* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download here - HKU
Management of acute coronary syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
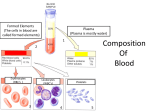
YPHY0001: Your lifestyle and your health A Healthy Heart • • • • • • • • • The heart lies at the centre of the cardiovascular system The heart is a muscular pump When heart muscle contracts, it squeezes blood out of the ventricle & into the artery The heart has 4 chambers: 2 atria and 2 ventricles The ventricles are the pumping chambers of the heart The ventricles of the heart eject blood at high pressure & high velocity After it has been ejected from the heart at high pressure, blood flows through blood vessels from high to low pressure, until it returns to the low-pressure chambers of the heart (the atria). blood = continuously circulated around the vascular system the heart gives the blood enough ENERGY to keep it flowing through the blood vessels Structures in the Heart • • • • • • • • • • • • • 1. Ventricles Ventricles are the muscular pumping chambers of the heart They convert chemical energy (ATP) to mechanical energy (muscle contraction) They transfer this energy to the blood by ejecting it out at high pressure & high velocity The structural properties of the ventricles are ideally suited to the pumping function: thick muscular walls allow a forceful contraction, which ejects the blood at high pressure Energy (pressure) required by the blood depends on the distance that the blood will travel The heart contains 2 pumps: The right ventricle pumps blood to the pulmonary circulation (lungs) for gas exchange • This distance is relatively short • The right ventricular muscle is thinner • It reaches a pressure of about 25 mmHg during contraction The left ventricle pumps blood to the systemic circulation (all the rest of the body) • This distance is longer • The left ventricular muscle is thicker • It reaches a pressure of about 120 mmHg during contraction 2. Valves Entrances to, & exits from, ventricles have valves Function = to prevent backflow of blood AV valves are flaps of connective tissue (valve leaflets) anchored to the ventricular muscle by tough “strings” of connective tissue (chordae tendinae) Semilunar valves are “pockets” of connective tissue in the walls of the arteries, just where they exit from the ventricles When ventricles contract: • Ventricular pressure = much higher than atrial pressure • Pressure pushes upwards on AV valve leaflets, which makes them move up to cover the hole • Atrio-ventricular (AV) valves close to stop blood flowing backwards from the ventricles to the atria • Chordae tendinae are attached to contracting ventricular muscle, which pulls down on the AV valve leaflets and stops them from being pushed right up into the atrium YPHY0001: Your lifestyle and your health • • • • • • • Outflow of blood from the ventricle flattens the semilunar valve pockets against the artery wall, so blood can flow out unimpeded When the ventricles relax after their contraction: • Ventricular pressure drops to zero • Arterial pressure is higher than ventricular, & blood starts to flow backwards towards the ventricle • The backflow fills the “pockets” of the semilunar valves,which occludes the artery and stops any further backflow • Semilunar valves close: blood from the arterty is prevented from entering the ventricle • Atrial pressure is higher than ventricular, so AV valves open • Blood flows from the atria into the ventricles • Blood flow pushes the valve leaflets flat against the ventricular walls so they do not impede the flow • Ventricles fill with blood (ready for the next contraction) 3. Atria Atria = thin-walled: ⇒ contraction is weak (~10mmHg) Mainly, they act as a passive conducting chamber: • Venous return of blood back to the heart is continuous • While the ventricles are contracting, AV valves are closed • Blood cannot enter the ventricles so it accumulates in the atria, which stretches them, & gradually raises atrial pressure When the ventricular contraction stops & the AV valves open, blood rushes from the atria into the ventricles Blood continues to flow back from the veins, through the atria, & into the ventricles (passive flow, pressure gradient) Just before the ventricular contraction, the atria contract, & squeeze the last ~20% of blood into the ventricles The Circulatory (Vascular) System AORTA ↓ LARGE ARTERIES ↓ SMALLER ARTERIES ↓ ARTERIOLES ↓ CAPILLARIES ↓ VENULES ↓ SMALL VEINS ↓ LARGE VEINS ↓ VENA CAVAE • 2 circulatory systems: systemic & pulmonary • pulmonary - deoxygenated blood through lungs • eliminate carbon dioxide • pick up more oxygen • systemic - oxygenated blood & nutrients to body • oxygen & nutrients diffuse into active cells • waste products diffuse from cells to blood YPHY0001: Your lifestyle and your health • • • • • • • • • • • • • • • • • • • • Aorta & large arteries Highly elastic Large diameter / low resistance Distribute blood to organs without using up much of its energy (pressure) Convert pulsatile cardiac output to continuous arterial flow Function = pressure storage / flow buffering Small arteries / arterioles Muscular & thick walled Spiral orientation of smooth muscle ⇒ contraction reduces diameter Function = resistance vessels (pre-capillary resistance) • maintain blood pressure • control distribution of blood