* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Failure
NK1 receptor antagonist wikipedia , lookup
Plateau principle wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Metalloprotease inhibitor wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Discovery and development of beta-blockers wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Psychopharmacology wikipedia , lookup
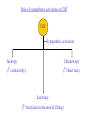
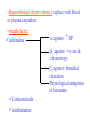
Renin inhibitors Renin Heart Failure Inotropic agents -Blockers ACE Sympathetic activity Angiotensin II ARBs Vasoconstriction Aldosterone Vasodilators Spironolactone Cardiac remodeling CO Na+, water retention Diuretics Cardiac filling Role of sympathetic activation in CHF CHF Sympathetic activation Inotropy Chronotropy ( contractility) ( Heart rate) Lusitropy ( Ventricular relaxation & filling) -Adrenoceptor antagonists: • agonists dobutamine as also dopamine provide relief in CHF but their long term use increases mortality •Long term administration of -antagonists reduce mortality rate in CHF •Initially the systolic function decreases but over 2-4 months it recovers and improvement beyond baseline occurs •Mechanism of beneficial effects in CHF not clear By preventing myocardial ischemia without significantly influencing serum electrolytes, they may decrease frequency of unstable tachyarrhythmias Betterment of left ventricular morphology by decreasing left ventricular size and increasing ejection fraction By inhibiting sustained sympathetic discharge, they reduce catecholamine induced cardiomyote toxicity and prevent or delay myocardial contractile dysfunction Decrease cardiomyocyte apoptosis May induce positive myocardial remodeling by decreasing oxidative stress on myocardium •Drugs used: metoprolol, carvedilol, bisoprolol- other -blockers are not effective •Combined and blocker is preferred •Carvedilol has additional advantages that it reduces free radical induced lipid peroxidation and prevents cardiac and vascular smooth muscle mitogenesis independent of its or receptor blocking activity • Adrenoceptor blockers have proven utility in improving symptoms, hospitalization and mortality in patients of CHF •They are recommended for use in patients along with ACE inhibitors or ARBs •Recommended only when the ejection fraction of heart is <35% to counter the deleterious effects of circulating catecholamines •They are usually given in small doses initially, less than 1/10th of the final dose and gradually titration of dose is done •Not recommended for use in patients with severe, new onset or acutely decompensated CHF Heart Failure Inotropes- for increasing ventricular contractions: •Cardiac glycosides- digitalis, digoxin, oubain • Adrenergic and dopaminergic agonistsdobutamine •PDE inhibitors- Inamrinone, milrinone Cardiac cell Ca2+ 3 Na+ Ca2+ Cations NCX Ca2+ Depolarised ATPase Ryanodine receptor (RyR2) K+ SR SERCA2 Na+ Ca2+ Ca2+ NCX 2 K+ Ca2+ Na+K+ (LType) ATPase 3 Na+ Polarised Na+ •Na+K+ATPase •H+K+ATPase •Cardiac glycosides bind and inhibit the phosphorylated sub unit of sarcolemal Na+K+ATPase •They Na+ extrusion from cell and its level in cell •At therapeutic serum levels they: Increase vagal tone and decrease sympathetic tone Decrease automaticity Increase maximal diastolic resting membrane potential in atrial and AV nodal tissues Prolongs ERP and slows conduction in AV nodal tissues These effects result in sinus bradycardia or arrest, prolongation of AV nodal conduction and AV block •In higher concentrations it increases sympathetic activity. Simultaneously, there is Ca2+ overload which together may cause development of cardiac arrhythmias •Non-cardiac effects: Blood vessels- constriction (direct) in normal; in CHF vasodilatation due to decreased sympathetic activity Kidney- Diuresis GIT- anorexia, nausea,vomiting (CTZ) CNS- disorientation, hallucinations, visual & colour disturbances •Uses: CHF PSVT Atrial flutter/Atrial fibrillation ADRs: • Cardiac • CNS- fatigue, neuralgia, blurred vision • GIT- anorexia, nausea, vomiting, abdominal cramps • Endocrinal- gynaecomastia in males Contraindications: Hypokalemia, children below 10 years age, elderly with renal/hepatic impairment MI, hypothyroidism, myocarditis Dobutamine: •Racemic mixture that stimulates both 1 and 2 receptors and (-) enantiomer that is agonist and (+) enatiomer that is partial agonist of adrenoceptors •1-positive ionotropic and increase in stroke volume •Relatively little increase in heart rate •Vasoconstriction by (-) enantiomer is countered by (+) enatiomer and 2 agonist activity- ultimate result is a decrease in PVR and mild decrease in systemic blood pressure •Continuous infusion 2-3 g/kg/min •Tolerance may occur after some time •ADRs: tachycardia, arrhythmias PDE Inhibitors: Inamirinone, milrinone •Decrease cellular degradation of cAMP resulting in increased levels in cardiac and smooth muscle myocytes •Produces positive inotropic effect on heart and dilatation of resistance and capacitance vessels •Nett effect: positive ionotropy and decrease in pre and after load resulting in improvement in cardiac output •Also called “inodilator” (inotropy + vessel dilatation) •Theophylline, caffeine have low cardiac specificity and side effects, so are not used •Inamirinone and milrinone are selective PDE3 inhibitors •Directly stimulate myocardial contractility & relaxation Shock •Haemorrhaegic (hypovolemic): replace with blood or plasma expanders •Anaphylactic : Adrenaline agonist- BP 1 agonist- +ve ino & chronotropy 2 agonist- bronchial relaxation Physiological antagonist of histamine Corticosteroids Antihistamine •Cardiogenic: Dopamine hydrochloride 2-5 g/kg/min i.v. infusion till a maximal dose of 20-50 g/kg/min is achieved Dobutamine NE- rare- reserved for patients with refractory hypotension •Septicemic (warm shock): Dopamine hydrochloride Chemotherapeutic agent Recombinant activated protein- C known as drotrecogin alpha (activated)- continuous infusion 24 g/kg/hr for 96 hrs, improves rate of mortality Vasopressin (ADH)- peripheral vasoconstriction by V1 receptors Corticosteroids Adrenaline, dobutamine