* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
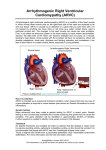
Download Arrhythmogenic right ventricular cardiomyopathy Is it right?
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Echocardiography wikipedia , lookup
Myocardial infarction wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
Linköping University Medical Dissertations No. 1257 Arrhythmogenic right ventricular cardiomyopathy Is it right? Meriam Åström Aneq Division of Cardiovascular Medicine Department of Medical and Health Sciences Linköping University, Sweden 1 Meriam Åström Aneq, 2011 Cover illustration drawn by Jasmine Åström Aneq Published article has been reprinted with the permission of the copyright holder. Printed in Sweden by LiU-Tryck, Linköping, Sweden, 2011 ISBN ISSN 978-91-7393-089-5 0345-0082 2 To Jasmine & Linda You do not know what you can miss before you try Franklin P. Adams 3 4 TABLE OF CONTENTS ABSTRACT .................................................................................................................. 9 POPULÄRVETENSKAPLIG SAMMANFATTNING ....................................... 11 LIST OF ORIGINAL PAPERS................................................................................ 15 ABBREVIATIONS .................................................................................................... 17 INTRODUCTION..................................................................................................... 19 ARRHYTHMOGENIC RIGHT VENTRICULAR CARDIOMYOPATHY .... 21 1. Etiology ............................................................................................................ 21 1:1 Molecular genetics .................................................................................. 21 1:2 Other possible pathogenic mechanisms .............................................. 23 2. Pathophysiology ............................................................................................. 23 3. Histopathology ............................................................................................... 24 4. Clinical features and imaging ..................................................................... 24 4:1 Clinical presentation ............................................................................... 25 4:2 Electrocardiography ............................................................................... 26 4:3 Exercise testing ........................................................................................ 28 4:4 Echocardiography ................................................................................... 28 4:5 Magnetic resonance imaging ................................................................ 29 4:6 Other modalities...................................................................................... 29 5. Differential diagnosis ................................................................................... 30 6. Natural history ................................................................................................ 31 7. Management of ARVC patients .................................................................. 31 7:1 Physical activity ...................................................................................... 31 7:2 Anti-arrhythmic pharmacological therapy ......................................... 32 5 7:3 Implantable cardioverter defibrillator (ICD) ...................................... 32 7:4 Evaluation of relatives ............................................................................ 32 AIM OF THE THESIS .............................................................................................. 35 STUDY POPULATIONS ......................................................................................... 37 METHODS ................................................................................................................. 39 1. Echocardiography .......................................................................................... 39 2. Magnetic resonance imaging ....................................................................... 42 3. Signal-averaged electrocardiogram ............................................................ 45 4. Genetic analysis ............................................................................................. 45 5. Reproducibility studies ................................................................................ 47 STATISTICS .............................................................................................................. 49 RESULTS .................................................................................................................... 51 GENERAL DISCUSSION ....................................................................................... 57 1. Aspects on right ventricular anatomy and physiology .......................... 57 2. Challenges in right ventricular imaging ................................................... 59 2.1 Echocardiography ................................................................................... 59 2.2 Magnetic resonance imaging ................................................................ 62 3. Signal- averaged electrocardiography in ARVC ...................................... 63 4. Genetics in ARVC .......................................................................................... 64 CONCLUSION .......................................................................................................... 67 IMPLICATIONS AND FUTURE PERSPECTIVES ............................................ 69 APPENDIX 1 .............................................................................................................. 71 ACKNOWLEDGEMENTS ...................................................................................... 79 6 REFERENCES ............................................................................................................ 83 7 8 Abstract ABSTRACT Arrhythmogenic right ventricular cardiomyopathy (ARVC) is an inherited uncommon heart disease, where sudden cardiac death in young seemingly healthy persons may be the first symptom. ARVC is probably more common than previously known, due to diagnostic difficulty. A combination of clinical findings and results from non-invasive as well as invasive investigations is used to diagnose the disease. However non-invasive visualisation of the right ventricle (RV), the predominantly affected part in ARVC, and assessment of its function have some limitations due to RV anatomy and function. The aim of this thesis is the evaluation of new non-invasive modalities in the assessment of right ventricular volume and function with focus on patients with ARVC. Clinical and non-invasive follow-up of fifteen patients with ARVC during a mean period of 8 years disclosed that progression of the disease is not uniform but generally "slow" in well controlled patients. However individual variation may occur. The determination of RV volume on magnetic resonance imaging relies on short axis (SA) views obtained as a spinoff from assessing short axis LV. These LV slices do not follow the curvature of the long axis of the RV and, segmentation of the inflow and outflow region of the RV is difficult in this view. A new axially rotated long axis acquisition (RLA) was tested and its feasibility in assessment of RV volume was evaluated. The RLA acquisition seems to be able to improve assessment of RV volume and function by reducing the uncertainty in defining the basal slice of the RV. A third study concentrates on analysis of RV regional and general function based on echocardiographic speckle tracking. Two dimensional (2D) longitudinal strain based on speckle tracking as well as tissue Doppler Imaging was used on patients with ARVC, their first degree relatives and in healthy subjects. 2D strain showed a good feasibility in the analysis of RV function in relatives and controls but less in ARVC patients probably due to the progressive myocardial cell death with fibro-fatty replacement of the RV wall. In order to detect and follow up echocardiographic changes in this patient category, an index was developed combining dimensional and functional parameters for the left and for the right ventricle. This index could 9 be used as a tool in the echocardiographic evaluation and serial assessment of RV function. Advances in the molecular genetics of ARVC have provided new insights into the understanding of the disease. Hitherto, 9 candidate genes have been identified. A new mutation in the plakophilin 2 gene was detected in a three generation family. The clinical phenotype related to this mutation was highly variable, from sudden cardiac death (SCD) or anatomical changes at an early age to non-penetrance. This suggested the need to include genetic testing as a part of the diagnostic work-up of ARVC patients and in relatives, to rule out mutation carriers. The studies have evaluated and developed methods for studying the right ventricle with special emphasis on ARVC. With the ultimate goal of preventing sudden death in ARVC, a combination of genetic testing and improved diagnostic methods may create an improved algorithm for risk stratification and selection to prophylactic treatment . 10 Summary in Swedish POPULÄRVETENSKAPLIG SAMMANFATTNING Plötslig död under ansträngning hos unga personer beror oftast på en dold hjärtsjukdom. Varje fall är en tragedi och innebär, förutom förlust av en ung människas liv, svåra konsekvenser för familj och omgivning. En orsak till plötslig död hos unga är en ärftlig hjärtsjukdom, arytmogen högerkammarkardiomyopati (ARVC), som medför att hjärtmuskelväggen omvandlas till fett- och bindväv vilket ger en benägenhet för rytmrubbningar som kan utlösas av fysisk ansträngning. Sjukdomen är svår att diagnostisera i tidiga stadier med de undersökningstekniker som finns, dels på grund av dess diskreta utbredning initialt, och pga. svårigheter att bedöma höger kammare, den mest drabbade delen av hjärtat vid ARVC. På senare år har 9 olika genetiska avvikelser kopplade till sjukdomen identifierats. Syftet med denna avhandling är att utveckla metoder för att förbättra känsligheten vid diagnostik av ARVC med bildgivande hjärtundersökningsmetoder och vid genetisk undersökning av patienter och anhöriga. Uppföljning av femton patienter med ARVC under en period på 6-10 år har visat att sjukdomsutvecklingen oftast är långsam, men individuella skillnader kan förekomma. Det har också noterats att vänster kammare drabbas tidigt i sjukdomsförloppet. Användning av magnetkameraundersökning för bedömning av höger kammare har visat sig ge värdefull tilläggsinformation. Beräkning av volymen baseras dock på tvärsnittsbilder som är framtagna för vänster kammare och tar mindre hänsyn till höger kammares annorlunda form och rörlighet. Detta försvårar avgränsningen av framförallt det översta (basala) snittet i höger kammare och ger en osäkrare volymberäkning. Vi har utvecklat ett nytt sätt att samla in bilderna genom att utgå från högerkammares längsgående axel mellan klaffen och hjärtspetsen. Bildinsamlingen sker från 6 roterande snitt med 30 graders vridning runt längs axeln. Metoden ökar tillförlitligheten i 11 mätningen av höger kammares volym genom tydligare avgränsning av höger kammares samtliga delar. Ultraljudsundersökningar med nya metoder som mäter storleken av muskelns förkortning (longitudinell och radiell strain) har utvecklats under de senaste åren för bedömning av vänster kammare. Tillämpning av metoden på höger kammare hos en grupp patienter och deras anhöriga samt en åldersmatchad grupp friska frivilliga har visat att metoden är genomförbar i höger kammare och visar avvikande fynd hos patienter med ARVC. Anhöriga kunde däremot inte skiljas från friska med denna metod. För att väga samman tidiga diskreta förändringar och följa deras utveckling har vi tagit fram ett ekokardiografiskt index för höger respektive vänster kammare baserat på diameter och funktion. Genetisk diagnostik av ARVC har nyligen startat i Sydöstra sjukvårdregionen, varvid en tidigare inte beskriven genetisk avvikelse som orsakar ARVC har påvisats. Undersökning av familjemedlemmar i tre generationer med denna mutation har visat stor variation i sjukdomsbilden, från plötslig död hos en 18 årig man till helt friska anlagsbärare. Dessutom visar studien vikten av genetisk och klinisk bedömning i kombination med känsliga metoder för hjärtundersökningar för att ställa rätt diagnos vid ARVC. 12 13 14 List of papers LIST OF ORIGINAL PAPERS This thesis is based on the following original publications, which will be referred to in the text by their Roman numerals: I Åström Aneq M; Lindström L; Fluur C; Nylander E. Long-term follow-up in arrhythmogenic right ventricular cardiomyopathy using Tissue Doppler Imaging. Scand Cardiovasc J 2008; 42(6): 368-74 II Åström Aneq M; Nylander E; Ebbers T; Engvall J. Determination of right ventricular volume and function using multiple axially rotated MRI slices. Clin Physiol Funct Imaging 2011; 31(3): 233-9 III Åström Aneq M; Engvall J; Brudin L; Nylander E Evaluation of right and left ventricular function using speckle tracking echocardiography in patients with arrhythmogenic right ventricular cardiomyopathy and their first degree relatives. Submitted IV Åström Aneq M; Fluur C; Rehnberg M; Söderkvist P; Engvall J; Nylander E; Gunnarsson C. Novel plakophilin2 mutation in a three generation family with arrhythmogenic right ventricular cardiomyopathy Submitted (Articles reprinted with permission) 15 16 Abbreviations ABBREVIATIONS ARVC SCD TFC RV LV LDAC ECG SAECG LBBB RBBB PVC RVOT-T LVOT VTI RVOT/BSA RVIT/BSA WMSI TAPSE TAPSV Sw 2D-strain AVO AVC MRI SA RLA bSSFP ICD Arrhythmogenic right ventricular cardiomyopathy Sudden cardiac death Task Force Criteria Right ventricle Left ventricle Left-dominant arrhythmogenic cardiomyopathy Electrocardiogram Signal-,averaged electrocardiogram Left bundle branch block Right bundle branch block Premature ventricular contraction Right ventricular outflow tract tachycardia Left ventricular outflow tract velocity time integral Right ventricular outflow tract related to body surface area Right ventricular inflow tract related to body surface area Wall motion score index Tricuspid annular plane systolic excursion Tricuspid annular plane systolic velocity Systolic velocity in the myocardial wall Two dimensional strain Aortic valve opening Aortic valve closure Magnetic resonance imaging Short axis Rotated long axis Balanced Steady-state free precession sequence Implantable cardioverter defibrillator 17 18 18 Introduction INTRODUCTION Sudden cardiac death (SCD) is still a problem although mortality from cardiovascular disease has decreased in recent decades. In Europe as well as in the United States, the incidence of SCD is estimated at almost 50-100 cases/100.000 people per year with some geographic variation [1, 2]. Resuscitation is still unsuccessful in 70% to 95% of the cases of Out-of-Hospital Cardiac Arrest [3, 4]. Sudden cardiac death is defined as unexpected death due to heart problems within a short time period, generally one hour from the onset of symptoms, in a person without any prior fatal condition[5]. For unwitnessed deaths, the World Health Organization definition extends to up to 24 hours [6]. The main cause of SCD is coronary heart disease but in people younger than 35 years, the leading cause is arrhythmia due to cardiomyopathies, abnormalities of the cardiac conducting system or coronary artery anomalies. One cardiomyopathy recognised as a cause of SCD is arrhythmogenic right ventricular cardiomyopathy (ARVC). It is considered as a cause of SCD in 3% of young athletes in the US and up to 20% in northern Italy. This geographical variation may be due to a more prevalent genetic abnormality or to more investigations with focus on this disease being performed in Italy. In many cases, sudden death is the first manifestation of ARVC. In a cohort of 100 patients with ARVC, Corrado et al. found that sudden death was the first manifestation of the disease in 22 patients [7]. Similar numbers were reported by other authors where SD accounted for 20-75% of the fatal outcome in ARVC [8, 9]. The prevalence of ARVC is estimated to 1 per 1000 to 1 per 5000 [10]. However this value could be higher as in many cases the disease is first recognized post mortem. Although ARVC is relatively uncommon in the general population, the increased risk for SD during exercise in adolescence or young adulthood is not only devastating for families, but also has impact on the community and the system of medical care. 19 19 The research in this thesis focuses on the diagnosis and follow-up of arrhythmogenic right ventricular cardiomyopathy using anatomical and functional myocardial parameters obtained from echocardiography and magnetic resonance imaging as well as initial experiences from molecular genetic testing. 