* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Schizophrenia an Autoimmune Disorder
Survey
Document related concepts
Childhood immunizations in the United States wikipedia , lookup
DNA vaccination wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Common cold wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Inflammation wikipedia , lookup
Immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Molecular mimicry wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Autoimmunity wikipedia , lookup
Innate immune system wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Transcript
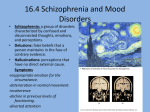
IMMUNOLOGY 1 Schizophrenia: an Autoimmune Disorder By Jennifer Kitchen March 4, 2013 IMMUNOLOGY 2 Schizophrenia is a mental disorder that can impair a person’s ability to function. A schizophrenic person may suffer from a wide array of pathological and behavioral issues. These symptoms, considered either positive or negative manifestations, can make daily living difficult. A schizophrenic person may suffer from positive manifestations, such as delusions, hallucinations, disorganized speech, and grossly disorganized or catatonic behavior (Frazier and Dryzmkowski, 2009). These symptoms make dealing with reality much harder but along with a loss of many main functions living can be a struggle. Negative manifestations of schizophrenia include affective flattening, (a disturbance of feeling and emotion), alogia (loss of language or the ability to communicate), and avolition (lack of motivation or drive) (Frazier and Dryzmkowski, 2009). Feelings of no purpose and no desire, along with the inability to convey these disturbances to others are daily struggles a schizophrenic person must deal with. Research into the underlying causes of these symptoms has come to some amazing discoveries in immunology and genetics. Relatives of a schizophrenic person have a greater risk, ten to one, of becoming schizophrenic than people who do not have a relative with schizophrenia, as this disorder is hereditary (Frazier and Dryzmkowski, 2009). Researchers have looked into the genetic link and found an association. Different gene loci have been located on chromosome 6p22.1 and researchers are considering them the most probable genes for schizophrenia (Müller and Schwarz, 2010). This region, 6p22, contains genes involved in immune regulation and the immune response is what “turns on” the schizophrenic genes. For decades, viruses have been seen as the promoter of this disorder but recently new findings show that it is not the virus or infectious agent, but the immune IMMUNOLOGY 3 response, which determines the risk for schizophrenia (Müller and Schwarz, 2010). This mental disorder is actually acquired through infection stimulating the immune response, which in turn affects a genetic aspect that “turns on” schizophrenia. The Immune Response and Schizophrenia Inflammation is usually the protective response tissues have to injury, which serves to destroy, dilute, or wall off both the injurious agent and the injured tissues. Inflammation may be caused by infectious injury due to a bacterium or virus. The reaction often helps protect the body. Research found signs of chronic inflammation of the brain (encephalitis) were seen in schizophrenics, which produces neurodegeneration (Müller and Schwarz, 2010). The neurodegenerative effects of this chronic immune response explain some of the symptoms seen in patients with schizophrenia. Cytokines are small proteins released by cells that have specific effects on the interactions between cells, communications between cells, or the behavior of cells. The cytokines includes the interleukins, lymphokines, and cell signal molecules, such as tumor necrosis factor and interferons. It can be shown that the cytokine, Interleukin-8, increases the risk for schizophrenia in offspring of mothers who had increased levels of this IL-8 during pregnancy (Müller and Schwarz, 2010). Interleukin-8 (IL-8) is a cytokine derived from endothelial cells, fibroblasts, keratinocytes, macrophages, and monocytes that causes chemotaxis of neutrophils and T-cell lymphocytes. Chemotaxis is a response leukocytes have to products, such as IL-8, formed by immunological reactions. In chemotaxis, leukocytes are attracted to and accumulate at the site of the IMMUNOLOGY 4 reaction as part of the inflammatory response. Other cytokines have also been shown to express neuropsychiatric side effects (depression, anxiety, hypomanic mood, etc.) in patients treated with, interferon-gamma and Interleukin-2 (IL-2) (Schwartz and Shechter, 2010). The proinflammatory response, when occurring in the central nervous system (CNS), can be mentally impairing if the reaction goes on for too long. The immune response is not made to stay active for long periods. The cytokines calling forth leukocytes to the site of infection or trauma and causing chronic inflammation is seen to increase risk for schizophrenia. Many studies are proposing a link between systemic inflammation and this disorder, viewing inflammation in the CNS as leukocytes attacking the brain (Schwartz and Shechter, 2010). When the immune system prolongs inflammation, abnormal behavior may ensue and long-term damage to the brain incurs. Schizophrenia can be seen as a degenerative disease, as the immune system attacks cells in the CNS, oligodendrocyte cell loss, impaired synaptic connectivity, and pyramidal cell dendrite shrinkage occur (Carter, C. J., 2011). The autoimmune response in actuality is killing the brain cells. Schizophrenia is a mental disorder brought about by an infection causing the immune system to over-react and causes a genetic “switch” to be turned on. There is no knowing if an individual has the precursor gene for schizophrenia without having a genetic test done to see if there is an abnormal sequence in chromosome 6p22.1. Still, more studies need to be done to confirm if this different gene loci is the culprit. Since schizophrenia is genetic, there is no vaccine to prevent it and the best anyone can do is comply with treatment if they are diagnosed with this disorder (Frazier and Dryzmkowski, 2009). Living life with the schizophrenia is an experience not everyone IMMUNOLOGY 5 can understand. Day to day living can be difficult, as well as simple daily tasks. The symptoms are often controlled by the use of anti-psychotic drugs, psychotherapy, and family support (Frazier and Dryzmkowski, 2009). With support and a plan, a person can avoid many psychotic breaks or episodes. Research into the causes of schizophrenic symptoms is leading to new discoveries in immunology and genetics. Chromosome 6p22 and the inflammatory response are going to need looked at further but may open up new doors to treatment someday soon. Not only may this research benefit schizophrenia patients, it may also lead to new interventions in other neuropathological disorders, such as bipolar disorder. Only time will tell what great discoveries come from the genetics and immunological fields. IMMUNOLOGY References Carter, C. J., (2011), Schizophrenia: a pathogenetic autoimmune disease caused by viruses and pathogens and dependent on genes. Journal of Pathogens; 2011. doi:10.4061/2011/128318. http://www.hindawi.com/journals/jpath/2011/128318/ . Frazier, M. S., and Dryzmkowski, J. W. (2009). Essentials of Human Diseases and Conditions (4th Ed.). St. Louis, MO: Saunders Elsevier Inc. Müller, N., and Schwarz, M.J., (2010). Immune System and Schizophrenia. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2971548/ . Schwartz, M. and Shechter, R., (April 2010). Protective autoimmunity functions by intracranial immunosurveillance to support the mind: the missing link between health and disease. Molecular Psychiatry 15: 342-354. doi:10.1038/mp.2010.31. http://www.nature.com/mp/journal/v15/n4/full/mp201031a.html . 6