* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 23 outline
Survey
Document related concepts
Transcript
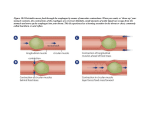
Chapter 23 Digestive System Overview of the Digestive System A. Role of the digestive system 1. Preparing food for absorption 2. Process of altering the chemical and physical components of food so that it can be absorbed and used by body cells Overview of the Digestive System B. Organization of the digestive system 1. Organs of Digestive system a. Segments of the Gastrointestinal track (GI) 1) 2) 3) Mouth Oropharynx Esophagus 4) 5) 6) 7) 8) Stomach Small Intestine Large Intestine Rectum Anal Canal Figure 23.2 Gastrointestinal tract activities. Ingestion Mechanical breakdown • Chewing (mouth) • Churning (stomach) • Segmentation (small intestine) Digestion Food Pharynx Esophagus Propulsion • Swallowing (oropharynx) • Peristalsis (esophagus, stomach, small intestine, large intestine) Stomach Absorption Lymph vessel Small intestine Large intestine Blood vessel Mainly H2O Feces Defecation © 2013 Pearson Education, Inc. Anus Overview of the Digestive System b. Accessory Organs 1) Salivary glands 2) Tongue 3) Teeth 4) Liver 5) Gallbladder 6) Pancreas 7) Vermiform appendix Overview of the Digestive System 2. Wall of the GI track a. The GI track is essentially a tube with walls fashioned of four layers of tissue. 1) Mucosa – inner most layer 2) Submucosa – thicker than muscosa 3) Muscularis – wraps around the submuscosa 4) Serosa – Outermost layer Figure 23.6 Basic structure of the alimentary canal. Intrinsic nerve plexuses • Myenteric nerve plexus • Submucosal nerve plexus Glands in submucosa Mucosa • Epithelium • Lamina propria • Muscularis mucosae Submucosa Muscularis externa • Longitudinal muscle • Circular muscle Mesentery Nerve Artery Gland in mucosa Vein Duct of gland outside Lymphatic vessel alimentary canal © 2013 Pearson Education, Inc. Serosa • Epithelium (mesothelium) • Connective tissue Lumen Mucosa-associated lymphoid tissue Overview of the Digestive System b. Modifications of layers 1) Variations in the epithelial layer 2) Upper esophagus have protection from abrasion 3) Small intestine has a muscosal layer which has microvilli to enhance absorption Mouth A. Structure of the Oral Cavity 1. Lips 2. Cheeks 3. Hard Palates – consists of portions of four bones 4. a. Two maxillae b. Two palatines Soft Palates Figure 23.7a Anatomy of the oral cavity (mouth). Soft palate Palatoglossal arch Uvula Hard palate Oral cavity Palatine tonsil Tongue Oropharynx Lingual tonsil Epiglottis Hyoid bone Laryngopharynx Esophagus Trachea © 2013 Pearson Education, Inc. Sagittal section of the oral cavity and pharynx Figure 23.7b Anatomy of the oral cavity (mouth). Upper lip Gingivae (gums) Palatine raphe Hard palate Soft palate Uvula Palatine tonsil Superior labial frenulum Palatoglossal arch Palatopharyngeal arch Posterior wall of oropharynx Tongue Sublingual fold with openings of sublingual ducts Lingual frenulum Opening of Submandibular duct Gingivae (gums) Oral vestibule Lower lip © 2013 Pearson Education, Inc. Anterior view Inferior labial frenulum Mouth 4. Tongue a. Skeletal muscle covered by a mucous membrane b. Mastication – chewing c. Deglutition – swallowing d. Papillae – Taste buds Figure 23.8 Dorsal surface of the tongue, and the tonsils. Epiglottis Palatopharyngeal arch Palatine tonsil Lingual tonsil Palatoglossal arch Terminal sulcus Foliate papillae Vallate papilla Medial sulcus of the tongue Dorsum of tongue Fungiform papilla Filiform papilla © 2013 Pearson Education, Inc. Mouth B. Salivary glands 1. Three pairs of compound tubuloveolar glands secrete a major amount – about 1 liter of saliva each day Figure 23.9a The salivary glands. Tongue Parotid gland Teeth Ducts of sublingual gland Parotid duct Masseter muscle Frenulum of tongue Body of mandible (cut) Sublingual gland Posterior belly of digastric muscle Mylohyoid muscle (cut) Submandibular duct Anterior belly of digastric muscle Submandibular gland © 2013 Pearson Education, Inc. Mouth C. Teeth 1. Typical tooth a. Crown – exposed portion of a tooth and is covered by enamel Figure 23.11 Longitudinal