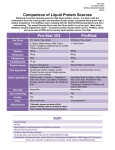
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download C - IS MU
Western blot wikipedia , lookup
Lipid signaling wikipedia , lookup
Protein–protein interaction wikipedia , lookup
Biochemical cascade wikipedia , lookup
Peptide synthesis wikipedia , lookup
Signal transduction wikipedia , lookup
Two-hybrid screening wikipedia , lookup
Cryobiology wikipedia , lookup
Paracrine signalling wikipedia , lookup
Proteases in angiogenesis wikipedia , lookup
Biochemistry wikipedia , lookup
Protein structure prediction wikipedia , lookup
Connective tissue - extracelular matrix Collagen anad elastin – structure and biosynthesis Proteoglycans, fibronectin and laminin Bone tissue. 2009 (J.S.+ E.T.) Connective tissue • The main component is extracelular matrix determines mechanic properties of tissue • Proportion of cells is low. 2 Cells in the connestive tissue • fibroblasts and fibrocytes (chondroblasts and chondrocytes, osteoblasts and osteocytes) produce the major components of extracellular matrix, • histiocytes (fixed and free macrophages) scavenge foreign particles and tissue detritus, • mast cells (mastocytes) releasing heparin and histamine, • adipose cells (adipocytes), • leukocytes, namely lymphocytes, plasmocytes, and monocytes (circulating macrophages, leaving vessels through diapedesis 3 Etracellular matrix • Fibrilar components – fibrils of collagen and reticulin,in some connective tissue types elastin fibres, and • Interfibrillar component (the amorphous ground substance) proteoglycans and hyaluronic acid, fibronectin, laminin and other cell adhesion glycoproteins, in bones, voluminous insoluble mineral component. 4 Main components of extracelullar matrix Cell cytoskeleton receptor Fibronectine Colagen fibrils Elastic fibers Hyaluronic acid Meisenberg, Simmons:Principles of Medical Biochemistry proteoglycanes 5 Function of extracelular matrix •Fills the spaces between cells, binds cells and tissue together Supporting function for cells Regulation: of polarity of the cells cell division adhesion motion Grow and regeneration of tissues Determining the shape of tissue Architecture of tissue and organs Membrane filtration barrier Exchange of metabolites, ions and water 6 Collagen • The most abundant protein in the body (25% of proteins in adults) • Present in all connective tissues • Responsible for strength and flexibility • 27 (?) types of collagen known in human – they differ by structure and function • Only some types are fibilar (I, II, III, V,VI, XI ) • In all collagen types is present (at least partially) typical triplhelix 7 Approximate collagen content in various tissues Tissue Demineralized bone Tendons Skin Cartilage Arteries Lung Liver Collagen content % 90 80-90 50-70 50-70 10-25 10 4 8 Amino acids in collagen • Fibrilar collagens (-chains) polymer of repeats GlyX-Y where: in position X is very often proline, 3-hydroxyproline, Glu, His, Leu, Phe, in position Y 4-hydroxyproline, Thr, Lys, Arg. • At each third position is glycin, in average each forth amino acid is proline or hydroxyproline • The content of glycine 30%, hydroxyproline and hydroxylysine 25% 9 -helix Secondary structure of chains High content of proline and hydroxyproline the chain forms polyproline type helix (the chain cannot turn to be stabilized by hydrogen bonds between C=O and NH of peptide bond unlike the -helix). Secondary structure is an extended helix left – handed helix with 3 amino acids per turn. Secondary structure is stabilized by formation of trimers at which three helical peptides are wound around each other in right-handed triple helix – structure is held together by hydrogen bonds between peptide bonds of interacting polypeptides 10 Tropocollagen structure • The basic structural unit of collagen is triple helix 300 x 1,5 nm • in collagen type I two chains 1(I) and one chain 2(I) (structural formula [1(I)]22(I)) 11 Structure tropocollagen