* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
History of genetic engineering wikipedia , lookup
Gene therapy of the human retina wikipedia , lookup
Biology and consumer behaviour wikipedia , lookup
Epigenetics of human development wikipedia , lookup
Gene expression profiling wikipedia , lookup
Site-specific recombinase technology wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Gene expression programming wikipedia , lookup
Genome evolution wikipedia , lookup
Genomic imprinting wikipedia , lookup
X-inactivation wikipedia , lookup
Population genetics wikipedia , lookup
Neuronal ceroid lipofuscinosis wikipedia , lookup
Saethre–Chotzen syndrome wikipedia , lookup
Designer baby wikipedia , lookup
Oncogenomics wikipedia , lookup
Medical genetics wikipedia , lookup
Frameshift mutation wikipedia , lookup
DiGeorge syndrome wikipedia , lookup
Down syndrome wikipedia , lookup
Genome (book) wikipedia , lookup
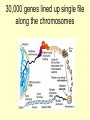
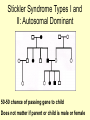
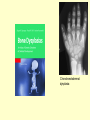
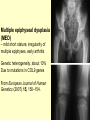
Genetics of Stickler Syndrome Noralane M. Lindor, M.D. Department of Medical Genetics Mayo Clinic, Rochester, Minnesota Stickler, G. B.et al., Hereditary progressive arthro-ophthalmopathy. Mayo Clin. Proc. 40: 433-455, 1965. • …from a long experience at the Mayo Clinic with multiple members of a kindred, described a new dominant entity consisting of progressive myopia beginning in the first decade of life and resulting in retinal detachment and blindness. Affected persons also exhibited premature degenerative changes in various joints with abnormal epiphyseal development and slight hypermobility in some. From On Line Mendelian Inheritance in Man (OMIM) 2007 Stickler Syndrome • Genetic disorder of connective tissue • Due to mutation in one of several genes that encode different types of collagen proteins that are important ingredients of connective tissue of the eye, ear, cartilage, and other tissues. Construction of a body part • Bricks • Mortar • Cells • “Connective tissue” What is mortar? • Recipe of multiple ingredients • What is connective tissue? • Recipe of multiple ingredients • • • • • Elastin Fibrillin Collagens Tissue growth factors Etc, etc, etc Where does connective tissue come from? How is it made? • Secreted by the cells themselves based on the genetic instructions within those cells Stickler Syndrome • A clinical diagnosis– • i.e., diagnosis does not depend on genetic mutation being found • Note: mutations in the genes causative of some cases of Stickler Syndrome can also cause other syndromes that are not Stickler Syndrome Stickler Syndrome:consider dx if have findings in >2 categories • Eye: congenital/early onset cataract, congenital vitreous anomaly, rhegmatogenous retinal detachment, myopia >-3 diopters • Craniofacial: midface hypoplasia, bifid uvula, cleft palate, micrognathia • Ear: sensorineural or conductive hearing loss, hypermobility of middle ear structures • Joints: hypermobility, spondyloepiphyseal dysplasia, early onset osteoarthritis Edited Slide • Clinical variability of Stickler syndrome • Courtesy of: Journal of Med Genetics Metaphase spread of chromosomes from one cell Organization of human chromosomes into a “karyotype” 46,XY 30,000 genes lined up single file along the chromosomes Chromosome 19 hundreds to thousands of different genes on each chromosome Name and address of the 4 genes associated with Stickler Syndrome • • • • COL2A1 COL11A1 COL11A2 COL9A1 chromosome 12q13 chromosome 1p21 chromosome 6p21.3 chromosome 6q13 COL11A1 Stickler Syndrome gene locations COL11A2 COL2A1 COL9A1 Individual collagen molecule is a triple helix Repetitve sequence Gly-X-Y where X and Y are frequently proline. It forms a threestranded triple helix Edited Slide Variation in the Vitreous Phenotype of Stickler Syndrome Can Be Caused by Different Amino Acid Substitutions in the X Position of the Type II Collagen Gly-X-Y Triple Helix Variation in the VitreousPhenotype of Stickler Syndrome Can Be Caused by Different Amino Acid Substitutions in the X Position of the Type II Collagen Gly-X-Y Triple Helix COL2A1 exon 2 Mutations American