* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Survey
Document related concepts
Transcript
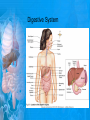
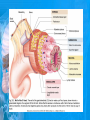
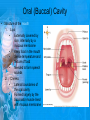
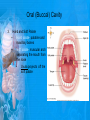
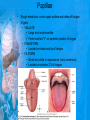
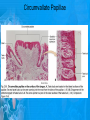
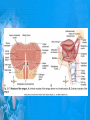
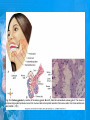
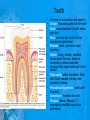
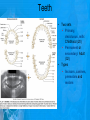
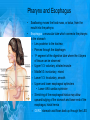
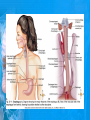
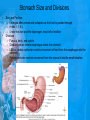
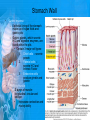
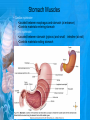
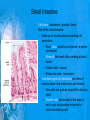
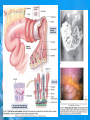
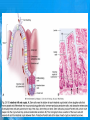
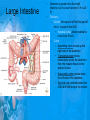
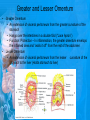
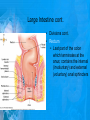
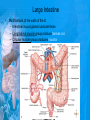
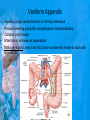
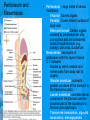
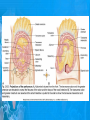
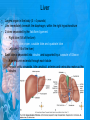
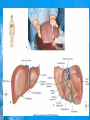
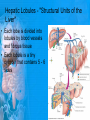
Chapter 25: Anatomy of the Digestive System Dr. Kim Wilson Digestive System Consists of two parts: 1. Gastrointestinal tract – a tube from mouth to anus • Mouth • Pharynx • Esophagus • Stomach • Small and large intestine 2. Accessory organs of digestion – teeth, tongue, salivary glands, liver, gall bladder, pancreas Digestive System Functions of the Digestive System • Ingestion – Taking in food and liquids • Secretion – Water, enzymes, acid or buffers secreted into the gastrointestinal tract • Mixing and propulsion – Food is churned and moved along the GIT by peristalsis. • Digestion – Food is mechanically and chemically broken into smaller particles • Absorption – Passage of digested substances into GIT wall and then into blood & lymph • Defecation – Elimination of undigested or unabsorbed waste in the feces. Walls of the Digestive Tract Consists of 4 layers of tissue: 1. Mucosa • Innermost layer made up of the mucous epithelium, lamina propria and the muscularis mucosa 2. Submucosa • Contains many glands, blood vessels and parasympathetic nerves that forms the submucosal (Meissner’s) plexus 3. Muscularis • Inner layer of circular muscle and outer layer of longitudinal smooth muscle • Contains Auerbach (myenteric) plexus between the 2 muscle layers 4. Serosa • Outermost layer, same as the visceral peritoneum • Connected to the parietal peritoneum via the mesentery Oral (Buccal) Cavity • Structure of the mouth 1. Lips • Externally covered by skin, internally by a mucous membrane • Keep food in the mouth • Sense temperature and texture of food • Needed to form speech sounds 2. Cheeks • Lateral boundaries of the oral cavity • Formed largely by the buccinator muscle lined with mucous membrane Oral (Buccal) Cavity 3. Hard and Soft Palate • Hard palate: palatine and maxillary bones • Soft palate: muscular arch separating the mouth from the nose • Uvula projects off the soft palate Oral (Buccal) Cavity 4. Tongue • 3 parts: root, tip, and body • Skeletal muscle covered by mucous membrane • Covered with papillae which contain taste buds • Lingual frenulum helps anchor the tongue to the floor of the mouth • Rich supply of blood vessels allows for quick absorption (sublingual medications) • Intrinsic muscles: originate and insert in the mouth, used for mastication and speech • Extrinsic muscles: insert into the tongue, but originate from the hyoid or skull bones, used for swallowing (deglutition) and speech Papillae • • Rough elevations; cover upper surface and sides of tongue 3 types • VALLATE • Large and mushroomlike • Form inverted "V" on posterior portion of tongue • FUNGIFORM • Located on sides and tip of tongue • FILIFORM • Small and white in appearance (very numerous) • Located on anterior 2/3 of tongue Circumvallate Papillae Oral (Buccal) Cavity 5. Salivary Glands • Parotid glands • Anterior and inferior to the ear • Produce watery saliva containing enzymes; open into the mouth via the Stenson ducts • Inflammation = mumps • Submandibular glands • At the mandibular angle • Produce saliva containing enzymes and mucus • Wharton ducts open into the mouth on either side of the frenulum • Sublingual