http://images.google.cz/imgres?imgurl=http://upload.wikimedia.org/wikipedia/commons/e/e6/1bkv_collagen_03 .png&imgrefurl=http://commons.wikimedia.org/wiki/File:1bkv_collagen_03.png&usg=__DsSk6K65I8yH5sp_E CT7frEovzU=&h=1673&w=2400&sz=630&hl=cs&start=61&tbnid=apq7uZTRaGosmM:&tbnh=105&tbnw=15 0&prev=/images%3Fq%3Dtriple%2Bhelix%2Bcollagen%26gbv%3D2%26ndsp%3D20%26hl%3Dcs%26sa%3 DN%26start%3D60 12 Glycosylation of collagen • Hydroxy groups of hydroxylysine are modified by posttranslational (cotranslational) glycosylation • Most often glucose a galactose 13 Chain types in collagen • Amino acid composition of polypeptide chains is variable • About 30 separarate genes are known • Best described and mostl wide-spread are 1 and 2 chains 14 Collagen types • Fibril-forming collagens - type I,II,III, V, XI (90% of all collagens) • Network forming collagens – type IV, VIII, X • FACIT*s– type IX,XII, XIV, XVI, XIX • Transmembrane collagens – XIII, XVIII • Others….. *fibril associated collagens with interupted triple helices 15 Some structural divergences in collagen types I, II, III Collagen I – the most common type (skin, bones, tendons, dentin), pevný v tahu. Slightly glycosylated (~1 %); no cysteinyl residues. Collagen II – the main type in the hlavní typ hyalinne cartilage of joints. High degree of glycosylation, no cysteinyl residues. Collagen III (skin, aorta, uterus)elastic type, forms the thin reticuline fibrils. Very low glycosylation, cysteinyl residue are present, small number of disulfide bridges. 16 Collagen IV • The main componet of basement membranes ( e.g. renal glomeruli, capsule of eye lens). • do not form fibrils – its flexible triple helices include some non-helical segments and at their C-ends there are globular domains, • chains associate into the networks • Saccharidic component about 15 %, cysteinyl residues and disulfide bridges are present. Globular domain 17 Collagen IV Association of monomers by carboxy terminals interaction – formation of dimers Asociation of four dimers at the amino terminal domains Formation of lattice from tetramers 18 Synthesis of collagen Fibroblasts, chondroblasts and osteoblasts • First phase has intracellular location: The synthesis of separate procollagen chains (pro-1, pro-2, etc.) Cotranslational hydroxylation of Pro a Lys and glycosylation of hydroxylysine (Hyl) in ER Formation of procollagen from three chains Secretion of procollagen by exocytosis • Second phase is located extracellulary Removal of N- and C-terminal propeptides – formation of tropocollagen Agregation of tropocollagen units – formation of protofibrils Interaction of protofibril with proteoglycans – formation of microfibrils Collagen ripening – oxidation of lysine side chains to allysine, formation of intermolecular links 19 Details of collagen biosynthesis: Synthesis of chains and glycosylation Ribosomal synthesis of separate procollagen chains (pro-1, pro-2, etc.), the chains enter the endoplasmic reticulum. Removal of leader sequence formation of procollagen chains Cotranslational hydroxylation of Pro a Lys – monooxygenase reaction Glycosylation of 5-hydroxylysin (Hyl) - glycosyltransferases 20 Hydroxylation of proline and lysine residues monooxygenáza (askorbate, Fe2+) CO2 proline 2-oxoglutarate 4-hydroxyproline succinate 5-hydroxylation lysine residues is analogical For both hydroxylation reaction ascorbate is necessary 21 Scurvy Ascorbic acid deficiency hydroxylations do not proceed Hydroxyproline residues are required for stabilization of triple helix by hydrogen bond formation Melting temperature of collagen can drop from 420 to 240 Most part of abnormal collagen is degraded in the cell Subcutaneous hemorrages, bleeding gums, poor wound healing etc. 22 Iniciation of triple helix formation Extension sequencies – sequencies of 20-35 AA on both amino- and carboxy- terminals with high content of cysteine residues Formation of procollagen triple-helix