* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download T CELL DEFICIENCY - immunology.unideb.hu
Infection control wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Neonatal infection wikipedia , lookup
Complement system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Innate immune system wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
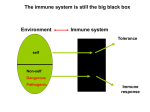
The immune system is still the big black box Environment Immune system Tolerance self Non-self Dangerous Pathogenic Immune response PATHOGENS HAVE SHORT GENERATION TIME PATOGENS Virus Bacteria 3 hrs Viruses 3 hrs Diversity Fast development parasites Humans have longer generation time, Need a sophysticated protection system Birth Development, education Reproducrion at 35 IMMUNODEFICIENCIES AGE AND HEALTH DEPENDENT IMMUNOSUPPRESSIVE DRUGS • INHERITED (PRIMARY) • ACQUIRED – Loss of function mutation of genes of the immune system – Enhanced susceptibility to infections – Particular types of pathogens depending on the gene defect – Did not show up until 1950 - antibiotics – Due to infectious diseases – AIDS – Other virus infections – Malnutrition – Artificial immunosuppression • Drugs • Radioactive irradiation PRIMARY IMMUNODEFICIENCIES • MOST ARE RECESSIVE MUTATION OF SINGLE GENES – Dominant traits have been eliminated from the population – Autosomal genes • Disease in homozygous children • Heterozygous children are carriers – X-linked genes • Single gene defect causes disease in males • Single gene defect in females renders the affected woman carrier – Mutation in the IFNγ receptor results in binding without intracellular signaling - dominant DISSEMINATED INFECTION BY THE BCG STRAIN OF Mycobacterium USED FOR VACCINATION The impact of recessive and dominant mutations in the IFN-γ receptor on monocyte activation. Numerous Immunodeficiency loci reside on the X chromosome CGD: Chronic Granulomatous Disease WAS: Wiscott-Aldrich Syndrome SCID: Severe Combined Immunodeficiency XLA: X-linked Agammaglobulinemia XLP: X-linked Lymphoproliferative Disease XLHM: X-linked Hyper-IgM Syndrome TYPES OF INHERITED IMMUNE DEFICIENCIES • ANTIBODY DEFICIENCY • T CELL DEFICIENCY • - recurrent sinopulmonary and GI infections beginning after 3-4 mo. • - SCID, opportunistic infections beginning early in infancy – T cell development – B cell development • (XLA, IgA deficiency) – B – T cell collaborations • CD40 ligand, hyper IgM • IL-7/Jak3 • RAG-1 RAG-2 • Artemis – Thymus epithelial cells • DiGeorge syndrome – Purin catabolism – DNS repair enzyme defect – MHC class II synthesis blockade TYPES OF INHERITED IMMUNE DEFICIENCIES 2. • PHAGOCYTIC SYSTEM – CD18 (CR3, CR4, LFA1) – NADPH oxidase (CGD) – Vesicular fusion • COMPLEMENT SYSTEM • some infections, primarily with encapsulated organisms and Neisseriae – Soluble and membrane factors – C3 – C1 – C4 – Complement inhibitors Immunodeficiencies caused by B-cell defects Approx. 70% of all IDs Late Manifestation (7-9 month) Increased sensitivity to: Encapsulated bacteria Streptococcus pneumoniae Haemophylus influenzae Infection by Enterovirus, parasites SERUM IG LEVELS AS THE DEVELOPMENT OF THE IMMUNE SYSTEM PROGRESSES „Who are missing?” ANTIBODY DEFICIENCY INABILITY TO CLEAR EXTRACELLULAR BACTERIA • X-LINKED AGAMMAGLOBULINEMIA XLA (Bruton’s agammaglobulinemia) 1:200,000 Symptoms – First few months of life is relatively normal (maternal Ig) – Tonsils are small, lymph nodes are barely palpable – Recurrent infection of sinuses and of the middle ear. Pneumonia. – Pyogenic bacteria – permanent tissue demage caused by enzyme release from bacteria