20 20 ARRHYTHMOGENIC RIGHT VENTRICULAR CARDIOMYOPATHY Arrhythmogenic right ventricular dysplasia/cardiomyopathy was first described by G Fontaine et al. 1978[11]. Shortly thereafter, in 1982, Marcus et al. described 24 cases of ARVC [12] followed by multiple case reports from all over the world. ARVC is a disease of cardiac muscle causing replacement of muscle cells by fatty tissue and fibrosis mainly in the right ventricle. The disease was originally considered as a dysplastic process (ARVD) with congenital absence of ventricular myocardium but clinical and pathological studies have shown that the abnormalities are acquired and are of a progressive character. 1. Etiology 1:1 Molecular genetics In 30-50% of cases, ARVC has a familial occurrence, usually with an autosomal dominant inheritance pattern [13, 14]. A rare autosomal recessive variant, Naxos disease, with similar myocardial involvement and typical palmoplantar keratosis and wooly hair has also been described [15] There is evidence that ARVC is predominantly a disease of the desmosome. Five genes encoding the desmosome have been identified hitherto, in addition to 5 other genes or loci that have not yet been tracked to individual gene modification. Desmosomes are protein structures in the cell membrane permitting cell-to-cell adhesion. They occur in almost all solid tissues, but diseases related to mutation in these proteins are manifested only in the heart muscle cells and in the skin. This has been explained by continuous mechanical stress of the epithelium and the myocardium that at least in part alters the biomechanical behaviour of cells leading to myocyte detachment and 21 21 death. Two of the desmosomes containing proteins are intercellular; desmoglein-2 and desmocollin-2 and three are intracellular; plakoglobin, plakophilin-2, and desmoplakin (Fig. 1). In addition to cell adhesion, they have a function in cell-cell communication and tissue differentiation. The first identified gene in the dominant form of ARVC (ARVC2) is coding for the ryanodine receptor-2. This gene is now known to be present in cathecholaminergic polymorphic ventricular tachycardia (CPVT) suggesting a CPVT phenocopy rather than true ARVC. [2, 16-18]. Fig. 1. Schematic figure of Desmosomal Structure The desmosomal complex comprises two intercellular proteins: desmoglein (DSG)-2 and desmocollin (DSC)-2. The intracellular portions of these proteins interact with three other proteins: junctional plakoglobin (JUP), plakophilin (PKP)-2 and desmoplakin. The desmoplakin terminal part anchors Desmin filaments, the cytoskeleton. Modified from Sen-Chowdhry et al. [19]. In addition, two other non-desmosomal protein mutations have been reported to cause ARVC; the transmembrane protein 43 encoded by the TMEM43 gene [8], and the transforming growth factor beta -3 (Tb3), a cytokine-stimulating fibrosis and modulating cell adhesion [20]. The causative effect of these two mutations in relation to ARVC is still controversial. Patients carrying multiple mutations in a single gene (compound heterozygosity) or in two different genes (digenic heterozygosity) are more frequent than previously suspected (almost 13%) and this may contribute to the complexity of disease inheritance and variable penetrance of ARVC. This is 22 22 also a reason for an extended mutation screening beyond the identification of one mutation especially in families with a particularly severe phenotype [21]. However, it is noteworthy that failure to identify a mutation in the known genes does not exclude the disease and additional contributing gene mutations may still await detection. 1:2 Other possible pathogenic mechanisms 1:2:1 The role of inflammation in ARVC is still unresolved. The presence of inflammatory infiltrates in histology specimens particularly during the acute ‘hot phases’ of the disease suggests that ARVC could be either a sequel or trigged by a myocarditis. However if the inflammation is causative or just an effect of cell death is still unkown [22]. The causative role of viral infections [23, 24] and a genetic predisposition to infection/immune reaction in ARVC patients has also been proposed. 1:2:2 The mechanism of cell death by apoptosis has been discussed as apoptotic nuclei were found in up to 35% of patients in some studies [25, 26], but the role of apoptosis as a pathogenic pathway in ARVC is still to be defined. 2. Pathophysiology The prevailing hypothesis on desmosomal gene mutations causing ARVC is based on the effect of mechanical stress leading to the weakness of the intercellular junction causing disruption and degeneration of myocytes and their replacement by fibrofatty scar tissue. In this structural model, environmental factors such as exercise or inflammation could exacerbate impairment of cell adhesion and hasten disease progression. Progressive atrophy of the myocardium in ARVC occurs from the subepicardium to the endocardium. The residual islands of surviving myocardial cells left within the affected fibro-fatty area constitute a substrate for ventricular arrhythmias. Initially the disease has a regional distribution but 23 23 later on it becomes more global. Transmural atrophy of the myocardium causes aneurysmal dilatation and wall motion abnormalities which lead, in advanced stages, to heart failure. Although ARVC was initially considered to be strictly confined to the right ventricle, autopsy and sensitive imaging techniques have shown that most patients with ARVC have biventricular involvement [27-29]. It has been suggested that regular intense exercise causing volume overload and cavity enlargement of a thin-walled RV with high distensibility is a reason for the predominating RV involvement of ARVC. LV changes usually affect both the septum and the LV free wall, often regionally, with a predilection for the posteroseptal and posterolateral wall. 3. Histopathology Based on histology findings in different cohorts, two histopathologic variants have been described [30]; fibrolipomatosis type I with almost only fatty replacement and a small amount of fibrosis surrounding the surviving myocardial cells leading to an increased wall thickness, ‚pseudohypertrophy‛ of the RV, and the fibrolipomatosis type II with extensive replacement of myocytes by fibrosis and fatty tissue leading to thin wall and saccular aneurysm [31]. 4. Clinical features and imaging ARVC is generally diagnosed in young adults. In at least 80% of cases the diagnosis is made in patients below 40 years of age, although the disease has been described up to the ninth decade and in children [32, 33]. The disease is extremely uncommon below the age of 10 years. For unclear reasons, men are more frequently affected than women [34]. For a definite diagnosis, histology compatible with ARVC on specimens from autopsy, an explanted heart or from endomyocardial biopsy is required. However, diagnosis by endomyocardial biopsy is difficult due to the patchy involvement of the 24 24 disease. The septum, where the biopsy is usually taken, is not often involved. This, in combination with multiple potential etiologies of arrhythmias of RV origin, and difficulties in the assessment of RV structure and function, has prompted the establishment of standardized diagnostic criteria. The Task Force Criteria (TFC) proposed by Mc Kenna et al [35] are subdivided into major and minor criteria according to the specificity of their association with ARVC. They are based on structural, histological, electrocardiographic, arrhythmic, and familial features of the disease (Appendix 1). Occasionally, the left ventricle may be the predominant site of involvement. Left-dominant variants of ARVC (LDAC) that primarily affect the left ventricle have been identified in vivo and on post-mortem examination [36, 37]. Clinical features include arrhythmia of RBBB morphology and progressive structural abnormalities of the left ventricle. This disorder can be difficult to differentiate from other causes of left ventricular dysfunction. Marked arrhythmias in conjunction with relatively mild LV dysfunction may suggest the presence of regional LDAC. Accordingly, ARVC may manifest as cardiac failure involving both ventricles and may be difficult to distinguish from other forms of global heart failure. 4:1 Clinical presentation The most common clinical manifestations in ARVC are related to arrhythmia and conduction disturbances. Ventricular arrhythmia with an origin in the right ventricle display left bundle branch block morphology (LBBB). Advanced disease with extended left ventricular involvement may display ventricular ectopy with right ventricular branch block (RBBB) morphology. A history of syncope or dizziness, especially during exercise can be reported. Over time, symptoms related to heart failure, such as dyspnoea, oedema and fatigue may occur. However, ARVC is frequently asymptomatic, with the initial manifestation being sudden unexpected death. 25 25 4:2 Electrocardiography The electrocardiogram (ECG) is one of the most important diagnostic methods in ARVC. Abnormalities of depolarisation, conduction and repolarisation secondary to atrophy of ventricular walls reflect the pathophysiology of the disease. 4:2:1 Twelve lead-ECG T-wave inversion in anterior precordial leads (beyond V1) in the absence of RBBB is a sensitive finding in ARVC, reported to be present in between 37 and 81% of cases [38, 39], but the common pattern of T-wave inversion in ischemic heart disease and other cardiopulmonary diseases reduces its specificity. However, in the absence of RBBB, the presence of T-wave inversion in V1-V3 in young adults or middle aged subjects who have no apparent heart disease is uncomman, less than 3% in the study by Marcus [40]. Furthermore T-wave inversion in combination with ectopic ventricular beats of LBBB morphology should raise the suspicion of ARVC. Depolarisation and prolongation of conduction involving right precordial leads in the absence of RBBB can be detected as prolongation of the QRS complex (exceeding 110 ms in V1-V3). This was seen in 35 to 76% of cases [41, 42]. The epsilon wave (Fig. 2a) is a distinct deflection between the end of the QRS complex and the onset of the T wave. The presence of an epsilon wave is a major criterion but detected only in 1-25% of cases [43]. Finally selective prolongation of the S-wave duration in V1-V3 is seen in 34 to 71% of patients [44]. The variable presence of these findings in several studies can be related to the extent of right ventricular structural and functional abnormalities in the patients studied [45]. 4:2:2 Signal-averaged electrocardiogram (SAECG) SAECG permits the registration of low-amplitude potentials within the terminal portion of the QRS complex (late potential) that are not of sufficient amplitude to be visible on the 12-lead ECG. ARVC was one of the first pathologic non-ischemic disorders in which the presence of late potentials were identified [46] (Fig. 2b). 26 26 Fig. 2 a. ECG showing Epsilon wave b. Pathological late potentials on the SAECG 27 27 4:2:3 Ambulatory ECG monitoring This is performed to detect spontaneous arrhythmia. Monitoring is usually done for 24-48 hours, but in symptomatic patients longer registrations may be indicated to capture arrhythmia. The presence of more than 1000 premature ventricular contractions (PVC) of LBBB morphology on 24h Holter monitoring is a minor criterion in ARVC. When the subject has a family member with confirmed ARVC the presence of 500 PVC of LBBB type constitutes a major diagnostic criterion for ARVC . The presence of sustained or non-sustained ventricular tachycardia of LBBB morphology can also be detected [47]. 4:3 Exercise testing Exercise testing in general is recognized for its ability to unmask ventricular arrhythmia during physical exercise. However, in ARVC, the diagnostic utility in clinical decision making and in follow-up remains to be established. It is noteworthy that lack of arrhythmia during exercise should not be considered as reassuring [48]. 4:4 Echocardiography Identification of right ventricular morphological abnormalities by echocardiography is difficult as the abnormalities due to ARVC may be limited to small regions in the ventricular wall. Typical echocardiographic findings are often localized to the inflow and/or outflow tracts. The apex region was described earlier as part of the affected ‚triangle of dysplasia‛ but recent observations have shown that involvement of the apex is a late finding. The main changes are regional dilatation of the RVOT and/or the inflow part. Structural wall abnormalities such as localized wall tinning are important diagnostic features but hard to find in the trabeculated thin right ventricular wall. Micro-aneurysms in the anterior or inferior RV walls are specific for ARVC. In other forms of ARVC, pseudo-hypertrophy of the RV wall with a 28 28 thick moderator band can be seen [49]. In this variant, histology shows a predominance of fatty tissue and less fibrosis. Myocardial dysfunction is regional in the early stages without apparent effect on global RV function. Early changes in regional function can easily be overlooked. Later on, dilatation and dysfunction of both ventricles may occur accompanied by mural thrombosis within aneurysms or in the atrial appendages when heart failure is complicated by atrial fibrillation. 4:5 Magnetic resonance imaging MRI offers an extensive visualisation of the right ventricular chamber, permitting the detection of microaneurysm and wall bulging. Furthermore, the calculation of right and left ventricular volumes and ejection fraction is more precise with MRI compared to echocardiography [50]. Myocardial delayed enhancement MRI can detect fibrosis especially in the advanced form [51]. However, the detection of intramyocardial fat in the RV wall is unreliable. The presence of pericardial fat in contact with the thin RV wall as well as the high prevalence of adipose infiltration in normal hearts [52] makes this finding less specific for the diagnosis of ARVC. 4:6 Other modalities 4:6:1 Computer Tomography Most centers use MRI in the diagnosis and follow up of ARVC patients. However in many cases the prophylactic implantation of a cardioverter defibrillator (ICD) is necessary to prevent SCD. After such implantation, MRI is contraindicated but CT may help in the serial assessment of right ventricular function [53]. 