section of a canine tooth within its bony socket (alveolus). Enamel Dentin Crown Neck Dentinal tubules Pulp cavity (contains blood vessels and nerves) Gingival sulcus Gingiva (gum) Cement Root Root canal Periodontal ligament Apical foramen © 2013 Pearson Education, Inc. Bone b. The outer shell of the tooth is also covered by dental tissues (greatest proportion of the tooth shell c. Pulp cavity consists of connective tissue, blood, and lymphatic vessels and sensory nerves Figure 23.10 Human dentition. Incisors Central (6–8 mo) Lateral (8–10 mo) Canine (eyetooth) (16–20 mo) Molars First molar (10–15 mo) Second molar (about 2 yr) Deciduous (milk) teeth Incisors Central (7 yr) Lateral (8 yr) Canine (eyetooth) (11 yr) Premolars (bicuspids) First premolar (11 yr) Second premolar (12–13 yr) Molars First molar (6–7 yr) Second molar (12–13 yr) Third molar tooth) Inc. © 2013(wisdom Pearson Education, (17–25 yr) Permanent teeth 2. Types of teeth a. Twenty deciduous teeth – baby teeth (does not include premolars i. Incisors ii. Canine (eyetooth) iii. Molars b. Thirty-two permanent teeth i. Incisors – cutting ii. Canine – tear and pierce iii. Premolars (Bicuspids) iv. Molars – grinding and crushing Pharynx A. Bolus – mass of food B. Deglutition (swallowing) moves food (bolus) from the mouth to the stomach C. Used for digestion and respiration Figure 23.13 Deglutition (swallowing). (1 of 5) Bolus of food Tongue Pharynx Epiglottis Glottis Trachea 1 During the buccal phase, the upper esophageal sphincter is contracted. The tongue presses against the hard © 2013 Pearson Education, Inc. palate, forcing the food bolus into the oropharynx. Figure 23.13 Deglutition (swallowing). (2 of 5) Uvula Bolus Epiglottis Esophagus 2 The pharyngeal-esophageal phase begins as the uvula and larynx rise to prevent food from entering respiratory passageways. The tongue blocks off the mouth. The upper esophageal sphincter relaxes, allowing food © 2013 Pearson Education, Inc. to enter the esophagus. Figure 23.13 Deglutition (swallowing). (3 of 5) Upper esophageal sphincter Bolus 3 The constrictor muscles of the pharynx contract, forcing food into the esophagus inferiorly. The upper esophageal © 2013 Pearson Education, Inc. sphincter contracts (closes) after food enters. Figure 23.13 Deglutition (swallowing). Bolus of food Tongue Uvula Pharynx Bolus Epiglottis Epiglottis Glottis Trachea Esophagus 1 During the buccal phase, the upper esophageal sphincter is contracted. The tongue presses against the hard palate, forcing the food bolus into the oropharynx. 2 The pharyngeal-esophageal phase begins as the uvula and larynx rise to prevent food from entering respiratory passageways. The tongue blocks off the mouth. The upper esophageal sphincter relaxes, allowing food to enter the esophagus. 4 Peristalsis moves food through the esophagus to the stomach. Relaxed muscles Circular muscles contract Upper esophageal sphincter 3 The constrictor muscles of the pharynx contract, forcing food into the esophagus inferiorly. The upper esophageal sphincter contracts (closes) after food enters. Relaxed muscles 5 The gastroesophageal sphincter surrounding the cardial oriface opens, and food enters the stomach. Bolus of food Longitudinal muscles contract Circular muscles contract Gastroesophageal sphincter closed Gastroesophageal sphincter opens Stomach © 2013 Pearson Education, Inc. Bolus Esophagus A. Collapsible, muscular, mucus – lined tube 1. About 25 cm (10 inches) long 2. Extends from the pharynx to the stomach 3. Passage way for food, pushing the food toward the stomach Esophagus B. First segment of the digestive tube 1. Upper esophageal sphincter – helps prevent air from entering during respiration 2. Lower esophageal sphincter – also called cardiac sphincter junction between esophagus and stomach Figure 23.13 Deglutition (swallowing). (4 of 5) 4 Peristalsis moves Relaxed muscles food through the esophagus to the stomach. Circular muscles contract Bolus of food Longitudinal muscles contract Gastroesophageal sphincter closed Stomach © 2013 Pearson Education, Inc. Esophagus C. Gastroesophageal reflux disease (GERD) 1. Backward flow of stomach acid up through the cardiac sphincter 2. Treated by elimination of excess stomach acid or by surgery to strengthen the LES (cardiac sphincter) Figure 23.13 Deglutition (swallowing). (5 of 5) Relaxed muscles 5 The gastroesophageal sphincter surrounding the cardial oriface opens, and food enters the stomach. Circular muscles contract Gastroesophageal sphincter opens © 2013 Pearson Education, Inc. Stomach A. Size and Position of the stomach 1. 