* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Antigen
DNA vaccination wikipedia , lookup
Major histocompatibility complex wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Innate immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adaptive immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Molecular mimicry wikipedia , lookup
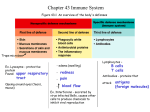
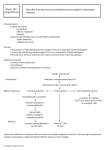
SPECIFIC CELLULAR RESPONSE Paulina Roszkowska The lymphoid system Main part - lymphocytes – differentiate from stem cells in the primary organs, migrate to secondary, recognize antigens by specific receptors • Central (primary) organs: * thymus - proliferation and maturation T lymphocytes, selection for tolerance to autoantigens * bone marrow – proliferation and maturation B lymphocytes • Secondary (peripheral): an environment in which mature lymphocytes T i B interact with antigen, cooperate with phagocytes and accessory cells * spleen – responds to blood-borne antigens * lymph nodes – lymph-borne antigens absorbed via skin, * mucosal tissue - MALT (GALT, BALT), .. – protects the mucosal surface - there is continuous lymfocyte traffic - from the blood stream into lymphoid tissues and back again Non-specific and Specific Immunity: Contrasts Non-specific Specific (natural, native, innate) (acquired, adaptive) • system in place prior to exposure to antigen – can be enhanced after exposure to antigen through effects of cytokines • lacks discrimination among antigens • • • is induced by specific antigen Is activated later than non-specific has memory – Learnt by experience – Enhanced by second exposure • Is poorly effective without innate immunity The non-specific and specific immune systems interact with each other! Antigen (Ag) A substance that can induce a specific immune response and react with the products of it. Epitope – single determinant of antigen, binds with paratope of antibody Feature of antigens • Immunogenicity – ability of recognition of the antigen and production of cellular or humoral response • Antigenicity - ability of raction with products of cellular or humoral response • Specificity – reaction of antibody or specific lymphocytes with epitope Hapten A substance that is non-immunogenic but which can react with the products of a specific immune response. Haptens are small molecules which could never induce an immune response by themselves but they can when coupled to a carrier molecule. Haptens have the property of antigenicity but not immunogenicity. Superantigens – proteins produced by pathogens, which are not processed by antigen presenting cells but can binds to variable region of β chain on TCR of T cells and to MHC class II on antigen presenting cells (APC) and activate Tcell – Large numbers of activated T cells release cytokines having pathological effects Antigenic peptides must normally be processed in order to triger the TCR recognition in MHC groove. It gives: low frequency of antigenantigen specific cells Superantigens (e.g.staphyloccocal toxins) are not processed but bind directly to MHC II only. It gives: high frequency of antigenantigen specific cells: polyclonal response ANTIGEN + LYMPHOCYT = IMMUNE RESPONSE but • different antigens • react with different cells of immune system • and cause different response CELLS OF IMMUNE SYSTEM Leucocytes Adaptive and innate immunity depends upon LEUCOCYTES Innate immunity is mediated largely by GRANULOCYTES Adaptive immunity mediated by LYMPHOCYTES The growth, development and activities of granulocytes and lymphocytes are interconnected and co-operative. Lymphocyte subsets CLP T CELLS B CELLS Common lymphoid precursor T Th Activate B cells and macrophages T HELPER CELLS CTL Kill virusinfected cells CYTOTOXIC T LYMPHOCYTES B PC Produce antibodies PLASMA CELLS Lymphocytes 20-40% of whole leucocytes in blood, morphologically different: • T - 70% -TCR receptor + CD 3 – Th 1, Th 2 – helper » 50-55% » CD4 – co-receptor for MHC-II, 95% small lymphocytes – Tc – cytotoxic » 20-25% » CD8 - MHC-I – 50% small lymphocytes – Ts – suppressor ? (CD8 but also CD4) • B - 10-20% -CD19 CD20 CD21 + -IgM, IgD, MHC-II receptors, only few IgG,IgA,IgE expression • NK - (CD56, CD57) - large granular have Lymphocytes • express characteristic surface markers detected by monoclonal antibodies- cluster of differentiation antigens CD (> 150 is known now) • Markers are responsible for phenotype and biological