glands • In front of the submandibular glands • Drained by ducts of Rivinus • Produce mucus saliva Teeth • • • • • • • • • • Involved in mastication and speech Crown: Exposed portion of the tooth Neck: enameled part of tooth below gum line Root: anchors the tooth into the periodontal membrane Enamel: Hard, protective outer covering Dentin: living, cellular, calcified tissue within the root, dentin is covered by cellular bone-like structure that helps hold tooth in the socket. Pulp cavity within the dentin, filled with blood vessels, nerves, and connective tissue Periodontal ligaments: hold tooth in socket. Cementum: Anchors the root Gingiva: dense, fibrous C.T. covered by stratified squamous epithelium. Teeth • Two sets • Primary, deciduous, milk: Childhood (20) • Permanent or secondary: Adult (32) • Types • Incisors, canines, premolars and molars Pharynx and Esophagus • • Swallowing moves the food mass, or bolus, from the mouth into the pahrynx Esophagus: a muscular tube which connects the pharynx to the stomach – Lies posterior to the trachea – Pierces through the diaphragm – 1st segment of the digestive tube where the 4 layers of tissue can be observed – Upper 1/3: voluntary, striated muscle – Middle1/3: involuntary, mixed – Lower 1/3: Involuntary, smooth – Upper and lower esophageal sphincters • Lower AKA cardiac sphincter – Stretching of the esophageal hiatus may allow upward bulging of the stomach and lower end of the esophagus; hiatal hernia – GERD: stomach acid flows back up through the LES Stomach Size and Divisions • • Size and Position – Enlarged after a meal and collapses as the food is pushed through – Holds 1- 1.5 L – Under the liver and the diaphragm, most left of midline Divisions – Fundus, body, and pyloris – Cardiac portion: where esophagus meets the stomach – LES or cardiac sphincter controls movement of food from the esophagus into the stomach – Pyloric sphincter controls movement from the stomach into the small intestine Stomach Wall • Gastric mucosa – Epithelial lining of the stomach made up of rugae folds and gastric pits – Gastric glands, which secrete HCl and digestive enzymes, are found within the pits • Contain 3 major cell types: 1. Chief cells – secrete pepsin 2. Parietal cells – secrete HCl and Intrinsic Factor 3. Endocrine cells – produce ghrelin and gastrin • Gastric muscle – 3 layers of muscle: longitudinal, circular and oblique • Increases contraction and mixing ability Stomach Muscles • Cardiac sphincter •Located between esophagus and stomach (at entrance) •Controls materials entering stomach • Pyloric sphincter •Located between stomach (pylorus) and small intestine (at exit) •Controls materials exiting stomach Functions of the Stomach 1. 2. 3. 4. 5. 6. 7. Food reservoir – food is stored until it can be digested Secrete gastric juice for digestion of food Churns and mixes food Secretes intrinsic factor important in B12 uptake Small amount of absorption; drugs, water, alcohol, some fats Secretes gastrin ( regulates digestive functions) and ghrelin (increases apetite) HCl destroys pathogens Small Intestine • • 3 divisions: duodenum, jejunum, ileum Wall of the small intestine – Made up of circular plicae containing villi projections • Each villus contains an arteriole, a venule and lacteal • Microvilli line each villus creating a brush border • Goblet cells – mucus • Endocrine cells – hormones – Intestinal crypts of Lieberkuhn are sites of mitosis where new enterocytes are formed • New cells are pushed up and the old ones shed • Paneth cells are located at the base of each crypt and produce enzymes to inhibit bacterial growth • Large Intestine • Diameter is greater than the small intestine, but it is much shorter (5 ft vs 20 ft) Divisions – Cecum: blind pouch off the first part of the LI, located in the LRQ • Ileocecal valve allows material to move from SI to LI – Colon • Ascending colon moves up the right side of the abdomen • Transverse colon moves horizontally across the abdomen from the hepatic flexure to the splenic flexure • Descending colon moves down the left side of the abdomen • Sigmoid colon extends below the colon and connects to the rectum Greater and Lesser Omentum • Greater Omentum • An extension of visceral peritoneum from the greater curvature of the stomach • Hangs over the intestines in a double fold (“Lace Apron”) • Function: Protection – In inflammation, the