29 29 4:6:2 Angiography Angiography was previously the gold standard for detection of RV abnormalities [54]. However, recent development of new methods has obviated the need for angiography. 4:6:3 Electrophysiologic study (EPS) EPS may have a role in the differential diagnosis of arrhythmia of right ventricular origin [55, 56]. 5. Differential diagnosis In the presence of RV tachycardia and /or dilatation of the RV, other structural diseases should be ruled out e.g. congenital heart disease such as left- right shunts at the atrial level, and acquired diseases such as pulmonary hypertension, myocardial infarction and systemic inflammatory and infiltrative diseases[57]. Idiopathic right ventricular outflow tract tachycardia (RVOT-T) is a benign, non-familial disorder that is often difficult to differentiate from ARVC in early stages, especially since recent MRI studies have shown structural abnormalities in the outflow tract in RVOT-T. A definite diagnosis may not be possible at first presentation. Case studies have reported patients that have been assigned a diagnosis of RVOT-T but later developed typical features of ARVC [58]. Brugada syndrome is another disorder that can be difficult to differentiate from ARVC in some cases. Clinical and histopathological studies have shown a definite overlap between Brugada and ARVC [59, 60]. Myocarditis, usually viral and predominantly involving the RV may be difficult to differentiate from ARVC particularly during the acute phase with arrhythmias [61, 62]. For differential diagnosis, the progress during follow-up is important. The RV may dilate as a normal adaptation to regular intensive physical activity in the so called ‛athlete´s heart‛. This has to be considered in the differential diagnosis of ARVC [63, 64]. 30 30 6. Natural history Four distinct phases have been described in the natural history of ARVC [7] 1. The early ‚concealed‛ phase is associated with minor ventricular arrhythmia and subtle structural changes. Patients are often asymptomatic, but nonetheless at risk of SCD especially during physical activity. 2. In this stage, an overt electrical disorder is manifest, with symptomatic ventricular arrhythmia and more obvious morphological and function abnormalities of the right ventricle. 3. RV failure caused by disease progression. 4. Biventricular heart failure in advanced stages which can be difficult to differentiate from dilated cardiomyopathy. However the evaluation of familial patterns suggests that a distinct stepwise progression to more advanced stages of disease seldom occurs. 7. Management of ARVC patients 7:1 Physical activity Athletes with probable or definite diagnosis of ARVC should be excluded from most competitive sports, according to the 36th Bethesda conference [65] In the larger group of non competitive young patients who are asymptomatic or mildly symptomatic there is usually a desire to have an active recreational lifestyle. However the definition of low intensity activity is difficult. Recommendations on exercise need to be individualized for each patient and the intensity of physical activity considered. As a help for the clinician, Maron et al. categorized sports activities into high, moderate, and low level intensity [66]. Participation in intensive exercise should be avoided even in the presence of antiarrhythmic protection afforded by an implanted ICD [67] 31 31 7:2 Anti-arrhythmic pharmacological therapy Pharmacological therapy is the recommended initial treatment for a patient with mild, well tolerated arrhythmia. Treatment consists of beta blockers and class I and class III antiarrhythmic drugs. Sotalol has been reported to be the most effective pharmacological antiarrhythmic treatment in ARVC [68] 7:3 Implantable cardioverter defibrillator (ICD) ICD is an effective method for terminating malignant ventricular tachyarrhythmias. However the most relevant question is whether there is a balance between the benefit of preventing arrhythmic death and the risk of complications and side effects from ICD implantation. A correct diagnosis of the disease on the basis of detailed investigations is essential before ICD implantation is considered. Recommended indications for ICD implantation in ARVC include secondary prevention after survived cardiac arrest or documented sustained VT. ICD therapy as primary prophylaxis in asymptomatic patients or relatives with high risk profile must be based on individual risk assessment because of the lack of data supporting this approach. The main indication for primary prophylactic ICD is currently based on either history of SCD in early age in the family, or evidence of extensive RV dysfunction as well as involvement of the LV. In a cohort of 42 ARVC patients with ICD, Rogin et al. showed that 78% of patients experienced at least one appropriate discharge during an average of 3,5 years of follow-up [69]. Similar findings were reported by other authors [70-72]. 7:4 Evaluation of relatives First degree relatives of deceased or living patients with ARVC should undergo a cardiac evaluation[13]. Modified Task Force Criteria have been proposed because the original TFC are highly specific but not sensitive enough to evaluate relatives who may have an early form of the disease (Appendix 1) 32 32 [13, 73]. Further investigations are needed regarding the sensitivity and specificity of these criteria, the need and frequency of repeated follow-up and risk stratification of relatives. 33 33 34 34 Aim of th thesis AIM OF THE THESIS The general aim of this thesis is to investigate how non- invasive methods may improve diagnosis in arrhythmogenic right ventricular cardiomyopathy. Specific aims: To study the progress and the rate of change in echocardiographic parameters during long term follow-up in patients with ARVC (Paper I) To explore the value of using tissue Doppler imaging in the follow-up of patients with ARVC (Paper I) To evaluate whether a new axial orientation modality for the assessment of RV volume and function by MRI will help to overcome the limitations of the standard short axis orientation (Paper II) To study the feasibility of using two dimensional strain analysis based on speckle tracking applied to the RV (Paper III) To test the ability to detect regional RV dysfunction at early stage, in relatives of ARVC patients using myocardial strain based on speckle tracking (Paper III) To describe the phenotype of a new mutation in the plakophilin 2 gene in a three generation family with ARVC (Paper IV) 35 35 36 Study populations STUDY POPULATIONS Healthy controls (II,III) Totally 25 healthy volunteers were included, whereof 20 were examined by both MRI (II) and echocardiography with analysis of myocardial strain (III). Three of the remaining subjects underwent MRI alone and two had only echocardiography. The healthy subjects were recruited by advertisements on the university web page and among medical students. All were asymptomatic and lacked family history of premature cardiovascular disease. No one received cardiac medication. All underwent a bicycle ergometer exercise test to confirm the absence of heart disease. Those who had abnormal ECG or exercise test were excluded. ARVC patients (I,III,IV) In paper I, all patients from the South East region with a diagnosis of ARVC for more than 6 years were included. There were fifteen patients, 9 male and 6 female. The diagnosis was based on the conventional Task Force Criteria. Patients were examined regularly according to a follow-up program. In this analysis we focused on the first and last echocardiographic examination during the study period. Two of these patients were also reported in paper IV. In paper III, we studied all males with an ARVC diagnosis, which included nine patients from study I, and eight patients with an ARVC diagnosis of less than 5 years. First degree relatives (paper III) Since 1995, a screening protocol for first degree relatives (children, parents or siblings) of ARVC patients has been followed. In this cohort nineteen males, 18 years or older were included and underwent echocardiogram with focus on right ventricular function. 37 37 Table 1. Characteristics of the male (M) and female (F) population studied. Patients I Relatives Controls 15(9M*,6F) 22-58 yr ** (mean 40) 23 M‡ 22-64 (mean 39) II III 17 M 32-70 yr † (mean 49) 19 M 19-73 yr (mean 29) IV 8 subjects (4M, 4F) in an ARVC affected family 22 M 24-66 yr (mean 36) * All included in paper III, and two included in paper IV. ** Age at the time of the first investigation † Age at the examination ‡ 20 of these controls are included in paper III Ethical approval for studies (I,II,III,IV) was obtained from the Regional Ethical Review Board in Linköping. 38 38 Methods METHODS 1. Echocardiography Paper I, III, IV The echocardiogram was performed with the subject in the left lateral decubitus position. A 2-dimensional, colour, pulsed and continuous-wave Doppler examination was recorded following the recommendations of the American Society of Echocardiography for transthoracic studies [74]. We used the ultrasound systems Acuson 128XP (Acuson corporation, Mountainview, CA,USA) for the first examination in paper I and Vivid 5 or Vivid 7 (GE Medical Systems, Horten, Norway) for the last examination in paper I and in paper III. Data were obtained from multiple standard views of the left and right ventricle (Figure 1, paper I). At least three regular beats of each view were recorded during quiet respiration. In paper I, wall motion score index (WMSI) was assessed in a sixteen (LV) and seven (RV) segment model. Each segment was classified according to a scale with 6 levels: 0=not visualised, 1= Normal, 2=Mild hypokinesia, 3=Severe hypokinesia, 4=Akinesia and 5= Dyskinesia. A score was calculated for each ventricle as an average value of analysed segments. The presence of isolated sacculation (S) and wall thinning (T) was reported. All analyses were performed by a single observer. 1:1 Annular motion analysis by M-mode A 2-dimensionally–guided M-mode cursor was placed on the lateral or the septal part of the mitral annulus to record the annular motion towards the cardiac apex in systole from a standard apical 4-chamber view (paper I). An identical recording was obtained from the lateral (paper I,III) and posterior (paper I) part of the tricuspid annulus. Care was taken to orient the beam perpendicularly to the motion of the annular structure. The total 39 39 systolic displacement was measured from end-diastole (the initial deflection of the QRS complex in the ECG) to the highest point of contraction as initially validated by Kaul et al. [75]. 1:2 Longitudinal strain based on speckle tracking The strain measured by two dimensional echocardiography is called Langrangian strain (e) and is defined as the change of myocardial fibre length during stress at end-systole compared to its original length in a relaxed state at end-diastole. Negative strain indicates fibre shortening or myocardial thinning, whereas a positive value describes lengthening or thickening. The two dimensional loops from routine echocardiographic examinations were processed offline. The end-systolic frame was identified from by definition on the parasternal or apical long axis (3-chamber) view, where the aortic valve is ‚optimally visible‛. The time point of aortic valve closure was marked. The four chamber view with focus on the left and then on the right ventricle was recorded with a frame rate ranging between 40 to 70 frames/s. All images were stored digitally and analyzed on the Echo Pac work station (GE Medical Systems, EchopacPC, version 6.0.1). A complete cardiac cycle was required for processing. Offline analysis began with tracing the endocardial border. The software then automatically defined an epicardial and midmyocardial line and processed all frames of the loop based on the identification of natural acoustic markers in the myocardium. Myocardial deformation was defined as strain an expressed in terms of percent shortening. The length of each wall was automatically divided into 3 segments; base, mid and apex. Since the apex of the RV can be difficult to expose on echocardiography, we chose to focus on the basal and mid ventricular segments (Fig. 3) 40 40 Methods Fig. 3. Determination of longitudinal strain in an apical four chamber view. Left upper panel:The lateral wall of the right ventricle is divided into 3 segments; base, mid and apex. M-mode representation of peak systolic strain (left lower panel). The right upper panel shows time –curves of longitudinal strain for each myocardial segment, and the right lower panel displays the calculated values. 1:3 Echocardiography index Multivariate discriminant analysis was used to detect differences between ARVC-patients and controls in order to investigate the relative role of parameters from the right and left ventricle for the discrimination of the two groups. The parameters used for the right ventricle were right ventricular outflow and right ventricular inflow tract related to body surface area (RVOT/BSA, RVIT/BSA), tricuspid annular plane systolic excursion (TAPSE), tricuspid annular systolic velocity and longitudinal strain based on speckle tracking of the basal and mid RV free wall segments. For the left ventricle the parameters were LV diameter, left ventricular outflow tract velocity time integral (LVOT VTI), mitral annular systolic velocity from the lateral and septal walls, strain based on speckle tracking of the basal and mid segments of the septum and lateral wall. Significant components were reassembled to create separate indices for the right and left ventricles and recalculated for each individual showing the distribution of the first degree relatives related to patients and healthy controls. 41 41 2. Magnetic resonance imaging Paper II The MRI image acquisition was performed in a Philips 1.5T Achieva scanner (Philips Healthcare, Best, the Netherlands), using a five-element cardiac synergy surface coil. Cine-MR, synchronised using retrospective ECG gating, was performed with a balanced steady-state free precession sequence (bSSFP). bSSFP uses a high number of excitation pulses to provide a high signal-tonoise ratio (SNR) and better definition of structure compared with gradient echo-sequences. The echo time (TE) was 1.5 ms, repetition time (TR) 3.0 ms, flip angle 60º and pixel size 1.25x1.25 mm2 for all image acquisitions. Three long axis planes of the left ventricle (2- and 4- chamber views as well as the apical long-axis view) were obtained for orientation. The short axis plane was planned on the LV, covering the entire heart with on average 19 (range 17-25) short axis, 8mm thick slices. Using sensitivity encoding (SENSE) reconstruction, each SA slice took 6 heart beats to acquire. A long axis was drawn in the RV cavity joining the middle of the tricuspid annulus to the RV apex. Six long axis slices were acquired, by incrementally rotating 30 º rotation around this original RV long axis. Every long axis slice was acquired during 12 hearts beats. Six slices were considered as a suitable compromise between potential spatial information and time spent for image acquisition. The order of the sequence of axial and short-axis acquisition was assigned randomly for each patient. In addition, two-dimensional cine through-plane PC-MRI velocity data were acquired in a plane perpendicular to the main flow direction in the ascending aorta (AoA), just downstream from the aortic valve (AoV). All scans were performed by a single operator. To test the accuracy of the volume estimation for different geometries, a phantom study was performed using both SA and RLA acquisitions. We used symmetrical objects such as a bottle and a pear, in addition to a banana simulating the irregular crescentric right ventricular cavity. For all phantoms, six RLA slices were acquired, and sufficient SA slices to cover the complete phantom. Imaging parameters were identical for both the RLA and SA acquisitions (Fig. 5). True phantom volumes were measured immediately after the MR investigation, by immersing the objects in a beaker of water. 