among the various organs & tissues Control of blood flow rate: flow through a blood vessel depends on: • The “driving force” along the vessel, which is the pressure gradient • “How difficult” it is for blood to flow through the particular blood vessel, which is the resistance Capillaries Very thin wall Minimal barrier to diffusion Allows materials to exchange easily between the blood and tissues Veins & venules Thin wall, mainly smooth muscle Main function = volume storage Pressure acts: • in longitudinal direction to produce flow • outwards to stretch vessel Veins have thin walls: ⇒ they stretch easily Small pressure increase → large volume increase Veins are usually in a stretched state, which allows them to accommodate 75% of the total blood volume If the blood pressure drops, muscular walls of veins contract, which reduces the volume of the veins This returns extra blood to the heart, which increases cardiac output and blood pressure cardiac outpu Ìt Ì peripheral resistance È less flow from artery to capillary Ì Ë increased volume in artery È increased stretch of arterial wall È more potential energy transferred to wall È • higher pressure Both the heart and the blood vessels contribute equally to the determination of the blood pressure YPHY0001: Your lifestyle and your health • • • • • • Unusual properties of heart muscle Heart continues to beat at 75 bts/min (or more) throughout your entire life (= at least once every 0.8 seconds!) Cardiac output supplies blood flow to the entire body: ⇒ supplies oxygen & removes waste products from all cells of the body (including itself!) If the heart fails, the whole body dies Strongly dependent on the oxygen supply • Heart muscle cannot undergo anaerobic metabolism • At resting heart rates, most oxygen is extracted from the blood • Little “oxygen reserve” available Any increase in cardiac work requires an increase in coronary blood flow to supply additional oxygen for metabolism If the heart is weak or damaged, it creates a vicious cycle: Weak or damaged heart ↓ Weak contraction, smaller cardiac output ↓ Less blood supply to cardiac muscle ↓ Insufficient oxygen supply to cardiac muscle ↓ Further weakening & damage to heart muscle • • • • • • • • • • • • • • Ischaemic heart disease One of the most common diseases of the heart Coronary arteries become narrowed In milder cases, the blood supply to the heart is sufficient at rest, but can not increase when the heart needs to work harder (e.g. exercise) In severe cases, the heart can not even get enough blood supply at rest In the worst cases, a heart attack (myocardial infarction) occurs, and a piece of the heart dies! Narrowing of coronary arteries can occur in several ways: • Deposition of fatty material on the arterial wall (atherosclerosis) • Partial blockage by a blood clot • Spasm of the muscles in the arterial wall Consequences of cardiac ischaemia If the blood supply to the heart muscle is insufficient for its needs It does not have enough oxygen to create the energy stores (ATP) → feeling of fatigue It does not have a high enough flow rate to wash out the waste products → pain The accumulation of waste products further reduces the ability of heart muscle to contract → cardiac output drops → blood & oxygen supply to other regions is impaired (→ breathlessness) Mild disease may only be noticeable as poor exercise tolerance (feeling of fatigue & breathlessness) As the disease becomes worse, there is chest pain during exercise (exertional angina) Further progression → fatigue & breathlessness at rest, and chest pain with any mild exertion Heart attack is an acute event - a sudden decrease in blood supply e.g. blockage by a clot YPHY0001: Your lifestyle and your health • • • • • • • • Lifestyle factors & heart disease Many people develop atherosclerosis In some cases, this is for genetic reasons In other cases, it occurs due to poor lifestyle choices! Diet • Atherosclerosis is more likely to develop if the diet is: • High in fat • High in cholesterol • Low in antioxidants (fresh fruit & vegetables) • Different people have different tolerances to fat/cholesterol in the diet • Key factor is the serum level of lipid & cholesterol Lack of exercise • Exercise stimulates the growth of new blood vessels in the heart • During exercise, chemicals (growth factors) are released from the cells lining the blood vessels • Therefore, exercise improves the blood supply to the heart muscle • Exercise also lowers the blood pressure (reduces the hypertension risk factor) Cigarette smoking • Chemicals from the cigarette smoke enter the blood through the lungs • They damage the lining of the blood vessels • This increases the probability of atherosclerosis forming at the site of damage • Risk of coronary artery disease is in direct proportion to the number of cigarettes smoked • In a smoker, it takes 10 years of zero smoking for the risk to return to normal High blood pressure (poor compliance with medication) Diabetes mellitus (uncontrolled blood glucose) • Either high blood pressure or high blood glucose can damage the blood vessel lining • This increases the risk of atherosclerosis • Therefore it increases the risk of coronary artery disease • Persons with either of these diseases must always comply very carefully with medical regimes, or they may develop the additional problem of heart disease