* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Pediatric Cardiac Emergencies
History of invasive and interventional cardiology wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Rheumatic fever wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Aortic stenosis wikipedia , lookup
Congenital heart defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
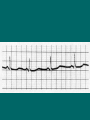
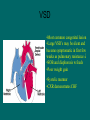
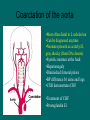
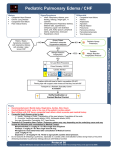
Pediatric Cardiac Emergencies Gavin Greenfield Peggy Thomsen • 4 year old female presents with fast breathing, “grunting”, cough x 5 days • seen 2 days earlier and started on steroids and bronchodilators • initial vitals: HR 150, BP 100/85, RR 36, T 37.5 • 1 month old with irritability, poor feeding (fatigues), failure to thrive, fast breathing • no fever or runny nose • physical exam: HR 160, RR 60 with minimal respiratory distress, gallop rhythm, rales Infant Cardiac Disease Leading to ER Presentation • Congenital • Acquired – Cardiomyopathy – Myocarditis (usually with CHF) – Dysrhythmias Congestive Heart Failure • the physiologic state in which cardiac output is unable to meet tissue metabolic demands (Rosen) • CO = HR x SV • SV dependent upon preload, afterload, contractility CHF - Presentation • infants: irritable, poor feeding (early fatigue), failure to thrive, respiratory symptoms • always consider in patients with respiratory symptoms – often misdiagnosed as respiratory illness / infection CHF - Etiology • Increased Preload – L to R shunts (VSD, PDA, AV fistula) – severe anemia • Increased Afterload – HTN – Congenital (aortic stenosis, coarctation of aorta) • Decreased Contractility – – – – – – myocarditis, pericarditis with tamponade cardiomyopathy (dilated or hypertrophic) Kawasaki syndrome (early phase) metabolic: electrolyte, hypothyroid myocardial contusion toxins: dig, calcium channel blockers, beta blockers • Dysrhythmia CHF - Etiology • presents immediately at birth – anemia, acidosis, hypoxia, hypoglycemia, hypocalcemia, sepsis • presents at 1 day (congenital) – PDA in premature infants • presents in first month (congenital) – HPLV, aortic stenosis, coarctation, VSD presents later • presents later (acquired) – myocarditis, cardiomyopathy (dilated or hypertrophic), SVT, severe anemia, rheumatic fever Myocarditis • leading cause of dilated cardiomyopathy and one of the most common causes of CHF in children • etiology: idiopathic, viral, bacterial, parasitic • hallmark is CHF • failure to respond to bronchodilators in wheezing child • treatment includes inotropes, afterload reduction, diuretics, antibiotics, antivirals Pericarditis • sharp stabbing precordial pain • worse with supine and better leaning forward • no sensory innervation of the pericardium – pain referred from diaphragmatic and pleural irritation Etiology • infectious – – – – – viral bacterial TB fungal parasitic • Connective tissue – RA – Rheumatic fever – SLE • Metabolic / Endocrine – uremia – hypothyroid • Hematology / Oncology – bleeding diathesis – malignancy • Trauma • Iatrogenic Pericarditis • usually a benign course • virulent bacteria (H. flu, E. coli) can cause constrictive pericarditis and subsequent tamponade – may need urgent pericardiocentesis • uncomplicated pericarditis usually responds to rest and anti-inflammatories Chest Pain • 4% of children will have a cardiac origin • remainder: MSK, pulmonic (asthma, bronchitis, pneumonia), GI • Cardiac causes: myocarditis, pericarditis, structural abnormalities such as congenital heart disease or hypertrophic cardiomyopathy • 14 year old male collapses at school while in class • non-responsive for one minute • feels fine in the department • Approach? Syncope • 20-50% of adolescents experience at least one episode of syncope – most cases benign • Pathophysiology – vascular – orthostatic, hypovolemia – neurally mediated – hypoxia: PE, CNS depression from OD, CO – cardiac Cardiac Syncope • Dysrhythmias – tachy – brady • Outflow obstruction • Myocardial Dysfunction • cardiac syncope often precedes future sudden cardiac death Sudden Cardiac Death • includes those causes that directly relate to cardiovascular dysfunction • one third of all sudden deaths Sudden Cardiac Death • Etiology – – – – – – – – – – myocarditis cardiomyopathy (hypertrophic) cyanotic and noncyanotic congenital heart disease valvular heart disease congenital complete heart block WPW long QT syndrome Marfan syndrome coronary artery disease anomalous coronary arteries Risk Factors for Serious Cause of Syncope • history of cardiac disease in patient • FH of sudden death, cardiac disease, or deafness • recurrent episodes • recumbent episode • exertional • prolonged loss of consciousness • associated chest pain or palpitations • medications that can alter cardiac conduction What to look for in the Department: EKG • Long QT syndrome – congenital or acquired – get paroxysmal v tach with torsades de pointes – congenital long QT associated with hypertrophic cardiomyopathy – long QT defined as corrected QT longer than 0.44 s – T wave alternans sometimes present – can have normal ECG in the department – two clinical syndromes not associated with structural heart disease: Romano-Ward and Jervell-LangeNielsen Other dysrhythmias • WPW and other SVT’s • AV block – usually acquired, rarely congenital • Sick sinus syndrome Idiopathic Hypertrophic Cardiomyopathy • aka IHSS • both a fixed and dynamic subvalvular obstruction • characterized by ventricular hypertrophy with principle involvement of the ventricular septum • associated with long QT • autosomal dominant • often presents with exertional syncope • 10 year mortality is 50% for children diagnosed by age 14 Other structural cardiac diseases • dilated cardiomyopathy – usually secondary to myocarditis – syncope and death secondary to ventricular dysrhythmias or severe myocardial dysfunction • arrhythmogenic RV dysplasia • congenital cyanotic and non-cyanotic heart disease • valvular diseases – aortic stenosis • coronary artery anomalies – exertional syncope or sudden death – aberrant artery passes between aorta and pulmonary artery • 2 week old infant brought in by parents with difficulty breathing • HR 180, BP 50/P, RR 80, T 37.5 • history and physical • investigations • repeat vitals: HR 30, no BP, RR 12 • “definitive treatment”: • 4 year old male presents with 2 weeks history of cough, fast breathing, fatigue, decreased exercise tolerance, “puffy eyes” • On exam: tachypneic, moderate respiratory distress, O2 sats 92%, bilateral crackles • 6 month male presents with failure to thrive, fast breathing, blue lips • On exam tachypnea but no respiratory distress, lips and extremities blue, oxygen saturations 70% Congenital Heart Disease • Fetal to Neonatal Circulation Anatomic Classification; 4 groups • Right to Left Shunt – Tetralogy of Fallot – Transposition of the Great Arteries – Tricuspid Atresia • Left to Right Shunt – ASD – VSD – PDA • Stenotic – Aortic valve stenosis – Pulmonic valve stenosis – Aortic coarctation • Mixing – Truncus – Total Anomalous Pulmonary Venous CHD Classified as Cyanotic vs. Acyanotic • Cyanotic (R to L shunt and mixing lesions) – tetralogy of Fallot – transposition of great vessels – tricuspid atresia – total anomalous pulmonary venous return – truncus arteriosus – hypoplastic left heart syndrome CHD Classified as Cyanotic vs. Acyanotic • Acyanotic (L to R shunts, stenotic lesions) – ASD – VSD – PDA – aortic valve stenosis – pulmonic valve stenosis – aortic coarctation Cyanosis • Classified as central or peripheral • Central cyanosis (always abnormal) – mucous membranes, trunk, extremities – classified as cardiac (R to L shunt) or pulmonary • Peripheral cyanosis (acrocyanosis) – – – – no involvement of mucous membranes involves hands, feet, circumoral area common in neonates from vasomotor instability CHF, PVD, shock, cold extremities Congenital Heart Disease • History – feeding difficulties – tachypnea – diaphoresis – syncope – cyanotic episodes – failure to thrive Congenital Heart Disease • Physical Examination – colour: pink, blue, gray – vitals: tachypnea, tachycardia, BP – symptoms suggestive of infection – palpation and auscultation of precordium – chest auscultation – survey for organomegaly – pulses in all extremities Cyanotic Congenital Heart Disease • R to L shunts • mixing lesions Tetralogy of Fallot – the classic cyanotic lesion • RV outflow obstruction • RVH • VSD • overriding aorta • CXR reveals boot shaped heart with decreased pulmonary blood flow • 2 month old female with known tetralogy of Fallot brought in with 24 hour history of vomiting and diarrhea • On exam: moderate dehydration • during IV attempts patient becomes irritable and cyanotic Treatment of Tet Spell • quiet, calm environment • knee-chest or squatting position – increases afterload thus decreasing R to L shunting • Oxygen • Morphine – to treat hyperpnea and decrease systemic catecholamines • Phenylephrine – increases afterload thereby decreasing R to L shunt • Manual external aortic compression below level of renal arteries • Propranolol – to block beta receptors in infundibulum therefore lessening RV outflow obstruction Consider • consider small volume challenge (5-10 cc/kg) to increase preload and reduce dynamic outflow obstruction • ?NaHCO3 for correction of acidosis • may need general anesthesia if severe and/or prolonged spell • interim prophylactic treatment with propranolol while awaiting surgery Acyanotic Congenital Heart Disease • L to R shunts • stenotic lesions VSD •Most common congenital lesion •Large VSD’s may be silent and become symptomatic in first few weeks as pulmonary resistance •SOB and diaphoresis w feeds •Poor weight gain •Systolic murmur •CXR demonstrates CHF • 2 week old infant brought in by parents with difficulty breathing • HR 180, BP 50/P, RR 80, T 37.5 • history and physical • investigations • repeat vitals: HR 30, no BP, RR 12 • “definitive