greater omentum envelops the inflamed area and “walls it off” from the rest of the abdomen • Lesser Omentum • An extension of visceral peritoneum from the lesser curvature of the stomach to the liver (Holds stomach to liver) Large Intestine cont. • Divisions cont. • Rectum • Last part of the colon which terminates at the anus; contains the internal (involuntary) and external (voluntary) anal sphincters Large Intestine • Modifications of the walls of the LI – Intestinal mucus glands lubricate feces – Longitudinal muscle group produce taeniae coli – Circular muscle group produces haustra Veniform Appendix • • • • • Accessory organ whose function is not fully understood Possible breeding ground for nonpathogenic intestinal bacteria Contains lymph tissue Inflammation is known as appendicitis McBurney’s point: area in the RLQ which is extremely tender to touch with appendicitis Peritoneum and Mesenteries • Peritoneum – large sheet of serous membrane • Visceral: Covers organs • Parietal: Covers interior surface of body wall • Retroperitoneal: Certain organs covered by peritoneum on only one surface and are considered behind the peritoneum; e.g., kidneys, pancreas, duodenum • Mesenteries: two layers of peritoneum with thin layer of loose C.T. between • Routes by which vessels and nerves pass from body wall to organs • Greater omentum: connects greater curvature of the stomach to the transverse colon. • Lesser omentum: connects lesser curvature of the stomach and the proximal part of the duodenum to the liver and diaphragm. 32 • Transverse mesocolon, sigmoid mesocolon, mesoappendix. Liver • • • • Largest organ in the body (3 – 4 pounds) Lies immediately beneath the diaphragm, within the right hypochondrium 2 lobes separated by the falciform ligament – Right lobe (5/6 of the liver) • Right lobe proper, caudate lobe and quadrate lobe – Left lobe (1/6 of the liver) Each lobe is separated into lobules and supported by a capsule of Glisson – A central vein extends through each lobule – Hepatic cells, sinusoids, bile canaliculi, arteries and veins also make up the lobules Hepatic Lobules - "Structural Units of the Liver" • Each lobe is divided into lobules by blood vessels and fibrous tissue • Each lobule is a tiny cylinder that contains 5 - 6 sides Liver – Hepatic Lobule Function • Hepatic lobule function – Blood enters lobule from hepatic artery – Blood oxygenates hepatocytes – Sinusoids contain phagocytic Kupffer cells – Blood continues along the sinusoids to the central vein – Central veins lead to the main hepatic veins which drain into the inferior vena cava – Bile formed by hepatocyes passes through the canaliculi to join bile ducts Liver – Bile Ducts • Bile Ducts • Small bile ducts join to form the right and left hepatic ducts which join to form the common hepatic duct • The common hepatic duct merges with the cystic duct from the gallbladder to form the common bile duct • Bile is emptied into the SI at the duodenum via the major duodenal papilla Functions of the Liver • Liver cells detoxify substances • Liver cells secrete bile which aids in fat digestion • Liver cells help metabolize proteins, fats and carbohydrates • Liver cells store iron, vitamins A, B12 and D • Produces plasma proteins and serves as a site of hematopoeisis during fetal development Gallbladder • Lies underneath the liver • Cholecystitis – GB inflammation • Cholelithiasis – gallstone formation • Cholecytectomy – GB removal Gallbladder Functions • The GB stores bile and concentrates it • During fat digestion, the GB contracts and ejects bile into the duodenum • Jaundice results when an obstruction of bile flow occurs • Bile cannot be lost through the feces and enters the blood, creating a yellowish skin hue Pancreas • Pancreas both endocrine and exocrine • Head, body and tail • Endocrine: pancreatic islets. Produce insulin, glucose, and somatostatin • Exocrine: groups acini (grapelike cluster) form lobules separated by septa, produce digestive enzymes • Intercalated ducts lead to intralobular ducts lead to interlobular ducts lead to the pancreatic duct. • Pancreatic duct joins common bile duct and enters duodenum at the hepatopancreatic ampulla controlled by the hepatopancreatic ampullar 42 sphincter Functions of the Pancreas • Functions of the pancreas • Acinar cells secrete digestive enzymes • Beta cells secrete insulin • Alpha cells secrete glucagon