* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 212_spring_2005_Platelets
Artificial gene synthesis wikipedia , lookup
Mitogen-activated protein kinase wikipedia , lookup
Two-hybrid screening wikipedia , lookup
Western blot wikipedia , lookup
Endocannabinoid system wikipedia , lookup
G protein–coupled receptor wikipedia , lookup
Proteolysis wikipedia , lookup
Paracrine signalling wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Lipid signaling wikipedia , lookup
Proteases in angiogenesis wikipedia , lookup
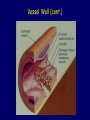
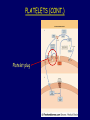
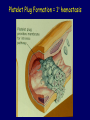
Hemostasis & Thrombosis: Platelet Disorders Beth A. Bouchard BIOC 212: Biochemistry of Human Disease Spring 2005 HEMOSTASIS Hemorrhage Thrombosis Hemostasis HEMOSTASIS (CONT.) 1). INITIATION Vessel wall – endothelial cells and subendothelial components 2). LOCALIZATION Platelets – circulating cellular elements 3). PROPAGATION/AMPLIFICATION Plasma coagulation proteins (factors) 4). TERMINATION Plasma coagulation protein inhibitors 5). ELIMINATION Fibrinolytic system Vessel Wall: Endothelial cells • Physically separate platelets from subendothelial proteins that can induce platelet activation • Produce 2 potent vasodilators and inhibitors of platelet function: prostacyclin (prostaglandin I2, PGI2) and nitric oxide Increase the concentration of the cyclic nucleotides cGMP and cAMP in platelets, which down regulate the signalling pathways that support platelet activation • Express CD39 on their surface, which enzymatically hydrolzes ADP, a potent platelet agonist release by activated platelets Vessel Wall (cont.) Response to Vessel Wall Injury: Platelet adhesion and activation • Exposure of flowing blood and platelets to subendothelial components • Platelets bind to the subendothelial collagen bound to von Willebrand factor (vWF), which is secreted from endothelial cells directly into the subendothelial space or adsorbed from plasma following endothelial cell secretion • vWf also binds directly to platelets via glycoprotein Ib-IX • Platelet interactions with collagen (via a specific platelet membrane receptor) and platelet activating factor (PAF), from the vessel wall, leads to their activation Platelets adhered to damaged endothelium Response to Vessel Wall Injury: Vasoconstriction • Temporarily reduces local blood flow and hence, blood loss • Mediated in part by serotonin and thromboxane A2 (TXA2) from activated platelets Serotonin is released from platelet dense granules TXA2 is a product of platelet prostaglandin metabolism PLATELETS PLATELETS (CONT.) Platelet plug Platelet Plug Formation = 1° hemostasis Platelet Plug Formation: Platelet activation • Bind to subendothelial proteins and associated vWF subsequent to blood vessel injury • Activated via their interaction with collagen and PAF • Additional platelet agonists include ADP, epinephrine, thrombin, immune complexes, and high shear stress – all of the compounds interact with specific platelet membrane receptors • Several platelet activation pathways are initiated Platelet Plug Formation: Platelet activation events • Platelet shape change: extend pseudopodia, which facilitates aggregation and coagulant activity • Release of alpha and dense granule contents including a number of compounds involved in hemostasis • Aggregation Activated platelets Platelet Plug Formation: Platelet aggregation • Platelet activation results in the functional expression of membrane receptors normally expressed in a non-functional state (glycoprotein IIb-IIIa) • Fibrinogen from the plasma or released from activated platelet alpha-granules binds to activated glycoprotein IIb-IIIa membrane receptors effectively bridging platelets to each other Platelets adhered to and aggregated upon collagen Platelet Plug Formation Platelet Plug Formation • Measured clinically as the bleeding time • Normal bleeding time is from 2 – 10 min • Usually the bleeding time is sufficient to detect defects of platelet adhesion and aggregation, in which it is prolonged Disorders of Platelet Adhesion or Aggregation • Affecting constituents of the vessel wall • Affecting the ability of the platelet to interact with the subendothelium at sites of blood vessel injury • Affecting the ability of the platelet to interact with other platelets Vessel Wall Defects • von Willebrand’s disease: a group of autosomal dominant disorders that result in reduced or abnormal synthesis of vWF • Defects in collagen synthesis Ehlers-Danlos Syndrome: congenital defect in collagen synthesis Scurvy: results from vitamin C (ascorbic acid) deficiency, which is involved in collagen synthesis Excess exogenous or endogenous corticosteroids: also leads to acquired deficiency in collagen synthesis Platelet Defects • Bernard-Soulier Syndrome: expression of low levels of or defective glycoprotein IbIX on the platelet surface • Glanzmann’s thrombasthenia: expression of low levels of or defective glycoprotein IIb-IIIa on the platelet surface Other Defects • Fibrinogen: deficiency or production of abnormal protein • Acquired disorders include low platelet count (thrombocytopenia) as a result of defective formation of platelets by the bone marrow or excessive destruction of platelets Antiplatelet Drugs