeworm eggs Ingestion Sucker Defecation Cow host Human host Adult tapeworm in human intestine Ingestion Beef containing tapeworm cysts Larvae migrate to muscle tissue and form cysts Flatworms Flukes (parasitic) Tapeworms (parasitic) Nematodes Ascarid worms (heartworm) Hookworms Filarial worms Pinworms Heartworm Pinworm Eggs are ingested Eggs contaminate fingers Larvae hatch in small intestine Eggs embryonate Larvae migrate to on perianum colon & mature Larvae enter lungs & cause coughing Larvae penetrate skin & enter bloodstream Gravid adults migrate out of anus & lay eggs Pinworms are the most common worm infection in the U.S. (over 40 million cases per year—usually in children). Larvae migrate to grass Larvae hatch & develop in soil Larvae are coughed up & swallowed Larvae reach small intestine, mature, & start feeding Eggs are passed in feces and enter soil Flatworms Flukes (parasitic) Tapeworms (parasitic) Nematodes Ascarid worms (heartworm) Hookworms Pinworms Filarial worms Segmented worms Leeches