* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download THYROID TUMOURS
Survey
Document related concepts
Transcript
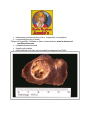
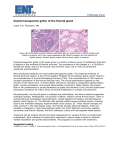
THYROID TUMOURS Benign – adenomas Malignant Solitary thyroid nodule – discrete nodule within normal thyroid gland. Mostly non neoplastic e.g. Hyperplasia, cysts etc as well as benign neoplasms Solitary Thyroid Nodule - more likely to be neoplastic than multiple nodules Nodules in younger patients have likelihood of being neoplastic than those in older patients Nodules in males - likelihood of being neoplastic DXT to head, neck - incidence of thyroid Cancer “Hot” nodules - likelihood of being benign ADENOMAS Follicular adenomas Discrete solitary masses; often non-functioning hence “cold” nodules Small no. may be functional thyrotoxicosis (“toxic adenomas” – “hot” nodules). This is independent of TSH stimulation Morphology Well-circumscribed nodule, surrounded by well-defined capsule; adjacent compressed thyroid tissue (diff from MNG); also growth pattern is distinct from adj non neoplastic thyroid*. Histo shows uniform closely packed colloid filled follicles of different sizes (macro, micro, trabecular, foetal) Variants – Hurthle cell, clear cell, signet ring cell etc. Nuclear pleomorphism & atypia may be present in few cases (does NOT imply malignancy) Important to examine capsule for integrity – INTACT CAPSULE NECESSARY TO QUALIFY AS AN ADENOMA Evaluation of adenomas Radioactive iodine uptake scan – usually “cold nodule” U/S – cystic/solid FNAC Biopsy – definitive diagnosis of adenoma vs. Cancer can ONLY BE MADE ON HISTOLOGY – adenoma should show NO capsular or vascular invasion CARCINOMAS Papillary Ca Follicular Ca Medullary Ca Anaplastic Ca PATHOGENESIS OF CA’S Genetic factors Follicular Ca – 50% have RAS mutations; translocations between PAX8 & the peroxisome proliferatorPPAR present in 30% Papillary Ca – mutations of tyrosine kinase receptors RET or NTRK1; mutations of BRAF oncogene; mutations of RAS oncogenes Medullary Ca – arise from parafollicular (C cells); familial cases associated with MEN 2; 95% show RET proto-oncogene mutations Anaplastic Ca – De Novo or de-differentiation of well differentiated papillary/ follicular Ca; p53 mutations impt. Environmental factors DXT – esp during 1st 2 decades of life (radiation to head and neck was used to treat tonsillar enlargement, acne, tinea capitis!) DXT as a risk factor – atom bomb, Chernobyl nuclear disaster (1986) associated with markedly high incidence of paediatric thyroid Cancer Papillary Ca Commonest thyroid Ca 20–40 yrs age Solitary/multifocal, often cystic Histo – Papillary structures (diff from those in hyperpl – fibrovasc cores, more complex, epithelium may be atypical) Psammoma bodies Characteristic nuclear features : Optically clear / “empty”/ ground glass/ “orphan Annie eye” nuclei Intranuclear pseudoinclusions (due to invagination of cytoplasm) Longitudinal grooving of nuclei *Diagnosis of papillary Ca based on these nuclear features even in absence of papillary structures. Lymphatic spread favoured. Usually cold nodules Unlike follicular Ca’s they can accurately be diagnosed on FNAC Follicular Cancer • • • • • • 2nd commonest cancer F>M, tend to be a decade older than pts with papillary Ca Morphology – uniform cells forming follicles with dense eosinophilic colloid No nuclear features of papillary Ca, no psammoma bodies Presence of capsular or vasc invasion May be minimally or widely invasive Medullary Carcinoma Neuroendocrine origin, from C cells calcitonin (useful in diagnosis & follow-up) 80% sporadic, remainder associated with MEN 2A or 2B or as familial tumours without assoc MEN synd (FMTC) MEN2 associated cases occur in young pts Familial cases – bilateral & multicentric Histo – polygonal to spindle shaped cells nests, trabeculae, follicles; amyloid deposition; surrounding thyroid tissue shows C cell hyperplasia in familial cases; presence of calcitonin – IHC Clin – mass effects, paraneoplastic synd caused by secretion of a peptide hormone eg VIP, serotonin, hypocalcaemia not prominent despite raised calcitonin levels Anaplastic Cancer • • • • • • Undifferentiated tumours Aggressive 50% have h/o MNG; 20% have h/o de-differentiated Ca; 20-30% have concurrent de-diff Ca, freq papillary Poor prognosis Histo – anaplastic cells, GC’s, MF’s, sarcomatoid appearance Clin – rapidly growing bulky neck mass, compression sympt common REFERENCE • • Robbins Basis of Pathology 8th edition Pages 1118 - 1126 THANK YOU