function: – T – CD2- binds sheep blood cells – CD3- signal tranduction • release cytokines: • Th1: Il-2, IFN , TNF • Th2: Il-2, Il-4, Il-5, Il-6, Il-9 Il-10, Il-13 • possess receptors for: • • • • • • cytokins, MHC, Fc (CD16, CD64), C, integryns (CD2 - LFA), selektyns (CD62 - E, L, P) T or B actiovation releases additional expression of surface markers, antigens Lymphocyte antigen receptors Lyc B T T and B cells are essentially inactive until they encounter antigen. T and B cells express ANTIGEN RECEPTORS The B cell antigen receptor is a membrane-bound antibody SURFACE IMMUNOGLOBULIN The T cell antigen receptor IS NOT membrane bound antibody but a distinct molecule T CELL ANTIGEN RECEPTOR Each antigen receptor binds to a different antigen What Does The B Cell Immunoglobulin (Ig) Receptor Recognize? 1. Proteins (conformational determinants, denatured or proteolyzed determinants) 2. Nucleic acids 3. Polysaccharides 4. Some lipids 5. Small chemicals (haptens) Uniqueness of B Cells • Express both immunoglobulin (Ig) and class II MHC on cell surface • Capable of producing antibody of same specificity as that of its surface Ig AND • Capable of functioning as an antigen presenting cell What Does the T Cell Receptor (TCR) Recognize? Only fragments of proteins (peptides) associated with MHC molecules on surface of cells • • • Helper T cells (Th) recognize peptide associated with MHC class II molecules Cytotoxic T cells (Tc) recognize peptide associated with MHC class I molecules Every TCR on an individual T cell has one specificity T cell receptor (TCR) • The specificity for immune responses resides in the T cell receptor (TCR) • recognizes pathogen (antigen)-derived peptides bound to major histocompatibility complex (MHC) molecules expressed on the surface of nucleated cells –APC (antigen presenting cells). Types of antigens: • T –dependent antigen – need recognition by both T and B lymphocytes to produce antibodies, – most antigens, – mainly proteins, – humoral and cellular response • T-independent antigen – recognition by B lymphocytes B, – mainly polysaccharides: capsule of S.pneumoniae, H.influenzae, N.miningitidis – only antibodies are produced, no cellular response Location of Pathogen Determines Which T Cell Population Responds • Cytosolic: – cells harboring pathogens in the cytosol are recognized and killed by cytotoxic T cells (Tc) that express CD8 • Vesicular: – cells are recognized by a subpopulation of helper T cells (Th1) that express CD4, which enable the infected cell to kill the pathogen • Extracellular: subpopulation of helper T cells (Th2) that express CD4 Location of Pathogen Determines Which T Cell Population Responds Intracellular • reside in two intracellular compartments: – Cytosolic: • viruses and some bacteria • cytosol and nucleus connected via nuclear pores • cells harboring pathogens in the cytosol are recognized and killed by cytotoxic T cells (Tc) that express CD8 Extracellular - site of most bacteria as: -T-independent antigen -T-dependent antigen subpopulation of helper T cells (Th2) that express CD4 – Vesicular: • some bacteria, some parasites • membrane-bound entities (endoplasmic reticulum, endosomes, lysosomes, Golgi apparatus) • cells are recognized by a subpopulation of helper T cells (Th1) that express CD4, which enable the infected cell to kill the pathogen elicits antibody (humoral) response - elicits cell-mediated response Exogenous Antigens must be processed in order to be recognised by T cells T Y Soluble native Ag Cell surface native Ag Soluble peptides of Ag Cell surface peptides of Ag presented by cells that express MHC antigens Cell surface peptides of Ag ANTIGEN PROCESSING No T cell response No T cell response No T cell response No T cell response T cell response IMMUNE RESPONSE Leukocyte Migration and Localization • Bone marrow and thymus (primary lymphoid tissues) – produce B cells and T cells • B cells and T cells recirculate through spleen and lymph nodes (secondary lymphoid tissues) Lymphocyte Recirculation • Antigen presenting cells (APC) pick up antigen and migrate to secondary lymphoid tissues and interact with T cells and B cells • Secondary lymphoid tissues (lymph nodes, spleen) main sites where lymphocytes encounter antigen • Frequency of lymphocytes having a receptor specific for a given antigen is low Leukocyte Migration and Localization Bone marrow Macrophage Thymus T T B B cell cell cell cell T cell Naive