and phagocytes bronchiectasis, chronic lung disease • Haemophilusinfluenzae, Streptococcus pneumoniae, Staphylococcus aureus, – Oral polio vaccine disseminate and cause poliomyelitis – T-cell responses to intracellular bacteria is normal (mycobacteria) – Lack of mature B cells plasma cells in the periphery ANTIBODY DEFICIENCY INABILITY TO CLEAR EXTRACELLULAR BACTERIA • X-LINKED AGAMMAGLOBULINEMIA XLA (Bruton’s agammaglobulinemia) Genetic defect – Mutation in the Bruton’s tyrosine kinase, essential for B cell activation and development – NO B CELLS IN THE PERIPHERY – block at pre-B cell stage – Carrier mother XX HEALTHY non-random inactivation of X in B cells – Son XY DISEASE Son XY HEALTHY – Increased susceptibility to bacteria and enteroviruses Treatment – monthly injections of Gamma glob. (IVIG) When a T-cell defect results in antibody deficiency X-LINKED HYPER IgM SYNDROME DIMINISHED ANTIBODY PRODUCTION AS A RESULT OF INHERITED DEFECT OF T CELL HELP • HYPER IgM SYNDROME (XLHIM) Symptoms – Susceptibility to pyogenic bacteria/opportunistic infection • Sensitivity to pyogenic bacteria Haemophilusinfluenzae, Streptococcus pneumoniae, Staphylococcus aureus • opportunistic infections – No specific antibody response to T-dependent antigens • low IgG, IgA, IgE – No germinal center formation – No leukocytosis but neutropenia – No macrophage activation by T cells CD40 – CD40L • opportunistic infections • sores and blisters in the mouth and throat • injection of GM-CSF (GMCSF is produced by macrophages) Lack of germinal centers in lymph nodes of X-linked Hyper-IgM syndrome patients DIMINISHED ANTIBODY PRODUCTION AS A RESULT OF INHERITED DEFECT OF T CELL HELP • HYPER IgM SYNDROME XLHIM Genetic defect Defect of the DC40L membrane receptor gene – X-linked, disease in males Treatment – antibiotics, – monthly injections of Gamma glob. (IVIG) – injection of GM-CSF (neutropenia) •HYPER IgM SYNDROME (Autosomal) -Intrinsic B cell defect, activation induced deaiminase (AID) deficiency. Cytidine uridine conversion. -The enyme is involved in affinity maturation and Ig. class switch - Lack of opportunistic infections SELECTIVE IgA DEFICIENCY 1/800 - Chronic lung disease, - Tendency to develop respiratory and gastrointestinal allergies and autoimmunity - Over 40% of patients have anti-IgA antibodies – blood products containing IgA can cause severe allergic response. -Some are related to MHC class III region Other receptors promoting isotype switching Interactions of B cell activation factor of the TNF family receptor (BAFF) and a proliferation-inducing ligand (APRIL) with their receptors BAFF-R, transmembrane activator and calcium-modulating ligand (CAML) interactor (TACI) and B cell maturation antigen (BCMA) control B cell development and homeostasis. BAFF binds to BAFF-R, TACI and BCMA, while APRIL binds only to TACI and BCMA. The functional outcomes of BAFF and APRIL interactions with their receptors are listed. Simultaneous binding of APRIL to TACI and heparan sulphate proteoglycans mediates IgA production. T CELL IMMUNODEFICIENCIES SEVERE COMBINED IMMUNODEFICIENCY SCID DEFECT IN T CELL FUNCTIONS T cells are involved in all aspects of adaptive immunity • Persistent and recurrent infections with a broader range of pathogens than patients with B cell deficiences • Neither T cell-dependent antibody response nor cellular immunity are functional • T-, B+ NK- SCID • T- B- NK+ X-LINKED SEVERE COMBINED IMMUNODEFICIENCY SCID (Over 50% of cases) Symptoms • Small body weight, failure to thrive • Persistent and recurrent infections with a broader range of pathogens than