* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Stem Cells – general characteristic and sources
Extracellular matrix wikipedia , lookup
List of types of proteins wikipedia , lookup
Cell culture wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Cell encapsulation wikipedia , lookup
Tissue engineering wikipedia , lookup
Cellular differentiation wikipedia , lookup
Somatic cell nuclear transfer wikipedia , lookup
Induced pluripotent stem cell wikipedia , lookup
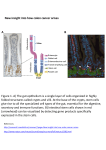
science 8 Research has demonstrated that it is possible to unlocked the differentiated state and allow mature cells to return to immature state from each all cells can be derived. Stem Cells – general characteristic and sources Monika Bieniasz1, Andrzej Chmura1, Artur Kwiatkowski1 Attribution: Department of General and Transplantation Surgery, Medical University of Warsaw, Warsaw, Poland 1. Department of General and Transplantation Surgery, Medical University of Warsaw, Warsaw, Poland #Corresponding author: Monika Bieniasz MD, PhD, Department of General and Transplantation Surgery, Warsaw Medical University, Nowogrodzka 59 street, 02-006 Warsaw, Poland. Phone:+48 225021470, Fax:+48 225022155, e-mail: [email protected] RUNNING TITLE Stem Cells KEYWORDS stem cells, induced pluripotent stem cells, somatic nuclear transfer, reprogramming, regenerative medicine WORD COUNT 3 104 CONFLICT OF INTERESTS no conflicts of interest ABSTRACT Stem cells are self-renewal and can generate differentiated progeny cells. There is an explosion of interest in stem cells over the last few years. It is related to the scientific findings concerning cellular reprogramming. Two scientists, John B. Gurdon and Shinya Yamanaka, have discovered that mature, specialised cells can be reprogrammed to become immature cells. This scientific findings revolutionised our understanding of how cells and organisms developed and provides hope for the use of stem cells in the regenerative medicine and treatment for the diseases. It is hope for patients suffering from incurable diseases in which conventional treatment does not give satisfactory results. It is great expectations for regenerative medicine concerning cell-based therapy such diseases as: diabetes, myocardial infarction, stroke, spinal cord injury, neurodegenerative disease of the brain, liver and kidney damage. The objective of this article are presentation of general characteristic and sources of stem cells. INTRODUCTION T here is considerably increase of interest in stem cells over the last few years. It is related to the scientific findings concerning cellular reprogramming which revolutionised our understanding of how cells and organisms develop. Two scientists have discovered that mature, specialised cells can be reprogrammed to become immature cells capa- ble of developing into all tissues of the body. John Bertrand Gurdon discovered in 1962 that the specialisation of cells is reversible. In a classic experiment, he removed the nucleus of a fertilized egg cell from a frog and replaced it with the nucleus of a mature cell taken from a mature intestinal cell. This modified egg cell developed into a normal tadpole. The DNA MEDtube Science Jun, 2014; Vol.II (2) science 9 of the mature cell still had all the information needed to develop all cells in the frog. More than 40 years later, in 2006, Shinya Yamanaka discovered, how intact mature cells in mice could be reprogrammed to become immature stem cells. He could reprogram mature cells to become pluripotent stem cells by introducing only a four genes, which are currently known as a “Yamanaka’s quartet”. In 2012 Sir John B. Gurdon and Shinya Yamanaka (fig. 1) were jointly awarded The Nobel Prize in Physiology or Medicine „for the discovery that mature cells can be reprogrammed to become pluripotent” (video 1) [1]. In the long-term, these discoveries may lead to new medical treatments. Progress in stem cell research provides hope for the use of stem cells in the regenerative medicine and treatment for the diseases. Special expectations concerning attempts to harness stem cells are associated with the treatment of such diseases, as diabetes, myocardial infarction, muscular dystrophy, stroke, spinal cord injury, neurodegenerative disorders and inflammatory bowel diseases. A potential use of stem cells for medical treatment was illustrated on the figure 2 [2]. DEFINITION, HIERARCHY AND HETEROGENEITY OF STEM CELLS Stem cells (SCs) have several characteristics that make