is initiated by formation of interchain disulfide bridges on C-terminal peptides – self-assembly C-terminal of procollagen Disulfide bridges between chains in N-terminal "extension“ parts of procollagen Three pro--chains (hydroxylated Pro and glycosylated Hyl) „Extension“ C-terminal parts of procollagen 23 Winding of the procollagen middle parts results in the triple helix Molecules of tropocollagen are translocated to Golgi apparatus, formation of secretory vesicles 24 Procollagen secretion • Secretory vesicles fuses with the membrane and releases procollagen into the extracellular space • Only triple helices can be secreted • Improperly coiled molecules are degraded 25 Conversion of procollagen to tropocollagen • Specifické procollagenpeptidases catalyze the removal of non-helical pro-peptides on both ends • (In clinical biochemistry, the abbreviations PINP and PICP). procollagen I N-terminal propeptide tropocollagen procollagen I C-terminal propeptide 26 Spontaneous association of tropocollagen units – - formation of protofibrils Bundles with diameter that corresponds to about 5 – 10 units. units in protofibrils are shifted by ¼ of their length, so that the regularity of gaps and overlaps generates the banding pattern in the fibrils N-terminals C-terminals 67 nm 27 Association of protofibrils with proteoglycans Protofibrils of collagen interact with glycosaminoglycan chains of proteoglycans: Proteoglycan Collagen protofibrils Chondroitin or keratan sulfates Core protein Bundles or felty tangles of protofibrils of fibrillar collagen types compose thick microfibrils. Hyaluronic acid 28 Maturing of collagen – formation of covalent crosslinks between the chains Oxidative deamination of lysine an nonglycated residues of hydroxylysine H2N CH2 CH2 C O CH2 CH2 C NH Lysine residue tropocollagen chain O2 Lysyl oxidase (Cu2+-enzyme) Allysine O CH CH2 C O NH3+H2O CH 2 CH2 C NH 29 Interchain covalent crosslinks originate in non-catalyzed reactions between the side chains of allysine and lysine residues. Simple covalent bridges join only two adjacent polypeptide chains, two types of those crosslinks are possible: – Aldimine type, when the aldehyde group of allysine reacts with the -amino group of lysine. The product is an aldimine (Schiff base): –CH2-NH2 + O=CH-CH2– –CH2-N=CH-CH2– (+ 2H –CH2-NH-CH2-CH2–) The reaction is rapid, but the product unstable. It is stabilized very slowly by hydrogenation, the crosslink is then called lysinonorleucine bridge. – Aldol type, when two aldehyde groups of allysine react with each other (aldol condensation). One aldehyde group remains free in the bridge, so that it can take part in another reaction. –CH2-CH=O + O=CH-CH2– –CH-CH(OH)-CH2– CH=O ( –C=CH-CH2– + H2O) CH=O The resulting aldol is unstable, but it can be stabilized by elimination of water (a double bond is formed) to the dehydroallysinealdehyde bridge.. 30 Interchain covalent crosslinks 31 Hydroxypyridinium type bridges. NH-CH-CO CH2 HO N NH CH2-CH2 CH CO + CH2-CH2-CH2 CH2 NH-CH-CO Aldimine bridges can react with the aldehyde group of another allysine side chain The heterocyclic pyridinium ring is closed that binds three polypeptide chains together through stable covalent bonds – the hydroxypyridinium type of crosslink is formed.. The hydroxypyridine ring is a very stable structure. It can be determined even after hydrolysis of all peptide bonds in collagen fragments, e.g., excreted into the urine, as deoxypyridinoline or pyridinoline. 32 Hydroxypyridinium bridge 33 Structure of collagen fibrils electron optical picture of soft connective tissue 1 m 0,3 - 3 m protofibrils are formed through aggregation of tropocollagen units Tropocollagen unit microfibrils – either a felty tangle or arranged bundles of protofibrils interacting with proteoglycans 10 - 30 nm 1,5 nm 34 Collagen degradation • Molecules of collagen are metabolically very stable, half-life may be several years. • Their breakdown is increased during starvation or inflammatory diseases. • Degradation by collagenases* *collagenases – enzymes from the family of matrix metaloproteinases (MMP). Proteinases containing Zn, that is necessary for their proteolytic function. 