* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PHENOTYPIC CHANGES IN IRRADIATED ENDOTHELIAL CELLS
Survey
Document related concepts
Transcript
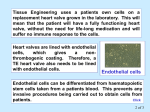
PHENOTYPIC CHANGES IN IRRADIATED ENDOTHELIAL CELLS: IMPLICATION OF THE ENDOTHELIAL TO MESENCHYMAL TRANSITION IN THE DEVELOPMENT OF HEALTHY DIGESTIVE TISSUE INJURY FOLLOWING RADIATION EXPOSURE Elodie Minteta, Valérie Buarda, Jean-Christophe Sabourinb, Marc Benderittera, Fabien Milliata and Agnès Françoisa a Radiobiology and Radiopathology Research Laboratory, Institute for Radiological Protection and Nuclear Safety, Fontenay-aux-Roses, France. b Department of Pathology, Rouen University Hospital, France Corresponding author’s email: [email protected] The exposure of the abdomino-pelvic region to ionizing radiation is associated with untoward healthy digestive tissue injury. Radiation fibrosis is characterized by an excessive and uncontrolled synthesis of extracellular matrix by mesenchymal cells. The endothelial to mesenchymal transition (EndoMT) is a process in which endothelial cells transdifferentiate into mesenchymal cells in response to stress. EndoMT was recently described as a possible source of mesenchymal cells contributing to fibrosis in injured heart, lung, and kidney, in a preclinical model of gastrointestinal inflammation, and in patients with ulcerative colitis and Crohn’s disease. The aim of this study was to determine the role of the EndoMT during the development of radio-induced intestinal fibrosis. Radiation-induced EndoMT was studied in vitro by analyzing the gene and protein expression profiles of irradiated human umbilical vein and intestinal microvascular endothelial cells (HUVEC and HIMEC) for different doses and times after irradiation. The induction of EndoMT was studied in vivo by using a model of transgenic mice expressing the green fluorescent protein (GFP) under the control of an endothelial specific promoter, Tie2. The Tie2-GFP mice received a single dose (27Gy) focalized on the colorectal region. A co-immunostaining of alpha-smooth muscle actin (α-SMA) and green fluorescent protein (GFP) was performed to identify mesenchymal cells having an endothelial origin. Irradiation induced the EndoMT process in HUVEC and HIMEC by increasing mesenchymal markers such as α-SMA and decreasing endothelial markers such as von Willebrand Factor (vWF), 7 days after 10Gy exposure. We also visualized an up-regulation at both gene and protein levels of the transcription factor Hey2, already known to take part in non-radio-induced EndoMT. Moreover, colocalization of α-SMA and vWF suggesting radiation-induced EndoMT was observed in mucosal and submucosal vessels of human rectum 6 weeks following radiation therapy for rectal adenocarcinoma. Finally, EndoMT process exists in our mouse model of radiation proctitis 7 and 14 days after irradiation. In conclusion, this is the first report of EndoMT as a putative participant to radiation-induced gut damage in vivo, and further studies will try to determine the role of Hey2 in the radio-induced EndoMT process in vitro and in vivo.