* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart and Neck Vessels
Remote ischemic conditioning wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Rheumatic fever wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Artificial heart valve wikipedia , lookup
Jatene procedure wikipedia , lookup
Congenital heart defect wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
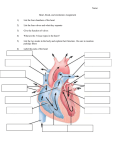
Heart and Neck Vessels Cardiovascular System • Heart & Blood Vessels • Pulmonary Circulation • Systemic Circulation • Precordium – area of chest overlying heart and great vessels. – Arteries & veins connected to the heart – Heart & Great vessels are b/t lungs in the middle 1/3 of the thoracic cage = Mediastinum Heart • Location- Heart extends from the 2nd to 5th ICS & from the Rt. Sternal border to the Lt. MCL • Base broader – upside down • Apex – points down & to the Lt. • Rt. Side anterior • Lt. Side posterior • 4 Chambers • Apical Pulse = during contraction, apex beats against the chest wall. Usually palpable in the Lt., 5th ICS, MCL Great Vessels • Above Base of the heart • Superior & Inferior Vena Cava return unoxygenated venous bld. to the Rt atrium • Pulmonary Artery leaves the Rt. Ventricle, bifurcates & goes to the lungs • Pulmonary Veins return oxygenated bld. to the Lt. Atrium • Aorta carries the bld. to the body • The aorta ascends from the Lt. Ventricle arches back @ the sternal angle and descends behind the heart • Remember arteries always away from the heart; veins always toward the heart – Pulmonary artery to lungs, pulmonary veins to heart Heart Wall • Pericardium – tough, fibrous, double-walled sac, surrounds & protects the heart – Has 2 layers containing pericardial fld. – Adherent to great vessels, esophagus, sternum, & pleurae & is anchored to the diaphragm • Myocardium- muscular wall of the heart. It doesw the pumping. • Endocardium – thin layer of endothelial tissue , lines the inner surface of the heart chamber & valves Chambers of the Heart • • • • • Right side – pumps blood to the lungs Left side – pumps blood to the body Septum- impermeable wall 2 Atria- holding chambers 2 Ventricles- muscular pumping chambers – RA; RV; LA; LV • Valves – separate the 4 chambers – Prevent backflow – Unidirectional – Open & close passively in response to pressure gradients in the moving bld. Heart Valves There are 4 heart valves • 2 Atrioventricular – AV valves- separate the atria & ventricles • Rt. AV. = tricuspid • Lt. AV. = mitral (bicuspid) • Diastole = the heart’s filling phase; AV valves open, ventricles fill with bld. • Systole = pumping phase, AV valves close to prevent backup • Semilunar valves – b/t ventricles & arteries – – – – The SL valves are: Pulmonic valve- rt. Side of the heart Aortic valve – lt. Side of the heart These valves open in systole (during pumping) Cardiac Cycle • 2 Phases – Diastole – ventricles relaxed, tricuspid & mitral valves open • The ventricles fill, the AV valves close= S1 (lub) or the 1st heart sound (remember the atria are filled, the ventricles are empty creating the pressure gradient) Cardiac cycle – Systole- ventricles are full, heart contracts, bld is pumped to lungs & body Heart Sounds • S1 – 1st heart sound • S2 – 2nd heart sound • Extra Sounds – 3rd heart sound – S3 – Ventricular Gallop – 4th heart sound – S4 – Atrial Gallop Heart Murmurs • What are they? • What causes a heart murmur? Heart Automaticity • • • • Conduction SA node – pacemaker AV node ECG • Electrical impulse slightly precedes mechanical events. Pumping Ability • 4-6 liters blood/min. – Cardiac output – Stroke volume Neck Vessels • Carotid Artery • Jugular Veins – Internal – External • Jugular Venous Pressure – Measurement – Angle of Louis – Normal JVP = 2cm or < Peripheral Vascular System • Blood and Lymph Transportation • Disease of Vascular System causes problems with delivery of nutrients & oxygen to tissues and removal of wastes. Arteries • • • • Oxygenated blood to all body tissues Strong & tough Elastic fibers Muscle fibers Pulses • • • • • • • Temporal Carotid Brachial Radial Ulnar Femoral Popliteal Pulses • Dorsalis pedis • Posterior tibial • Veins – Greater # – Closer to skin surface Lymphatics • Separate vessel system • Excess fluid from tissue • Prevents edema Worksheet # 6 Subjective Data • Chest pain • Dyspnea, orthopnea, cough, fatigue, cyanosis, pallor, edema, nocturia • Past Cardiac History • Last EKG • Family history • Personal habits • • • • Leg pain / cramps Swelling or skin changes Lymph node enlargement Medications Objective Data • Measure B/P in both arms – lying, sitting, standing • Palpate pulses bilaterally – – – – – Temporal Carotid * important to only palpate one side at a time * Brachial Radial ulnar – – – – Femoral Popliteal Dorsalis pedis Posterior tibial Jugular Venous Pressure JVP Supine- HOB 30-45 degrees, remove pillow Turn head away from examiner, shine light across neck to highlight pulsation Locate Angle of Louis & position a vertical ruler on reference point 2nd ruler horizontal to level of pulsation Read level on vertical ruler Normal JVP = 2cm. or < Inspect Precordial Area for Retraction or Bulging pulsation • Palpate – use palmar aspect of fingers or ulnar surface of hands to search for other pulsations – – – – Sternoclavicular Epigastric Aortic – right 2nd interspace Pulmonary – lt. 2nd interspace – Right ventricular – lt. Lower sternal border, 5th interspace – Apical – 5th interspace left MCL Percussion • To outline heart’s borders • Limited benefit with lg. Breasts, obese, muscular chest wall • Readily available Percuss for Cardiac Enlargement • Lt. Anterior axillary line 5th intercostal space & toward the sternal border • Resonance over lung – dull over heart • Normal – lt. Border of cardiac dullness 5th interspace MCL: @ 2nd interspace dullnes coincides with the lt. Sternal border • 2nd interspace to 5th MCL Auscultate • Inch stethoscope in a Z pattern from base of heart, across & down to Apex Aortic – 2nd rt. Interspace Pulmonary – 2nd lt. Interspace Erb’s Point – 3rd lt. Interspace Tricuspid – 5th interspace lt. Lower sternal border Apical – 5th interspace lt. MCL APE To Man Note during auscultation • • • • • Rate Rhythm S1- Apex S2 – Base Other sounds? Murmurs • Auscultate – Left side lying – Sitting leaning forward • Observe skin, mucus membranes, nails and chest • Carotid Arteries – Bruits – Neck in neutral position – Bell over carotid @ 3levels • Angle of jaw • Midcervical area • Base of neck Peripheral Vascular System • Arms – Inspect • • • • Skin color, nail beds Temperature Texture & turgor Lesions, edema, clubbing (160 degree angle base = Normal) • Capillary refill <2sec. • symmetry Palpate • Rate, rhythm, elasticity, force Grade force as : 1 - 4 0 = absent 4 = bounding Brachial, radial, ulnar Edema Allen Test • Used to determine the patency of the ulnar & radial artery Hands on knees, palms up Compress both radial arteries Instruct to open & close fists several times Open hands. Results = pink color – ulnar artery patent Repeat occluding ulnar artery Legs • Inspect – – – – – Symmetry Color Hair distribution Venous pattern Measure calf circumference Palpate Legs • • • • • Femoral Popliteal Dorsalis pedis Posterior tibial Inguinal lymph nodes • Edema – Grade scale 1+ to 4+ • • • • • 1+ slight indentation = 1cm. 2+ moderate = 2cm 3+ deep = 3cm. 4+ very deep = 4cm ( more accurate to classify by depth)