* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Constrictive pericarditis after tuberculosis in
Survey
Document related concepts
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Myocardial infarction wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
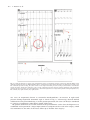
Grand Rounds Vol 11 pages 111–114 Specialities: Cardiology Article Type: Case Report DOI: 10.1102/1470-5206.2011.0025 ß 2011 e-MED Ltd Constrictive pericarditis after tuberculosis in adolescence Irina Kozarez, Gerhard Schuler and Steffen Desch Department of Cardiology, Heart Center Leipzig/University of Leipzig, Leipzig, Germany Corresponding address: I. Kozarez, Herzzentrum Leipzig, Strümpellstrasse 39, 04289 Leipzig, Germany. Email: [email protected] Date accepted for publication 21 October 2011 Abstract Constrictive pericarditis is a difficult diagnosis that requires a high degree of clinical suspicion due to unspecific signs and symptoms. We present a 73-year-old patient with symptoms of chronic heart failure. Cardiac catheterization revealed the diagnosis of constrictive pericarditis, likely as a late consequence after tuberculosis in adolescence. The patient underwent complete pericardectomy and had marked clinical improvement at follow-up. We describe the investigation and treatment options of this condition. Keywords Constricitive pericarditis; pressure tracing; pericardectomy. Case report The patient is a 73-year-old man with a known history of atrial fibrillation, pacemaker implantation due to total arteriovenous block, chronic renal failure (with an estimated glomerular filtration rate of 58.2 ml/min per 1.73 m2 according to the ‘‘modification of diet in renal disease’’ formula) and pulmonary tuberculosis several decades ago (1953). In the 3 months prior to admission the patient developed progressive exertional dyspnea accompanied by cyanosis of the lips. Physical examination revealed a right-sided pleural effusion and ascites. Echocardiography showed a left ventricular ejection fraction of 69% without any valve disorders, marked diastolic dysfunction, pericardial calcification and a small pericardial effusion. The patient underwent right and left heart catheterization under the working diagnosis of diastolic heart failure. Coronary angiography showed slight calcification of vessels without significant stenosis. Cardiac catheterization displayed several hemodynamic signs of constrictive pericarditis: Simultaneous right ventricular and left ventricular pressure curves were recorded. Dip and plateau (or square root) configuration of ventricular pressures reflects a rapid early diastolic filling of the ventricles, followed by lack of additional filling during late diastole (Fig. 1a). Near equalization of ventricular pressures during diastole and elevation of end diastolic right ventricular pressure (41/3 of right ventricular systolic pressure) are also evident in Fig. 1a. Fig. 1b displays the discordance of ventricular systolic pressures during the respiratory cycle (as left ventricular pressure increases during expiration, right ventricular pressure decreases (and This paper is available online at http://www.grandrounds-e-med.com. In the event of a change in the URL address, please use the DOI provided to locate the paper. 112 I. Kozarez et al. Fig. 1. (a) Dip and plateau (or square root) configuration (circle) of ventricular pressures (rapid early diastolic filling of the ventricles, followed by lack of additional filling due to compression in mid and late diastole). The black arrows point to the left ventricular pressure tracing, the yellow arrows to the right ventricular pressure tracing. (b) Discordance of ventricular systolic pressures during the respiratory cycle (as left ventricular pressure increases during expiration, right ventricular pressure decreases (and vice versa on inspiration). (c) Kussmaul sign (increase in right atrial pressure during inspiration). LV, left ventricle; RV, right ventricle; RA, right atrium. vice versa on inspiration), known as ventricular interdependence. An increase in right atrial pressure during inspiration (Kussmaul sign) is shown in Fig. 1c. Fluoroscopy showed marked calcification of the pericardium (Fig. 2). In the patient presented, the cause can likely be attributed to a history of pulmonary tuberculosis during adolescence. The patient underwent successful excision of the pericardium 8 weeks after the diagnosis was established and experienced a major improvement in symptoms in the weeks after surgery, which was maintained at the time of the latest follow-up (9 months after surgery). Constrictive pericarditis after tuberculosis in adolescence 113 Fig. 2. Pericardial thickening (red arrows). 758 left anterior oblique view without caudal or cranial angulation. The blue arrow points to a right atrial pacemaker lead, the yellow arrow to a right ventricular lead and the green arrow to a pigtail catheter in the left ventricle. Discussion The diagnosis of constrictive pericarditis is difficult because of its common clinical signs with many other possible diagnoses and the rarity of this condition. Constrictive pericarditis should be considered in patients with signs of right heart failure[1]. Tuberculosis is one of the known causes of the disease, although the incidence of tuberculosisrelated cases is declining. Other causes include scarring after open heart surgery, radiation therapy, direct trauma and viral infection[2]. Traditionally, increased pericardial thickness has been considered a specific diagnostic feature of constrictive pericarditis, but these days there is also a subset of patients with hemodynamic signs of constrictive pericarditis and normal thickness of the pericardium[3]. Several criteria on invasive pressure tracings have been examined for the diagnosis of constrictive pericarditis. Among these, the change in the ventricular pressure curves during the respiratory cycle (reflecting ventricular interdependence) is unique to patients with constrictive pericarditis[4]. According to guidelines, there are two therapeutic options for the treatment of constrictive pericarditis[5]: (i) pericardectomy which is considered the only definitive treatment and potential cure (although perioperative mortality is high); (ii) medical management, which is generally ineffective in most patients unless a prominent inflammatory component is present. A recent study has demonstrated a potential beneficial role of colchicine and also the use of corticosteroids in acute and recurrent pericarditis[6]. Survival after pericardectomy differs among the various causes and is best for idiopathic or miscellaneous forms of constrictive pericarditis[2]. There are no randomized trials that compare medical with surgical therapy. Teaching points Constricitive pericarditis is a difficult diagnosis that should be suspected in patients with symptoms and signs of right heart failure and a medical history compatible with the condition. The diagnosis can be established on the basis of clinical symptoms and several hemodynamic signs in catheter pressure curve tracings. 114 I. Kozarez et al. References 1. Asher CR, Klein AL. Diastolic heart failure: restrictive cardiomyopathy, constrictive pericarditis and cardiac tamponade: clinical and echocardiographic evaluation. Cardiol Rev 2002; 10: 214–29. 2. Bertog SC, Thambidorai SK, Parakh K, et al. Constrictive pericarditis: etiology and causespecific survival after pericardiectomy. J Am Coll Cardiol 2004; 43: 1445–52. doi:10.1016/ j.jacc.2003.11.048. 3. Talreja DR, Edwards WD, Danielson GK, et al. Constrictive pericarditis in 26 patients with histologically normal pericardial thickness. Circulation 2003; 108: 1852–7. doi:10.1161/ 01.CIR.0000087606.18453.FD. 4. Talreja DR, Nishimura RA, Oh JK, Holmes DR. Constrictive pericarditis in the modern era: novel criteria for diagnosis in the cardiac catheterization laboratory. J Am Coll Cardiol 2008; 51: 315–9. doi:10.1016/j.jacc.2007.09.039. 5. Maisch B, Seferović PM, Ristić AD, et al. Task Force on the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology. Guidelines on the diagnosis and management of pericardial diseases executive summary. Eur Heart J 2004; 25: 587–610. 6. Imazio M, Trinchero R, Brucato A, et al. COlchicine for the Prevention of the Postpericardiotomy Syndrome (COPPS): a multicentre, randomized, double-blind, placebo-controlled trial. Eur Heart J 2010; 31: 2749–54. doi:10.1093/eurheartj/ehq319.