* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download lymphocyte homing migration recirculation
Immune system wikipedia , lookup
Atherosclerosis wikipedia , lookup
Duffy antigen system wikipedia , lookup
Innate immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
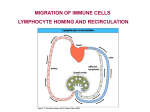
A BÉLFALHOZ KAPCSOLÓDÓ SZERVEZETT LIMFOID SZÖVET ÉS IZOLÁLT LIMFOID FOLLICULUS Villus Bél lumen Epithelium Kripta Peyer patch M sejt Izolált limfoid folliculus Lamina propria Nyirok Mesenteriális nyirokcsomó felé LYMPHOCYTE HOMING MIGRATION RECIRCULATION LYMPHOCYTE RECIRCULATION 1. Homing – most lymphocytes reside in lymphoid organs, few in circulation 2. Recruitment - chemokines Few antigen-specific lymphocytes should migrate to the site of antigen ANTIGEN RECOGNITION (lymph node) The appropriate effector lymphocyte populations shoud migrate to the site of antigen EFFECTOR/MEMORY CELLS (tissue, lymphoid tissue) 3. Migration Among tissues, organs Lymph node - Lymph node, Lymph node - Tissues BLOOD CIRCULATION - LYMPHATICS 4. Adhesion molecules HOMING RECEPTORS Antigen independent appearance (dependent on activation state of lymphocyte Selectins Integrins Ig supergene family molecules LIGANDS FOR VASCULAR ENDOTHELIAL CELL RECEPTORS Adressin ligands INTERACTION WITH THE EXTRAVASCULAR CONNECTIVE TISSUE Binding, detachement MIGRATION OF LYMPHOCYTES IN CENTRAL AND PERIPHERAL LYMPHOID ORGANS B BONE MARROW MALT SALT BALT SPLEEN T THYMUS BLOOD HEV TISSUES LYMPH NODES Lymphatics Thoracic duct 1. The central lymphoid organs are not connected to lymphatics – Isolated from the environment 2. The spleen has no lymph circulation – immune response to blood borne antigens 3. HEV – high endothelial venules – special entry sites of blood circulating lymphocytes to peripheral lymphoid organs 4. 1 lymph node circle/hour, 25 billion lymphocytes (25x109)/lymph nodes/day Role of endothelial cells in trafficking and recirculation Endothelial cells are involved in: Vasomotor tone, vascular permeability, regulation of coagulation, immune modulation and lymphocyte extravasation High endothelial venules Post-capillary venules Constitutively present in secondary lymphoid tissue Present in non-lymphoid tissues Need to allow egress of naïve cells from the circulation Molecules expressed by endothelial cells regulate trafficking and recirculation through lymphoid and non-lymphoid tissues MIGRATION OF LYMPHOCYTES NAIVE LYMPHOCYTES Homing to lymphoid tissues Homing receptor on naive lymphocyte L-selectin – carbohydrate binding Ligand on HEV - mucin-like adressin CD34+ and GlyCAM-1 sulphated sialyl-Lewisx Lymph node - PNAd – retention (peripheral node addressin) Naive lymphocyte L-selectin CD34 HEV HIGH ENDOTHELIAL VENULES HEV Lymphocytes slow down and bind to HEV LFA-1 integrin – ICAM-1/2 Ig family CCL21 chemokine and CCR7 chemokine receptor Limfocyte Homing I NAIVE LYMPHOCYTES Homing to lymphoid tissues Homing receptor on naive lymphocyte L-selectin – carbohydrate binding Ligand on HEV – mucin-like adressin CD34+ and GlyCAM-1 sulphated sialyl-Lewisx PSGL-1 Lymph node – PNAd - retention High endothelial venules HEV Blood enters lymph node via the artery Post capillary venules in the paracortex have cuboidal endothelial cells HIGH ENDOTHELIAL VENULES - specialised properties to allow lymphocytes and nothing else into the lymph node High endothelial venules Post capillary venules in 2º lymphoid tissue are called HIGH ENDOTHELIAL VENULES. Specialised to allow lymphocytes and nothing else into the lymph node Post capillary venules in other tissues are lined by simple squamous epithelium HEV Limfocita Homing II Extravasation HIGH ENDOTHELIAL VENULES HEV Lymphocytes slow down and bind to HEV LFA-1 integrin – ICAM-1/2 Ig family CCL21 chemokine and CCR7 chemokine receptor Initial lymphocyte adhesion to antigen presenting cell in LN EFFECTOR/MEMORY LYMPHOCYTES Return to the site of stimulation (antigen) Mucosal surface- MADCAM-1 Retention in spleen, lymph node LFA-1 – ICAM-1/2 integrin – cell and extracellular matrix Migration through activated endothelial cells of inflammed tissues Lamina propria in gut Mucosal epithelium Dermis in skin Activated/effector/memory lymphocyte LFA-1 ICAM-1 VLA-4 VCAM-1 Activated endothel ALTERED EXPRESSION OF CELL SURFACE ADHESION MOLECULES T-cell activated in mucosal tissue associated lymphoid tissues return to MALT Adhesion molecules and chemokines controlling T- cell homing to Lamina propria T-cell activated in mucosal tissue associated lymphoid tissues return to MALT Differences between armed, effector T cells and naïve T cells - Naïve CD4 cells CD44 LFA-1 CD45RA CD2 CD45RO VLA-4 Activated L-selectin Naïve Associates with TcR and CD4 - phosphatase activity reduces threshold of T cell signalling + + + + + - - - ++ ++ ++ - + ++ Homing to lymph node Adhesion molecules Homing Differential to inflamed splicing of vascular CD45 mRNA in naïve & armed endothelium T cells MIGRATION OF LYMPHOCYTES IN CENTRAL AND PERIPHERAL LYMPHOID ORGANS B BONE MARROW MALT SALT BALT SPLEEN T THYMUS BLOOD HEV TISSUES LYMPH NODES Lymphatics Thoracic duct 1. The central lymphoid organs are not connected to lymphatics – Isolated from the environment 2. The spleen has no lymph circulation – immune response to blood borne antigens 3. HEV – high endothelial venules – special entry sites of blood circulating lymphocytes to peripheral lymphoid organs 4. 1 lymph node circle/hour, 25 billion lymphocytes (25x109)/lymph nodes/day Elephantiasis caused by blockage of lymphatic vessels with Wuchereria bancrofti microfilariae INAPPROPRIATE DRAINAGE IN CHRONIC INFLAMMATION TOLERANT STATE