patients with B cell deficiences • Opportunistic infections (Candida albicans, Pneumocystis carnii pneumonia) Candida albicans infection in children with SCID Normal SCID The Hart shadow is clearly visible In the absence of the thymus SEVER COMBINED IMMUNODEFICIENCIES The SCID phenotype can be caused by various gene defects • X-SCID – The common γ-chain of interleukin receptors is mutated IL-7 receptor – Part of IL2,4,7,9, 15, 21 Receptor • • Autosomal SCID – mutation of Jak3 kinase IL-7 receptor-mediated signaling Defect in the catabolism of purin bases – autosomal (T- B- NK+) – Adenosine deaminase (ADA) mutation – mental retardation – Purin nucleotide phosphorilase (PNP) • Accumulation of purin metabolites • Highly toxiC for developing lymphocytes, • Mutation of RAG enzymes – autosomal (Omen syndrome T- B- SCID) – No or little somatic gene rearrangement (RAPIDLY FATAL) – No circulating peripheral lymphocytes or very narrow repertoire • Mutation of a DNA repair enzyme – autosomal – DNA-dependent protein kinase (DNA-PK) involved in the cleavage of hairpins in somatic gene rearrangement • Bare lymphocyte syndrome – inhibited MHC synthesis – No CD4+ T cell response – CIITA co-activátor, RFX promoter binding protein or other transcription factor mutation • DiGeorge szyndrome – Development of thymic epithelial cells is inhibited – T cell development is inhibited SEVER COMBINED IMMUNODEFICIENCIES The SCID phenotype can be caused by various gene defects • Defect in the catabolism of purin bases – autosomal (T- B- NK+) – Adenosine deaminase (ADA) mutation – mental retardation – Purin nucleotide phosphorilase (PNP) • Accumulation of purin metabolites • Highly toxic for developing T lymphocytes, less toxic for developing B lymphocytes Treatment: Bone marrow transplantation, preferably from a histocompatible sibling Gene therapy DiGeorge Syndrome • Hypoparathyroidism • Thymic hypoplasia leading to variable immunodeficiency Peripheral T cells missing or greatly reduced • Opprtunistic infections • Other features: • Characteristic facial expression • Deletion in 22q11 in > 80% • Affected gene(s) is a transcription factor in the T-box family called Tbx1 Immunodeficiency caused by defects in B and T cell development • Wiskott-Aldrich syndrome WAS – X-linked A disease of defective reorganization of the actin cytoskeleton Symptoms – Thrombocytopenia, small platelet size (decreased production of platelets in B. Marrow, increased destruction in spleen) – Eczema – No antibodies to carbohydrate antigens (role for T cells?) – pyogenic and opportunistic infections severe infection with varichella (chicken pox) and herpes simplex (impaired CD8+ T-cell response) – Rearrangement of cytoskeleton upon T cell activation in the polarized contact with B cells, macrophages and target cells – Low IgM high IgA, IgE serum levels – Pyogenic bacterial, and opportunistic infections – B cell lymphomas Genetic defect – Mutation in the WAS protein (WASP) expressed in white blood cells and megakaryocytes Treatment Bone marrow transplantation Wiskott-Aldrich syndrome WAS Defective T/B communication Expressed in white blood cells and megakaryocytes Capping of TCR is defective in WASP negative T cells resting anti CD3 treated T cells from wt-mice T cells from WASP-/- mice DEFECTS IN PHAGOCYTE FUNCTION ENHANCED SUSCEPTIBILITY TO BACTERIAL INFECTIONS • DEFICIENCY OF CD18/LEUKOCYTE ADHESION (LAD) – Common β-subunit of CR3, CR4 and LFA-1 – Blocked phagocyte migration from blood to infection site – Inhibited uptake and degradation of opsonized bacteria – Persistant infection with extracellular