42 42 Methods Fig. 4. 3D visualization of the six slices rotated around the long axis. A. depicts a pear and B. the right ventricular chamber as seen from the apex with the septum at the left. Image analysis All calculated volumes from the phantom studies were based on still images and were, as well as the cine images, evaluated using the freely available analysis software Segment (v1.702, http://segment.heiberg.se) (Fig. 3). Two observers measured all the data independently. For the short axis datasets, a consensus was reached before segmentation on which basal slice to include. The volume of added, as well as of deleted slices was analyzed independently and the stroke volume recalculated. For the left ventricular volumes, at least half of the periphery of each ventricular slice had to be present in each time frame to allow its inclusion in the volume. When this rule was applied, a consensus procedure was not necessary for the left ventricle. Aortic flow volume (stroke volume) was calculated by multiplying aortic cross sectional area with mean flow from a slice placed cranial to the coronary ostia. 43 43 Fig. 5 The right ventricular end diastolic ED (A-C) and end systolic ES(B-D) slices on short axis (upper) and rotated long axis (Lower) acquisitions. A B C D 44 44 Methods 3. Signal-averaged electrocardiogram Paper I, III, IV SAECG is recorded using bipolar XYZ ECG leads. The X lead is positioned at the fourth intercostal space in both midaxillary lines. The Y lead is positioned on the superior aspect of the manubrium and on either the upper left leg or left iliac crest and the Z lead between the fourth intercostal space (V2 position) and directly posterior on the left side of the vertebral column. The signal is filtered using a high and low pass-filter (25 or 40-250HZ). Between 250- 400 beats are averaged to improve the signal-to noise ratio and facilitate the detection of low-amplitude potentials. Analysis of the filtered QRS complex includes 1) the filtered QRS duration(fQRS) ; 2) the root-mean-square voltage in the last 40 ms of the filtered QRS (RMS 40ms); and 3) the duration of the high frequency low-amplitude signal of the filtered QRS not exceeding 40 μV (HFLA < 40 μV) Criteria for normal values in SAECG were published in 1991 and 1996 by a joint committee of the AHA and the ESC [76, 77] and are the following: 1) fQRS ≤ 114ms 2) RMS 40 >20 μV 3) HFLA 40 <38 ms These limits are applicable in the absence of bundle branch block with an unfiltered QRS duration less than 120ms. Pathological late potentials are considered to be present when at least two of three parameters exceed the normal range. 4. Genetic analysis Paper IV During a genetic consultation, the first degree relative to a deceased proband(the first one in the family who have been in contact with medical 45 45 care) received oral and written information and the issue of genetic testing was discussed. A blood sample was collected, DNA extracted and a Polymerase Chain Reaction method (PCR) used to amplify the coding parts of the candidate genes followed by DNA sequencing. Genetic alterations were assessed for plakophilin2 (PKP2), desmoplakin (DSP), desmoglein 2 (DSG2), desmocollin 2 (DSC2) and the detected pathological mutations was compared and novel variants were deposited to international ARVC-Database (http://www.arvcdatabase.info)[78]. Based on the patient pedigree, and after informed consent, blood samples were collected from remaining first degree relatives for mutation analysis. 46 46 Methods 5. Reproducibility studies In paper II, for the determination of the intra- observer variability, one observer repeated measurements of RV volumes on MRI both SA and RLA orientation, at least three months after the first measurements. In the second analysis, the operator was blinded to the results of the first measurements. In paper III, all strain measurements were repeated by the same observer who was blinded to the initial values, at least 5 weeks after the first analysis, in a random sample of 12 echocardiographic studies (4 patients, 4 relatives and 4 controls). To define interobserver variability, measurements in the same random sample were assessed by a second independent observer blinded to the results obtained by the previous investigator. 47 47 48 48 Statistics STATISTICS All values are presented as mean ± SD (Paper II, III). The statistical significance of differences was calculated using the paired Student’s t-test. Significance was based on p values of less than 0.05 (Paper I). In paper II, to test the agreement between the two orientations, the method of Bland and Altman was used [79]. Agreement was determined as the mean difference between the two views, with limits determined from the mean value ± 1.96 standard deviations. The intra- and inter-observer variabilities were expressed as the coefficient of variability, which is the standard deviation of the differences divided by the mean of the measurements and expressed as a percentage (Paper II) or as standard error of a single determination (Smethod) using the formula first proposed by Dahlberg [80]. Smethod was also expressed as % over all means (Paper III). Statistical analysis were performed using Statistica 8.0 (Statsoft Inc, Tulsa, Oklahoma, USA). 49 49 50 50 Results RESULTS Paper I We performed a long- term follow up in 15 patients with ARVC using ECG, SAECG and echocardiography including tissue Doppler imaging. The mean follow-up period was 8.7 years (6-10). No death occurred during this period. The reason for referral to our department was ventricular tachycardia in 6/15 (40%), syncope in 3/15 (20%) and family history of ARVC or SCD with ARVC findings at autopsy in 4/15 (27%). Table 2. Symptoms and findings at the first examination (left column) and those occurring during follow-up in addition to the initial symptoms (right column). First investigation n/total % Ventricular arrhythmias 6/15 (40%) Syncope 3/15 (20%) T-wave inversion beyond V1 12/15 (80%) Patol. SAECG( 2/3 or 3/3) 9/15 (60%) RVOT dilatation (>2cm/m2) 6/15 (40%) RVIT dilatation 10/15 (67%) Sacculation/bulging 2/14 (14%) Follow-up n/total % 8/15 (53%) 3/15 (20%) 12/15 (80%) 10/15 (67%) 7/15 (47%) 11/15 (73%) 5/14 (36%) Echocardiographic results of the right ventricular function during follow-up are shown in (Fig.6) 51 51 Fig. 6. Variation in tricuspid annular plane systolic excursion (TAPSE) and systolic velocity on tissue Doppler imaging at the first (1) examination and at the follow-up (2) A B A. TAPSE: Tricuspid annular motion on M-mode at the first (1) and the last (2) examination B. TALs: Tricuspid lateral systolic annular velocity at the first (1) and the last (2) examination The data indicate a progression of the recorded signs of disease. The rate of progression was generally slow, but with individual variation. Paper II A method for the determination of RV volume using MRI was developed and tested in phantoms and healthy individuals. The phantom result shows no significant difference between volumes acquired with the two MRI methods and the reference method which based on the displacement of water (Table 3). Table 3. Volume of 3 phantoms measured with MRI in short axis and rotated long axis orientations compared to the displaced volume of water. Bottle Pear Banana Short axis 515 ml 216ml 126ml Rotated long axis 516 ml 214ml 132ml 52 52 Real volume 515ml 215ml 129ml Results A consensus between the two observers whether to include or exclude the basal slice from the RV volume was necessary in 9/23 (39%) controls leading to a difference in EDV of 6-20ml (8-21%) or ESV 12-21ml (20-27% of the total volume). After the consensus, EDV, ESV, SV and EF for the right ventricle did not differ between the SA and RLA views with p-values in excess of 0.05. Thus, it was confirmed that a problem with the short axis method is the difficulty to define the basal limits of the right ventricle and that in many cases, consensus was needed to obtain an acceptable reproducibility. This seems to be overcome with our axial method that is planned to be tested in different RV pathologies in the future. Paper III Sensitive methods for the detection of early signs of ARVC in patients and their relatives are needed. The development of genetic methods cannot replace phenotypic characterization but provide additional building blocks for a deeper understanding of the disease. In this study, we compared ARVC patients with first degree relatives and healthy age- matched controls. Table 4. Clinical and electrocardiographic characteristics of the study population Age (years) Arrhythmiarelated symptoms T-inversion beyond V1 Late potentials on SAECG ARVC (n=17) Median (range or %) Relatives (n=19) Median (range or %) Controls (n=22) Median (range or %) P-values 49 (32-70) 29 (19-73) 36 (24-66) 0,44 13 (76%) 2 (11%) 0 13(76%) 0 0 9/14* (64%) 3/19 (16%) 0 SAECG: Signal-averaged electrocardiogram. *SAECG was not recorded in 3 patients due to frequent arrhythmia or ongoing cardiac pacing. 53 53 Using discriminant analysis on left and right ventricular echocardiography parameters, an LV and an RV index was developed based on data from ARVC patients and controls (Fig. 7). Fig. 7. Distribution of first degree relatives in relation to patients and healthy volunteers. The lower the index (<0) the closer to normal (healthy controls). Paper IV Methods for the detection of genetic alterations are now being developed and applied in patients. 25 of the patients with ARVC in our region have been tested for mutations in Plakophilin 2, Desmoplakin, Desmocollin 2 and Desmoglein 2. In this process, we detected novel genetic alterations, and the inheritance pattern of p. Trp 123X, in a 3-generation family and the nature of the mutation indicates a functional consequence resulting in the ARVC phenotype. Genetic analysis of the first degree relatives to a patient who suffered a sudden cardiac death showed new mutation in the plakophilin 2 gene. The proband´s mother, sister and two of her three children were shown to carry the same mutation (Fig. 8). 54 54 Results Fig. 8. Pedigree of a three generation family with a novel mutation in PKP2. 55 55 56 56 Discussion GENERAL DISCUSSION The right ventricle was until recently considered as a passive conduit[81]. However, during the past three decades the function of the RV has gained attention. A better understanding of the prognostic role of right ventricular function for many acquired and congenital heart diseases as well as its influence on global cardiac function through biventricular interaction has raised the interest in RV physiology and function [82-91]. However, the assessment of RV function is still incomplete in daily practice partly because of its difficult and inaccessible morphology [92, 93]. 1. Aspects on right ventricular anatomy and physiology The right ventricle has a complex and unique morphology. In contrast to the ellipsoid outline of the LV, the shape of the RV is more or less triangular when viewed laterally. In a normal heart with normal loading and electrical conduction, the RV appears crescentic in cross-section, wrapping around the left ventricle with the septum concave to the LV [94]. Three components have been described forming the RV: 1.the inlet portion extending between the hinge line of the tricuspid valve and the insertion of the papillary muscles 2.the apex with thick muscular trabeculations and 3. the outlet or infundibulum. Furthermore, there is a thick muscular band, crista supraventricularis, between the inflow and outflow tract, participating in the contraction of the free wall. The right ventricle has a thin wall (3-5mm) as it pumps at a lower systolic pressure than the LV. Over the years, the architectural arrangement of the myocytes within the ventricular mass remains a subject of controversy. In the Torrent-Guasp helical model, the cardiac fibres are described as a continuous band connecting the two ventricles as a helix with two loops: An apical loop with descending and ascending oblique fibres that build the septum and left ventricular wall and a basal loop with transverse fibres that 57 57 form the right ventricular free wall and overlap the septum [95]. The myocardial structure of the right ventricular wall was described as two principal layers; an inner layer with longitudinal fibres and a superficial layer with circumferential fibres in the inflow region becoming more longitudinal in the outflow tract [96]. The LV chamber has an oblique subepicardial, a longitudinal subendocardial and predominantly a circular fibre direction in between [97] (Fig.9). Fig. 9. The helical myocardial model The helical model of the heart when unfolding the basal loop of the RV. showing the transverse fibre orientation of free walls inflow and longitudinal on the outflow tract. PA:pulmonary artery. Ao: Aorta (Fig. Torrent-Guasp. Reprinted with permission. Copyright 2011 Elsevier) Advocating a different model, RH Anderson describe the myocardial structure as arranged with each myocyte anchored to other myocytes within a supporting fibro-collagenous matrix, forming different bundles, the bundles of myocardial fibres having various orientation [98] (Fig.10). Fig. 10. Various fibre orientation in the myocardium Short axis views at apex, mid and basal level showing variation in fibre orientation within the ventricular mass. Histological sections in the upper panels and their schematic representation in the lower panels. (Fig. RH Anderson reprinted with permission. Copyright 2011, Elsevier) The contraction of the right ventricle occurs in a "peristaltic" manner with the outflow tract contracting 25-50ms after the inflow [99]. The right and left stroke volumes are almost equivalent, as the bronchial circulation could be 58 58 Discussion considered as non-significant. Normally the RV ejects the same stroke volume as the LV using only one-fourth of the LV stroke work. This is possible in part because of the low systolic pressure and high compliance of the pulmonary circulation and the high compliance of the thin RV wall [100]. 2. Challenges in right ventricular imaging An attempted complete visualization of the RV and careful assessment of its function are still incompletely done in most cardiac investigations. A number of difficulties need to be addressed to successfully image the RV: 1. The anterior retrosternal location of the RV limits acoustic access by echocardiography. 2. The three components of the RV chamber; inlet, apex and infundibulum are located in different planes which require different views for visualization of the entire RV by echocardiography. 