* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Discovery and development of angiotensin receptor blockers wikipedia , lookup
NMDA receptor wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Serotonin syndrome wikipedia , lookup
Neuropharmacology wikipedia , lookup
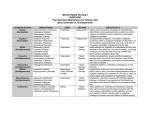
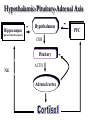
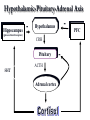
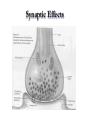
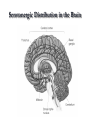
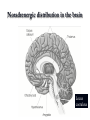
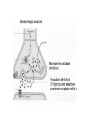
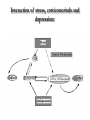
Mood Disorders Neurobiological Causes and Pharmacological Intervention Key issues and questions Target of antidepressant or mood-stabilizing drugs: People with Mood Disorders! What constitutes a “Mood Disorder”? What is the neurochemical basis of clinically significant mood change? What is the neurochemical basis of changes produced by drugs that treat mood disorders? How well do the drugs work? Mood Disorders The structure of mood disorders Normal affective responses on a continuum-brief in duration vs. dominant and sustained Unipolar Mood Disorder A state of depression (or mania) Mostly depression Bipolar Mood Disorder Alternation between depression and mania Subtypes Bipolar I (full manic episodes) Bipolar II (hypomanic episodes) Cyclothymia (“moodiness” – up and down) Anxiety Disorders Nature of Unipolar Mood Disorders Depressive Disorders Melancholic depression (40-60%)-symptoms Atypical depression (~15%)-symptoms Dysthymia-symptoms If there are different levels of depression, and different types, is the underlying neurochemical problem different in nature or degree? Therefore, are pharmacological therapies different for each subtype? Facts & Statistics 7-8% lifetime prevalence Usually recurrent Major Depression or Dysthymia: Females > Males Mean age of onset: 25 yrs ~50% concordance for monozygotic twins Length of episode varies Remission is common Risk of suicide Bipolar Disorders: Females = Males Similar in children and adults, ~80% concordance in monozygotic twins Genetic influence on depression Risk of developing unipolar depression increases with multiple family members with depression Behaviors addressed by antidepressant drug use DSM IV Criteria 1-4 for major depressive episode (5/9): 1. Persistence of depressed mood nearly every day (> 2 weeks) 2. Diminished interest or pleasure, eg., loss of libido (anhedonia and vegetative) 3. Weight fluctuations and loss of appetite (vegetative) 4. Insomnia or hypersomnia (vegetative) Specific behavioral changes that need to be targeted by antidepressant drugs DSM IV Criteria 5-9 for Depression 5. Psychomotor agitation or retardation (feelings of restlessness or being slowed down) 6. Fatigue or loss of energy 7. Worthlessness; guilt 8. Inability to think, concentrate or act decisively 9. Preoccupation with thoughts of death or suicidal ideation Anxiety Disorders Panic Attack Agoraphobia Panic Disorder w/o agoraphobia (GAD) Social Anxiety Disorder period of intense fear or discomfort in which the following occurs: sweating, trembling, choking, chest pain, nausea, dizziness, fear of losing control, derealization or depersonalization, chills or hot flashes fear in social situations exposure to social situations provokes anxiety social situations avoided distress interferes with normal routine Obsessive Compulsive Disorder Depression Subtypes Melancholic anxious, loss of pleasure in all activities dread future insomnia, early morning awakening loss of appetite symptoms worst in the morning excessive inappropriate guilt Atypical lethargic, fatigued increase in appetite symptoms best in morning extreme sensitivity to environmental stimuli (perceived or actual/positive or negative) Dysthymia symptoms of depression chronic but less severe Physiological Correlates Neurochemical changes reduced or elevated norepinephrine levels differences in the number of serotonin receptors may be regulated by dysfunction in serotonin activity “biogenic amine hypothesis” Dysfunction in cortisol secretion what is the basis of this elevation in cortisol? Stress Response CRF-corticotropin releasing factor orchestrates behavioral/endocrine/immune response to stress-interaction with NE interactions with brain areas responsible for fear reaction, transforming experiences into feeling and memory system CRF administered to laboratory rats results in symptoms of “depression” excessive levels may explain behavioral symptoms of sleep disturbances, appetite changes, psychomotor symptoms CRF has two receptor subtypes-novel targets of antidepressant therapy? Hypothalamic-Pituitary-Adrenal Axis Hippocampus - - Hypothalamus PFC (glucocorticoid receptors) CRH Pituitary NE ACTH Adrenal cortex - Hypothalamic-Pituitary-Adrenal Axis Hippocampus - - Hypothalamus PFC (glucocorticoid receptors) CRH Pituitary 5HT ACTH Adrenal cortex - Dexamethasone Suppression Testnot a diagnostic tool Dexamethasone – synthetic glucocorticoid Reduces ACTH production “normal” patients show reduction (suppression) in cortisol levels in blood depressed patients do not abnormal negative feedback loop-most prominent in melancholic depression Dexamethasone Suppression Test-continued Some, but not all, depressed individuals show lack of dexamethasone suppression of cortisone Marginal differences between “suppressors” and “nonsuppressors” in response to pharmacotherapy