lymphocytes Dendritic cell B cell Spleen and lymph nodes Primed lymphocytes T B cell cell APC Tissues Antigen Presenting APC – Antigen Presenting Cells • Heterogenic population: – Langerhans cells – present to Th1 – B cells– present to Th2 – macrophages– phagocytes • Role of APC: – antigen processing (degradation into small peptides), – binding with MHC-II and – presentation to T CD4 • All cells can present antigen to T CD8 posses MHC-I SELF MHC RESTRICTION • In order for a T cell to recognize and respond to a foreign protein antigen, it must recognize the MHC on the presenting cell as self MHC. – Helper T cells recognize antigen in context of class II self MHC. – Cytolytic T cells recognize antigen in context of class I self MHC. • The process whereby T cells become restricted to recognizing self MHC molecules occurs in the thymus. Class I MHC Molecules Class II MHC Molecules • expressed on surface of all nucleated cells • expressed on surface of some nucleated cells, mainly antigen presenting cells (APC) • recognized by TCR of helper T cells • CD4 binds to class II MHC-peptide complex • source of peptide is vesicular compartment • recognized by TCR of cytotoxic T cells • CD8 binds to class I MHC-peptide complex • source of peptide is cytosolic compartment Different cellular pathways for association of peptide with MHC class I and class II molecules Class I MHC Pathway Peptide is presented by MHC-I to CD8 cytotoxic T cell Plasma membrane Peptide passes with MHC from Golgi body to surface Viral protein is made on cytoplasmic ribosomes Globular viral protein - intact rER Peptide associates with MHC-I complex Proteasome degrades protein to peptides Peptide transporter protein moves peptide into ER Golgi body Peptide with MHC goes to Golgi body MHC class I alpha and beta proteins are made on the rER Class II MHC Pathway Peptide MHC-II complex is presented to CD4 helper T cell Endosome fuses with plasma membrane Immunodominant peptide binds to class II MHC Golgi body Globular protein CD4 helper T cell Endosome Fusion of endosome and exocytic vesicle Endocytosis Lysosome Exocytic vesicle fuses with endosome releasing Ii from αβ dimer Protein is processed to peptides in endosome or lysosome Class II MHC α Synthesis 3 chains: α,β and Ii β Ii Endoplasmic reticulum Immune response Different cells cause different response Immunologic responce T cells + antigen B cells + antigen humoral antigen T-independent antigen memory T cells memory effector T cells - Tc lymphocytes Th macrophages NK lymphocytes memory B cells memory effector B cells -plasma cells antybodies HUMORAL RESPONSE CELLULAR RESPONSE • Main phases of the immune response: induction phase – recognition of antigen • central phase – activation, – clonal selection and prolipheration of T and B lymphocytes • effector phase – elimination of antigen mediated by antibodies and effector cells Cell medited specific response Immune response phases: 1. INDUCTION – recognition of antigen by T lymphocyte, 2. central phase – 3. the main function of CD4 cell- regulation by cytokines EFFECTOR – elimination of antigen, pathogen: • • • • macrophages activation (Th1 - IFN)) – better destroing of intracellular bacteria: mycobacteria, brucella, listeria cytotoxicity – T CD8 (Th - Il-2 + APC - Il-12) cell-cell interaction against whole cells: virus-infected, tumour, transplant cells..by perforins, Fas ligand ADCC- antibody dependent cell citytoxity –K cells, receptor Fc (CD16), bind antigens conected with cell LAK – Il-2 activated lymphocytes NK ? TcCD8, NK activated, • viruses in cytosol, MHC class I pathway, Tc response • extracellular bacteria, MHC class II pathway, Th2 response, Ab formation • intracellular bacteria, MHC class II pathway, Th1 response Th response Naïve Th Cells Can Differentiate Into Th1 or Th2 Cells Naive Th cells Short-term Long term Chronic stimulation stimulation Th1 cell Memory cells IFNγ IL-2 ThP ThO ThM cell cell cell Th2 cell IL-2 IFNγ IL-2 IL-4 IL-5 IL-10 IL-4 IL-5 IL-6 IL-10 IL-2 Counter regulation of Th cell subsets IFN- Th1 - IL-10 - Th2 Balanced response Th1 - IL-10 IFN- Th2 Th2 Dominant Th1 Th1 Dominant - Th2 Functions of Th1 and Th2 Cells Th1 Th2 cell cell Inhibits production IL-10 IFNγ IL-4 IL-5 Activates Activates Macrophage Mast cell B cell Eosinophil Antibodies (including IgE) Th 1 response Th1 -Th cells are a subset of T cells that express a unique antigen on their surface called CD4. -A subpopulation