them unique in comparison with other mammalian cells. Stem cells definition includes three main criteria [3, 4]: 1. ability to self-renew, for several cell divisions, which is a prerequisite for sustaining the stem cell pool, 2. ability to generate at the single cell level differentiated progeny cells, in general of multiple lineages, 3. ability to functionally reconstitute a given tissue in vivo. Stem cells reveal high plasticity [5]. The plasticity can be explain by transdifferentiation (direct or indirect) and fusion. Transdifferentiation is describes by the conversion of a cell of one tissue lineage into a cell of an entirely distinct lineage with loss of the tissue-specific markers and function of the original cell type, and acquisition of the identity of a different phenotype through the expression of the gene pattern of other tissue (direct) or through the achievement of a more primitive less specialized state and the successive differentiation to another cell type (indirect or dedifferentiation) [6]. Stem cells can be classified under four categories that describe their potency, or, the extent into which they can differentiate. These four categories are totipotent, pluripotent, multipotent and monopotent. The developmental hierarchy of stem cells was presented in table 1 [7] and fig. 4 [8]. MEDtube Science Jun, 2014; Vol.II (2) Most primitive stem cell of the adult mammalian is the zygote, which is the result of the fusion of two haploid cells during fertilization. The zygote, as a totipotent stem cell, is able to give rise to both the embryo and the placenta. The “artificial” counterpart of the totipotent zygote is referred to as a clonote. The clonote can be created in the laboratory with an experimental approach known as somatic cell nuclear transfer, involving removal of the nucleus from a somatic cell and its transfer into an enucleated oocyte. On the second day after fertilization (24 to 25 hours), the zygote has undergone the first cleavage to produce a 2-cell embryo. The first blastomers obtained from the first division of the zygote or the clonote are still totipotent stem cells [9]. Approximately four days after fertilization, when the blastomers have divided into 32-cell stage, the embryo is called a morula. Cells which form the morula have already lost their totipotency and become pluripotent. The growing morula develops a central cavity and becomes the blastocyst, which contains cells that are precursors for extra-embryonic tissues. This distinct group of cells is known as the inner cell mass (ICM) (fig. 3). Pluripotent stem cells are isolated from ICM of a blastocyst, from the epiblast of cylinder-stage embryo (EPSC) or could be derived in ex vivo cultures from epiblast-derived primordial germ cells (PGC) – as a population of so-called embryonic germ cells (EGC). Pluripotent stem cells give rise to all three germ layers (ectoderm, mesoderm and endoderm), but not to the trophoblast (fig. 4) [8]. Embryonic development and the subsequent adult life are viewed as a continuum of decreasing differentiation ability. After implantation and gastrulation, cells become progressively restricted to specific lineages. Multipotent stem cells contribute to monopotent stem cells that are committed to particular organ/tissues. In recent years, there were discovered a small population of stem cells, which has been named very small embryonic-like stem cells (VSELs). Polish scientist, professor Mariusz Z. Ratajczak, and his scientific team hypothesize that VSELs could be a population of epiblast-derived pluripotent stem cells, which is deposited in various tissues (e. g., bone marrow) and survives into adulthood [8]. Stem cells can be also classified into four types based on their origin. These four categories contain [5]: • stem cells from embryons, • stem cells from fetus, • stem cells from the umbilical cord, • stem cells from the adult. Human embryonic stem cells (hESCs) are obtained from the inner cell mass of the 5- to 6-day old human blastocyst. During embryonic development, the ICM develops into two distinct layers, the epiblast and the hypoblast. The hypoblast forms the yolk sac, and the epiblast differentiates into three primordial germ layers (ectoderm, mesoderm and endoderm). Embryonic stem cells present two distinctive properties: they are science able to differentiate into all derivatives of three primary germ layers (pluripotency), and they are capable of propagating themselves indefinitely, under defined conditions [10]. The main problem concerning embryonic stem cells application is the risk of teratoma and other cancer formation. The understanding the mechanisms of embryonic stem cells differentiation should provide answers for reprogramming of stem cells from adult tissues [7]. Human embryonic germ cells (hEGCs) originate from the primordial germ cells of the gonadal ridge of 5- to 9-week old fetuses and are pluripotent. Human embryonic germ cells have been successfully isolated and characterised [11]. 