* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download An usual cardiac manifestation of a very common
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Echocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Myocardial infarction wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
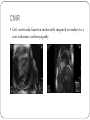
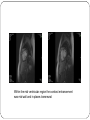
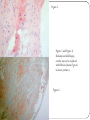
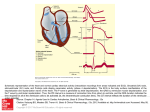
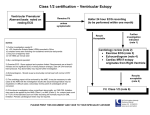
An usual cardiac manifestation of a very common systemic inflammatory condition Tweedie J1, Roberts MJ1, Herron B1, Sheppard M2, McClements B3. 1 Royal Victoria Hospital, Grosvenor Road, Belfast. 2. National Heart and Lung Institute, Imperial College London. 3. Mater Infirmary Hospital, Crumlin Road Belfast Presenting complaint A 69 year old lady presents to the primary percutaneous intervention service (PPCI) with central crushing chest pain. ECG demonstrates right bundle branch block Angiographically normal coronary arteries and mild left ventricular impairment. Represents seven months later with generalised fatigue, chest pain and muscle ache PMH Polymyalgia Rheumatica Hypertension Hyperlipidaemia Hospital Course Clincial examination unremarkable ECG – junctional bradycardia and right bundle branch block NT Pro-BNP significantly elevated at 2051 Echocardiography – moderate left ventricular impairment Cardiomyopathy bloods negative Beta-blocker discontinued Class III NYHA CMR Left ventricular function moderately impaired secondary to a non-ischaemic cardiomyopathy Within the mid ventricular region the contrast enhancement was mid wall and in places transmural Figure 5 Figure 5 and Figure 6 Endomyocardial biopsy, cardiac myocytes replaced with fibrosis (stained green in lower picture). Figure 6 Conclusion Diagnosis of left ventricular systolic impairment secondary to PMR was made. The patient was commenced on high dose oral glucocorticosteroid and remains under review. A previous case report describes resolution of CMR findings and left ventricular dysfunction six months after commencing oral corticosteroid therapy3, follow-up CMR is awaited. This case highlights the importance of considering systemic causes of LV dysfunction even when an association is not well recognised.