treatment”: Differential Dx of Infant Shock • infection (septic shock/ meningitis) – bacterial: GBS, E. coli, S. aureus – virus: enteroviruses, H. simplex • metabolic: amino/organic acidopathies, urea cycle defect • ‘hypoxic shock’: eg. RSV, C.N.S. depression • heart disease: congenital or acquired LV Outflow Obstruction LV Outflow Obstruction • Aortic coarctation • Hypoplastic left heart syndrome • Aortic stenosis (presents later) • Rosen: “any neonate in shock that does not respond to fluids or pressors has LV outflow obstruction until proven otherwise” • complete obstruction incompatible with life unless there is shunting Coarctation of the aorta •Most often distal to L subclavian •Can be diagnosed anytime •Neonates present as acutely ill, gray shocky (from DA closure) •Systolic murmur at the back •Hepatomegaly •Diminished femoral pulses •BP difference b/t arms and legs •CXR demonstrates CHF •Treatment of CHF •Prostaglandin E1 Duct Dependant Lesions • Duct needed to perfuse lungs or periphery • Lungs – Tetralogy of Fallot, transposition of great arteries, tricuspid or pulmonary atresia • a patent ductus arteriosus results in preserved pulmonary blood flow • Periphery – Aortic coarctation (severe) and Hypoplastic left heart Treatment of acute decline in patients with ductal dependant lesions • Open the closed duct • Prostaglandin E1 0.1 ug/kg/min infusion • reduce dosage as perfusion and colour return • Rosen: “any infant in the first week of life with decreased perfusion, hypotension, or acidosis should be considered a candidate for PGE1 administration” What do you need to know about PGE ? • it functions by dilating vascular smooth muscle, both systemically and in the pulmonary vascular bed • it’s use in CHD pts’ is to maintain patency of the PDA, whether to maintain PBF or to maintain systemic blood flow past a Classification Review • pink child in respiratory distress suggests acyanotic chd (L to R shunt, coarct, aortic stenosis) • blue cyanotic child in little respiratory distress suggests R to L shunt or mixing lesions • gray, shocky baby suggests outflow tract obstruction Bradyarrhythmias • Etiology – hypoxia, acidosis, hypoglycemia – excess vagal stimulation (ex. intubation) • Treatment – Epinephrine – Atropine if known vagally mediated or heart block Congenital Bradyarrhythmias • complete AV block – autoimmune injury to fetal conduction system secondary to maternal autoimmune disease – atropine, isoproteronol, epinephrine may be tried temporarily prior to pacing Tachyarrhythmias • Supraventricular Tachycardia – re-entrant with accessory pathway (AV nodal or WPW) – re-entrant without accessory pathway (reentry occurs within sinus node or within atrium) – ectopic • nonspecific presentations in infants Murmurs • Areas – aortic: R 2nd intercostal space – pulmonic: L 2nd intercostal space – mitral: apex – tricuspid and VSD: L lower sternal border • Pathologic – diastolic, holosystolic, late systolic, continuous Innocent Heart Murmurs • History – normal growth and development, normal exercise tolerance – no history of cyanosis • Physical Examination – – – – Grade II or less, localized varies with position (decreased with upright posture) normal precordium normal pulses • Lab – normal EKG, normal CXR 3 innocent murmurs • Still’s – short ejection systolic murmur – musical or vibratory quality – heard best between apex and left sternal border • physiologic pulmonary flow murmur – harsh, located at pulmonic area • peripheral arterial stenosis – low-intensity systolic ejection murmur best heard in axilla and back • 8 year old male presents with fever, arthralgias • mother mentions that he had a sore throat 3 weeks ago for a few days with spontaneous resolution • a throat swab was done and positive for GAS but patient better so did not take the prescribed antibiotics Acute Rheumatic Fever • school aged children • associated with certain strains of Group A betahemolytic streptococcal infections • the streptococcal organism stimulated antibody production to host tissues – CT of heart, joints, CNS, subcutaneous tissues, skin • carditis is an endomyocarditis with valvulitis involving mitral and aortic valves • 2 to 6 weeks post streptococcal pharyngitis Jones Criteria • Major – carditis • new or changing murmur • cardiomegaly, CHF • pericarditis – – – – migratory polyarthritis chorea erythema marginatum subcutaneous nodules • Minor – fever – arthralgia – history of previous ARF – elevated ESR, CRP – prolonged PR on EKG – Rising titer of antistreptococcal antibodies ER Treatment • management of complicating features of carditis (CHF) – significant carditis or CHF managed with glucocorticoids • high-dose ASA 75-100 mg/kg/day • pencillin • long term management of rheumatic heart disease Pediatric EKG’s General Principles • RV Dominance at birth; gradually changes to LV dominance • axis up to +180 in normal newborn • T waves negative in right precordial leads until adolescence (except they are upright in first week of life)