3. The complex, triangular and crescentic shape of the RV is difficult to model geometrically, unlike the LV 4. The extensive wall trabeculation can be challenging for delineation in MRI, CT and echocardiography 5. The thin wall of the inflow tract can be difficult to differentiate from right atrial wall in the delineation of the RV using MRI, CT and radionuclide ventriculography. The solution has often been to resort to using visual estimation only, in clinical routine. 2.1 Echocardiography Echocardiography plays an important role in the screening, diagnosis, and follow up of ARVC patients and their relatives as it is non-invasive, available and relatively inexpensive. It is invaluable in the presence of an ICD, which excludes using MRI. Due to RV morphology, contraction along the long axis is the predominant systolic motion pattern in the RV. 59 59 M-mode and Tissue Doppler imaging Tricuspid annular systolic motion (TAPSE) reflects the long axis oriented motion of the RV. Kaul et al showed in 1984 that tricuspid annular systolic excursion on echocardiography correlates with radionuclide right ventricular ejection fraction, which then was the gold standard for characterization of RV systolic function [75]. Different studies have shown a good reproducibility of TAPSE and have used this method as a diagnostic tool for RV dysfunction [101-107]. Samad et al. found that TAPSE below 15 mm was associated with increased mortality in patients with a first acute myocardial infarction [107]. In the follow up of 817 patients with heart failure for 4 years, Kjaergaard et al. found that TAPSE below 14 mm was related to higher mortality and adverse outcome [82]. Later on, the contraction of subendocardial longitudinal fibres was reliably assessed from apical views, using tissue Doppler imaging [108, 109]. In a study of patients with advanced heart failure, Meluzin et co-workers showed that tricuspid annular plane systolic velocity TAPSV <12cm/s identified RVEF <45% on first-pass radionuclide ventriculography with 90% sensitivity and 88% specificity [110]. TAPSV was also compared to RVEF determined by MRI. Wahl et al. showed that TAPSV <9cm/s had a high specificity for RV dysfunction with a negative predictive value of 99%[111]. As we found in our long term follow-up of ARVC patients in paper I, TAPSE and systolic tricuspid annular velocity are robust methods for the follow up of patients with a progressive disease such as ARVC. We showed a higher change in TAPSV than in TAPSE over time. This can be interpreted in terms of a higher sensitivity in detecting RV dysfunction using wall velocity than annular displacement. Similar findings were shown by other authors [112]. A limitation in tissue Doppler imaging (both spectral and color Doppler) is the dependency on the angle of Doppler insonation. This can be more important in the right ventricle as the triangular shape of the RV can complicate the alignment with the ultrasound beam, especially when investigating bulging RV wall segments beneath the RV base. Strain measurement based on speckle tracking Speckle tracking echocardiography is based on the distribution of myocardial fibres that create a unique pattern of backscattered ultrasound, ‚speckles‛. 60 60 Discussion These speckles create a unique fingerprint that enables tracking myocardial motion during the cardiac cycle. Since each speckle may move in relation to its neighbours, local deformation may be determined [113, 114]. The computer-based solutions for speckle tracking are basically ‚black boxes‛ but their output may be assessed by comparison with other techniques. Unlike tissue Doppler imaging, speckle tracking is robust, shows less angle dependency, and can track the myocardium in the transverse as well as in the axial direction. In our hands, the assessment of the basal and mid segments of the left and right ventricles was highly feasible and reproducible in our population of healthy volunteers and relatives to patients with ARVC (Paper III). However in the study of the right ventricular free wall of ARVC patients, this was less feasible (59% compared to 95% in relatives and 86% in the volunteers) due to the thinning of the myocardium in pathologic segments of the wall. We limited our measurements to basal and mid segments of the ventricular wall as the apex of the right ventricle frequently is inaccessible with echocardiography. Furthermore, previous studies have shown that measurements of velocity and strain in the apex of normal left and right ventricles have displayed low accuracy compared to measurements in the basal and mid segments [115-117]. Longitudinal strain based on speckle tracking showed no difference between first degree relatives and controls (Paper III). Several contributory factors may be operative. The probability that all 19 relatives in our cohort would lack a mutation is low, as the penetrance in ARVC has been reported to be 30-66% [118-121]. At the time of the investigation, all relatives may have had a normal phenotype, i.e. the ARVC genotype had not yet become clinically obvious, or the strain method is not sensitive enough to detect slight abnormalities in myocardial deformation. It is noteworthy that the ARVC disease process starts in the subepicardium and advances towards the endocardium. That may suggest that longitudinal deformation of the right ventricle is affected later on. As the abnormalities in early stages of ARVC might be subtle and difficult to recognize with echocardiography, we used discriminant analysis to develop an index for the left and for the right ventricle including both dimensional and functional echocardiographic parameters. Using these indices we found that some of the relatives had an index closer to that of the ARVC patients than other relatives. Further evaluation of this index is needed; including female patients and relatives as well as controls and extending the cohort to recently detected patients and relatives. Incorporating diastolic functional data is also possible. Including the results of genetic analysis in future studies might help 61 61 detect different phenotypic expressions of genetic mutations. In the future, left and right ventricular indices may be used clinically as tools for detection as well as following the appearance of typical features of ARVC patients and their relatives. 2.2 Magnetic resonance imaging The superiority of MRI over other techniques for right ventricular assessment rests on its unique ability to image the entiree ventricle. It is useful for diagnosing ARVC especially in cases where regional motion abnormalities on MRI correspond to areas with high signal intensity on late enhancement (Delayed contrast-enhanced viability using Gadolinium). Quantitative measurements of the RV volume and function are however subject to a relatively large degree of variability compared to the LV [122, 123]. The reproducibility of MRI measurements is crucial in follow-up. In clinical practice, RV volume analysis relies on short axis (SA) views obtained simultaneously when assessing the LV. An important difficulty to overcome in using the SA is how to define the basal slice and how to reliably exclude atrial volume from the ventricular measurement. Errors in defining the boundaries of this large slice can result in significant differences in serial measurement [124-126]. The interstudy measurements by the same reader showed a good reproducibility even if it was lower compared to that of the LV. However the intraobserver and interobserver variability were large indicating that observer subjectivity is a limiting factor in the interpretation of the right ventricular MR images [123, 127]. To reduce this variability, different methods have been used to 1. improve definition of the inflow/outflow tract, e.g identification of the right atrioventricular ring by the visualization of the right coronary artery [128], combination of long-axis sections with short-axis sections in the same dataset [129], axial slice orientation with orthogonal stack covering the heart from a level below the diaphragm to the pulmonary bifurcation [130-132] or modified RV short axis slices located with respect to the RV long axis [133]. 2. to reduce variability and analysis time in post-processing by utilisation of automatic or semi-automatic segmentation [134, 135]. Each one of these changes showed some improvement in volume measurement. However, despite these suggestions, serious limitations due to RV shape and heart position in the thorax still remain. We used cut planes rotated along the long 62 62 Discussion axis of the RV to obtain an optimal visualization of the RV inflow and outflow tract thereby reducing the uncertainty due to the basal slice in SA (paper II). Improvement of RV volume assessment has become necessary as the modified Task Force Criteria rely on quantitative data from RV volume and function [73]. However, delineation of the endocardium and the trabeculae of the thin RV wall create difficulties. A consistent approach to delineation is crucial. The RLA method to analyze global and regional wall motion is promising especially in the population of ARVC patients and their relatives, but further studies are necessary. 3. Signal- averaged electrocardiography in ARVC In the early 1980´s, SAECG was recommended in patients recovering from myocardial infarction to help determine their risk for sustained ventricular tachyarrhythmia. The presence of pathologic late potentials has been determined by criteria suggested by Breithardt et al. In post myocardial infarction patients, SAECG has a high negative predictive value between 9598%, but the positive predictive value is low, in the range of 15-22%[76]. The use of SAECG has now been expanded to other non-ischemic causes of ventricular tachyarrhythmia. In our paper I, nine of fifteen patients had late potentials (60%) at the first examination. Among these patients, five (56%) had experienced sustained ventricular tachycardia (VT). However in 3 patients (38%) with documented sustained VT, the SAECG was normal. In paper III, nine of fourteen (64%) men with ARVC had late potentials on the SAECG. In numerous series of patients with ARVC, late potentials were observed in 50 to 85% of patients [12, 136-139]. Mehta et al and Nava et al found a good correlation between the presence of late potentials and the extent of the disease, but less correlation with ventricular arrhythmia[138, 140]. In 75 members of 11 families with ARVC (both healthy and with various degree of disease), Oselladore et al. found that 91% of patients with an abnormal SAECG had the disease but only 44% of the subjects with pathologic late potentials had ventricular arrhythmia [141]. The abnormality on the SAECG appears to be correlated with the severity of the disease and does not give precise information about electrical instability in these patients [141]. In a study of the correlation between two-dimensional echocardiography parameters and SAECG in a group of thirty-three ARVC patients, Park et al. 63 63 found a pathologic SAECG in the absence of significant abnormalities on the echocardiogram (RV and LV dimension, RV fraction shortening and LVEF), suggesting that electrical late potentials may occur before detectable morphological changing on echocardiography[142]. The presence of 2 or 3 pathological parameters in SAECG has been considered a minor criterion for the diagnosis of ARVC. Marcus et al. showed that using one pathological parameter instead of two for the diagnosis of pathologic late potentials, increased the sensitivity at a slightly reduced specificity [73]. The presence of one of three pathological parameters is now accepted as criterion for the presence of late potentials in the modified Task Force Criteria for ARVC (Appendix 1). In the normal population, there is a small fraction with abnormal SAECG; 18 of 482 normal healthy (3.7%) in the study of Yakubo et al., about 4% in other studies [138, 139, 143]. As with many other measurements, the distribution of late potentials apparently overlaps between samples of healthy and sick people drawn from the population. 4. Genetics in ARVC The detection of a pathogenic mutation in a patient fulfilling the diagnostic criteria of ARVC has important implications for family members. Screening will identify relatives who are unknown mutation carriers. This enables diagnosis and facilitates prevention of possible complications. In addition, excluding a pathogenic mutation in a family member justifies ‚dismissal‛ from regular cardiological follow-up. However, pathogenic mutations are at present only identified in approximately 40-60% of ARVC patients [144], which implicates additional disease causing genes to be identified. ARVC can lead to sudden death, heart failure or have a completely asymptomatic course, probably due to effects of different mutations. However, this cannot explain variation in the disease expression between families carrying the same mutation, and among members of the same family. A suggestion that modifier genes or environmental influences contribute to the phenotype expression has been made. However, study of monozygotic twins showed different clinical expression and severity of ARVC, even if they were exposed to similar lifestyle [145]. 64 64 Discussion Mutations in the PKP2 gene described by Gerull et al. were found in up to 43% of ARVC patients, and affected family members carries mutations in up to 70% [118]. Several studies [146, 147] indicates an increased susceptibility with a lower mean age of onset for ARVC in patients carrying PKP2 mutations compared to ARVC patients with mutations in the other disease causing genes. Furthermore, a high clinical variability is sometimes reported, varying from complete lack of symptoms to a severe disease phenotype among carriers with the same mutation. The majority of affected subjects have predominant right ventricular involvement and a high degree of penetrance (66% to 100%) with a large variation in the age at the earliest manifestation of disease. The youngest patient with ARVC was 8 years old and two 15 year old patients showed advanced RV abnormalities at post-mortem [120]. In the Van Der Zwaag cohort of 53 mutation carriers, 7 (13%) persons died a SCD before age 30, while 40% did not experience any symptoms at age 60. A possible explanation for this high variability may be the presence of more than one contributing mutation, since multiple gene mutations results in a more severe phenotype and more frequent SCD [148]. However, this was not found in the population described by van der Zwaag despite analysis for other desmosomal genes. In our reported three generation family with the novel PKP 2 mutation, there was a heterogeneous expression of the disease. The mother, subject II:2, was phenotypically normal beside a positive biopsy, while her daughter III:3 and grandchild IV:1 have extensive right ventricular abnormalities. Subject III:1 was the victim of SCD (Fig. 8). Analysis of other desmosomal genes showed no other concomitant mutations. The ARVC diagnosis is difficult and clinically challenging and minor signs may escape detection, where genetic information may aid. A false-positive diagnosis in subject III:2 was first assigned, based on pathological late potentials and slight RV abnormalities on echocardiography and MRI. Syrris et al. reported 5 false positive cases in relatives, relying on wall motion abnormalities and premature ventricular beats exceeding 2000 in a 24-hour period [120]. This emphasizes the need to include genetic information in the diagnosis of ARVC as it is proposed in the modified TFC [73]. 