10 largely in the bone marrow, where hematopoietic stem cells reside, divide and differentiate into all the blood cell types. Bone marrow possesses stem cells that are hematopoietic stem cells and mesenchymal in origin [10]. Hematopoietic stem cells (HSCs) are present in circulating blood and umbilical cord blood and are able to sustain production of all blood cells throughout life. Bone marrow transplantation and peripheral blood stem cell transplantation are current clinical procedures to restore stem cells that have been destroyed by high doses of chemotherapy and/or radiation therapy [12]. Mesenchymal stem cells (bone marrow stroma) Fetal stem cells are primitive cell types found in the organs of fetuses. These stem cells are capable to differentiate into two types of stem cells: pluripotent stem cells and hematopoietic stem cells. Fetal blood, placenta and umbilical cord are rich sources of fetal hematopoietic stem cells [10, 12]. The tissue rejection due to fetal cells application may limit the usefulness of fetal stem cells [12]. Umbilical cord stem cells contais circulating stem cells. The cellular contents of umbilical cord blood appear to be quite distinct from those of bone marrows and adult peripheral blood [13]. The frequency of umbilical cord blood hematopoietic stem cells equals or exceeds that of bone marrow and they are known to produce large colonies in vitro, have long telomeres and can be expanded in long term culture [12]. Adult stem cells are any stem cells obtained from mature tissues. Most adult stem cells are lineage-restricted (multipotent) and are predominantly referred to by their tissue origin (endothelial stem cells, mesenchymal stem cells, adipose-derived stem cells, etc.) [14]. They play essential roles on local tissue repair and regeneration. The therapeutic application of adult stem cells is not as controversial as embryonic stem cells, because the production of adult stem cells does not require the destruction of embryo [12]. Adult stem cells include: • hematopoietic stem cells, • mesenchymal stem cells, • hepatic stem cells, • pancreatic stem cells, • intestinal stem cells, • epidermal stem cells, • bone and cartilage stem cells, • neural stem cells, • eye stem cells. Hematopoietic stem cells (bone marrow and peripheral blood) Blood cells and certain kinds of epithelial cells survive for the shortest time in comparison to all the cell types in the body. The replenishment process occurs Mesenchymal stem cells (MSCs) are multipotent stem cells and can be isolated from several other tissues, including adipose tissue, placenta, amniotic fluid, umbilical cord blood and fetal tissues. MSCs are able to differentiate into adipocytes, osteocytes, chondrocytes, smooth muscle cells and hematopoietic supportive stroma [15]. In a steady state and or in response to injury, turnover of stromal tissue and occurs through the participation of a population of stem cells found in the stromal tissue [16]. The isolation of a large number of potent HSCs/ MSCs sets the basis of new methods for tissue regeneration and cell therapy [17]. Hepatic stem cells Mammals are said to survive surgical resection of at least 75% of the liver by regeneration. The original tissue can be restored in 2-3 weeks [18]. Liver mass is restored primarily through the activation of hepatocytes [19]. It is suggested that mature hepatocytes could serve their own physiologic precursors [20]. Liver oval cell, a blast-like cell and with the capability of self renewing and multipotent differentiation, is considered as the liver-specific stem cell. In multiple independent studies, these liver oval cells have been shown to present molecular markers of adult hepatocytes, (albumin, cytokeratins 8 and 18), bile duct cells (cytokeratins 7 and 19, OV-6, A6), fetal hepatoblasts (AFP), and haematopoietic stem cells (Thy -1, Sca-1, c-kit). Oval cells isolated from the liver represent a promising source for cell-based therapy [12]. Pancreatic stem cells Pancreatic stem cells have the