* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Snímka 1 - TOP Recommended Websites
Survey
Document related concepts
Discovery and development of ACE inhibitors wikipedia , lookup
Metalloprotease inhibitor wikipedia , lookup
Discovery and development of integrase inhibitors wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Effects of long-term benzodiazepine use wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Serotonin syndrome wikipedia , lookup
Prescription costs wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Pharmacognosy wikipedia , lookup
Drug interaction wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Norepinephrine wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Neuropharmacology wikipedia , lookup
Transcript
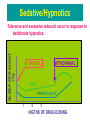
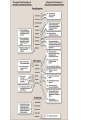
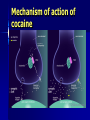
Antidepressants. Antianxiety, Psychostimulants and Psychodyleptics Anton Kohút Depression is pervasive mood altering ilnesses affecting energy, sleep, appetite, libido and the ability to function Antidepressants. Depression Symptoms: depression intensive feelings of sadness hopelessness inability to experience pleasure in usual activities mania enthusiasm rapid though and speech paterns it is an affective disorders characterized by changes in mood (depression or mania) - about 10% of population - experience with depression woman:man ratio - 2:1 Depression is due to a decrease of noradrenaline, serotonine, Mania is due to oposite changes, The bases of the treatment of depression is increase of Na and 5-HT. ? first great theory - role of monoamine neurotransmitters (NE, 5-HT) defficiency of neurotransmitters - depression simplistic theory problem - timming of antidepressant effect on neurotransmitts is far from the timing of the antidepressant effect on mood newer theories - role of neurotransmitter receptors disturbancies in signal transducion Classification of antidepressants 1. Tricyclic antidepressants (TCAs) – Imipramine, Nortriptyline, Amitriptyline, Doxepin Clomipramine Desipramine 2. Monoamine oxidase inhibitors (MAOIs) – Phenelzine, Tranylcypromine 3. Selective serotonin (5-HT) reuptake inhibitors (SSRIs) – Fluoxetine, Fluvoxamine, Sertraline, Paroxetine 4. Reversible monamine oxidase inhibitors (RIMAs) – Moclobemide New antidepressants 5. Norepinephrine Reuptake Inhibitors (NRI) -Reboxetine 6. Norepinephrine and Dopamine Reuptake Inhibitors (NDRI) - Bupropion 7. Serotonin / norepinephrine reuptake inhibitors - Venlafaxine 8. Noradrenergic and Specific Serotoninergic Antidepressants (NaSSA) –Mirtazapine, Mianserine 9. Serotonin-2A antagonists/serotonin reuptake inhibitors – Trazodone 10. Serotonin-2A antagonists/norepinephrine reuptake inhibitors – Nefazodone Classification of antidepressive drugs Tricyclic antidepressants (TCAs) • TCAs prevent the reuptake of NA and 5HT from the synaptic cleft • This re-uptake blockade leads to the accumulation of 5-HT and NA in the synaptic cleft Tricyclic antidepresants (TCA) inhibition of re-uptake increase of NE, 5-HT also blockade of M, H1 1 receptors 2-3 weeks for antidepressive action many years drug of choice M-receptors dry mouth, urine retention, constipation, blurred vision M+1-receptors - tachycardia, hypertension, postural hypotension, H1-receptors sedative effects, body weight gain Side effects of TCAs 1. Anticholinergic -mucosal dryness -constipation -urinary retention -confusion -blurred vision -aggravation of glaucoma 2. Anti alpha adrenergic - orthostatic hypotension 3. Antihistaminic -sedation 4. Quinidine-like - cardiac arrhytmias and block Selective Serotonin Reuptake Inhibitors (SSRI) inhibiion of 5-HT re-uptake increase of 5-HT effect on postsynaptic 5-HT and 5HT1A presynaptic receptors stimulation of 5-HT1A receptors „down-regulation“ lower effect on 5-HT release from presynaptic neurons inhibition of NE reuptake blockade of 1, H1 alebo M- receptors cardotoxic, hypotensive, sedative effects most often prescribed antidepressants today SEROTONINE SYNDROME – combination of SSRI + MAO - lifethreating consequences tremor, convulsions, abdominal pain, diarhea, hypertension, tachycardia, cardiovacular colaps . Fluoxetine in depresion of different etiology PK food prolongs time of absorpion 95% to plasma albumine metabolised in the liver major metabolite (norfluoxetine) simmilar effect as a fluoxetine Side effects lower incidence and intensity GIT - nausea, anorexia, CNS - insomnia, tremor, headache, vertigo CVS - orthostatic hypotension MAO inhibitors (IMAO) first antidepressive agents used clinically "clasical" (e.g. tranylcypromine) irreverzible, nonselective inhibition of MAO-A and MAO-B for antidepressive effects - inhibition