* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Blood
Atherosclerosis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Innate immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
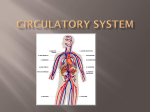
Introduction to Hematology • Hematology is the study of the blood. • - Blood: is the fluid which cells are free and suspended. • It can cross the tissues. • Has red color. • Has volume of 5-6 liters, this is 7-8% of the total body weight. • Has PH of 7.3-7.4 (alkaline). • Specific gravity is 1.055-1.056 • It is composed of plasma (~53-58% of the blood volume), before clotting occurs, and serum after clotting occurs. • Plasma consists of 91-92% water, and 8-9% solids. • Solids are: Albumin. Glucose. Fibrinogen. Sodium. Calcium. Potassium. Cholesterol. Magnisium. Carbon dioxide. Phosphorus. Neutral fats. Glucose. NPN group. Oxygen. • And many other products. • Also there are such substances, like antibodies, hormones, complement, and enzymes. • Cellular parts of the blood (45-47%): • Consists of: – The erythrocytes (RBCs) (~45%) • Contain hemoglobin • Function in the transport of O2 and CO2 – The Leukocytes (WBCs) and platelets (thrombocytes) (~1%) • Leukocytes are involved in the body’s defense against the invasion of foreign antigens. • Platelets are involved in hemostasis which forms a barrier to limit blood loss at an injured site. • The cells are forming about 45-47% of the total blood volume in male and 42% in female. This percentage is determined by centrifugation and is known as heamatocrit (PCV), which is the percentage of the packed red blood cells. Function of the blood: • Nutritive: The blood transports nutrients from the gut to all parts of the body for use or storage. • Respiratory: the blood carries the oxygen to the tissue and remove carbon dioxide and other waste products from the tissues to be excreted by the lung, kidney, liver, and skin • The blood regulates the temperature of the body, because it is constantly in motion. • Transportive: The blood transports the hormones from the endocrine glands to the tissues. • Excretory: To excrete the waste products of metabolism, for example urea, and uric acid. Blood Cells Production (Hemopoiesis) Hematopoiesis is a term describing the formation and development of blood cells. -- Cells of the blood are constantly being lost or destroyed. Thus, to maintain homeostasis, the system must have the capacity for self renewal. This system involves: • Proliferation of progeny stem cells • Differentiation and maturation of the stem cells into the functional cellular elements. • In normal adults, the proliferation, differentiation, and maturation of the hematopoietic cells (RBCs, WBCs, and platelets) is limited to the bone marrow and the widespread lymphatic system and only mature cells are released into the peripheral blood. Sites of production: – Fetus: 0-2 months (yolk sac). 2-7 months (liver and spleen). 5-9 months (bone marrow). – Infants: bone marrow (all bones). – Adults: vertebrae, ribs, sternum, skull, proximal ends of the femur, sacrum and pelvis. • Hematopoiesis in the bone marrow is called medullary hematopoiesis • Hematopoiesis in areas other then the bone marrow is called extramedullary hematopoiesis • Extramedullary hematopoiesis may occur in fetal hematopoietic tissues (liver and spleen) of an adult when the bone marrow cannot meet the physiologic needs of the tissues. This can lead to hepatomegaly and/or splenomegaly (increase in size of the liver or spleen because of increased functions in the organs). • Hematopoietic tissue includes tissues involved in the proliferation, maturation, and destruction of blood cells. Definitions: • Thrombocytopenia: decrease in platelets in the blood. • Splenectomy: removal of the spleen. • Hypersplenism (splenomegaly) – in a number of conditions the spleen may become enlarged. • Leukopenia: decreased in WBCs. • Thrombocytopenia: decreased in platelets. • Pancytopenia: when all three cells types are decreased. Derivation of blood cells • The committed lymphoid stem cells will be involved in lymphopoiesis to produce lymphocytes • The committed myeloid stem cell can differentiate into any of the other hematopoietic cells including erythrocytes, neutrophils, eosinophils, basophils, monocytes, macrophages, and platelets. Erythrocyte: • Normal erythrocyte is a round biconcave disk like cell; it is non-nucleated, containing haemoglobin. It measures about 7.2-7.8 microns. • Life span: the average is 80-120 days. • Function: RBC carry oxygen from the lung to the body cells and carry carbon dioxide from the body cells to the lung. • Erythrocytosis: increased in the blood cells count, which may lead to polycythemia: increasing in the Hemoglobin concentration above 18.5 g/dl in adult males and 15.5 g/dl in adult females, with elevated haematocrit and RBCs count. • Reticulocyte: is a very young erythrocyte which contains remainant of RNA. The precipitated RNA is seen when stained with a supravital stain such as new methylene blue or brilliant crystal blue dyes. • Reticulocytosis: increased blood reticulocyte count. Hemopoietic tissues produce blood cells: • Red bone marrow produces