potential to differentiate into all three germ layers. The best candidate sources for adult pancreatic stem or progenitor cells are: duct cells, exocrine tissue, nestin-positive islet -derived progenitor cells, neurogenin-3-positive cells, pancreas-derived multi-potent precursors; and mature beta-cells. Major markers present on the surface of pancreatic stem cells include Oct-4, Nestin, and c-kit. DCAMKL-1 is a novel putative stem/progenitor MEDtube Science Jun, 2014; Vol.II (2) 11 marker, can be used to isolate normal pancreatic stem/progenitors, and potentially regenerate pancreatic tissues [12]. Intestinal stem cells science either due to injury or diseases, it is unable for the corneal ocular repairing and regeneration [32]. It is suggested that many corneal disorders such as in keratoconus, anirdia and alkali burns are likely associated with the corneal stem cell deficiency [12]. The gastrointestinal epithelial lining undergoes rapid renewal throughout life. Epithelial cell renewal in the intestine is sustained by multipotent stem cells located in the crypts of Lieberhahn. In the small intestine, epithelial cells of enterocytic, goblet and enteroendocrine origin differentiate as they migrate from a crypt up an adjacent villus and leave the intestine ones they reach the villus tip. In the colon, epithelial cells migrate from the crypt toaflat surface cuff that surround its opening [21]. POTENTIAL SOURCES OF STEM CELLS TO REGENERATE TISSUES AND ORGANS Epidermal stem cells Pluripotent stem cells obtained from banked embryons derived by fertilization The human skin comprises the outer epidermis and underlying dermis. Keratinocyte is the most important cell type in the epidermis. Keratinocyte divides and is housed in the basal layer of the epidermis. The epidermis houses stem cells at the base of the hair follicle and their self-renewing properties allow for the re-growth of hair and skin that occurs continuously. New keratinocytes are produced continuously during adult life to replace squames shed from the outer skin layers and the hairs that are lost. Stem cells differentiate into an intermediate cell called “the transient amplifying cell” [22]. “The transient amplifying cell” can regenerate themselves and also give rise to the more differentiated keratinocytes that are displaced from the basement membrane and form the superficial layers of the epidermis [23]. Bone and cartilage stem cells Bone itself has been found to have both uncommitted stem cells as well as committed osteoprogenitor cells [24, 25]. Articular cartilage has a very limited capacity of repair in vivo. In case of injury to cartilage, stem cells do participate in the repair process [26, 27]. Neural stem cells Neural stem cells are known to reside in the subventricular zone of the forebrain and in the dental gyrus of the hippocampus and they consistently generate new neurons [28-30]. Eye stem cells Human corneal stem cells locate on cornea limbus, which is between the colored and white part of the eye. In steady state and in the response to injury to the corneal epithelium, the limbal corneal stem cells divide to produce daughter transient amplifying cells that proliferate, migrate onto the central cornea and become terminally differentiated to replace the lost cells [31]. In the case of limbal stem cell deficiency, MEDtube Science Jun, 2014; Vol.II (2) The first documentation of the isolation of embryonic stem cells from human blastocysts was in 1994 [10]. Since then, obtain and culture techniques of human embryonic stem cells have been substantially improved. Pluripotent stem cells can be potentially derived from four sources, as shown in table 2 and video 2 [7]. Each of these potential sources has advantageous and limitations [7]. The method of obtaining pluripotent stem cells from banked embryons, derived by fertilization for clinical purposes, was abandoned because of the fact that banked embryos cells has incompatibility with the potential recipient cells, and therefore embryonic cell lines will differentiate into cells with another histocompatibility antigens than the potential recipient [7]. Addictionally, use of human embryos faces ethical controversies that hinder the applications of human ES cells. It is difficult to generate patient- or disease -specific ES cells, which are required for their effective application [33]. Pluripotent SCs isolated from embryons derived by therapeutic cloning The method of therapeutic cloning involves in vitro creating an cell, which