* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Erin Hardie
Neuropsychology wikipedia , lookup
Embodied cognitive science wikipedia , lookup
Cognitive neuroscience wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Visual selective attention in dementia wikipedia , lookup
Microneurography wikipedia , lookup
Stereopsis recovery wikipedia , lookup
Neuroregeneration wikipedia , lookup
Neuroesthetics wikipedia , lookup
C1 and P1 (neuroscience) wikipedia , lookup
Visual extinction wikipedia , lookup
Split-brain wikipedia , lookup
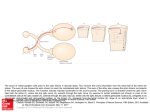
Undetected agenesis of the corpus callosum with associated hydrocephalus: a rare cause of bilateral optic atrophy and a homonymous hemianopsia Erin Hardie, O.D. VisionAmerica of Birmingham Ocular Disease Residency Abstract Commonly, homonymous visual field defects and optic atrophy are found in vascular or compressive lesions; however, this case presents a rare visual manifestation of a patient with undetected agenesis of the corpus callosum and associated hydrocephalus. Patient Demographics A 31 year-old black female is referred to our clinic for a glaucoma evaluation secondary to enlarged optic nerve head cupping. She had no visual complaints and had not noticed any peripheral vision loss. Her ocular history included esotropia as a child with three prior strabismus surgeries between the ages five to eight years old. She currently wears a glasses correction of 0.50-4.00 X 177 OD and -1.25-4.00 X 010 OS. Her medical history was insignificant with the exception of being 36 weeks pregnant and taking a prenatal vitamin daily. Pertinent Findings Visual acuities with her current correction measured 20/40 in the right eye, pinhole no improvement, and 20/25 in the left eye, pinhole 20/20. Upon confrontation fields, she exhibited loss of the right side of both fields with the inferior nasal quadrant missing in the left eye and the entire temporal field missing in the right eye. Pupils were equal, round and reactive to light without an afferent papillary defect in both eyes. Cover test showed a small angle residual right esotropia with a slight hypotropia with a combined latent nystagmus. Intraocular pressures were 15mm in the right and 14mm Hg in the left at 9:00am by Tonopen applanation. Pachymetry readings were 535um for the right and 530um for the left cornea. All anterior segment findings were normal with only slight meibomian gland dysfunction in both eyes. Upon dilation with punctual occlusion, her optic nerves showed symmetrical cupping of 0.6 with a more marked optic nerve pallor in both eyes. Other than slight venous dilation in both eyes the retinal periphery and macula were normal. (OCT and optic nerve head photos available for presentation/poster). Humphrey 24-2 threshold visual field testing in both eyes exhibited a right homonymous hemianopsia respecting the vertical midline characteristic of a left optic tract lesion. (VF also available for presentation) Optical coherence testing was less reliable because of her latent nystagmus, but showed a generalized loss of the retinal nerve fiber layer in both eyes. An MRI of the brain and orbits without contrast (also available), showed “compensated” hydrocephalus with a marked absence of the posterior corpus callosum and no mass present. Differential Diagnoses Differential diagnoses include conditions that can cause optic atrophy and a homonymous visual field. As for optic atrophy, numerous different entities can cause bilateral optic atrophy such as hereditary, metabolic, post-inflammatory, traumatic, demyelinating, and consecutive etiologies. Optic atrophy is characterized by pallor of the optic nerve without accompanying optic nerve cupping. This atrophy is a consequence of the death of the ganglion cell layer axons which comprise the optic nerve. Optic pallor is commonly misdiagnosed as Glaucoma, as was the case with our patient. It can present unilaterally or bilaterally and can include an APD if the underlying disease is asymmetric; decreased acuity, dyschromatopsia, and visual field defects are also frequently found. To review the pathophysiology, there are 1.2 million optic nerve fibers that run through the optic nerve from the axons of the inner retina (1). There are two ways to acquire axonal cell damage. Anterograde degeneration starts with damage in the retina and progresses towards the brain, whereas, retrograde degeneration originates in the brain and goes towards the optic nerve. Because this patient had a homonymous hemianopsia accompanying her optic atrophy, the main differential diagnoses included primarily retrograde etiologies. Our top differential for this patient was primary bilateral optic atrophy developing from a type of compressive lesion or vascular insult to the posterior cortex. When a space occupying lesion develops in the brain or orbits, it presses on the neural