of MAO-A 2-3 weeks for antidepressive action use of "clasical" MAOI is now limited - side effects, interactions (food, drugs) tyramine (contained in some foods - chees, red wine, beer) is normally inactivated by MAO-B in the gut MAO inhibitors elevated tyramine tyramine causes release of stored catecholamines tachycardia, hypertension, headache, cardiac arrhythmias patients must avoid tyramine-containing foods RIMA (Reversible Inhibitors of MAO-A) Moclobemide specific inhibition of MAO-A (reversible) inhibition of deamination of 5-HT, NE, D PK good absorption in GIT 50% bound to plasma albumine 95% excreted in urine as an inactive metabolites Side effects insomnia, nausea, headache, dizziness, desorientation, nervousness effect on CVS in combination with tyramine - less important New antidepressants Norepinephrine Reuptake Inhibitors (NRI) Reboxetine introduced in 1997 inhibition of NE re-uptake minimal effect on 5-HT a D depression, narcolepsy, panic fear 98% bound to 1 acid glycoproteine Side effects well tolerated obstipation, dry mouth, urine retention, insomnia, tachycardia Norepinephrine and Dopamine Reuptake Inhibitors (NDRI) Bupropion weak inhibitor of D and NE re-uptake major metabolite - strong NE re-uptake inhibitor suitable for patients with intolerability or low response to SSRI suitable to supress withdrawal symptoms in nicotinedependent people contraindicate in epileptic patients - proconvulsive effect Serotonin and Norepinephrine Reuptake Inhibitors (SNRI) action similar to TCA - NE and 5-HT re-uptake inhibition no effects on M, H1 and 1-adrenergic receptors Venlafaxine low doses 5-HT, moderate doses NA, high doses D metabolised in the liver - O-desmethylvenfalaxine - active metabolit Side effects nausea, constipation, somnolece, nervousness, headache serotonine syndrome Noradrenergic and Specific Serotoninergic Antidepressants (NaSSA) blockade of 2-receptorov release of NE a 5-HT Mirtazapine high affinity to 2-receptors antagonist of 5-HT2, a 5-HT3 and h1-receptors Side effects somnolence, dry mouth, increase of apetite, body weight gain, constipation, serotonine syndrome Mianserine selective antagonist of presynaptic 2-adrenergic receptors partial effect on 1, 5-HT2, 5-HT3 h1- receptorov main metabolites biological activity Side effects hypersensitivity, nausea, tremor Utilization of antidepressants Edvard Munch Anxiety unpleasant state of tension, apprehension, or uneasiness. Disorders involving anxiety are the most common mental disturbances Causes of Anxiety 2). Drug-Induced: – Stimulants Amphetamines, cocaine, TCAs, caffeine. – Sympathomimetics Ephedrine, epinephrine, pseudoephedrine phenylpropanolamine. – Anticholinergics\Antihistaminergics Trihexyphenidyl, benztropine, meperidine diphenhydramine, oxybutinin. – Dopaminergics Amantadine, bromocriptine, L-Dopa, carbid/levodopa. 3). Drug Withdrawal: BDZs, narcotics, BARBs, other sedatives, alcohol. Anxiolytics 1) Benzodiazepines (BZDs). 2) Barbiturates (BARBs). 3) 5-HT1A receptor agonists. 4) 5-HT2A, 5-HT2C & 5-HT3 receptor antagonists. If ANS symptoms are prominent: • ß-Adrenoreceptor antagonists. • 2-AR agonists (clonidine). Benzodiazepines Benzodiazepines (BZD) Mechanism of action BDZ receptors Benzodiazepines Actions Reduction of anxiety Sedative and hypnotic actions Anticonvulsant Muscle relaxant (relax spasticity of ckeletal muscle). Pharmacokinetic aspects Are well absorbed from GIT, They bind strongly to plasma protein, have high lipid solubility, fast cross blood-brainbarrier: rapid onset of action The effect of long-acting increases with the age. Therapeutic uses Anxiety anxiety that accompaniges some forms of depression. Muscular disorders-muscle spasm, spasticity from degenerative disorders, Seizures- grand mal epilepic seizures, acute treatment of alcohol withdrawal Sleep disorders. Side effects Disturbance of intellectual functioning and motor activity impairs manual skils, Potential for dependence and withdrawal syndrome. Properties of Benzodiazepines • BDZs have a wide margin of safety if used for short periods. Prolonged use may cause dependence. • BDZs have little effect on respiratory or cardiovascular function compared to BARBS and other sedative-hypnotics. • BDZs depress the turnover rates of norepinephrine (NE), dopamine (DA) and serotonin (5-HT) in various brain nuclei. • Keep in mind that with formation of active metabolites, the kinetics of the parent drug may not reflect the time course of the pharmacological effect. Prototype drug is diazepam (Valium), which has active metabolites (desmethyl-diazepam and oxazepam) and is long acting (t½ = 20-80 hr). • Estazolam, oxazepam, and lorazepam, which are directly metabolized to glucoronides have the least residual (drowsiness) effects. • All of these drugs and their metabolites are excreted in urine. • Metabolizmus BDZ From Katzung, 1998 Classification of anxiolytic and hypnotic drugs I. Benzodiazepines a. Used as anxiolytics: alprazolam, chlordiazepoxid, diazepam, lorazepam b. Used as hypnotics: flurazepam, nitrazepam, temazepam Long – acting (1-3 days): diazepam, nitrazepam, flurazepam Intermediate acting (10 20 hours): alprazolam, lorazepam Flumazenyl –BDZ antagonist II. Other Anxiolytic drugs ( buspirone (5-HT1A agonist), Buspirone “second generation anxiolytics” has strong anxiolytic properties almost no sedative effect, drowsiness or hypnosis minimal amnesia and dementia does not potentiate other sedatives no abuse potential it is 5-HT1A agonist has both antianxiety and antidepressant effects used for a variety of conditions metabolized very quickly, grapefruit juice increases effect slow onset of action Jennifer Glasgow Hypno-sedative drugs They produce a pronounce, graded, dose-dependent depression of the central nervous system. Hypno-sedative drugs terminology Sedation can bedefined as a supression of responsiveness to a constant level of stimulation, with decreased spontaneous activity Hypnotic effects involve more pronounced depression of the CNS than sedation, and this can be achieved with most sedative drugs simply increasing the dose. Hypno-sedatives I. generation – barbiturates (obsolete) II. generation – benzodiazepines (BDZs) III. generation – zolpidem, zaleplon Hypnotics a. Barbiturates . - Long acting (1-2 days) : phenobarbital. - Intermediate acting (3-8 hours): amobarbital, aprobarbital, pentobarbital,. - Ultrashot acting (20 minutes): thiopental b. Other sedatives and hypnotics Antihistamines Ethanol Barbiturates • In the elderly and in those with limited hepatic function, dosages should be reduced. • Phenobarbital and meprobamate cause autometabolism by induction of liver enzymes. • Strong physiological dependence may develop upon long-term use. • Depression of the medullary respiratory centers is the usual cause of death of sedative/hypnotic overdose. Also loss of brainstem vasomotor control and myocardial depression. Toxicity/Overdose • Withdrawal is characterized by increase anxiety, insomnia, CNS excitability and convulsions. • Drugs with long-half lives have mildest withdrawal. • Drugs with quick onset of action are most abused. • No medication against overdose with BARBs. • Contraindicated in patients with porphyria. Sedative/Hypnotics SLEEP PER NIGHT (%) Tolerance and excessive rebound occur in response to barbiturate hypnotics. CONTROL WITHDRAWAL REM NREM III and IV 1 2 3 NIGTHS OF DRUG DOSING Respiratory Depression BARBS Coma/ Anesthesia BDZs Ataxia Sedation Anticonvulsant Anxiolytic DOSE Miscellaneous Drugs Buspirone Chloral hydrate Hydroxyzine Meprobamate (Similar to BARBS) Zolpidem (BZ1 selective) Zaleplon (BZ1 selective) Zolpidem • Structurally unrelated but as effective as BDZs. • Minimal muscle relaxing and anticonvulsant effect. • Rapidly metabolized by liver enzymes into inactive metabolites. • Dosage should be reduced in patients with hepatic dysfunction, the elderly and patients taking cimetidine. Psychostimulants Psychostimulants – general considerations • are drugs: • that produce wakefullness and arousal and stimulate behavior, • their current clinical use is limited to treatment of specific sleep disorders such as narcolepsy, and certain childhood behavioral problems such as attention deficit disorder, • more importantly, the psychomotor stimulants are a class of drugs widely self-administered for non-medical reasons. • including cocaine, amphetamine, methylphenidate,fenfluramine, phentermine, ephedrine and cathinone Amphetamines Amphetamine • (1) induce the release of dopamine and NA from the nerve terminal; • (2) amphetamine can interact with dopamine containing synaptic vesicles, releasing free dopamine into the nerve terminal; • (3) prevent the degradation of dopamine, • (4) inhibits re-uptake transporter. Pharmacological actions the primary effects of an oral dose are: wakefulness, alertness, decrease fatigue mood elevation, increased ability to concentrate an increase in motor and speech activity amphetamines also diminish the awareness of fatigue person may push exertion to the point of severe damage or even death. stimulate the respiratory center, especially when respiration is depressed by centrally acting drugs, (barbiturates and alcohol) amphetamine can reverse the marked sedation and behavioral retardation resulting from reserpine-like drug depresses appetite by their action on the lateral hypothalamus rather than an effect on metabolic rate Side effects CVS: cardiac stimulation leads to headache, palpitations, cardiac