in terms of development potential is equivalent to the zygote [34]. This cell is called „a clonote”. Oocyte cytoplasm, from which the nucleus containing the haploid number of chromosomes is removed, and then the mature cell nucleus containing diploid number of chromosomes is inserted in it, is used to create a clonote. The chromosomes inserted into the oocyte cytoplasm are „de-differentiated”. Oocyte cytoplasm is „biochemical incubator,” which includes a lot of enzymes that can modify the DNA. DNA is undergone demethylation and rearrangement reaction. It is determined the appropriate pattern of methylation and acetylation of histone proteins, which leads to remodel of chromatin structure and allows to return differentiated DNA, obtained from the donor’s somatic cell, to the state as it appeared in the fertilized oocyte. It creates the possibility of early developmental gene expression. This procedure is called somatic cell nuclear transfer. The created clonote has genes which are compatibile with the genes from a cell which was a nuclear donor. The resulting embryonic stem cells are perfectly matched to the patient’s immune system and no immunosupressants would be require to prevent rejection [35]. science The main obstacle to extensive use of therapeutic cloning is limited access to human oocytes, and the observations that the pluripotent stem cells derived from animal clonote, similar to embryonic cells, can form teratomas in experimental animal study [7]. Pluripotent SCs isolated from adult tissues Adult stem cells are, especially in the area of hematopoietic stem cells, better understood than any other aspect of stem cell biology [36]. Cell-based therapy dates back to the first bone marrow transplant in 1956 [37]. It has been found that progenitor cell populations are present in many tissues other than the bone marrow, including the gastrointestinal tract, skin, brain and muscle [35]. Adult stem cells tend to be tissue-specific and can differentiate into cell types associated with the organ system in which they reside [38, 39]. Currently, it is known that niches of stem cells exist in many tissues, such as bone marrow, blood, liver, pancreas, brain, skin, the gastrointestinal tract, the eye, skeletal muscle, and dental pulp [35]. Induced pluripotent stem cells (iPSCs) Induced pluripotent stem cells (iPSCs) are obtained by in vitro transformation of cultured adult somatic cells with genes encoding transcription factors crucial for the development of embryonic stem cells (Oct-4, Klf4, Nanog, c-myc) [7]. In mid 2006, Takayashi i Yamanaka reported that mouse embryonic fibroblasts and adult mouse fibroblast can be reprogrammed into an induced pluripotent state [Takahashi, Zhao]. They evaluated 24 genes that were thought to be important for embryonic stem cells and identified 4 crucial genes that were required to bestow embryonic stem cell-like properties on fibroblasts. Mouse embryonic fibroblasts and adult fibroblasts were co-transuced with retroviral vectors, each carrying Oct3/4, Sox2, c-Myc and KLF4. The resultant iPSCs possessed the immortal growth characteristics of self-renewing ESCs. iPSCs were injected into mouse blastocyst and they contributed to a variety of diverse cell types, demonstrating their developmental potential [40]. 12 mice [Zhao]. SUMMARY On the threshold of the third millennium, the man reached for the technology, which has been attributed to Supreme Beings. Progress in biological sciences and genetics drew secrets of organisms formation and their regeneration. The Nobel Prize winners, Sir John Gurdon and Shinya Yamanaka, introduce us in the exciting world of stem cells and regenerative medicine. Progress in stem cells research provides hope for the use of stem cells in the regenerative medicine. It can be assumed that stem cells will be used for any treatment options, including extending the life, in the near future. It has been suggested that instead of whole organ transplantation, surgeons will transplant cells with high regenerative potential, which will repair damaged organs. Continuous technical progress give the scientists hope for the immediate future and for the realization of the mythological idea of regeneration, which was describe in the story of Prometheus. CITE THIS AS MEDtube Science Jun. 2014; 2(2), 8-14. LIST OF THE FIGURES Fig. 1. Sir John Bertrand Gurdon (left) and Shinya Yamanka (right) during the Nobel Prize Award Ceremony [1]. Fig. 2. Potential uses of stem cells [2]. Fig. 3. Blastocyst opened to