35 Collagen and diseases of connective tissue • Fibroses - overproduction of collagen - lung fibrosis - liver cirhosis - atherosclerosis • Inherited abnormalities in collagen structure Osteogenesis imperfecta (brittle bones) mutation in the gene for 1 and 2 chains of collagen I – impaired formation of triple helices of collagen collagen fall prey to intracellular proteases Ehlers-Danlos syndrom group of diseses, at least 10 types characterized by stretchy skin and loose joints („india rubber“ man) impairment of collagen synthesis due to mutation of genes hyperexensibility of the skin, abnormal tissue fragility, increased joint mobility, „cigarette paper“ scars 36 Elastic fibres • components of elastic connective tissue and elastic cartilage • arterial walls, pulmonary alveoli, skin, ligamentum nuchae • composed of elastin surrounded by a microfibrillar sheath that consists of glycoprotein fibrilin and fibromodulin. During the formation of elastic fibres, those two proteins are arranged in the form of oxytalan fibrils, which serve as a mould that is then filled by tropoelastin, and in which tropoelastin is crosslinked to mature elastin. 37 Elastin • Produced by smooth muscle cells, fibroblasts and chondrocytes • Probably only one genetic type of elastin, variants arise by alternative splicing • Amorphous structure with large amount of crosslinks, non soluble. • The main amino acids are glycine (31%), proline (11%), valine, alanine (22%) and other hydrophobic AA • Only small portion of hydroxyproline (1%) • No glycosylation • Chains don't have a regular secondary structure • Precursor in the synthesis is tropoelastin 38 Covalent crosslinks in elastin Derived from allysine Simple bridges between two residues- aldol or aldimine type Merodesmosine - three side chains (the reaction of aldol with the lysine side chain) - acyclic. Four side chains of allysine and lysine form a tetrafunctional crosslink (the reaction of merodesmosine with allysine) with the stable pyridinium structure called either desmosine or isodesmosine: CH2-CH2-CH2 CH2-CH2 CH2-CH2 CH2-CH2 CH2-CH2 + N N+ CH2 CH2 CH2-CH2-CH2 desmosine CH2-CH2-CH2 CH2-CH2-CH2 isodesmosine After the maturation of crosslinks elastine become highly insoluble, extremly 39 stable and has very low turnover rate. Elasticity of elastin During relaxation – compact disordered structure, hydrophobic interactions between the chains. Strech loosens these interactions, while the elastin network is still held together by covalent crosslinks tah uvolnění 40 Synthesis, zrání and maturation of elastin The synthesis of elastin occurs only in the last phase of foetal development, it is completed practically soon after the childbirth. The later synthesis of considerable amounts of elastin is not supposed. INTRACELLULAR synthesis in fibrocytes and leiomyocytes of blood vessel walls PROELASTIN Peptide fragments ? posttranslational processing (incl. limited proline hydroxylation) soluble TROPOELASTIN SECRETION OF TROPOELASTIN into the EXTRACELLULAR matrix partial degradation of tropoelastin chains insoluble ELASTIN incorporation into the fibrilin mould, spatial arrangement (coacervation), allysine is formed (lysyloxidase), non-catalyzed formation of desmosines (crosslinking), interactions with proteoglycans a very long biological half-life 41 Degradation of elastin specific elastases antielastase factors supporters of breakdown ozone, (NO)x, tobacco smoke, in vessels – intercalation of LDL, bile and fatty acids α1-antitrypsin, α2-macroglobulin, HDL in blood vessels peptide fragments (some of them are potent immunogens) 42 Elastin exhibits a very long biological half-life (the half-life of elastin in the