* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 43:The Body`s Defenses - Volunteer State Community
Survey
Document related concepts
Complement system wikipedia , lookup
DNA vaccination wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Transcript
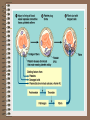
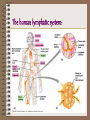
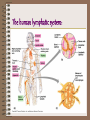
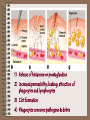
The Lymphatic System Chapter 43, Campbell, 6th edition Nancy G. Morris Volunteer State Community College The fluid compartment includes: • plasma of the blood • interstitial fluid of the tissues • lymph of lymphatic system Plasma: • 90% water • contains electrolytes – inorganic salts (dissolved ions) that maintain osmotic balance & buffer blood (electrolyte balance maintained by kidneys) • contains plasma proteins – – immunoglobulins – transport lipids through the blood – fibrinogens – blood clotting – serum – plasma – clotting factors • transports nutrients, metabolic wastes, respiratory gases, hormones Cellular elements include: 1) Erythrocytes – RBC’s 2) Leukocytes -WBC’s 3) Platelets - thrombocytes Erythrocytes – RBC’s • biconcave discs that transport oxygen • mm3 of human blood contains 5-6 million RBC’s • in mammals, RBC’s lack nuclei & mitochondria; they generate ATP exclusively by anaerobic metabolism (Who knew?) • contain hemoglobin, an iron containing protein that irreversibly binds oxygen; about 250 million molecules per erythrocyte Leukocytes • white blood cells function in defense and immunity • 5,000-10,000 per mm3 of blood • 5 types of leukocytes: – lymphocytes (specialized during infection produce body’s immune response) – – – – basophils eosinophils neutrophils monocytes SEM: specialized lymphocytes attacking a cancer cell Platelets or thrombocytes: • • • • fragments of cells 2-3 µm in diameter originate in bone marrow lack nuclei function in blood clotting Replacement of cellular elements: • cells must be replaced as they wear out • average RBC lives 3-4 months before being destroyed by phagocytic cells in the liver & spleen • components are usually recycled • pluripotent stem cells give rise to all three blood cells • stem cells form early in the embryo & are renewed by mitosis • found in red bone marrow, especially ribs, vertebrae, breastbone, pelvis Blood clotting: • a clot forms when platelets clump together to form a temporary plug • platelets release clotting factors that initiate a cascade reaction which prothrombin is converted to thrombin • thrombin converts inactive water -soluble fibrinogen to active insoluble fibrin • anticlotting factors prevent spontaneous clotting in healthy tissues Circulatory Diseases: • Hemophilia – an inherited defect in any step involved in clot formation • Thrombus – spontaneous clot form • Cardiovascular disease – leading cause of death in US (50% of all deaths) • Heart attack – death of the cardiac muscle • Embolus – moving clot • Atherosclerosis ( Figure 42.16) Circulatory Health: 1. Smoking 2. Lack of exercise 3. Diet high in animal fat All lifestyle choices correlate directly with an increased risk of cardiovascular disease. Lymphatic system: 1) returns fluid from interstitial spaces to the circulatory system 2) includes satellite organs important to defense 3) filter lymph by removing and phagocytosizing pathogens Vocabulary: • Lymph – the fluid part (similar in composition to the interstitial fluid) • Lymph vessels – transport lymph – have valves to prevent backflow of fluid – depend on movement of skeletal muscles to squeeze lymph along Vocabulary: • Lymph nodes – specialized lymphatic tissue – filter the lymph & attack viruses & bacteria • Lymph capillaries – penetrate the small intestine villi, absorb fats, & transport from digestive to circulatory system The human lymphatic system: An overview of the body’s defenses: First line of defense: • Skin – Unbroken skin is a barrier against bacteria & viruses – Secretions from sweat & sebaceous glands produce a pH of 3 to 5 – Bacterial colonization inhibited by washing action of sweat, tears, saliva & mucous – Secretions contain antimicrobial proteins: lysozyme – an enzyme which digests bacterial cell walls • Mucous membranes First line of defense: • Mucous membranes – Secrete mucus – a viscous fluid which traps microbes and others particles – Line the digestive, respiratory, and genitourinary tracts First-line respiratory defenses: ciliated epithelial cells and mucus producing cells of the respiratory system Second line of defense: • Phagocytosis -- the body’s internal mechanism of nonspecific defense – Neutrophils – Constitute about 60-70% of all leukocytes – Average life span only a few days – Upon injury, chemicals released by the invading microbes attract neutrophils to the site. This is chemotaxis. Phagocytic Neutrophil Phagocytosis by a macrophage Second line of defense: • Monocytes - 5% of all leukocytes – Migrate into tissues developing into macrophages (“big eaters”) – Extend long pseudopodia that can attach to polysaccharides on the microbe’s surface, engulf microbe, and lysosomes digest – Some bacteria have capsules to which macrophages can not attach – Other are resistant to lysosomal destruction Second line of defense: • Figure 43.4 (p. 842) • The Human Lymphatic System • Returns fluids from the interstitial fluid to the circulatory system – – – – – – Adenoids Tonsils Lymph nodes Thymus Spleen Appendix - Right lymphatic duct - Thoracic duct - Peyer’s patches The human lymphatic system: Second