reveal the inner cell mass. Fig. 4. Developmental hierarchy in stem cell (SC) compartment [8]. FIG. 1. SIR JOHN BERTRAND GURDON (LEFT) AND SHINYA YAMANKA (RIGHT) DURING THE NOBEL PRIZE AWARD CEREMONY [1]. Reprogramming by transduction of 4 defined factors can be done with human cells [41]. Yamanaka’s group determined that the introduction of a mouse receptor for retroviruses into human dermal fibroblasts using a lentivirus improved the transduction efficiency from 20% to 60%. Yamanaka demostrated that retrovirus-mediated transfection of Oct3/4, Sox2, c-Myc and Klf4 generates human iPSCs that are similar to human embryonic stem cells in terms of morphology, proliferation, gene expression, surface markers and teratoma formation. iPSCs can differentiate into all three germ layers in vitro and form teratomas when are injected into immunodeficient MEDtube Science Jun, 2014; Vol.II (2) science 13 FIG. 2. POTENTIAL USES OF STEM CELLS [2]. LIST OF THE TABLES Table 1. Developmental hierarchy in stem cell (SC) compartment [7]. Table 2. Potential sources of stem cells [7]. TABLE 1. DEVELOPMENTAL HIERARCHY IN STEM CELL (SC) COMPARTMENT [7]. FIG. 3. TOTIPOTENT SCS Give rise to both embryo and placenta. The physiological totipotent stem cell is a zygote or first cleavage blastomeres. The artificial counterpart is a clonote obtained by nuclear transfer to an enucleated oocyte. PLURIPOTENT SCS Give rise to all three germ layers of the embryo after injection to the developing blastocyst. Pluripotent stem cells from the inner mass (ICM) of the blastocyst are known as embryonic stem cells (ESCs). MULTIPOTENT SCS Give rise to cells from one or two of the germ cells layers (ecto--, meso- or endoderm) only. MONOPOTENT SCS Tissue-committed stem cells that give rise to cells of one lineage, e. g. hematopoietic stem cells, epidermal stem cells, neural stem cells, liver stem cells, intestinal epithelium stem cells or skeletal muscle stem cells. BLASTOCYST OPENED TO REVEAL THE INNER CELL MASS. McHugh PR. Zygote and “Clonote” – The Ethical Use of Embryonic Stem Cells. NEJM 2004; 351 (3): 209-211 [43]. TABLE 2. POTENTIAL SOURCES OF STEM CELLS [7]. Pluripotent SCs isolated from banked embryons derived by fertilization Pluripotent SCs isolated from embryons derived by therapeutic cloning Pluripotent SCs isolated from adult tissues Pluripotent SCs obtained in result to somatic cell transformation (induced pluripotent stem cells iPSCs) Risk of teratomas formation + + -/? + HLA incompatibility + Donor of oocyte is required + + - - Ethical problems YES YES/NO* NO NO * The problem differently perceived by the major world religions. FIG. 4. DEVELOPMENTAL HIERARCHY IN STEM CELL (SC) COMPARTMENT [8]. LIST OF THE VIDEOS Video 1. The Nobel Prize Ceremony 2012. Video 2. The sources of stem cells. BIBLIOGRAPHY PGC – epiblast-derived primordial germ cells MEDtube Science Jun, 2014; Vol.II (2) 1. MLA style: „The Nobel Prize in Physiology or Medicine 2012”. Nobelprize.org. Nobel Media AB 2014. http://www.nobelprize. org/nobel_prizes/medicine/laureates/2012/, the last access: 20 Sep 2014, 01:20 p. m. 2. Häggström M. Medical galery of Mikael Häggström 2014. Wikiversity Journal of Medicine 1 (2). DOI:10.15347/ WJM/2014.008. ISSN 20018762. 3. Verfaillie CM. Adult stem cells: assessing the case for pluripotency. Trends Cell Biol. 2002; 12: 502-508. 4. Verfaillie C. Pluripotent stem cells. Transfusion Clinique et Biologique 2009; 16: 65-69. 5. Lodi D, Iannitti T, Palmieri B. Stem cells in clinical practise: applications and warning. Journal of Experimental & Clinical Cancer Research 2011; 30: 9-29. 6. Fortier LA. Stem Cells: Classifications, Controversies, and Clinical Applications. Veterinary Surgery 2005; 34: 415-423. 7. Ratajczak MZ and Suszyńska M. Quo vadis regenerative medicine? Acta Haematologica Polonica 2013; 44: 161-170. 8. Ratajczak MZ, Zuba-Surma EK, Wysoczynski M, Wan Wu, science 9. 14 Ratajczak J, Wojakowski W and Kucia M. Hunt for pluripotent stem cell – Regenerative medicine search for almighty cell. Journal of Autoimmunity 2008; 30: 151-162. 33. Yamanaka S. Strategies and new developments in the generation of patient-specific pluripotent stem cells. Cell Stem Cell 2007; 1: 39–49. Rideout WM, Rideout 3rd WM, Eggan K and Jaenisch R. Nuclear cloning and epigenetic reprogramming of the genome. Science 2001; 293: 1093-1098. 34. Yang X, Smith SL, Tian XC, Lewin HA, Jean-Paul Renard J-P and Wakayama T. Nuclear reprogramming of cloned embryos and ist implications for therapeutic cloning. Nature Genetics 2007; 39: 295-302. 