wall of aorta is referred to be about 40 years). After the childbirth, the synthesis of elastin is distinctly reduced, if it is possible at all. The loss of tissue elasticity (namely of skin, large vessels, lung) in aging organisms is indisputable. Much attention is paid to the elastin degradation. Wrinkles are the sign of low skin elasticity that decreases by 2 - 5 % per decade (extrapolated to neonatal period). Wrinkles represent rather a cosmetic problem, though it is extremely interesting from the commercial point of view to those who produce cosmetics and feign the knowledge how to remove wrinkles. The loss of vessel wall elasticity in ageing doesn't quite depend on the low elastin content, but rather on elastin modification due to partial degradation caused by activity of elastase (released mostly by polymorphonuclear leukocytes), supported by the interactions of elastin fibres with LDL or bile acids. The loss of lung tissue elasticity is associated directly with the degradation of elastin in the walls of alveoli. Elastase is released from circulating neutrophils but, under normal conditions, elastase is nearly completely inhibited by α1-antitrypsin. Inherited deficit of 1-antitrypsin or factors that diminish its effect (smoking, ozone in the ground smog) distinctly increase the risk of pulmonary emphysema. 43 Fibrilin •The main component of microfibrils (oxytalan and elastic fibres) • large glycoprotein •Secreted by fibroblasts, becomes incorporated into the insoluble microfibrils • Marfan syndrom : mutation of fibrilin gen fibrilin is deffectiveabnormalities in in connective tissue it affects the eyes (dislocation of the lens), the skeletal system (most patients are tall, exhibit long digits) cardiovascular system (weakness of the aortic media, dilatation of ascending aorta) 44 Proteoglycans • The main component of amorphous ground substance • glycosaminoglycans connected with core protein „bottle-brush“ Chains of GAG Core protein N-end 45 Function of proteoglycans and glycosaminoglycans • Formation of cell-free ground substance – – – – Pressure resistance Shape recovery Lubrication of joints Hydration of cartilages • binding plenty of water • structural organization of extracellular matrix - formation of networks - binding of Ca2+ in bones • Cell adhesion and migration • Enzyme regulation, membrane receptors 46 Glycosaminoglycans (GAGs) • unbranched acidic polysaccharides that consist of repeating disaccharide units [ glycosamin – uronic acid]n Glukosamine, galactosamine (often acetylated) Glucuronic, galacturonic, iduronic Specific –OH groups of saccharides may be sulfated 47 Main types of glycosaminoglycans Heteroglycan Složení • hyaluronic acid • Glc-NAc, Glc-UA • chondroitin-4-sulfate • Gal-NAc-4-sulfate, Glc-UA • chondroitin-6-sulfate • Gal-NAc-6-sulfate, Glc-UA, • keratan sulfate • Gal-NAc, sulfate • heparin • Glc-NAc, Glc/Ido-UA, sulfate • dermatan sulfate • Gal-NAc, Glc/Ido-UA, sulfate 48 Occurence of GAG Type of GAG occurence Hyaluronic acid Embryonal tissues, sinovial fluid, eye, cartilage, loose connective tissue Dermatan sulfate skin, vessels, heart valve Chondroitin sulfate cartilage, bone, heart valve heparin(sulfate) liver, skin Heparan sulfate Basement membranes, components of cell surfaces Keratan sulfate cornea, bone, cartilage 49 Hyaluronic acid COO O Main GAG of extracelular matrix, not sulfated HO OH 4 O Ob O HO 1 GlcUA 3 COO OH NHCOCH3 O b OH 1 GlcNAc O OH 50 Structure of proteoglycans • complexes of glycosaminoglycans and specific proteins • the content of heteroglycans up to 95 %, chains of 10-100 monosacharide units chains of GAG • chains of glycosaminoglycans are covalently attached to core protein • most often O-glycosidic bond between protein and vazba mezi proteinem a glycan, the terminal sequence is Gal-Gal-Xyl • proteoglycans can non-covalently bind hyaluronic acid through a globular domain at the N-end of core protein Core