2. The stomach lies in the upper part of the abdominal cavity under the liver and diaphragm After meals the stomach is enlarged Stomach B. Divisions of the stomach 1. Fundus – above the opening of the esophagus 2. Body- Central part 3. Pylorus – lower portion Stomach C. Sphincter muscles 1. Guard both stomach openings 2. Muscle consisting of circular fibers 3. Cardiac sphincter controls the opening of the esophagus into the stomach 4. Pyloric sphincter controls the opening from the pyloric portion of the stomach into the first part of the small intestine Figure 23.19 Peristaltic waves in the stomach. Pyloric valve closed Pyloric valve closed 1 Propulsion: Peristaltic waves move from the fundus toward the pylorus. 2 Grinding: The most vigorous peristalsis and mixing action occur close to the pylorus. © 2013 Pearson Education, Inc. Pyloric valve slightly opened 3 Retropulsion: The pyloric end of the stomach acts as a pump that delivers small amounts of chyme into the duodenum, simultaneously forcing most of its contained material backward into the stomach. Stomach D. Gastric Muscosa 1. Chief cells – secrete enzymes of gastric juice 2. Parietal cells – secrete hydrochloric acid 3. Endocrine cells – secrete ghrelin – a hormone that stimulates the hypothalamus to increase appetite and gastrin which influences digestive functions Figure 23.14 Anatomy of the stomach. Cardia Fundus Esophagus Muscularis externa • Longitudinal layer • Circular layer • Oblique layer Serosa Body Lumen Lesser curvature Rugae of mucosa Greater curvature Duodenum Pyloric sphincter (valve) at pylorus Liver (cut) Pyloric canal Pyloric antrum Fundus Body Spleen Lesser curvature Greater curvature © 2013 Pearson Education, Inc. Figure 23.15a Microscopic anatomy of the stomach. Surface epithelium Mucosa Lamina propria Muscularis mucosae Submucosa (contains submucosal Oblique plexus) layer Muscularis Circular externa layer (contains Longitudinal myenteric layer plexus) Stomach wall Serosa © 2013 Pearson Education, Inc. Layers of the stomach wall Figure 23.15b Microscopic anatomy of the stomach. Gastric pits Surface epithelium (mucous cells) Gastric pit Mucous neck cells Parietal cell Gastric gland Chief cell Enteroendocrine cell Enlarged view of gastric pits and gastric glands © 2013 Pearson Education, Inc. Figure 23.15c Microscopic anatomy of the stomach. Pepsinogen Pepsin HCI Mitochondria Parietal cell Chief cell Enteroendocrine cell Location of the HCl-producing parietal cells and pepsin-secreting chief cells in a gastric gland © 2013 Pearson Education, Inc. Stomach E. Gastric Muscle 1. Crisscrossing pattern of smooth muscle fibers 2. Stomach wall has the ability to contract strongly at many angles which causes mixing action of this organ. Stomach F. Functions of the stomach 1. Stores food 2. Secretes gastric juice 3. Churns the food, breaking it down into small particles 4. Secretes intrinsic factor 5. Limited amount of absorption – certain drugs, some water and alcohol and some short – chain fatty acids Stomach 6. Destroys pathogenic bacteria 7. Produces the hormone gastrin 8. Regulates the hormone ghrelin which increases appetite Small intestine A. Introduction 1. Small intestine is a tube measuring about 2.5 (1 inch) in diameter and 6 m (20 feet) in length. 2. Coiled and looped Figure 23.28 Mechanisms promoting secretion and release of bile and pancreatic juice. 1 Chyme enter -ing duodenum causes duodenal enteroendocrine cells to release cholecystokinin (CCK) and secretin. 2 CCK (red dots) and secretin (yellow dots) enter the bloodstream. 3 CCK induces secretion of enzyme-rich pancreatic juice. Secretin causes secretion of HCO3− -rich pancreatic juice. 