10. Bongso A, Fong CY, Ng SC and Ratnam SS. Blastocyst transfer in human in vitro fertilization; the use of embryo coculture. Cell Biol. Int. 1994; 18: 1181-1189. 11. Shamblott MJ, Axelman J, Wang S et al. Derivation of pluripotent stem cells from cultured human primordial germ cells. Proc Natl Acad Sci USA 1998; 95: 13726-13731. 12. Hui H, Tang Y, Hu M and Zhao X. Stem Cells: General Features and Characteristics. Stem Cells in Clinic and Research 2011. ISBN: 978-953-307-797-0, InTech. http://www. intechpochen.com/books/stem-cells-in-clinic-and-research/ stem-cells=general-features-and-characteristics; the last acces: 20 Sep 2014, 01:08 p. m. 13. Rogers I and Casper RF. Umbilical cord blood stem cells. In Best Practice & Research Clinical Obstetrics & Ginecology, eds: N. Fisk & J. Itskovitz, London: Elsevier Ltd. 2004. 14. Gimble JM, Katz AJ and Bunnell BA. Adipose-derived stem cells for regenerative medicine. Circ Res 2007; 100 (9): 12491260. 15. Yagi H, Soto-Gutierrez A and Kitagawa Y et al. Bone marrow mesenchymal stromal cells attenuate organ injury induced by LPS and burn. Cell Transplant 2010; 19 (6): 823-830. 16. Owen ME. Marrow stromal stem cells. J Cell Sci Suppl 1988; 10: 63-76. 17. Körbling M and Freireich EJ. 25 years of peripheral blood stem cell transplantation. Blood 2003. 35. Hipp J and Atala A. Sources of Stem Cells for Regenerative Medicine. Stem Cell Rev 2008; 3: 3-11. 36. Ballas CB, Zielske SP and Gerson SL. Journal of Cellular Biochemistry – Supplement 2002; 38: 20-28. 37. Thomas ED, Lochte HL Jr, LU WC and Ferrebee JW. NEJM 1957; 257: 491-496. 38. Presnell SC, Petersen B and Heidaran M. Seminars in Cell & Developmental Biology 2002; 13: 369-376. 39. Spradling A, Drummond-Barbosa D and Kai T. Nature 2001; 414: 98-104. 40. Takahashi K and Yamanaka S. Induction of Pluripotent Stem Cells from Mouse Embryonic and Adult Fibroblast Cultures by Defined Factors. Cell 2006; 126, 663-676. 41. Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T, Tomoda K and Yamanaka S. Induction of Pluripotent Stem Cells from Adult Human Fibroblasts by Defined Factors. Cell 2007; 131 (5): 861-872. 42. Zhao R and Daley GQ. From Fibroblasts to iPs Cells: Induced Pluripotency by Defined Factors. Journal of Cellular Biochemistry 2008; 105: 949-955. 43. McHugh PR. Zygote and “Clonote” – The Ethical Use of Embryonic Stem Cells. NEJM 2004; 351 (3): 209-211. 18. Alison MR, Vig P, Russo F et al Hepatic stem cells: From inside and outside the liver? Cell Prolif 2004; 37: 1-21. 19. Fausto N. Cambell JS and Riehle KJ. Liver regeneration 2006. Hepatology 43 (2 suppl 1): 45-53. 20. Koniaris LG, McKillop IH and Schwartz SI et al. Liver regeneration. J Am Coll Surg 2003; 197: 634-659. 21. Alison2 MR, Poulsom R, Forbes S et al. An introduction to stem cells. J Path 2002; 197: 419-423. 22. Blanpain C, Lowry WE and Geohegan A et al. Self-renewal, multipotency, and the existence of two cell population within an epithelial stem cell niche. Cell 2004; 118: 530-532. 23. Levy V, Lindon C, Zheng Y, Harfe BD and Morgan BA. Epidermal stem cells arise from the hair follicle after wounding. The FASEB Journal 2007; 21: 1360-1366. 24. Gronthos S, Zannettino AC, Graves SE at al. Differential cell surface expression of STRO-1 and alkaline phospatase antigens on discrete developmental stages in primary cultures of human bone cells. J Bone Miner Res 1999; 14: 47-56. 25. Nuttall ME, Patton AJ, Olivera DL et al. Human trabecular bone cells are able to express both osteoblastic and adipocytic phenotype: Implications for osteopenic disorders. J Bone Miner Res 1998; 13: 371-382. 26. Metsaranta M, Kujala UM, Pelliniemi L et al. Evidence for insufficient chondrocytic differentiation during repair of full thickness defects of cartilage. Matrix Biol 1996; 15: 39-47. 27. Nakajima H, Goto T, Horikawa O et al. Characterization of cells in the repair tissue of full thickness of articular cartilage defects. Histochem Cell Biol 1998; 109: 331-338. 28. Mckay R. Stem cells in the central nervous system. Science 1997; 276: 66-71. 29. Gage FH. Mammalian neural stem cells. Science 2000; 287: 1433-1438. 30. Temple S. The development of neural stem cells. Nature 2001; 414: 112-117. 31. Moore JE, McMullen CB, Mahon G and Adamis AP. The corneal epithelial stem cell. DNA & Cell Biology 2002; 21: 443-451. 32. Daniels JT, Dart JKG, Turt SJ and Khaw PT. Corneal stem cells in review. Wound repair and regeneration 2001:483-494. MEDtube Science Jun, 2014; Vol.II (2)