RBCs, WBCs and platelets • Stem cells called hemocytoblasts multiply continually and are pluripotent (capable of differentiating into multiple cell lines) committed cells are destined to continue down one specific cell line • Stimulated by erythropoietin, thrombopoietin and colony stimulating factors (CSFs). Erythropoietin and Its Receptor • • • • About 90% is produced in the kidney, and the rest is produced in a variety of extrarenal sites. The signal that causes erythropoietin-secreting cells to synthesize and release the cytokine is hypoxia. Whenever the oxygen level within the cytoplasm of erythropoietin-producing cells falls below a critical level, erythropoietin is synthesized and secreted into the bloodstream. Once synthesized and released from the cell, erythropoietin travels in the bloodstream to the bone marrow, where it binds to receptors on erythroid cells, thereby initiating their proliferation and differentiation. Erythrocyte Homeostasis: • • • • • Classic negative feedback control Hypoxemia in kidneys EPO production ↑ Stimulation of bone marrow RBC count ↑ in 3-4 days Stimuli for erythropoiesis • Low levels of O2 • Increase in exercise • Hemorrhaging Erythrocyte Production • Erythropoiesis produces 2.5 million RBCs/second from stem cells (hemocytoblasts) in bone marrow • First committed cell is proerythroblast • Has receptors for erythropoietin (EPO) from kidneys; EPO stimulates development of erythroblast • Erythroblasts multiply & synthesize hemoglobin • Normoblasts discard their nucleus to form a reticulocyte named for fine network of endoplasmic reticulum • Enters bloodstream as 0.5 to 1.5% of circulating RBCs • Development takes 3-5 days & involves • Reduction in cell size, increase in cell number, synthesis of hemoglobin & loss of nucleus • Blood loss speeds up the process increasing reticulocyte count Nutritional Needs for Erythropoiesis • Iron : • is key nutritional requirement for erythropoiesis • Lost daily through urine, feces, and bleeding • Low absorption rate requires consumption of 0.5-2 mg/day • Dietary iron in 2 forms: ferric (Fe+3) & ferrous (Fe+2) • Stomach acid converts Fe+3 to absorbable Fe+2 • Gastroferritin from stomach binds Fe+2 & transports it to intestine • Absorbed into blood & binds to transferrin to travel bone marrow uses to make hemoglobin, muscle used to make myoglobin and all cells use to make cytochromes in mitochondria • Liver binds surplus to apoferritin to create ferritin for storage • B12 & folic acid (for rapid cell division) • vitamin C & copper (for cofactors for enzymes synthesizing RBCs) Leukocyte Production (Leukopoiesis) • Committed cell types -- B and T progenitor lymphocytes and granulocyte-macrophage colonyforming units • Possess receptors for colony-stimulating factors released by mature WBCs in response to infections • Red bone marrow stores and releases granulocytes and monocytes • Some lymphocytes leave bone marrow unfinished go to thymus to complete their development (T cells) • Circulating WBCs do not stay in bloodstream • Granulocytes leave in 8 hours & live 5 days longer • Monocytes leave in 20 hours, transform into macrophages and live for several years • WBCs providing long-term immunity • (lymphocytes) last decades Leukocyte Descriptions (WBCs) • Granulocytes – – – • eosinophils - 2-4% basophils - <1% neutrophils - 45-70% Agranulocytes – – Lymphocytes (B and T cells) - 25-33% Monocytes - 3-8% • • • • • • Granulocyte Functions Neutrophils ( in bacterial infections) Phagocytosis of bacteria. Releases antimicrobial chemicals. Eosinophils ( in parasitic infections or allergies) Phagocytosis of antigen-antibody complexes, allergens & inflammatory chemicals. • Release enzymes destroy parasites such as worms. • Basophils ( in chicken pox, sinusitis, diabetes) • Secrete histamine (vasodilator). • Secrete heparin (anticoagulant). Agranulocyte Functions • Lymphocytes ( in diverse infections & immune responses) • Destroy cancer & foreign cells & virally infected cells • “Present” antigens to activate other immune cells • Coordinate actions of other immune cells • Secrete antibodies & provide immune memory • Monocytes ( in viral infections & inflammation) • Differentiate into macrophages • Phagocytize pathogens and debris • “Present” antigens to activate other immune cells (APC) Platelet Production (Thrombopoiesis) • Hemocytoblasts that develop receptors for thrombopoietin from liver or kidney become megakaryoblasts • Megakaryoblasts repeatedly replicates its DNA without dividing forms gigantic cell that remains in bone marrow called megakaryocyte (100 μm in diameter) • Infoldings of megakaryocyte cytoplasm splits off cell fragments that enter the bloodstream as platelets (live for 10 days) • Some stored in spleen and released as needed • Platelets • Small fragments of megakaryocyte cytoplasm, 2-4 μm diameter & containing “granules” • Pseudopods provide amoeboid movement & phagocytosis. Functions: • Secrete clotting factors, growth factors for endothelial repair, and vasoconstrictors in broken vessels. • Form temporary platelet plugs. • Dissolve old blood clots. • Phagocytize bacteria. • Attract WBCs to sites of inflammation.