arrhythmias, anginal pain CNS: euphoria, dizziness, tremor, irritability, insomnia, convulsion (at higher doses), hyperthermia and coma addiction - including psychic dependence, tolerance and physical dependence. others: weight loss, psychotic reaction which are often misdiagnosed as schizophrenia. Therapeutic Uses hyperkinesias - methylphenidate narcolepsy - amphetamine or methylphenidate obesity - fenfluramine METHYLXANTINS METHYLXANTINS Caffeine is found in varying quantites in the beans, leaves, and fruit of over 60 plants, Caffeine Metabolites: • theobromine - vasodilator • theophylline -, smooth muscle relaxant • paraxanthine - increase the lipolysis METHYLXANTINES Caffeine: Coffee (100-150 mg/cup) Tea (30-40 mg/cup) Cocoa (15-18mg/cup) Theophylline: Tea and cocoa Theobromine: Cocoa Mechanisms of action of metylxantins Caffeine acts through multiple mechanisms: is an antagonist of adenosine receptors. It results in increased activity of the dopamine Caffeine can also increase levels of epinephrine/adrenaline - inhibitor of the enzyme cAMP-phosphodiesterase causes intracellular calcium release (independent of extracellular calcium) caffeine intensifies and prolongs the effects of epinephrine and epinephrinelike drugs such as amphetamine, methamphetamine, or methylphenidate Pharmacological Activity/ Adverse Effects Low Doses: 100-250mg/caffeine (oral doses) - increase mental alertness, decrease drowsiness lessen fatigue Larger Doses: 250-600mg/caffeine - irritability, restlessness, tremor, insomnia, headache, palpitations Large Doses: > 1000 mg - excitement, delirium and clonic seizures Cardiovascular System: Increase rate and force of the heart by directly stimulating myocardium (low doses) Tachycardia and arrhythmias at higher doses. Peripheral vasodilation - decrease blood pressure (acute administration) Hypotension and cardiac arrest (rapid i.v. theophyline) muscle (theophylline > caffeine) Kidney: all xanthines are capable of producing some degree of diuresis in humans (Smooth Muscles: relaxes vascular smooth theophylline > caffeine) Miscellaneous: xanthines shorten clotting time by increasing tissue prothrombin and factor V. Side effects stimulate gastric secretions in patients with ulcer dehydration in children due to vomiting and transient diuretic action (theophyline) allergic reaction (aminophylline) psychic dependence (caffeine) high doses emesis, convulsion, lethal dose is about 10 g (about 100 cups of coffee) induces arrhytmias Therapeutic uses caffeine + plus ergot alkaloid (ergotamine): used to treat migraine headaches theophylline: prophylaxis for chronic asthma respiratory stimulant bronchodilator for relief of asthmatic symptoms Caffeine - addiction Cocaine Kokaín COCA Coca Bush (Erythroxylon) Main pschoactive substance: COCAINE Content (%): coca leaves 0.5 - 2.5 coca paste 30 - 80 crack up to 90 COCA PHARMACOLOGICAL EFFECTS Sought-after effects feelings of physical mental well being, euphoria increased alertness energy suppresion of hunger fatigue Short-term effects loss of appetite faster breathing, increased heart rate BP increased body temperature, sweating, dilation of pupils bizarre, violent behaviour larger doses: hallucinations, sense of power superiority, restlessness, hyperexcitability, irritability, panic paranoid psychosis (disappears if discontinued) excessive doses - convulsions, seizures, stroke, cerebral hemorrhage or heart failure Mechanism of action of cocaine COCA PHARMACOLOGICAL EFFECTS Long-term effects destruction of tissues in nose if sniffed respiratory problems if smoked infectious diseases, abscesses, if injected malnutrition, weight loss disorientation, apathy, confused exhaustion due to lack of sleep development of tolerance strong psychological dependence with continued use a state similar to paranoid psychosis may develop after stopping - long period of sleep then depression Cocaethylene COCA MEDICAL USE Cocaine as a local anaesthetic, in particular: in surgery of the ear, nose and throat never inject ! Hallucinogens Natural and Synthetic Hallucinogens are drugs that cause hallucinations. An hallucination is a sensory experience of something that does not exist outside the mind. • it may involve hearing, seeing, smelling, tasting or feeling something that isn't really there. • or, it may involve distorted sensory perceptions, so that things look, sound, smell, taste, or feel differently from the way they are. • usually produce so-called pseudo-hallucinations. user knows that what he or she is seeing, hearing, smelling, etc. is not real, but is a product of the drug. • London on hallucinogens Natural hallucinogens • Mescaline (san pedro cactus) • Psilocybin (magic mushrooms) Henbane (Hyoscyamus niger)