Some depressed patients, despite elevated cortisol, show no problems with adrenal or pituitary glands Melancholic vs. Atypical Depression Melancholic: hypercortisolism may explain symptoms of depression impaired feedback loop hyperactive, anxiety, insomnia, loss of appetite Atypical: CRF does not stimulate cortisol response impaired feedback loop lethargic, fatigued, hyperphagic, hypersomnic, Animal Models of Depression Diathesis-Stress concept Antidepressant drugs screened on the following preclinical paradigms: Behavioral Despair/Learned Helplessness HPA transgenic Olfactory Bulbectomy Biogenic Amine Hypothesis Evidence for: altered serotonin and norepinephrine levels in depressed and suicide victims (blood and CSF) drugs which reduce NE/5-HT result in depression/suicidal tendencies (reserpine) drugs which elevate serotonin and NE (MAOi, amphetamine) also alleviate symptoms Evidence against: response to SSRI’s is slow effect on serotonin reuptake is similar, but between-patient variability melancholic depressed patients show high NE - may be driving by high CRF levels answer: not a simple relationship Action of Antidepressant Drugs on CNS Effects on the following Monoamine neurotransmitters Norepinephrine (noradrenaline): NE Dopamine: DA Serotonin (5-hydroxytryptamine): 5-HT Treatment of Depression Pharmacotherapy Tricyclic antidepressants (TCA) Heterocyclic or 2nd and 3rd generation Monoamine oxidase inhibitors (MAOI) Selective serotonin reuptake inhibitors (SSRI) Non-Pharmacologic Electroconvulsive therapy (ECT) Action of Antidepressant Drugs on CNS Increase synaptic neurotransmitter levels Impair natural mechanisms for reducing monamine actions Reuptake pumps Enzymatic inactivation (MAO) Autoreceptors Alter receptor levels (after repeated use) Synaptic Effects drug inactivates monoamine oxidases Synaptic Transmission: the Synapse normal reuptake of NT substance from synaptic cleft to presynaptic neuron inhibition of reuptake pumps: more NT in synapse Serotonin/Permissive Hypothesis: Serotonin as “inhibitory” neurotransmitter Inhibit rage – self rage (suicide?) Mood disorders: release of inhibitory damper serotonin norepinephrine = mania Balance of 5HT and NE regulates mood MAO metabolizes serotonin in the presynaptic neuron Serotonergic Distribution in the Brain Synthesis of Norephinephrine: Noradrenergic distribution in the brain Locus coeruleus Receptor Subtypes (transmembrane proteins) 5-HT nine know receptor subtypes grouped into class 1, 2 and 3 5-HT1a is both presynaptic (autofeedback loop) and postsynaptic NE acute use vs. chronic use altered sensitivity/number receptors which types? Classes of Antidepressant Therapy: MAOi TCA Also used for anxiety disorders and pain Panic and phobia (MAO) Obsessive-Compulsive Disorder (TCA) Pain (TCA) SSRI (selective serotonin reuptake inhibitors) anxiety OCD – clomipramine, fluvoxamine, paroxetine, sertraline The receptor hypothesis of antidepressant action Alterations in receptor expression RECEPTOR neurotransmitter Clinical effect Introduction of drug therapy High level or mood Low level or mood Receptor Subtypes in Depressed Patients Not all studies find an association Increased number if 5HT1a neurons increased inhibition of 5HT transmission Altered number of 5HT2 receptors Presynaptic and postsynaptic Changes match chronic stress animal model Therapeutic Lag Theory: improved mood following SSRI treatment corresponds to augmented serotonergic transmission this enhanced 5-HT activity is partially due to autoreceptor blockade New therapy: combine SSRI with 5HT1a antagonist Problems: antidepressant efficacy correlated with postsynaptic 5HT1a receptor affinity The altered gene (s) hypothesis of antidepressant action Excess neurotransmitter leads to alterations in: Genes that code for receptors receptor expression sensitivity of receptors differences in expression in pre- and post-synaptic receptors upregulate or sensitize 5HT1a in hippocampus desensitize 5HT2 receptors elsewhere in the brain Genes that serve to protect and/or facilitate neuronal function (eg., brain derived neurotrophic factor) BDNF does not appear to be associated with disease Relationship of SSRI’s to BDNF levels and neuronal function Interaction of stress, corticosteriods and depression: Side effects MAO inhibitors dietary restrictions – serotonin syndrome Tricyclic Antidepressants cardiac arrhythmias, respiratory depression serotonin syndrome severe sedation Side effects Blockade of NE uptake Blockade of 5-HT uptake GI disturbances interactions with l-tryptophan increase/decrease in anxiety (dose dependent) sexual dysfunction Blockade of histamine receptors tachycardia tremors potentiation of depressant drugs sedation weight gain hypotension Blockade of Ach receptors blurred vision, drymouth constipation Efficacy of Antidepressant Therapy Use of a placebo or active control (randomized, controlled clinical trial) or any control Consistency of study populations Efficacy of one group over another? Treatment guidelines dose, duration, compliance starting dose-enduring response patient compliance-adverse events Efficacy subtypes MAOi atypical and refractory (fail to respond to other types of medications) SSRI mild to moderate depression better tolerated than TCAs do not take with MAOi TCA melancholic depression not effective in reactive depression Heterocyclics use when severe insomnia is present useful in elderly