Line of Defense: • Eosinophils • 1.5 % of all leukocytes • Defense against larger parasitic invaders such as blood flukes, Schistosoma mansoni • These cells position themselves against the parasite wall & discharge destructive enzymes Natural Killer (NK) cells • Nonspecific defense • Do not attack the microorganism directly but destroy virus-infected body cells & abnormal cells that could form tumors • Not phagocytic • Attach the cell membrane causing lysis The Inflammatory Response • Figure 43.5 • Upon injury, blood flow to the injury increases • This is responsible for the characteristic redness & heat of inflammation • The filled capillaries leak fluid into neighboring tissues causing edema (swelling) Inflammatory Response: • Initiated by chemical signals • Some arise from the invading organism itself • Others, such as histamine (produced by basophils), are released by cells of the body in response to tissue injury 1) Release of histamine or prostaglandins 2) Increased permeability; leaking; attraction of phagocytes and lymphocytes 3) Clot formation 4) Phagocytes consume pathogens & debris Nonspecific Defense: • Figure 43.1 • 1st line: skin, mucous membranes, & their secretions • 2nd line: phagocytic leukocytes, antimicrobial proteins, & inflammatory response • These are nonspecific because they do not distinguish among specific pathogens. Antimicrobial Proteins: • Lysozyme – enzyme in tears, saliva • Complement system – a set of 20 serum proteins which carry out a cascade of steps leading to the lysis of microbes • Interferon – secreted by virus infected cells, spread to adjacent non-infected cells and prevent their infection How specific immunity arises: • Lymphocytes – Provide specificity – Provide diversity • Because lymphocytes recognize & respond to specific microbes and foreign molecules, they are said to display specificity. • A foreign molecule that elicits a specific response by a lymphocyte is an antigen. How specific immunity arises • Vertebrates have two cells specialized in different types of antigens and they carry out different defensive actions. • B lymphocytes (mature in bone marrow) • T lymphocytes (mature in thymus) How specific immunity arises • Antigens can elicit a response by activating B lymphocytes to secrete proteins called antibodies. • Antigens have a quaternary structure for which a specific complimentary antibody is synthesized. • Antigen is a contraction of antibodygenerator. How specific immunity arises: • B cells have specific antigen receptors on the plasma membrane (membrane antibodies or immunoglobulins). Antigens can be agglutinated by the receptors on the surface or by free antibodies that have synthesized & secreted by B cells. • T cell receptors are just as specific but are never secreted. • A single B or T lymphocyte bears about 100,000 antigen receptors, all with exactly the same specificity. Specific receptors of lymphocytes Antigens elicit 2 responses: • Immune response • Immunological memory • Each antigen, by binding to specific receptors, selectively activates a tiny fraction of cells from the body’s diverse pool of lymphocytes; this relatively small number of selected cells gives rise to clones of thousands of cells, all specific for and dedicated to eliminating that antigen. • This is clonal selection. Primary Immune Response: • proliferation and differentiation of lymphocytes that occurs the first time the body is exposed to an antigen • requires 10 – 17 days from initial exposure to antigen for lymphocytes to response with maximum force • During this period, plasma cells are cloned which produce antibodies against the invading antigens. Clonal Selection : Figure 43.6 Antigens Cell proliferation clone of plasma cells Clone of memory cells Clonal Selection Secondary Immune Response: • occurs if and when an individual is exposed a second time to the same antigen • the response is faster (only 2 – 7 days), stronger, & prolonged. • Figure 43.7 • Memory cells are poised to proliferate & differentiate rapidly. Immunological Memory Immune Response: • Humoral Immunity • Involves B cell activation and results from the production of antibodies that circulate in the blood plasma & lymph. (Fluids were long ago called “humors.”) • Defend against free bacteria, toxins, and viruses in body fluid. • DEFEND AGAINST EXTRACELLULAR PATHOGENS B Lymphocyte Humoral Immunity Immune Response: • Cell-mediated immunity • Active against bacteria & viruses within infected body cells and against fungi, protozoa, & parasitic worms • Crucial in transplanted tissue & cancer cells – both of which are identified as “nonself.” • DEFEND AGAINST INTRACELLULAR PATHOGENS Overview of Immune Responses • Figure 43.10 • Figure 43.16 Immunity: • Can be achieved either naturally or artificially • Active immunity –occurs when the immune system responds to a foreign antigen acquired either by natural infection or artificially by immunization. • Passive immunity occurs when antibodies are transferred from one individual to another (mother to fetus; mother to breastfeeding child; artificially when antibodies produced by one organism transferred to another organism • Immune system’s capacity to distinguish self from nonself limits blood transfusion and tissue transplant • Abnormal immune function can lead to disease (allergy, rheumatoid arthritis, insulin-dependent diabetes) • AIDS – immunodeficiency disease caused by a virus. Figure 43.19 Budding HIV HIV on Lymphocyte HIV Infections Stages Cytotaxic Cell Cytotaxic Cell