4 Bile salts and, to a lesser extent, secretin transported via bloodstream stimulate Liver to produce bile more rapidly. 5 CCK (via blood stream) causes gallbladder to contract and Hepatopancreatic Sphincter to relax. Bile Enters duodenum. 6 During cephalic and gastric phases, vagal Nerve stimulates gallbladder to contract weakly. CCK secretion Secretin secretion © 2013 Pearson Education, Inc. Small intestine B. Divisions of the small intestine 1. Duodenum a. Uppermost division b. Part to which the pyloric end of the stomach attaches c. About 25 cm (10 inches) long d. Shaped like a C Small intestine 2. Jejunum – 2.5 m (8 feet) long 3. Ileum – 3.5 m ( 12 feet) long Small intestine C. Wall of the small intestine 1. Intestinal ling has circular folds that have many tiny projection call villi 2. Epithelial cells on the surface of villi can be seen by microscopy to have a surface resembling a fine brush is formed by microvilli Figure 23.22b Structural modifications of the small intestine that increase its surface area for digestion and absorption. Microvilli (brush border) Absorptive cells Lacteal Goblet cell Blood capillaries Mucosaassociated lymphoid tissue Intestinal crypt Muscularis mucosae Duodenal gland © 2013 Pearson Education, Inc. Villus Enteroendocrine cells Venule Lymphatic vessel Submucosa Figure 23.22c Structural modifications of the small intestine that increase its surface area for digestion and absorption. Absorptive cells Goblet cells Villi © 2013 Pearson Education, Inc. Intestinal crypt Figure 23.23 Microvilli of the small intestine. Mucus granules Microvilli forming the brush border Absorptive cell © 2013 Pearson Education, Inc. D. Function – Complete Digestion and food and nutrient absorption Large Intestine A. Size of the Large Intestine 1. Diameter is larger than that of the small intestine 2. Length is 1.5 to 1.8 m (5-6 feet) Figure 23.29a Gross anatomy of the large intestine. Left colic (splenic) flexure Right colic (hepatic) flexure Transverse mesocolon Transverse colon Epiploic appendages Superior mesenteric artery Descending colon Haustrum Ascending colon IIeum Cut edge of mesentery IIeocecal valve Tenia coli Sigmoid colon Cecum Appendix Rectum Anal canal © 2013 Pearson Education, Inc. External anal sphincter Large Intestine B. Divisions of the large intestine 1. Cecum 2. Colon a. Ascending colon – lies in a vertical position, on the right side of the abdomen b. Transverse colon – passes horizontally across the abdomen, below the liver, stomach and spleen Large Intestine c. Descending colon – lies in the vertical position on the left side of the abdomen d. Sigmoid colon – that courses downward below the iliac crest (joins the rectum) Large Intestine 3. Rectum a. Last part of the intestinal tube b. Anal canal c. Mucous lining is arranged in numerous vertical folds known as anal columns 1) Each which contains an artery and a vein 2) Hemorrhoids are enlargements of the veins in the anal canal Figure 23.29b Gross anatomy of the large intestine. Rectal valve Rectum Hemorrhoidal veins Levator ani muscle Anal canal External anal sphincter Internal anal sphincter Anal columns Pectinate line Anal sinuses Anus © 2013 Pearson Education, Inc. C. Function of large intestine 1. Absorption of water Figure 23.2 Gastrointestinal tract activities. Ingestion Mechanical breakdown • Chewing (mouth) • Churning (stomach) • Segmentation (small intestine) Digestion Food Pharynx Esophagus Propulsion • Swallowing (oropharynx) • Peristalsis (esophagus, stomach, small intestine, large intestine) Stomach Absorption Lymph vessel Small intestine Large intestine Blood vessel Mainly H2O Feces Defecation © 2013 Pearson Education, Inc. Anus Vermiform Appendix A. Wormlike tubular organ B. Average 8 to 10 cm (3 to 4 inches) in length C. Its function 1. It contains masses of lymphoid tissue 2. Plays an important role in the body immunity. It also stores bacteria upon the need during digestion Figure 23.30a Mesenteries of the abdominal digestive organs. Falciform ligament Liver Gallbladder Spleen Stomach Ligamentum teres Greater omentum Small intestine Cecum © 2013 Pearson Education, Inc. Figure 23.30b Mesenteries of the abdominal digestive organs. Liver Gallbladder