protein N-end 51 Proteoglycan aggregates A large number of simple monomeric proteoglycans bind their globular domains of core proteins non-covalently to a long chain of hyaluronic acid, each of these interactions is supported by two molecules of link glycoproteins formation of huge aggregates esp. in hyaline cartilages. C-end of the core protein of proteoglycan link glycoprotein hyaluronate 52 Various types of proteoglycans Agrecan – tha main proteoglycan in cartilage Versican – in many tissues, mainly vessels and skin Dekorin – small proteoglycan of many tissues Biglycan – small proteoglycan of cartilage 53 Fibronectin • • • • • • • • Cellular glue (cellular adhesive) Most abundant multiadhesive glycoprotein in connective tissue released by fibrocytes, endothelial cells, and other cell types the liver cells secrete fibronectin into the blood plasma (concentration 150 - 700 mg / l). large protein 5000 AK mediates the communication between collagen, proteoglycans and cell surface it interacts with receptors on the cell surface - in this way enables the adhesion of cells to the extracellular matrix - enables interaction between the exterior and the interior of the cell it is involved in migration of the cells 54 Structure of fibronectin • Two polypeptide chains connected near the carboxy ends by disulfidic bond. • Different parts of fibronectin bind to cell surface receptors, proteoglycans, collagen and fibrin NH3+ fibrin heparin collagen NH3+ integrins Cell membranes (RGD receptory) -ooc COO- 55 Integrins • Receptors for fibronectin • Transmembrane proteins • Provide a link between the internal cytoskeleton of cells and extracellular proteins such as fibronectin, collagen, laminin. • Are involved in a wide variety of cell signaling option 56 Meisenberg, Simmons:Principles of Medical Biochemistry Main components of extracelullar matrix Cell cytoskeleton receptor Fibronectine Colagen fibrils Elastic fibers Hyaluronic acid Meisenberg, Simmons:Principles of Medical Biochemistry proteoglycanes 57 Composition of basement membrane •Basement membrane is a thin translucent sheet of extracellular matrix with a thickness of 60 to 100 nm •It consist of: • a basal lamina facing the cell • reticular lamina facing the extracellular matrix •Components of basement membrane: collagen IV, laminin, heparansulfate proteoglycans 58 Composition of basement membrane collagen IV laminin Proteoglykans (perlecan) nidogen Plazmatic membrane integrin Actin fibres Meisenberg, Simmons:Principles of Medical Biochemistry 59 Laminin • In addition to collagen IV is the main protein of basement membranes. • Large heterotrimer (Mr 950 000) • High affinity to ither components of basement membranes (e.g. collagen, proteoglycans, sulfatated lipids ) • Laminin aggregates reversibly into a flat polymeric network at high concentrations of Ca2+ ions. Those polymers bind through another protein (either nidogen or entactin) type IV collagen and core proteins of proteoglycans. These interactions are the cause of anchoring epithelial cells onto components of basement membranes. These interactions are the cause of anchoring epithelial cells onto components of basement membranes. 60 Structure of laminin • • • • Heterotrimer cross-shaped protein. Polypeptide subunits , b a are joined through disulfide bridges Main secondary structure of all three subunits is -helix All three chains have extension at the amino-terminal end with globular domains.These domains allow binding of laminin to other components of extracellular matrix. Bindingsites for integrine or nidogen / entactin clustering of laminin (interaction with collagen or cellular surface heparin 61 The bone The bone is a tissue exhibiting very high metabolic activity The unremitting bone remodelation, both osteoresorption and bone formation, continues after the growth of bones is finished. The bulkiness and consistency of bones depends on the balance between resorption