* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 02 Cardiac Anatomy
Survey
Document related concepts
History of invasive and interventional cardiology wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Artificial heart valve wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
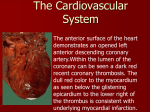
Essential Cardiac Anatomy and Physiology Tobias Schaeffter Division of Imaging Sciences and Biomedical Engineering King’s College London Learning objectives • Provide an overview on Heart Anatomy, Conducting System and Physiology • Provide terminology of the external and internal features of the heart • Show imaging examples of cardiac anatomy and physiology Heart Anatomy • Approximately the size of your fist – Weight = 250-300 grams • Location – In the mediastinum between the lungs – Superior surface of diaphragm – ⅔ of it to the left of midsternal line Anatomical Features of the Heart • Muscular organ with 4 internal chambers – 2 atria (lt. atrium & rt. atrium)receive blood from veins – 2 ventricles (lt. ventricle & rt. ventricle)pump blood into arteries • Superior aspect of heart is the “base”, where the blood vessels attach; • Inferior is the “apex”, which rests on the relaxed diaphragm Coverings of the Heart • Pericardium – a double-walled sac around the heart • Fibrous pericardium (pericardial sac) – outer layer that protects & anchors • Serous pericardium – double layered membrane with “pericardial fluid” – Protects and anchors the heart – Allows for the heart to work relatively friction-free Layers of the Heart Wall • Epicardium – visceral pericardium • Myocardium – cardiac muscle layer forming the bulk of the heart • Endocardium – endothelial layer of the inner myocardial surface Layers of Heart Wall § Epicardium (a.k.a. visceral pericardium) § Myocardium § Endocardium Cardiac muscle tissue • Cardiac muscle consists of heart muscle cells (cardiomyocytes) which are connected by intercalated discs to work as one functional organ • Intercalated discs support synchronised contraction of cardiac tissue. MR-DTI Heart Anatomy • External markings – Apex - pointed inferior region – Base - upper region – Coronary sulcus (feature that separates atria from ventricles) – Anterior and posterior interventricular sulcus (feature that separates right and left ventricles) • Internal divisions – Atria (superior) and ventricles (inferior) – Interventricular and interatrial septa Cardiac CT External Features § Auricles § Coronary sulcus – contains the coronary sinus § Anterior interventricular sulcus – contains coronary vessels § Posterior interventricular sulcus – contains coronary vessels Atria of the Heart • Atria - receiving chambers of the heart – Receive venous blood returning to heart – Separated by an interatrial septum (wall) • Fossa ovalis - remnant of foramen ovale (opening in interatrial septum in fetus) • Pectinate muscles mark atrial walls • Pump blood into ventricles • Blood enters right atria from superior and inferior venae cavae and coronary sinus • Blood enters left atria from pulmonary veins Internal Structures Cardiac MR SVC Interatrial septum Fossa ovalis Lt Atrium Rt Atrium Pectinate muscles Bicuspid (mitral) valve Coronary sinus (opening) Chordae tendineae Tricuspid valve Chordae tendineae Papillary muscle Papillary muscle IVC Deoxygenated blood Pulmonary veins Oxygenated blood Internal Structures Cardiac MR Ventricles of the Heart • Ventricles are the pumping chambers of the heart • Papillary muscles and trabeculae carneae muscles mark ventricular walls • Separated by an interventricular septum – Contains components of the conduction system • Right ventricle pumps blood into the pulmonary trunk • Left ventricle pumps blood into the aorta – 3xThicker myocardium due to greater work load • Pulmonary circulation supplied by right ventricle is a much low pressure system requiring less energy • Systemic circulation supplied by left ventricle is a higher pressure system and thus requires more forceful contractions Heart Valves • Heart valves ensure unidirectional blood flow through the heart • Two major types – Atrioventricular valves – Semilunar valves • Atrioventricular (AV) valves lie between the atria and the ventricles – R-AV valve = tricuspid valve – L-AV valve = bicuspid or mitral