65 65 66 66 Conlusion CONCLUSION This thesis has shown that the development of noninvasive modalities provides new insights in characteristics and diagnostics of arrhythmogenic right ventricular cardiomyopathy. The progression of echocardiographic abnormalities in patients with an established ARVC diagnosis was generally slow over an 8- year observation period but with individual exceptions. Tissue Doppler imaging contributed in diagnosis and follow-up of wall abnormalities. A new axial orientation modality in right ventricular volume assessment by MRI has shown improvement in visualisation of the basal RV. Two- dimensional strain analysis was feasible in the RV free wall as well as in the LV, at least in non advanced cases of ARVC. Longitudinal strain based on speckle tracking could be used in assessment of wall function in ARVC patients. An index combining echocardiographic measurements of dimensions and functional parameters was developed for the right and left ventricle respectively, aiming at early detection of subtle abnormalities in relatives of ARVC patients. In a family with a new mutation in the plakophilin 2 gene, we found that disease symptoms including SD occurred in young adults (below 20 years of age) with high penetrance in first degree relatives. Combining genetic testing with other clinical and imaging findings may help to enhance diagnosis in relatives. 67 67 68 68 Implications IMPLICATIONS AND FUTURE PERSPECTIVES Patients diagnosed with ARVC in our region and their first degree relatives have been subject to systematic follow-up according to a specific clinical and non-invasive protocol since the mid nineties. Integrating the results of the studies in this thesis, developed MRI and echocardiographic examination in the follow-up schedule will, in addition to improve the diagnosis for the patients and relatives, also constitute a platform for further research in the field. Detection of morphologic abnormalities will help to refine the algorithm for identification of minor deviations from normal, indicating probable phenotype expression, as well as providing a deeper knowledge of the natural history of the disease. Extended analysis to further test the strength of the developed MRI orientation, two dimensional strain as well as LV and RV echocardiographic indices are needed. It is important to further develop 3D-echocardiographic determination of RV volumes as a substantial number of patients with ARVC and their relatives are provided with a primary or secondary prophylactic ICD, which makes it difficult to use MRI for follow-up. Developing a genetic cascade screening will make it possible to focus the investigations and follow-up on those first degree relatives who are mutation carriers. Further studies of the phenotype-genotype correlation will aim at clarifying whether the rate of progression or propensity for ventricular arrhythmia can be explained by certain genetic variants. Further work is also needed to identify more of the genes that cause ARVC. In the hope of preventing SCD in ARVC, combination of genetic testing and improved diagnostic methods may create a better algorithm for risk stratification and selection to primary preventive ICD-treatment. 69 69 70 70 Appendix APPENDIX 1 Original and Revised Task Force Criteria for the diagnosis of ARVC Definite diagnosis:Two major or one major and two minor criteria, or four minor criteria, from different categories. Borderline diagnosis: One major and one minor, or three minor criteria from different categories. Possible diagnosis: One major or two minor criteria from different categories. The diagnosis of familial ARVC, in the context of proven ARVC in a firstdegree relative, is based on one of the following in a family member: T-wave inversion in right precordial leads V1, V2, and V3 in individuals over the age of 14 years. Late potentials by signal-averaged ECG (SAECG). Ventricular tachycardia of left bundle-branch block morphology on ECG, Holter monitor, or during exercise testing, or > 200 premature ventricular contractions in 24 hours. Either mild global dilatation or reduction in RV ejection fraction with normal LV or mild segmental dilatation of the RV or regional RV hypokinesis. (Modified Task Force Criteria 2010 [73] ) 71 71 72 72 Reviseted TFC Original TFC Mild global RV dilatation and/or ejection fraction with normal LV Mild segmental dilatation of the RV Regional RV hypokinesia By 2D Echo Regional RV akinesia, dyskinesia or aneurysm and 1 of the following (end diastole): PLAX RVOT ≥29 to <32mm PSAX RVOT ≥32 to <36mm Or fractional area change >33% to ≤40% By MRI Regional RV akinesia, dyskinesia or aneurysm or dyssynchronous RV contraction and one of the following: Ratio of RV end-diastolic volume to BSA ≥100 to <110 mL/m2 (male) or ≥90 to <100 mL/m2 (female) Or RV ejection fraction >40% to ≤45% Severe dilatation and reduction of RV ejection fraction with no (or only mild) LV impairment Localized RV aneurysms (akinetic or dyskinetic areas with diastolic bulging) Severe segmental dilatation of the RV By 2D Echo: Regional RV akinesia, dyskinesia or aneurysm and 1 of the following (end diastole): PLAX RVOT ≥32mm PSAX RVOT ≥36mm Or fractional area change ≤33% By MRI: Regional RV akinesia, dyskinesia or aneurysm or dyssynchronous RV contraction and one of the following: Ratio of RV end-diastolic volume to BSA ≥110 mL/m2 (male) or ≥100 mL/m2 (female) Or RV ejection fraction ≤40% By RV angiography: Regional RV akinesia, dyskinesia or aneurysm Minor Major 1. Global or regional dysfunction and structural alterations Fibrofatty replacement of myocardium on endomyocardial biopsy Residual myocytes <60% by morphometric analysis (or <50% if estimated), with fibrous replacement of the RV free wall myocardium in ≥1 sample, with or without fatty replacement of tissue on endomyocardial biopsy Original TFC Reviseted TFC Major Minor Residual myocytes 60% to 75% by morphometric analysis (or 50% to 65% if estimated), with fibrous replacement of the RV free wall myocardium in ≥1 sample, with or without fatty replacement of tissue on endomyocardial biopsy 2. Tissue characterization of wall Appendix 73 73 74 74 Reviseted TFC Original TFC Inverted T waves in right precordial leads (V1, V2 and V3) or beyond in individuals >14 years of age (in the absence of complete right bundle-branch block, QRS ≥120 ms) Major Minor Inverted T waves in leads V1, V2, V3, and V4 in individuals >14 years of age in the presence of complete right bundle-branch block Inverted T waves in leads V1 and V2 in individuals >14 years of age (in the absence of complete right bundle-branch block) or in V4, V5, or V6 Inverted T waves in right precordial leads (V2 and V3) (people age >12 years, in absence of right bundlebranch block) 3. Repolarization abnormalities Reviseted TFC Original TFC Late potentials (SAECG) Late potentials by SAECG in ≥1 of 3 parameters in the absence of a QRS duration of ≥110 ms on the standard ECG Filtered QRS duration (fQRS) ≥114 ms Duration of terminal QRS <40 microV (lowamplitude signal duration) ≥38 ms Root-mean-square voltage of terminal 40 ms ≤20 microV Terminal activation duration of QRS ≥55 ms measured from the nadir of the S wave to the end of the QRS, including R’, in V1, V2, or V3, in the absence of complete right bundle-branch block Epsilon wave (reproducible low-amplitude signals between end of QRS complex to onset of the T wave) in the right precordial leads (V1 to V3) Minor Epsilon waves or localized prolongation (>110 ms) of the QRS complex in right precordial leads (V1 to V3) Major 4. Depolarization/conduction abnormalities Appendix 75 75 76 76 Reviseted TFC Original TFC Nonsustained or sustained ventricular tachycardia of left bundle-branch morphology with superior axis (negative or indeterminate QRS in leads II, III, and aVF and positive in lead aVL) Major Minor Nonsustained or sustained ventricular tachycardia of RV outflow configuration, left bundle-branch block morphology with inferior axis (positive QRS in leads II, III, and aVF and negative in lead aVL) or of unknown axis >500 ventricular extrasystoles per 24 hours (Holter) on Holter). Left bundle-branch block–type ventricular tachycardia (sustained and nonsustained) (ECG, Holter, exercise) Frequent ventricular extrasystoles (>1000 per 24 hours 5. Arrhythmias Reviseted TFC Original TFC History of ARVC/D in a first-degree relative in whom it is not possible or practical to determine whether the family member meets current Task Force criteria Premature sudden death (<35 years of age) due to suspected ARVC/D in a first-degree relative ARVC/D confirmed pathologically or by current Task Force Criteria in second-degree relative Familial disease confirmed at necropsy or surgery ARVC/D confirmed in a first-degree relative who meets current Task Force criteria ARVC/D confirmed pathologically at autopsy or surgery in a first-degree relative Identification of a pathogenic mutation categorized as associated or probably associated with ARVC/D in the patient under evaluation. Minor Family history of premature sudden death (<35 years of age) due to suspected ARVC/D Familial history (clinical diagnosis (based on present criteria) Major 6. Family History Appendix 77 77 78 78 Acknowledgements ACKNOWLEDGEMENTS This thesis would not have been possible without the contribution and support from colleagues, friends and family. I would like to thank all of you. I would like to express a special gratitude to: Eva Nylander, professor and my supervisor, for always trusting my ability. I am heartily thankful for your encouragement and guidance making this work possible. Your great scientific knowledge and valuable discussions have been an enormous source of inspiration for me. Jan Engvall, associate professor and my co-supervisor, for support and constructive criticism in all the parts of the research process. I am deeply grateful for your presence in difficult times and also for all help with the English language. Thank you Jan! Lena Lindström, PhD, colleague and co-author, for introducing me into the mysteries of the right ventricle and ARVC. Christina Fluur, Lars Brudin, Tino Ebbers, Cecilia Gunnarsson and Peter Söderkvist and Malin Rehnberg co-authors for contributions in the studies and valuable discussions. Gudrun Lövdahl, sonographer, for the skilful technical and administrative assistance during all these years. Inger Ekman, sonographer, for valuable help with echocardiography and measurements of reproducibility, and Elin Wistrand, administrative assistant, for help and support in many ways. 79 79 My colleagues at the Department of Clinical Physiology, for providing a positive working climate. I want to thank you for substituting for me in the daily clinical work when I was absent for research. Jan Ohlsson, associate professor, and Pearl Ohlson, for revising my English. Kjell Jansson and Birgitta Janerot Sjöberg , present and former head of the Department of Clinical Physiology, Linköping, for enabling me to focus on the research and writing the thesis. My friends from near and far, for keeping the social life alive and pleasant. Ouafa and Zineb for the great time together. Mother, for the unequivocal love and support throughout, as always, for which my mere expression of thanks likewise does not suffice. Fatiha, my sister, for the support despite the long distance between us. Thank you for the encouragement and for all laughs. At last but absolutely not least, Linda and Jasmine, my wonderful girls. For enduring the evenings with a mother behind a computer instead of being with you. You brighten my life. Peter, my husband for great support and love. Financial support was obtained from ALF Grants, County Council of Östergötland, the Swedish Heart- Lung foundation, the Medical Research Council of Southeast Sweden, FORSS, the Carldavid Jönsson Foundation, the Stina and Birger Johansson Foundation and the Swedish Council for Research in Sports 80 80 81 81 82 82 References REFERENCES 1. 2. 3. 4. 5. 6. 7. 8. Zipes DP, Wellens HJ: Sudden cardiac death. Circulation 1998, 98(21):23342351. Priori SG, Aliot E, Blomstrom-Lundqvist C, Bossaert L, Breithardt G, Brugada P, Camm AJ, Cappato R, Cobbe SM, Di Mario C et al: Task Force on Sudden Cardiac Death of the European Society of Cardiology. Eur Heart J 2001, 22(16):1374-1450. Baskett PJ, Steen PA, Bossaert L: European Resuscitation Council guidelines for resuscitation 2005. Section 8. The ethics of resuscitation and end-of-life decisions. Resuscitation 2005, 67 Suppl 1:S171-180. Atwood C, Eisenberg MS, Herlitz J, Rea TD: Incidence of EMS-treated out-of-hospital cardiac arrest in Europe. Resuscitation 2005, 67(1):75-80. Goldberger JJ, Cain ME, Hohnloser SH, Kadish AH, Knight BP, Lauer MS, Maron BJ, Page RL, Passman RS, Siscovick D et al: American Heart Association/american College of Cardiology Foundation/heart Rhythm Society scientific statement on noninvasive risk stratification techniques for identifying patients at risk for sudden cardiac death: a scientific statement from the American Heart Association Council on Clinical Cardiology Committee on Electrocardiography and Arrhythmias and Council on Epidemiology and Prevention. Heart Rhythm 2008, 5(10):e1-21. Pratt CM, Greenway PS, Schoenfeld MH, Hibben ML, Reiffel JA: Exploration of the precision of classifying sudden cardiac death. Implications for the interpretation of clinical trials. Circulation 1996, 93(3):519-524. Corrado D, Basso C, Thiene G, McKenna WJ, Davies MJ, Fontaliran F, Nava A, Silvestri F, Blomstrom-Lundqvist C, Wlodarska EK et al: Spectrum of clinicopathologic manifestations of arrhythmogenic right ventricular cardiomyopathy/dysplasia: a multicenter study. J Am Coll Cardiol 1997, 30(6):1512-1520. Merner ND, Hodgkinson KA, Haywood AF, Connors S, French VM, Drenckhahn JD, Kupprion C, Ramadanova K, Thierfelder L, McKenna W et al: Arrhythmogenic right ventricular cardiomyopathy type 5 is a fully penetrant, lethal arrhythmic disorder caused by a missense mutation in the TMEM43 gene. Am J Hum Genet 2008, 82(4):809-821. 83 83 9. 10. 11. 12. 13. 14. 15. 16. 17. 18. Tabib A, Loire R, Chalabreysse L, Meyronnet D, Miras A, Malicier D, Thivolet F, Chevalier P, Bouvagnet P: Circumstances of death and gross and microscopic observations in a series of 200 cases of sudden death associated with arrhythmogenic right ventricular cardiomyopathy and/or dysplasia. Circulation 2003, 108(24):3000-3005. Peters S: Advances in the diagnostic management of arrhythmogenic right ventricular dysplasia-cardiomyopathy. Int J Cardiol 2006, 113(1):411. Frank R, Fontaine G, Vedel J, Mialet G, Sol C, Guiraudon G, Grosgogeat Y: [Electrocardiology of 4 cases of right ventricular dysplasia inducing arrhythmia]. Arch Mal Coeur Vaiss 1978, 71(9):963-972. Marcus FI, Fontaine GH, Guiraudon G, Frank R, Laurenceau JL, Malergue C, Grosgogeat Y: Right ventricular dysplasia: a report of 24 adult cases. Circulation 1982, 65(2):384-398. Hamid MS, Norman M, Quraishi A, Firoozi S, Thaman R, Gimeno JR, Sachdev B, Rowland E, Elliott PM, McKenna WJ: Prospective evaluation of relatives for familial arrhythmogenic right ventricular cardiomyopathy/dysplasia reveals a need to broaden diagnostic criteria. J Am Coll Cardiol 2002, 40(8):1445-1450. Sen-Chowdhry S, Lowe MD, Sporton SC, McKenna WJ: Arrhythmogenic right ventricular cardiomyopathy: clinical presentation, diagnosis, and management. Am J Med 2004, 117(9):685-695. Protonotarios N, Tsatsopoulou A, Fontaine G: Naxos disease: keratoderma, scalp modifications, and cardiomyopathy. J Am Acad Dermatol 2001, 44(2):309-311. Omae A, Katayama K, Kakiuchi Y, Okada N, Hijioka Y, Nagai Y, Ito Y, Hagiwara H, Kasahara A, Hayashi N et al: [A case of ventricular tachycardia occurred during interferon therapy in chronic hepatitis C]. Nippon Naika Gakkai Zasshi 1995, 84(10):1734-1735. Hayashi M, Denjoy I, Extramiana F, Maltret A, Buisson NR, Lupoglazoff JM, Klug D, Takatsuki S, Villain E, Kamblock J et al: Incidence and risk factors of arrhythmic events in catecholaminergic polymorphic ventricular tachycardia. Circulation 2009, 119(18):2426-2434. Liu N, Colombi B, Memmi M, Zissimopoulos S, Rizzi N, Negri S, Imbriani M, Napolitano C, Lai FA, Priori SG: Arrhythmogenesis in catecholaminergic polymorphic ventricular tachycardia: insights from a RyR2 R4496C knock-in mouse model. Circ Res 2006, 99(3):292-298. 