of Th1 cells, is the primary defense against intracellular pathogens (inside vesicles). – Th1 cells recognize antigen from the pathogen that are expressed on the surface of infected cells – release cytokines that activate the infected cell. – Once activated, the infected cell can then kill the pathogen. – For example, Mycobacterium tuberculosis, infects macrophages but is not killed because it blocks the fusion of lysosomes with the endosomes. Th1 cells that recognize M. tuberculosis antigens on the surface of an infected macrophage can secrete cytokines that activate macrophages. Helper (Th1) T Cells lysosome Macrophage Macrophage antigen mycobacteria Infected macrophage Activated infected macrophage Th1 cell Central Role of Macrophages in Natural and Specific Immunity • Involved in initial defense and antigen presentation and have effector functions Invading agent Macrophage Antigen presentation Macrophage Activated macrophage Macrophage Th cell Cytokines Lymphokines Cytokines Anti-microbial functions Anti-tumor functions Tc response Cytotoxic T lymphocytes (CTL) • CTLs are a subset of T lymphocytes that express a unique antigen on their surface called CD8. • These cells recognize antigens from the pathogen that are displayed on the surface of the infected cell and kill the cell. • CTLs kill by cytotoity and inducing apoptosis in the infected cell Cytotoxic (Tc) T Cells A B Cell expresses viral antigens C Cytotoxic T cell Virus infects cell Infected cell is killed by cytotoxic T cell by activation of nucleases that cleave host and viral DNA Features of Tc Killing • Antigen-specific • Requires cell-cell contact • Each Tc capable of killing many target cells Interactions of Tc Cell and Target Cel T cytotoxic lymphocyte LFA-1 TCR CD8 peptide Target cell ICAM-1 LFA-2 Class I MHC LFA-3 Mechanism of Arming Tc Cells Class I MHC 1. Cell expressing class I MHC presents antigen ( ) to a pre-Tc cell 3. Th cell makes cytokines Pre-Tc cell IFN IL-2 2. Antigen-presenting cell presents antigen in association with class II MHC to Th cell T helper cell Class II MHC APC 4. Pre-Tc cell differentiates to functional Tc cell Tc cell 5. Tc recognizes antigen on class I MHC-expressing target cell 6. Target cell is killed Main Mechanism of Tc Killing • Tc granules contain: perforin and granzymes • Upon contact with target cell, granule contents released, – perforin polymerizes and forms channel in target cell membrane – Granzymes (serine proteases) enter target cell through channel, activate caspases and nucleases, lead to apoptosis of target cell Mechanism of Tc Killing Tc cell Perforin Ca++ polymerizes Perforin monomers Tc cell Polyperforin channels Target cell Target cell Granzymes Which cells are involved in cellular immune response? Lymphokine activated killers (LAK) - develope from NK influenced by IL 2 - perform their function by antibody dependent cytotoxicity (ADCC) which requires an interaction with humoral specific response Mediators and Regulators of Specific Immunity • • • • • Interleukin-2 (IL-2) Interleukin-4 (IL-4) Interleukin-5 (IL-5) Interleukin-10 (IL-10) Interferon-gamma (IFN-γ) Interleukin-2 (IL-2) • Produced by Th>>Tc • Main growth factor for T cells T cell B cell Monocyte Activation IL-2 secretion NK Stimulation of division T cell Stimulation of division and IFN gamma release (and other Increase in NK mediators) Cell activity Interleukin-4 (IL-4) • Produced by Th2 cells • Stimulates Ig class switching to IgE isotype • Stimulates development of Th2 cells from naïve Th cells • Promotes growth of differentiated Th2 cells Interleukin-5 (IL-5) • Produced by Th2 cells • Promotes growth and differentiation of eosinophils • Activates mature eosinophils • IL-4 and IL-5 can work together Helminths opsonized with IgE can be killed by activated eosinophils Interleukin-10 (IL-10) • Produced by activated macrophages, Th2 cells • Inhibits production of IFN-γ by Th1 cells needed to activate macrophages Interferon-gamma (IFN-γ) • Produced by Th cells >> Tc and NK cells • Numerous functions in both natural and specific immunity Th1 cell > Tc cell NK Granulocyte Endothelial cell Activation Activation IFN gamma secretion Macrophage NK Activation Many cell types Weak anti-viral activity, Stops cell division, Stops hematopoiesis T cell T cell activation B cell Increase in NK cell activity Many cell types Differentiation, Induction of class I Stops cell division and class II MHC THE END