Journal of Human Genetics Collagen genes vs collagen fibers • 40 different genes encoding at least 27 different types of collagens • 22 different collagens seen in embryonic or mature eye • Only 6 different collagens seen in eye are also present in joint cartilage. These include Type II, V/XI, VI, IX, and XXVII. • Best candidate genes for Stickler syndrome Collagen Type II • Type II Collagen made up of three chains of collagen encoded by COL2A1 – Causes Stickler Syndrome Type 1 – The most common type – Eye finding most often persistence of vestigial vitreous gel in retrolental space, border by folded membrane, “membranous” Collagen Type XI • Type XI Collagen is made up of three different strands encoded by: – COL2A1 – COL11A1 – COL11A2 – Mutations in COL11A1 cause Stickler Syndrome type II – COL11A2 causes non ocular Stickler Syndrome or Stickler Syndrome Type III Genotype:Phenotype • Mutations in COL11A1 have typical Stickler eye findings– usually a beaded pattern vitreopathy (rarely membranous) “alpha 1 chain” • COL11A2 not expressed in vitreous (COL5A2 chain replaces it in Type XI Collagen) therefore no eye problems in Type II Stickler with COL11A2 mutations “alpha 2 chain” Collagen Type IX • Type IX Collagen composed of one strand each encoded by three different genes: – COL9A1 – COL9A2 – COL9A3 – Mutations in COL9A1 can cause autosomal recessive Stickler Syndrome– Type IV?? COL11A1 Stickler Syndrome gene locations COL11A2 COL2A1 COL9A1 + COL9A1 Stickler Syndrome Types I and II: Autosomal Dominant 50-50 chance of passing gene to child Does not matter if parent or child is male or female Stickler Syndrome due to COL9A1: autosomal recessive Both parents carry one gene mutation but do not have Stickler 25% probability of each child having Stickler Syndrome Child who inherits mutated gene from both mother and father have Stickler Syndrome First case in family: recessive or de novo dominant mutation? Putting all the genetics together Sticklertype Collagen Genes making 3 defect strands in this collagen I Type II COL2A1 II Type XI COL2A1, COL11A1, COL11A2 III non Type XI COL2A1, COL11A1, ocular COL11A2 “IV” Type IX COL9A1, COL9A2, (recessive) COL9A3 mutations COL2A1 COL11A1 COL11A2 COL9A1 Genetic testing available, moderately sensitive • • • • COL2A1 27-80% mutations found COL11A1 50-80% COL11A2 unknown but available COL9A1 unknown and unavailable BUT……….! Finding gene mutation not equal to diagnosis of Stickler Syndrome • Mutations in COL2A1 also cause: – – – – – – – – Achondrogenesis type II Hypochondrogenesis Spondyloepiphyseal dysplasia congenita Spondyloepimetaphyseal dysplasia Studwick type Kneist dysplasia Spondyloperipheral dysplasia Early-onset arthropathy AD rhegmatogenous retinal detachment Chondroectodermal dysplasia “Allelic disorder”: same gene, different disorder • Different types of disruption/mutation of a gene affects the collagen production in different ways • The clinical picture may vary a lot • Within a family, relatives have the same disorder because they have the same mutation, but severity can be quite variable. Furthermore…. • Mutations in COL11A1 can cause Marshall Syndrome– hypoplasia of midface and nasal bones and sinuses, myopia, cataracts, deafness, short stature, early arthritis, decreases hair and sweating • Allelic or different disorder? Furthermore…. • Mutations in COL11A2 can cause – Autosomal recessive otospondylometaepiphyseal dysplasia – Weissenback-Zweymuller Syndrome – Nonsyndromic sensorineural hearing loss Furthermore….. • Mutations in COL9A1 can cause a multiple epiphyseal dysplasia: short trunked short stature, multiple joints abnormal Multiple epiphyseal dysplasia (MED) – mild short stature, irregularity of multiple epiphyses, early arthritis Genetic heterogeneity: about 10% Due to mutations in COL9 genes From European Journal of Human Genetics (2007) 15, 150–154. Stickler Syndrome Genetic Testing – a choice, not a requirement • Medically helpful? Would it tell more than the family history? – Diagnosis correct? – Risk for eye complications? – Reproductive risks: 50%? 25%? <1%? – Prenatal diagnosis? • Psychologically – do you want/need to know? • Cost? Insurance issues….