84 84 References 19. Sen-Chowdhry S, Syrris P, McKenna WJ: Role of genetic analysis in the management of patients with arrhythmogenic right ventricular dysplasia/cardiomyopathy. J Am Coll Cardiol 2007, 50(19):1813-1821. 20. Beffagna G, Occhi G, Nava A, Vitiello L, Ditadi A, Basso C, Bauce B, Carraro G, Thiene G, Towbin JA et al: Regulatory mutations in transforming growth factor-beta3 gene cause arrhythmogenic right ventricular cardiomyopathy type 1. Cardiovasc Res 2005, 65(2):366-373. 21. Xu T, Yang Z, Vatta M, Rampazzo A, Beffagna G, Pilichou K, Scherer SE, Saffitz J, Kravitz J, Zareba W et al: Compound and digenic heterozygosity contributes to arrhythmogenic right ventricular cardiomyopathy. J Am Coll Cardiol 2010, 55(6):587-597. 22. Basso C, Thiene G, Corrado D, Angelini A, Nava A, Valente M: Arrhythmogenic right ventricular cardiomyopathy. Dysplasia, dystrophy, or myocarditis? Circulation 1996, 94(5):983-991. 23. Calabrese F, Basso C, Carturan E, Valente M, Thiene G: Arrhythmogenic right ventricular cardiomyopathy/dysplasia: is there a role for viruses? Cardiovasc Pathol 2006, 15(1):11-17. 24. Grumbach IM, Heim A, Vonhof S, Stille-Siegener M, Mall G, Gonska BD, Kreuzer H, Andreas S, Figulla HR: Coxsackievirus genome in myocardium of patients with arrhythmogenic right ventricular dysplasia/cardiomyopathy. Cardiology 1998, 89(4):241-245. 25. Mallat Z, Tedgui A, Fontaliran F, Frank R, Durigon M, Fontaine G: Evidence of apoptosis in arrhythmogenic right ventricular dysplasia. N Engl J Med 1996, 335(16):1190-1196. 26. Valente M, Calabrese F, Thiene G, Angelini A, Basso C, Nava A, Rossi L: In vivo evidence of apoptosis in arrhythmogenic right ventricular cardiomyopathy. Am J Pathol 1998, 152(2):479-484. 27. Lindstrom L, Nylander E, Larsson H, Wranne B: Left ventricular involvement in arrhythmogenic right ventricular cardiomyopathy - a scintigraphic and echocardiographic study. Clin Physiol Funct Imaging 2005, 25(3):171-177. 28. Sen-Chowdhry S, Syrris P, Ward D, Asimaki A, Sevdalis E, McKenna WJ: Clinical and genetic characterization of families with arrhythmogenic right ventricular dysplasia/cardiomyopathy provides novel insights into patterns of disease expression. Circulation 2007, 115(13):1710-1720. 29. Peters S: Left ventricular impairment in arrhythmogenic right ventricular dysplasia: what we can learn from angiography. Cardiology 1995, 86(6):473-476. 85 85 30. Basso C, Thiene G: Adipositas cordis, fatty infiltration of the right ventricle, and arrhythmogenic right ventricular cardiomyopathy. Just a matter of fat? Cardiovasc Pathol 2005, 14(1):37-41. 31. Thiene G, Basso C, Angelini A, Calabrese F, Valente M: Pathomorphological aspects of arrhythmogenic right ventricular cardiomyopathy. G Ital Cardiol 1999, 29(6):719-729. 32. Ferreira AC, Garcia SA, Pasquale MA, Canoniero MJ, Peter A: Arrhythmogenic right ventricular dysplasia in the elderly. Heart Dis 2003, 5(6):393-396. 33. Wang SS, Zhang ZW, Xu YM, Jiang QP, Li H, Qian MY, Li YF: [Diagnosis and treatment of arrhythmogenic right ventricular cardiomyopathy in children]. Zhongguo Dang Dai Er Ke Za Zhi 2010, 12(3):165-168. 34. Bauce B, Frigo G, Marcus FI, Basso C, Rampazzo A, Maddalena F, Corrado D, Winnicki M, Daliento L, Rigato I et al: Comparison of clinical features of arrhythmogenic right ventricular cardiomyopathy in men versus women. Am J Cardiol 2008, 102(9):1252-1257. 35. McKenna WJ, Thiene G, Nava A, Fontaliran F, Blomstrom-Lundqvist C, Fontaine G, Camerini F: Diagnosis of arrhythmogenic right ventricular dysplasia/cardiomyopathy. Task Force of the Working Group Myocardial and Pericardial Disease of the European Society of Cardiology and of the Scientific Council on Cardiomyopathies of the International Society and Federation of Cardiology. Br Heart J 1994, 71(3):215-218. 36. Sen-Chowdhry S, Syrris P, Prasad SK, Hughes SE, Merrifield R, Ward D, Pennell DJ, McKenna WJ: Left-dominant arrhythmogenic cardiomyopathy: an under-recognized clinical entity. J Am Coll Cardiol 2008, 52(25):2175-2187. 37. Coats CJ, Quarta G, Flett AS, Pantazis AA, McKenna WJ, Moon JC: Arrhythmogenic left ventricular cardiomyopathy. Circulation 2009, 120(25):2613-2614. 38. Nava A, Bauce B, Basso C, Muriago M, Rampazzo A, Villanova C, Daliento L, Buja G, Corrado D, Danieli GA et al: Clinical profile and long-term follow-up of 37 families with arrhythmogenic right ventricular cardiomyopathy. J Am Coll Cardiol 2000, 36(7):2226-2233. 39. Marcus FI, Zareba W, Calkins H, Towbin JA, Basso C, Bluemke DA, Estes NA, 3rd, Picard MH, Sanborn D, Thiene G et al: Arrhythmogenic right ventricular cardiomyopathy/dysplasia clinical presentation and diagnostic evaluation: results from the North American Multidisciplinary Study. Heart Rhythm 2009, 6(7):984-992. 86 86 References 40. Marcus FI: Prevalence of T-wave inversion beyond V1 in young normal individuals and usefulness for the diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia. Am J Cardiol 2005, 95(9):10701071. 41. Piccini JP, Nasir K, Bomma C, Tandri H, Dalal D, Tichnell C, James C, Crosson J, Calkins H: Electrocardiographic findings over time in arrhythmogenic right ventricular dysplasia/cardiomyopathy. Am J Cardiol 2005, 96(1):122-126. 42. Nasir K, Bomma C, Tandri H, Roguin A, Dalal D, Prakasa K, Tichnell C, James C, Spevak PJ, Marcus F et al: Electrocardiographic features of arrhythmogenic right ventricular dysplasia/cardiomyopathy according to disease severity: a need to broaden diagnostic criteria. Circulation 2004, 110(12):1527-1534. 43. Hurst JW: Naming of the waves in the ECG, with a brief account of their genesis. Circulation 1998, 98(18):1937-1942. 44. Peters S, Trummel M, Koehler B, Westermann KU: The value of different electrocardiographic depolarization criteria in the diagnosis of arrhythmogenic right ventricular dysplasia/cardiomyopathy. J Electrocardiol 2007, 40(1):34-37. 45. Cox MG, van der Smagt JJ, Wilde AA, Wiesfeld AC, Atsma DE, Nelen MR, Rodriguez LM, Loh P, Cramer MJ, Doevendans PA et al: New ECG criteria in arrhythmogenic right ventricular dysplasia/cardiomyopathy. Circ Arrhythm Electrophysiol 2009, 2(5):524530. 46. Nasir K, Rutberg J, Tandri H, Berger R, Tomaselli G, Calkins H: Utility of SAECG in arrhythmogenic right ventricle dysplasia. Ann Noninvasive Electrocardiol 2003, 8(2):112-120. 47. Cox MG, Nelen MR, Wilde AA, Wiesfeld AC, van der Smagt JJ, Loh P, Cramer MJ, Doevendans PA, van Tintelen JP, de Bakker JM et al: Activation delay and VT parameters in arrhythmogenic right ventricular dysplasia/cardiomyopathy: toward improvement of diagnostic ECG criteria. J Cardiovasc Electrophysiol 2008, 19(8):775-781. 48. Sequeira IB, Kirsh JA, Hamilton RM, Russell JL, Gross GJ: Utility of exercise testing in children and teenagers with arrhythmogenic right ventricular cardiomyopathy. Am J Cardiol 2009, 104(3):411-413. 49. Yoerger DM, Marcus F, Sherrill D, Calkins H, Towbin JA, Zareba W, Picard MH: Echocardiographic findings in patients meeting task force criteria for arrhythmogenic right ventricular dysplasia: new insights 87 87 50. 51. 52. 53. 54. 55. 56. 57. 58. from the multidisciplinary study of right ventricular dysplasia. J Am Coll Cardiol 2005, 45(6):860-865. Woodard PK, Bluemke DA, Cascade PN, Finn JP, Stillman AE, Higgins CB, White RD, Yucel EK: ACR practice guideline for the performance and interpretation of cardiac magnetic resonance imaging (MRI). J Am Coll Radiol 2006, 3(9):665-676. Tandri H, Bomma C, Calkins H, Bluemke DA: Magnetic resonance and computed tomography imaging of arrhythmogenic right ventricular dysplasia. J Magn Reson Imaging 2004, 19(6):848-858. Bomma C, Rutberg J, Tandri H, Nasir K, Roguin A, Tichnell C, Rodriguez R, James C, Kasper E, Spevak P et al: Misdiagnosis of arrhythmogenic right ventricular dysplasia/cardiomyopathy. J Cardiovasc Electrophysiol 2004, 15(3):300-306. Kimura F, Sakai F, Sakomura Y, Fujimura M, Ueno E, Matsuda N, Kasanuki H, Mitsuhashi N: Helical CT features of arrhythmogenic right ventricular cardiomyopathy. Radiographics 2002, 22(5):1111-1124. Blomstrom-Lundqvist C, Selin K, Jonsson R, Johansson SR, Schlossman D, Olsson SB: Cardioangiographic findings in patients with arrhythmogenic right ventricular dysplasia. Br Heart J 1988, 59(5):556563. Boulos M, Lashevsky I, Gepstein L: Usefulness of electroanatomical mapping to differentiate between right ventricular outflow tract tachycardia and arrhythmogenic right ventricular dysplasia. Am J Cardiol 2005, 95(8):935-940. Corrado D, Basso C, Leoni L, Tokajuk B, Bauce B, Frigo G, Tarantini G, Napodano M, Turrini P, Ramondo A et al: Three-dimensional electroanatomic voltage mapping increases accuracy of diagnosing arrhythmogenic right ventricular cardiomyopathy/dysplasia. Circulation 2005, 111(23):3042-3050. Ladyjanskaia GA, Basso C, Hobbelink MG, Kirkels JH, Lahpor JR, Cramer MJ, Thiene G, Hauer RN, MF VO: Sarcoid myocarditis with ventricular tachycardia mimicking ARVD/C. J Cardiovasc Electrophysiol 2010, 21(1):94-98. Ventura R, Steven D, Klemm HU, Lutomsky B, Mullerleile K, Rostock T, Servatius H, Risius T, Meinertz T, Kuck KH et al: Decennial follow-up in patients with recurrent tachycardia originating from the right ventricular outflow tract: electrophysiologic characteristics and response to treatment. Eur Heart J 2007, 28(19):2338-2345. 88 88 References 59. Schmidt T, Gerckens U, Ortmeyer D, Bootsveld A, Lampe E, Grube E: [Brugada syndrome or ARVD (arrhythmogenic right ventricular dysplasia) or both? Significance and value of right precordial ECG changes]. Z Kardiol 2002, 91(5):416-422. 60. Peters S: Arrhythmogenic right ventricular dysplasia-cardiomyopathy and provocable coved-type ST-segment elevation in right precordial leads: clues from long-term follow-up. Europace 2008, 10(7):816-820. 61. Hisaoka T, Kawai S, Ohi H, Ishijima M, Okada R, Hayashida N, Saiki S, Kobayashi H, Yoshimura H: Two cases of chronic myocarditis mimicking arrhythmogenic right ventricular dysplasia. Heart Vessels Suppl 1990, 5:51-54. 62. Michaels PJ, Kobashigawa JA, Child JS, Fishbein MC: Chronic right-sided myocarditis mimicking arrhythmogenic right ventricular dysplasia. Hum Pathol 2000, 31(5):618-621. 63. Maron BJ, Pelliccia A: The heart of trained athletes: cardiac remodeling and the risks of sports, including sudden death. Circulation 2006, 114(15):1633-1644. 64. Bauce B, Frigo G, Benini G, Michieli P, Basso C, Folino AF, Rigato I, Mazzotti E, Daliento L, Thiene G et al: Differences and similarities between arrhythmogenic right ventricular cardiomyopathy and athlete's heart adaptations. Br J Sports Med 2010, 44(2):148-154. 65. Pelliccia A, Zipes DP, Maron BJ: Bethesda Conference #36 and the European Society of Cardiology Consensus Recommendations revisited a comparison of U.S. and European criteria for eligibility and disqualification of competitive athletes with cardiovascular abnormalities. J Am Coll Cardiol 2008, 52(24):1990-1996. 66. Maron BJ, Chaitman BR, Ackerman MJ, Bayes de Luna A, Corrado D, Crosson JE, Deal BJ, Driscoll DJ, Estes NA, 3rd, Araujo CG et al: Recommendations for physical activity and recreational sports participation for young patients with genetic cardiovascular diseases. Circulation 2004, 109(22):2807-2816. 67. Maron BJ, Mitten MJ, Quandt EF, Zipes DP: Competitive athletes with cardiovascular disease--the case of Nicholas Knapp. N Engl J Med 1998, 339(22):1632-1635. 68. Basso C, Wichter T, Danieli GA, Corrado D, Czarnowska E, Fontaine G, McKenna WJ, Nava A, Protonotarios N, Antoniades L et al: Arrhythmogenic right ventricular cardiomyopathy: clinical registry and database, evaluation of therapies, pathology registry, DNA banking. Eur Heart J 2004, 25(6):531-534. 89 89 69. Roguin A, Bomma CS, Nasir K, Tandri H, Tichnell C, James C, Rutberg J, Crosson J, Spevak PJ, Berger RD et al: Implantable cardioverterdefibrillators in patients with arrhythmogenic right ventricular dysplasia/cardiomyopathy. J Am Coll Cardiol 2004, 43(10):1843-1852. 70. Wichter T, Paul M, Wollmann C, Acil T, Gerdes P, Ashraf O, Tjan TD, Soeparwata R, Block M, Borggrefe M et al: Implantable cardioverter/defibrillator therapy in arrhythmogenic right ventricular cardiomyopathy: single-center experience of long-term follow-up and complications in 60 patients. Circulation 2004, 109(12):1503-1508. 71. Piccini JP, Dalal D, Roguin A, Bomma C, Cheng A, Prakasa K, Dong J, Tichnell C, James C, Russell S et al: Predictors of appropriate implantable defibrillator therapies in patients with arrhythmogenic right ventricular dysplasia. Heart Rhythm 2005, 2(11):1188-1194. 72. Corrado D, Calkins H, Link MS, Leoni L, Favale S, Bevilacqua M, Basso C, Ward D, Boriani G, Ricci R et al: Prophylactic implantable defibrillator in patients with arrhythmogenic right ventricular cardiomyopathy/dysplasia and no prior ventricular fibrillation or sustained ventricular tachycardia. Circulation 2010, 122(12):1144-1152. 73. Marcus FI, McKenna WJ, Sherrill D, Basso C, Bauce B, Bluemke DA, Calkins H, Corrado D, Cox MG, Daubert JP et al: Diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia: proposed modification of the task force criteria. Circulation 2010, 121(13):15331541. 74. Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise JS et al: Recommendations for chamber quantification: a report from the American Society of Echocardiography's Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 2005, 18(12):1440-1463. 75. Kaul S, Tei C, Hopkins JM, Shah PM: Assessment of right ventricular function using two-dimensional echocardiography. Am Heart J 1984, 107(3):526-531. 76. Breithardt G, Cain ME, el-Sherif N, Flowers N, Hombach V, Janse M, Simson MB, Steinbeck G: Standards for analysis of ventricular late potentials using high resolution or signal-averaged electrocardiography. A statement by a Task Force Committee between the European Society of Cardiology, the American Heart Association 90 90 References 77. 78. 79. 80. 81. 82. 83. 84. 85. 86. 87. 