Lesser omentum Stomach Duodenum Transverse colon Small intestine Cecum Urinary bladder © 2013 Pearson Education, Inc. Figure 23.30c Mesenteries of the abdominal digestive organs. Greater omentum Transverse colon Transverse mesocolon Descending colon Jejunum Mesentery Sigmoid mesocolon Sigmoid colon Ileum © 2013 Pearson Education, Inc. Figure 23.30 Mesenteries of the abdominal digestive organs. Falciform ligament Liver Gallbladder Lesser omentum Spleen Stomach Duodenum Ligamentum teres Transverse colon Greater omentum Small intestine Cecum Urinary bladder Liver Lesser omentum Greater omentum Transverse colon Transverse mesocolon Pancreas Stomach Duodenum Transverse mesocolon Transverse colon Mesentery Descending colon Jejunum Mesentery Sigmoid mesocolon Sigmoid colon Greater omentum Jejunum Ileum Ileum Urinary bladder Rectum © 2013 Pearson Education, Inc. Visceral peritoneum Parietal peritoneum Peritoneum A. Membrane covering and holding in pace most of the organs of the digestive system B. Mesentery hold organs together (fan shape) Liver A. Location and Size of the Liver 1. Liver is the largest gland in the body 2. Lies under the diaphragm Figure 23.21 The duodenum of the small intestine, and related organs. Right and left hepatic ducts of liver Cystic duct Common hepatic duct Bile duct and sphincter Accessory pancreatic duct Mucosa with folds Tail of pancreas Pancreas Jejunum Gallbladder Major duodenal papilla Hepatopancreatic © 2013 Pearson Education, Inc. Duodenum ampulla and sphincter Main pancreatic duct and sphincter Head of pancreas Figure 23.24 Gross anatomy of the human liver. Sternum Nipple Liver Bare area Falciform ligament Left lobe of liver Right lobe of liver Gallbladder Lesser omentum (in fissure) Left lobe of liver Porta hepatis containing hepatic artery (left) and hepatic portal vein (right) Quadrate lobe of liver Ligamentum teres © 2013 Pearson Education, Inc. Round ligament (ligamentum teres) Bare area Caudate lobe of liver Sulcus for inferior vena cava Hepatic vein (cut) Bile duct (cut) Right lobe of liver Gallbladder Liver B. Liver lobes and lobules 1. Left lobe 2. Right lobe 3. Caudate lobe 4. Quadrate lobe 5. Hepatic lobules – made of hepatic cells Liver C. Bile ducts 1. Small bile ducts within the liver join the form two larger ducts that emerge from the under surface of the organ as the right and left hepatic duct 2. Hepatic duct merges with the cystic duct from the gallbladder to from the common bile duct Liver D. Functions of the Liver 1. Detoxify various substances 2. Secrete about a pint of bile a day 3. Important in the metabolism of proteins, fats (bile salts are important in the absorption of fats) and carbohydrates Liver 4. Produces important plasma proteins and serves as a site of blood cell production during fetal development 5. Storage of iron and vitamins Gallbladder 6. Gallbladder a. Size and Location of the gallbladder i. Pear shaped sac ii. 7 to 10 cm (3-4 inches)long iii. Can hold 30 to 50 ml of bile iv. Lies under the surface of the liver Gallbladder b. Structure of the gallbladder 1. Serous muscular and mucous layer 2. similar to the stomach wall 3. Surgical removal of the gallbladder is called cholesystectomy Gallbladder C. Functions of the gallbladder 1. Stores bile (fivefold to tenfold concentrations) 2. During digestion the gallbladder contracts ejecting the bile into the duodenum of the small intestine Pancreas A. Size and Location of the Pancreas 1. Grayish pink colored gland about 12 -15 cm (6-9 inches) 2. It resembles a fish with its head and neck in the C – shaped curved of the duodenum 3. Extends horizontally behind the stomach and its tail touching the spleen Pancreas B. Structure of the pancreas 1. Composed of two different types of glandular tissue one exocrine and endocrine 2. Has a pancreatic duct which empties into the duodenum at the same point of the common bile duct 3. Contains alpha cells and beta cells Pancreas C. Functions of the pancreas 1. Pancreas secrete the digestive enzymes found in pancreatic juice – important part in digestion 2. Beta cells of the pancreas secrete insulin (hormone that exerts a major control over Carbohydrate