bacteria • Pyogenic infections • Defect in wound healing, severe inflammation of the gums Lethal within the first decade of life without bone marrow transplant Omphalitis in LAD I patient DEFECTS IN PHAGOCYTE FUNCTION ENHANCED SUSCEPTIBILITY TO BACTERIAL INFECTIONS CHRONIC GRANULOMATOUS DISEASE – CGD (1 million in the US) Mutation of NADPH oxidase – any of the 4 subunits (gp91 X-linked) No superoxid O2- radical antibacterial activity is compromised Chronic intracellularbacterial or fungal infections – granuloma formation Aspergilus pneumonia IFN-gamma improves resistance. Mechanism?? Defect of glucose-6-phosphate dehydrogenase and myeloperoxidase less severe phenotype Diagnosis: NBT + PMA treatment of neutrophils. Lack of blue colour in CGD CGD patient with skin infections due to Serratia marcescens CHRONIC GRANULOMATOUS DISEASE – CGD Phox complex NBT staining of neutrophils Healthy CGD Carrier DEFECTS IN PHAGOCYTE FUNCTION ENHANCED SUSCEPTIBILITY TO BACTERIAL INFECTIONS CHÉDIAK-HIGASHI SYNDROME Abnormal giant granules in a variety of cells leading to: -hypopigmentation/partial albinism hair and eyes -severe immunodeficiency - NK cell defect Defect in vesicle fusion mechanism phagocytosed material is not delivered to lysosomes Persistent and recurrent bacterial infections Patients with CHS exhibit hypopigmentation of the skin, eyes, and hair; prolonged bleeding times; large bruises; recurrent infections; abnormal natural killer cell function; Infections most commonly involve the skin, the lungs, and the respiratory tract and are usually due to Staphylococcus aureus, Streptococcus pyogenes, and Pneumococcus species. Defective melanization of melanosomes occurs in oculocutaneous albinism In melanocytes, autophagocytosis of melanosomes occurs. MUTATION OR FUNCTIONAL INACTIVATION OF SOLUBLE COMPLEMENT PROTEINS RESULTS IN IMMUNODEFICIENCY Classical Lectin MBL C1Inh C1 MASP C4 C2 Alternative B-factor D-faktor Properdin HANE* C3 Pyogenic infections immune complex disease I-factor H-faktor C5 C6 C7 C8 Neisseria-infection severe pyogenic infections C9 *HANE - hereditary angioneurotic edema Neisseria-infection immune complex disease Pyogenic infections immune complex disease Stabilizes alternative C3 convertase MUTATION OF MEMBRANE BOUND COMPLEMENT PROTEINS RESULTS IN IMMUNODEFICIENCY DAF (Decay Accelerating Factor) HRF (Homologous Restriction Factor) MIRL (Membrane inhibitor of Reactive Lysis) CR1 (complement receptor 1) LFA(complement receptor 3,4) Intravascular hemolysis SLE* association Pyogenic infections *SLE- systemic lupus erythematosus MIRL = CD59 DAF accelerates the decay of classical and alternative C3 convertase DEFECTS IN COMPLEMENT COMPONENTS IMPAIR ANTIBODY RESPONSES ACCUMULATION OF IMMUNE COMPLEXES • DEFICIENCY OF C3 OR ITS ACTIVATION – Susceptibility to pyogenic bacteria – inefficient opsonization • DEFICIENCY OF C5-C9 – Neisseria – NO complement mediated lysis • DEFICIENCY OF EARLY C1-C4 – No C3b and C4b fragments No CR1-mediated erythrocyte transport of immune complexes – Accumulation of immune complexes in blood, lymph, extracellular fluid deposition in tissues tissue demage macrophage activation inflammation • DEFICIENCY IN COMPLEMENT INHIBITORY FACTORS – I factor – uncontrolled C3 C3b C3 depletion inefficient opsonization – Decay Accelerating Factor DAF or CD59 MAC inhibitor – autoimmune-like condition lysis of autologous erythrocytes paroxysmal nocturnal hemoglobulinuria – C1 inhibitor – uncontrolled activation of the classical pathway vasoactive C2 accumulation of fluid in tissues – epiglottal swelling may lead to death by suffocation