88. and the American College of Cardiology. Eur Heart J 1991, 12(4):473480. Cain M, Anderson J, Arnsdore M, Mason J, Scheinman M, Waldo A: Signal-averaged electrocardiography. J Am Coll Cardiol 1996, 27(1):238249. Baskett SJ, Henager J: Differentiating between post-Vietnam syndrome and preexisting psychiatric disorders. South Med J 1983, 76(8):988-990. BLAND DGAaJM: Measurement in Medicine: the Analysis of Method Comparison Studies. The Statistician 1983, 32:307-317. G D: Statistical methods for medical and biological students, 2nd edition edn. London; 1940. Sade RM, Castaneda AR: The dispensable right ventricle. Surgery 1975, 77(5):624-631. Kjaergaard J, Akkan D, Iversen KK, Kober L, Torp-Pedersen C, Hassager C: Right ventricular dysfunction as an independent predictor of shortand long-term mortality in patients with heart failure. Eur J Heart Fail 2007, 9(6-7):610-616. Morrison D, Goldman S, Wright AL, Henry R, Sorenson S, Caldwell J, Ritchie J: The effect of pulmonary hypertension on systolic function of the right ventricle. Chest 1983, 84(3):250-257. Chung T, Emmett L, Mansberg R, Peters M, Kritharides L: Natural history of right ventricular dysfunction after acute pulmonary embolism. J Am Soc Echocardiogr 2007, 20(7):885-894. Zhou S, Tan AY, Paz O, Ogawa M, Chou CC, Hayashi H, Nihei M, Fishbein MC, Chen LS, Lin SF et al: Antiarrhythmic effects of beta3adrenergic receptor stimulation in a canine model of ventricular tachycardia. Heart Rhythm 2008, 5(2):289-297. Gewirtz H, Gold HK, Fallon JT, Pasternak RC, Leinbach RC: Role of right ventricular infarction in cardiogenic shock associated with inferior myocardial infarction. Br Heart J 1979, 42(6):719-725. Goldstein JA, Vlahakes GJ, Verrier ED, Schiller NB, Tyberg JV, Ports TA, Parmley WW, Chatterjee K: The role of right ventricular systolic dysfunction and elevated intrapericardial pressure in the genesis of low output in experimental right ventricular infarction. Circulation 1982, 65(3):513-522. Gavazzi A, Berzuini C, Campana C, Inserra C, Ponzetta M, Sebastiani R, Ghio S, Recusani F: Value of right ventricular ejection fraction in predicting short-term prognosis of patients with severe chronic heart failure. J Heart Lung Transplant 1997, 16(7):774-785. 91 91 89. Borer JS, Hochreiter CA, Supino PG, Herrold EM, Krieger KH, Isom OW: Importance of right ventricular performance measurement in selecting asymptomatic patients with mitral regurgitation for valve surgery. Adv Cardiol 2002, 39:144-152. 90. Nagel E, Stuber M, Hess OM: Importance of the right ventricle in valvular heart disease. Eur Heart J 1996, 17(6):829-836. 91. Polak JF, Holman BL, Wynne J, Colucci WS: Right ventricular ejection fraction: an indicator of increased mortality in patients with congestive heart failure associated with coronary artery disease. J Am Coll Cardiol 1983, 2(2):217-224. 92. Sheehan FH, Kilner PJ, Sahn DJ, Vick GW, 3rd, Stout KK, Ge S, Helbing WA, Lewin M, Shurman AJ, Buechel EV et al: Accuracy of knowledgebased reconstruction for measurement of right ventricular volume and function in patients with tetralogy of Fallot. Am J Cardiol 2010, 105(7):993-999. 93. Alpert JS: The effect of right ventricular dysfunction on left ventricular form and function. Chest 2001, 119(6):1632-1633. 94. Dell'Italia LJ: The right ventricle: anatomy, physiology, and clinical importance. Curr Probl Cardiol 1991, 16(10):653-720. 95. Torrent-Guasp F, Ballester M, Buckberg GD, Carreras F, Flotats A, Carrio I, Ferreira A, Samuels LE, Narula J: Spatial orientation of the ventricular muscle band: physiologic contribution and surgical implications. J Thorac Cardiovasc Surg 2001, 122(2):389-392. 96. Loukas M, Tubbs RS, Louis RG, Jr., Apaydin N, Bartczak A, Huseng V, Alsaiegh N, Fudalej M: An endoscopic and anatomical approach to the septal papillary muscle of the conus. Surg Radiol Anat 2009, 31(9):701706. 97. Ho SY, Nihoyannopoulos P: Anatomy, echocardiography, and normal right ventricular dimensions. Heart 2006, 92 Suppl 1:i2-13. 98. Anderson RH, Razavi R, Taylor AM: Cardiac anatomy revisited. J Anat 2004, 205(3):159-177. 99. Brown KA, Ditchey RV: Human right ventricular end-systolic pressurevolume relation defined by maximal elastance. Circulation 1988, 78(1):81-91. 100. Redington AN, Gray HH, Hodson ME, Rigby ML, Oldershaw PJ: Characterisation of the normal right ventricular pressure-volume relation by biplane angiography and simultaneous micromanometer pressure measurements. Br Heart J 1988, 59(1):23-30. 92 92 References 101. 102. 103. 104. 105. 106. 107. 108. 109. 110. Ueti OM, Camargo EE, Ueti Ade A, de Lima-Filho EC, Nogueira EA: Assessment of right ventricular function with Doppler echocardiographic indices derived from tricuspid annular motion: comparison with radionuclide angiography. Heart 2002, 88(3):244-248. Hedman A, Alam M, Zuber E, Nordlander R, Samad BA: Decreased right ventricular function after coronary artery bypass grafting and its relation to exercise capacity: a tricuspid annular motion-based study. J Am Soc Echocardiogr 2004, 17(2):126-131. Alam M, Wardell J, Andersson E, Samad BA, Nordlander R: Right ventricular function in patients with first inferior myocardial infarction: assessment by tricuspid annular motion and tricuspid annular velocity. Am Heart J 2000, 139(4):710-715. Tei C, Pilgrim JP, Shah PM, Ormiston JA, Wong M: The tricuspid valve annulus: study of size and motion in normal subjects and in patients with tricuspid regurgitation. Circulation 1982, 66(3):665-671. Kukulski T, Hubbert L, Arnold M, Wranne B, Hatle L, Sutherland GR: Normal regional right ventricular function and its change with age: a Doppler myocardial imaging study. J Am Soc Echocardiogr 2000, 13(3):194-204. Ghio S, Recusani F, Klersy C, Sebastiani R, Laudisa ML, Campana C, Gavazzi A, Tavazzi L: Prognostic usefulness of the tricuspid annular plane systolic excursion in patients with congestive heart failure secondary to idiopathic or ischemic dilated cardiomyopathy. Am J Cardiol 2000, 85(7):837-842. Samad BA, Alam M, Jensen-Urstad K: Prognostic impact of right ventricular involvement as assessed by tricuspid annular motion in patients with acute myocardial infarction. Am J Cardiol 2002, 90(7):778781. Saxena N, Rajagopalan N, Edelman K, Lopez-Candales A: Tricuspid annular systolic velocity: a useful measurement in determining right ventricular systolic function regardless of pulmonary artery pressures. Echocardiography 2006, 23(9):750-755. Thohan V: Prognostic implications of echocardiography in advanced heart failure. Curr Opin Cardiol 2004, 19(3):238-249. Meluzin J, Spinarova L, Bakala J, Toman J, Krejci J, Hude P, Kara T, Soucek M: Pulsed Doppler tissue imaging of the velocity of tricuspid annular systolic motion; a new, rapid, and non-invasive method of evaluating right ventricular systolic function. Eur Heart J 2001, 22(4):340-348. 93 93 111. 112. 113. 114. 115. 116. 117. 118. 119. Wahl A, Praz F, Schwerzmann M, Bonel H, Koestner SC, Hullin R, Schmid JP, Stuber T, Delacretaz E, Hess OM et al: Assessment of right ventricular systolic function: Comparison between cardiac magnetic resonance derived ejection fraction and pulsed-wave tissue Doppler imaging of the tricuspid annulus. Int J Cardiol 2010. Kjaergaard J, Snyder EM, Hassager C, Oh JK, Johnson BD: Impact of preload and afterload on global and regional right ventricular function and pressure: a quantitative echocardiography study. J Am Soc Echocardiogr 2006, 19(5):515-521. Bohs LN, Trahey GE: A novel method for angle independent ultrasonic imaging of blood flow and tissue motion. IEEE Trans Biomed Eng 1991, 38(3):280-286. Korinek J, Wang J, Sengupta PP, Miyazaki C, Kjaergaard J, McMahon E, Abraham TP, Belohlavek M: Two-dimensional strain--a Dopplerindependent ultrasound method for quantitation of regional deformation: validation in vitro and in vivo. J Am Soc Echocardiogr 2005, 18(12):1247-1253. Fraser AG, Payne N, Madler CF, Janerot-Sjoberg B, Lind B, GrocottMason RM, Ionescu AA, Florescu N, Wilkenshoff U, Lancellotti P et al: Feasibility and reproducibility of off-line tissue Doppler measurement of regional myocardial function during dobutamine stress echocardiography. Eur J Echocardiogr 2003, 4(1):43-53. Lindqvist P, Waldenstrom A, Henein M, Morner S, Kazzam E: Regional and global right ventricular function in healthy individuals aged 2090 years: a pulsed Doppler tissue imaging study: Umea General Population Heart Study. Echocardiography 2005, 22(4):305-314. Cardim N, Oliveira AG, Longo S, Ferreira T, Pereira A, Reis RP, Correia JM: Doppler tissue imaging: regional myocardial function in hypertrophic cardiomyopathy and in athlete's heart. J Am Soc Echocardiogr 2003, 16(3):223-232. Gerull B, Heuser A, Wichter T, Paul M, Basson CT, McDermott DA, Lerman BB, Markowitz SM, Ellinor PT, MacRae CA et al: Mutations in the desmosomal protein plakophilin-2 are common in arrhythmogenic right ventricular cardiomyopathy. Nat Genet 2004, 36(11):1162-1164. Bauce B, Basso C, Rampazzo A, Beffagna G, Daliento L, Frigo G, Malacrida S, Settimo L, Danieli G, Thiene G et al: Clinical profile of four families with arrhythmogenic right ventricular cardiomyopathy caused by dominant desmoplakin mutations. Eur Heart J 2005, 26(16):1666-1675. 94 94 References 120. 121. 122. 123. 124. 125. 126. 127. 128. 129. Syrris P, Ward D, Asimaki A, Evans A, Sen-Chowdhry S, Hughes SE, McKenna WJ: Desmoglein-2 mutations in arrhythmogenic right ventricular cardiomyopathy: a genotype-phenotype characterization of familial disease. Eur Heart J 2007, 28(5):581-588. Awad MM, Calkins H, Judge DP: Mechanisms of disease: molecular genetics of arrhythmogenic right ventricular dysplasia/cardiomyopathy. Nat Clin Pract Cardiovasc Med 2008, 5(5):258267. Alfakih K, Plein S, Thiele H, Jones T, Ridgway JP, Sivananthan MU: Normal human left and right ventricular dimensions for MRI as assessed by turbo gradient echo and steady-state free precession imaging sequences. J Magn Reson Imaging 2003, 17(3):323-329. Pattynama PM, De Roos A, Van der Wall EE, Van Voorthuisen AE: Evaluation of cardiac function with magnetic resonance imaging. Am Heart J 1994, 128(3):595-607. Kramer CM, Barkhausen J, Flamm SD, Kim RJ, Nagel E: Standardized cardiovascular magnetic resonance imaging (CMR) protocols, society for cardiovascular magnetic resonance: board of trustees task force on standardized protocols. J Cardiovasc Magn Reson 2008, 10:35. Mooij CF, de Wit CJ, Graham DA, Powell AJ, Geva T: Reproducibility of MRI measurements of right ventricular size and function in patients with normal and dilated ventricles. J Magn Reson Imaging 2008, 28(1):67-73. Winter MM, Bernink FJ, Groenink M, Bouma BJ, van Dijk AP, Helbing WA, Tijssen JG, Mulder BJ: Evaluating the systemic right ventricle by CMR: the importance of consistent and reproducible delineation of the cavity. J Cardiovasc Magn Reson 2008, 10:40. Grothues F, Moon JC, Bellenger NG, Smith GS, Klein HU, Pennell DJ: Interstudy reproducibility of right ventricular volumes, function, and mass with cardiovascular magnetic resonance. Am Heart J 2004, 147(2):218-223. Beygui F, Furber A, Delepine S, Helft G, Metzger JP, Geslin P, Le Jeune JJ: Routine breath-hold gradient echo MRI-derived right ventricular mass, volumes and function: accuracy, reproducibility and coherence study. Int J Cardiovasc Imaging 2004, 20(6):509-516. Lotjonen JM, Jarvinen VM, Cheong B, Wu E, Kivisto S, Koikkalainen JR, Mattila JJ, Kervinen HM, Muthupillai R, Sheehan FH et al: Evaluation of cardiac biventricular segmentation from multiaxis MRI data: a multicenter study. J Magn Reson Imaging 2008, 28(3):626-636. 95 95 130. 131. 132. 133. 134. 135. 136. 137. 138. 139. 140. Alfakih K, Plein S, Bloomer T, Jones T, Ridgway J, Sivananthan M: Comparison of right ventricular volume measurements between axial and short axis orientation using steady-state free precession magnetic resonance imaging. J Magn Reson Imaging 2003, 18(1):25-32. Jauhiainen T, Jarvinen VM, Hekali PE: Evaluation of methods for MR imaging of human right ventricular heart volumes and mass. Acta Radiol 2002, 43(6):587-592. Fratz S, Schuhbaeck A, Buchner C, Busch R, Meierhofer C, Martinoff S, Hess J, Stern H: Comparison of accuracy of axial slices versus shortaxis slices for measuring ventricular volumes by cardiac magnetic resonance in patients with corrected tetralogy of fallot. Am J Cardiol 2009, 103(12):1764-1769. Strugnell WE, Slaughter RE, Riley RA, Trotter AJ, Bartlett H: Modified RV short axis series--a new method for cardiac MRI measurement of right ventricular volumes. J Cardiovasc Magn Reson 2005, 7(5):769-774. Nijveldt R, Germans T, McCann GP, Beek AM, van Rossum AC: Semiquantitative assessment of right ventricular function in comparison to a 3D volumetric approach: a cardiovascular magnetic resonance study. Eur Radiol 2008, 18(11):2399-2405. Fritz J, Solaiyappan M, Tandri H, Bomma C, Genc A, Claussen CD, Lima JA, Bluemke DA: Right ventricle shape and contraction patterns and relation to magnetic resonance imaging findings. J Comput Assist Tomogr 2005, 29(6):725-733. Blomstrom-Lundqvist C, Hirsch I, Olsson SB, Edvardsson N: Quantitative analysis of the signal-averaged QRS in patients with arrhythmogenic right ventricular dysplasia. Eur Heart J 1988, 9(3):301312. Marcus FI, Zareba W, Sherrill D: Evaluation of the normal values for signal-averaged electrocardiogram. J Cardiovasc Electrophysiol 2007, 18(2):231-233. Nava A, Folino AF, Bauce B, Turrini P, Buja GF, Daliento L, Thiene G: Signal-averaged electrocardiogram in patients with arrhythmogenic right ventricular cardiomyopathy and ventricular arrhythmias. Eur Heart J 2000, 21(1):58-65. Leclercq JF, Coumel P: Late potentials in arrhythmogenic right ventricular dysplasia. Prevalence, diagnostic and prognostic values. Eur Heart J 1993, 14 Suppl E:80-83. Mehta D, McKenna WJ, Ward DE, Davies MJ, Camm AJ: Significance of signal-averaged electrocardiography in relation to endomyocardial 96 96 References 141. 142. 143. 144. 145. 146. 147. 148. biopsy and ventricular stimulation studies in patients with ventricular tachycardia without clinically apparent heart disease. J Am Coll Cardiol 1989, 14(2):372-379; discussion 380-371. Oselladore L, Nava A, Buja G, Turrini P, Daliento L, Livolsi B, Thiene G: Signal-averaged electrocardiography in familial form of arrhythmogenic right ventricular cardiomyopathy. Am J Cardiol 1995, 75(15):1038-1041. Park Y, Cho Y, Lee DY, Jang GL, Lee H, Yang DH, Park HS, Chae SC, Jun JE, Park WH: Correlation between the parameters of signalaveraged ECG and two-dimensional echocardiography in patients with arrhythmogenic right ventricular cardiomyopathy. Ann Noninvasive Electrocardiol 2009, 14(1):50-56. Yakubo S, Ozawa Y, Saito S, Kasamaki Y, Komaki K, Hanakawa K, Sasaki Y, Aruga M, Miyazawa I, Kanda T et al: Normal limits of highresolution signal-averaged ECG parameters of Japanese adult men and women. J Electrocardiol 2000, 33(3):225-231. Sen-Chowdhry S, Syrris P, McKenna WJ: Genetics of right ventricular cardiomyopathy. J Cardiovasc Electrophysiol 2005, 16(8):927-935. Buja G, Nava A, Daliento L, Scognamiglio R, Miorelli M, Canciani B, Alampi G, Thiene G: Right ventricular cardiomyopathy in identical and nonidentical young twins. Am Heart J 1993, 126(5):1187-1193. Dalal D, Molin LH, Piccini J, Tichnell C, James C, Bomma C, Prakasa K, Towbin JA, Marcus FI, Spevak PJ et al: Clinical features of arrhythmogenic right ventricular dysplasia/cardiomyopathy associated with mutations in plakophilin-2. Circulation 2006, 113(13):1641-1649. Syrris P, Ward D, Asimaki A, Sen-Chowdhry S, Ebrahim HY, Evans A, Hitomi N, Norman M, Pantazis A, Shaw AL et al: Clinical expression of plakophilin-2 mutations in familial arrhythmogenic right ventricular cardiomyopathy. Circulation 2006, 113(3):356-364. Fressart V, Duthoit G, Donal E, Probst V, Deharo JC, Chevalier P, Klug D, Dubourg O, Delacretaz E, Cosnay P et al: Desmosomal gene analysis in arrhythmogenic right ventricular dysplasia/cardiomyopathy: spectrum of mutations and clinical impact in practice. Europace 2010, 12(6):861-868. 97 97