metabolism) 3. Alpha cells secret glucagons – which has a direct opposite effect on carbohydrate metabolism Figure 23.27 Activation of pancreatic proteases in the small intestine. Stomach Pancreas Epithelial cells Membrane-bound enteropeptidase Trypsinogen (inactive) © 2013 Pearson Education, Inc. Trypsin Chymotrypsinogen (inactive) Chymotrypsin Procarboxypeptidase (inactive) Carboxypeptidase Disorders of the Digestive System A. Heartburn 1. Backflow of stomach acid up into the esophagus 2. Heartburn is often caused by acid reflux which might be aggravated by a. Smoking b. Obesity c. Spicy foods Disorders of the Digestive System B. Ulcers 1. Is a craterlike wound or sore in a membrane caused by tissue destruction 2. These sores cause gnawing or burning pain and may ultimately result in hemorrhage 3. Gastroesophageal Reflux Disease (GERD) Figure 23.16a Photographs of a gastric ulcer and the H. pylori bacteria that most commonly cause it. A gastric ulcer lesion © 2013 Pearson Education, Inc. Figure 23.16b Photographs of a gastric ulcer and the H. pylori bacteria that most commonly cause it. Bacteria Mucosa layer of stomach H. pylori bacteria © 2013 Pearson Education, Inc. Disorders of the Digestive System C. Mumps 1. An acute viral disease characterized by swelling of parotid salivary glands 2. Can occur in children and adults (more of a severe infection in adults) Disorders of the Digestive System D. Tooth Decay 1. Common disease 2. Disease of the enamel, dentin, and cementum of teeth 3. Results in the formation of cavity Disorders of the Digestive System E. Appendicitis 1. Caused by the mucous lining of the appendix becoming inflamed. 2. If the appendix ruptures, it will release infectious material into the abdominal cavity can cause death. Normal appendix compared to abnormal appendix https://www.youtube.com/watch?v=lnVjXuyM6xk&list =PLBMkFNFXhVis9AUGNrFJWgSJHAjonB8cK&index=5 https://www.youtube.com/watch?v=9bnIuKiHdDE&in dex=4&list=PLBMkFNFXhVis9AUGNrFJWgSJHAjonB8cK https://www.youtube.com/watch?v=eKLqFnAmK6c&li st=PLBMkFNFXhVis9AUGNrFJWgSJHAjonB8cK&index=11 II. Digestion Physiology A. Digestive Enzymes 1. Enzymes are proteins which is made up of amino acids 2. Can denature (not work properly) 3. Function at a specific pH and temperature a. Amylase 1) Found in saliva 2) Optimal pH of neutral or slightly acidic b. Pepsin 1) Found in gastric juice (stomach) 2) The optimal pH is 2 (very acidic) 3) Pepsin must have HCl acid to function Chapter 26 B. Nutrients 1. Carbohydrates a. Sugars with C6H12O6 groups b. Examples 1) Polysaccharides include starches (from plants) and glycogen (from animals) 2) Disaccharides include sucrose lactose and maltose 3) Monoscaccharides (smallest carbohydrate molecule) glucose, galactose and fructose c. Enzymes affecting carbohydrate digestion 1)Surcease 2)Lactase 3)maltase Chapter 26 B. Nutrients 2. Proteins a. Are large chains of amino acids b. Enzymes affecting protein digestion 1) Proteases 2) Pepsin 3. Lipids a. Includes phospholipids and fats b. Enzymes affecting fats Lipase Chapter 26 C. Function of the organs 1. Mouth a. Saliva contains amylase b. Beginning digestion of carbohydrates 2. Stomach a. Gastric juice contains the enzyme Protease (pepsin) b. Beginning digestion of proteins Chapter 26 C. Function of the organs 3. Small Intestine 1. Pancreas a. Releases enzymes into the small intestine that breaks down proteins Produces both enzymes, trypsin and chymotrypsin produces protease b. Releases enzymes into the small intestine that breaks down carbohydrates - amylase c. Releases enzymes into the small intestine that breaks down fats - Lipase Chapter 26 C. Function of the organs 2. 3. Enzymes produced by the small intestine a. Peptidase – breaks down proteins into amino acids b. Surcease – breaks down sucrose into glucose and fructose c. Lactase – breaks down lactose (milk sugar) into glucose and galactose d. Maltase – (Malt sugar) – breaks down into glucose molecules Bile produced by the liver is released into the small intestine and completely breaks down fat Chapter 26 C. Function of the organs 4. Large Intestine 1. Absorption of water 2. Stores waste material