valve • AV valves prevent backflow of blood into the atria when ventricles contract • Chordae tendineae anchor AV valves to papillary muscles of ventricle wall – Prevent prolapse of valve back into atrium Fibrous Skeleton • Surrounds all four valves – Composed of dense connective tissue • Functions – Anchors valve cusps – Prevents overdilation of valve openings – Main point of insertion for cardiac muscle – Blocks direct spread of electrical impulses Aorta (ascending) Pulmonary artery Pulmonary trunk Pulmonary semilunar valve Aortic semilunar valve Trabeculae carneae Lt ventricle Rt ventricle Interventricular septum Atrioventricular Valve Function Semilunar Valve Function Semilunar Heart Valves • Semilunar valves prevent backflow of blood into the ventricles • Have no chordae tendinae attachments • Aortic semilunar valve lies between the left ventricle and the aorta • Pulmonary semilunar valve lies between the right ventricle and pulmonary trunk Atrioventricular (AV) valves § Tricuspid § Bicuspid Semilunar valves Heart Valves Cardiac US 3D reconstruction of the heart. To the left 2D US-images from the same dataset, showing tricuspid and mitral valves (above) and aortal and mitral valve (below) (source Wikipedia) Heart sounds (“lub-dup”) due to valves closing “Lub” - closing of atrioventricular valves “Dub”- closing of semilunar valves Heart Defects Conducting System • Cardiac muscle tissue has intrinsic ability to: – Generate and conduct impulses – Signal these cells to contract rhythmically • Conducting system – A series of specialized cardiac muscle cells – Sinoatrial (SA) node sets the inherent rate of contraction • “Autorhythmic (conducting) cells” – spontaneously generate action potentials Conducting System SA node (“pacemaker”) à à AV node à à AV bundle (of His) à à Bundle branches à à Purkinje fibers Innervation • Heart rate is altered by external controls • Nerves to the heart include: – Visceral sensory fibers – Parasympathetic branches of the vagus nerve – Sympathetic fibers – from cervical and upper thoracic chain ganglia Heart Excitation Related to ECG Figure 18.17 Electroanatomical Mapping Movement of blood through heart & heart sounds § The activity of the conduction system results in the contraction (systole) & relaxation (diastole) of the heart chambers § atria will contract as ventricles remain relaxed (atrial systole/ventricular diastole). Blood moves from atria to ventricles § as atria relax, ventricles begin to contract (atrial diastole/ventricular systole). The AV valves (tricuspid & bicuspid/mitral) close to prevent backflow of blood into atria. The closing of the valves makes a sound – “Lub” § as blood moves from ventricles to arteries (pulmonary trunk & aorta), pressure will increase in the arteries and decrease in the ventricles. Semilunar valves will then shut à “Dupp” as ventricles relax § all 4 chambers will be in diastole, and then cycle begins again Electrocardiography Cardiac Cycle • Cardiac cycle refers to all events associated with blood flow through the heart – Systole – contraction of heart muscle – Diastole – relaxation of heart muscle Phases of the Cardiac Cycle • Ventricular filling – Heart blood pressure is low as blood enters atria and flows into ventricles – AV valves are open, then atrial systole occurs Phases of the Cardiac Cycle • Ventricular systole – Atria relax – Rising ventricular pressure results in closing of AV valves – Isovolumetric contraction phase – Ventricular ejection phase opens semilunar valves Phases of the Cardiac Cycle • Isovolumetric relaxation – early diastole – Ventricles relax – Backflow of blood in aorta and pulmonary trunk closes semilunar valves • Dicrotic notch – brief rise in aortic pressure caused by backflow of blood rebounding off semilunar valves Phases of the Cardiac Cycle Pressure-Volume Loop Pressure-volume loop of left ventricle Cardiac Output (CO) and Reserve • CO is the amount of blood pumped by each ventricle in one minute • CO is the product of heart rate (HR) and stroke volume (SV) • HR is the number of heart beats per minute • SV is the amount of blood pumped out by a ventricle with each beat • Cardiac reserve is the difference between resting and maximal CO Cardiac Output: Example Left ventricular chamber assessment • CO (ml/min) = HR (75 beats/min) x SV (70 ml/beat) quantitativ e: discs contiguous stack of short axis slices Simpsons rule of • CO = 5250 ml/min (5.25 L/min) Short axis cine stack • p4CH • LV Volumes Papillary muscles: either SAX stack included or excluded in LV volumes (report to specify) • LVOT included in LV volume: the contour is drawn to include the outflow tract to the level of the aortic valve cusps. • The highest basal slice: can be identified when more than 50% of the blood volume is surrounded by myocardium every slice has a defined thickness (8mm) bbb= 0mm gap between the slices Regulation of Stroke Volume • SV = end diastolic volume (EDV) minus end systolic volume (ESV) • EDV = amount of blood collected in a ventricle during diastole • ESV = amount of blood remaining in a ventricle after contraction Factors Affecting Stroke Volume • Preload – amount ventricles are stretched by contained blood • Contractility – cardiac cell contractile force due to factors other than EDV • Afterload – back pressure exerted by blood in the large arteries leaving the heart Preload and Afterload Pressure-Volume Loop SYSTOLIC PRESSURE CURVE After-load Pre-load PRESSURE Isotonic (Ejection) Phase Isovolumetric Phase Stroke Volume DIASTOLIC PRESSURE CURVE End Systolic Volume End Diastolic Volume Extrinsic Factors Influencing Stroke Volume • Contractility is the increase in contractile strength, independent of stretch and EDV • Increase in contractility comes from: – Increased sympathetic stimuli – Certain hormones – Ca2+ and some drugs Major Vessels of the Heart • Vessels returning blood to the heart include: – Superior and inferior venae cavae • Open into the right atrium • Return deoxygenated blood from body cells – Coronary sinus • Opens into the right atrium • Returns deoxygenated blood from heart muscle (coronary veins) – Right and left pulmonary veins • Open into the left atrium • Return oxygenated blood from lungs Pathway of Blood Through the Heart and Lungs Blood Flow Through the Heart Major Vessels of the Heart Vessels conveying blood away from the heart include: – Pulmonary trunk • Carries deoxygenated blood from right ventricle to lungs • Splits into right and left pulmonary arteries – Ascending aorta • Carries oxygenated blood away from left atrium to body organs • Three major branches – Brachiocephalic – Left common carotid, – Left subclavian artery 4D MR-Flow Coronary Circulation • Coronary circulation – The functional blood supply to the heart muscle itself – R and L Coronary arteries are 1st branches off the ascending aorta – Coronary sinus (vein) empties into R. atrium • Collateral routes ensure blood delivery to heart even if major vessels are occluded Coronary Circulation - Arteries • Right Coronary Artery – Supplies blood to • Right atrium and posterior surface of both ventricles – Branches into the • Marginal artery - extends across surface of R. ventricle • Posterior interventricular artery • Left Coronary Artery – Supplies blood to • Left atrium and left ventricle – Branches into • Circumflex artery • Left Main Cardiac MRA Cardiac CTA Coronary Circulation: Arterial Supply Perfusion Data Courtesy S. Plein Stress PET/MR Rest Data Courtesy E. Nagel Coronary Circulation - Veins Coronary sinus: • Vein that empties into right atrium • Receives deoxygenated blood from: – Great cardiac vein - on anterior surface – Posterior cardiac vein • Drains area served by circumflex – Middle cardiac vein • Drains area served by posterior interventricular artery – Small cardiac vein • Drains blood from posterior surfaces of right atrium and ventricle Coronary Vein MRA Coronary Circulation: Venous Supply Learning objectives • Provide an overview on Heart Anatomy, Conducting System and Physiology • Provide terminology of the external and internal features of the heart • Show imaging examples of cardiac anatomy and physiology Readings • Achilles J. Pappano, Withrow Gil Wier, Matthew N. Levy; Cardiovascular Physiology; Mosby; 9th edition 2006 • Elaine N. Marieb, Essentials of Human Anatomy and Physiology, Pearson Education ; 10th edition 2010 • Lauralee Sherwood. Human Physiology: From Cells to Systems; Brooks Cole; 8th edition, 2012 • Robert F. Schmidt, Gerhard Thews, Human Physiology, Springer 1989 • Many slides from www.slideworld.org