and formation. Composition of bones Water 25 % in compact bone (12 % cementum, 10 % dentin, 1 % tooth enamel) Organic components 30 % Mineral components 40 % In dry bone tissue organic components 40 – 45 % mineral components 60 – 55 % 62 Components of extracellular matrix: organic components - collagen type I proteoglycans sialoprotein osteocalcin citrate mineral components - hydroxylapatite 3Ca3(PO4)2.Ca(OH)2 with octacalcium phosphate Ca8(HPO4)8.5H2O amorphous calcium phosphate Ca3(PO4)2 on the whole 85 % CaCO3 10 % CaF2 0.3 % CaCl2 0.2 % Mg3(PO4)2 1% alkaline salts 2% 63 Bone cells osteoclasts (modified macrophages, bone resorption) osteoblasts (a type of fibroblasts, bone formation) osteocytes (transformed aged osteoblasts) affect the activity of previous cell types by paracrine secretion of interleukins, tumor necrosis factor (TNF), osteoprotegerin, prostaglandins and other various growth factors. 64 Bone cells Osteoblasts • occur on the surfaces of growing or remodelated bones, less frequently inside adult bones. • they synthesize and insert osteoid (extracellular matrix), deposit the bone minerals, and consecutively settle and transform into osteocytes. • the surface of osteoblasts binds molecules of alkaline phosphate that support mineralization of the matrix. 65 Osteoclasts • occur at sites of active bone resorption, in resorption pits. • include many lysosomes exhibit high activity of acid phosphatase • osteoclasts liquidate fragments of collagen and other organic components through phagocytosis. 66 Osteocytes • prevailing cellular elements of mature bone • they are dispersed in lacunas and form a cellular net by means of contacts between their projections • life span of osteocytes is estimated to about 25 years, extinct cells initiated bone resorption. 67 Control of bone remodelation Bone resorption stimulated by parathyrin calcitriol inhibited by calcitonin estrogens Bone formation stimulated by (parathyrin) calcitriol inhibited by androgens estrogens glucocorticoids 68 Biochemical markers of bone metabolism are usefull in clinical biochemistry in tests of osteoporosis and other metabolic osteopathies. Biomarkers of bone formation Catalytic concentration of the bone isoenzyme of alkaline phosphatase (ALP) in serum – the isoenzyme is a marker of osteoblast activity, of which it is an ectoenzyme. Total activity of ALP can serve only as a very rough estimate due to prevalence of other isoenzymes. Concentration of osteocalcin (bone Gla protein, BGP) in serum – osteocalcin is a modulator of bone remodelation secreted by osteoblasts, its production is induced by calcitriol. Osteocalcin is the main non-collagen protein in the extracellular matrix of bones. Concentration of N-terminal or C-terminal propeptides of procollagen I in serum. procollagen I N-terminal propeptide (PINP) tropocollagen procollagen I C-terminal propeptide (PICP) 69 Biomarkers of bone resorption Catalytic concentration of the bone isoenzyme of acid phosphatase (ACP) in serum. This isoenzyme is one of the six ACP isoenzymes (called also tartrate-resistant ACP) considered a marker of osteoclast activity. Concentration of C-terminal telopeptide of collagen I (ICTP, or of C-terminal octapeptide, CTx) in serum or urine. C-terminal telopeptides are terminal non-helical sequences of tropocollagen I, without crosslinks. Excretion of N-terminal telopeptide of collagen I (INTP, NTx) into the urine – N-terminal non-helical sequences of tropocollagen I, which may include some crosslinks, too.. Determination of deoxypyridinoline and pyridinoline in the urine, and determination of galactosyl hydroxylysine in the urine. collagen I N-terminal telopeptide (INTP) galactosyl-hydroxylysine (after alkaline hydrolysis) collagen I C-terminal telopeptides (ICTP) Excretion of hydroxyproline (free or total) in the urine was in common use for years, but currently it is taken as an obsolete test of bone resorption. 70