tissue causing mechanical damage to its contents (2). There are many types of lesions that can cause similar ocular presentations to our patient such as optic nerve gliomas, pituitary adenomas, aneurysms, and a variety of brain tumors. Typically, these conditions manifest with dyschromatopsia, acute or chronic vision loss, optic nerve pallor, and a wide range of visual field defects; however most field defects respect the vertical midline if located more posteriorly in the occipital lobe. If no lesion is found on MRI causing primary optic atrophy, there are multiple causes of bilateral secondary optic atrophy which could have caused this patient’s presentation. Chronic papilledema is characterized by bilateral swelling of the optic nerves secondary to an increase in intracranial pressure. Until proven otherwise, bilateral papilledema is presumed to be secondary to an intracranial tumor unless a negative MRI and lumbar puncture point to idiopathic intracranial hypertension (4). In papilledema once the disc edema resolves, the optic nerves are left pallorous with edges that appear rough and poorly defined (2). Clinically, the patient will present with headaches, a slight decrease in acuity, paracentral field defects, and dyschromatopisa. Resolved anterior ischemic optic neuropathy also causes secondary optic atrophy and pallor but it is uncommonly a bilateral occurrence. Two types exist, non-arteritic and arteritic, the latter can manifest in both eyes but is rarely found in patients under the age of 55 years old. Most often patients present with an APD, an acute vision decline in the affected eye, and the nerve is swollen typically with hyperemia. The main cause of this inflammation is hypoperfusion of blood flow to the optic nerve either from systemic disease like hypertension or arteritis of medium-sized blood vessels in the eye (5). Other less common causes of secondary optic atrophy include were considered are toxic and nutritional optic neuropathy. Tobacco and alcohol are the two substances that often lead to visual deficits as many smokers and alcoholics exhibit inefficient Vitamin B12 intakes. Clinical characteristics include a slow decline in vision, dyschromatopsia, and uniquely temporal pallor of the optic nerve head (2). A final differential is glaucomatous optic neuropathy which is certainly capable of being misdiagnosed for optic atrophy; our case included. An important clinical finding is marked cupping of the optic nerve head with bayonetting of the vessels at the disc and possible drance hemorrhages. The visual field often reveals arcuate defects that point to the optic nerve, often with a nasal step. If asymmetric, an APD can be present but normally it is a slow process manifesting in older patients. Still, since the prevalence of glaucoma is much higher than optic atrophy, many practitioners fail to accurately differentiate the two. Diagnosis and Discussion After reviewing the MRI scan, the optic atrophy, homonymous visual field defect, and other ocular findings were attributed to her newly discovered neurological maldevelopment and the patient was educated on the findings. Her clinical presentation was considered a combination of both hydrocephalus and a absence of the posterior corpus callosum. Below is a review of the pathogenesis, clinical presentation, and management of hydrocephalus and agenesis of the corpus callosum, along with a current literature review of the documented visual symptoms and signs found in these two entities. Hydrocephalus is a distention of the ventricles in the brain by accumulated cerebral spinal fluid (CSF). Often, there is stenosis of the aqueduct of Sylvius that limits the flow of CSF which is called non-communicating hydrocephalus (6). Still, there is also a communicating type where CSF can freely flow between the ventricles, but is either over produced or not adequately drained from the cranium. Shunts are often employed to help divert the flow of CSF and facilitate drainage. The prognosis varies greatly and often depends upon the classification, etiology, and time of diagnosis of the condition; however, it is possible to be neurologically normal and approximately 29% can academically be considered average (7). This explains how our patient lived 31 years without a diagnosis. However, most patients have the congenital form and are discovered at birth with approximately 1 in 500 children having this diagnosis (6). These infants exhibit an increase in head circumference, possible seizures, and papilledema. There is also acquired hydrocephalus which begins later on in life and is often less severe. Our patient exhibited chronic compensated hydrocephalus and since she had no previous documentation of this disorder, it is nearly impossible to determine if it was congenital or acquired; more than likely it was present at birth. She had enlargement of both the third and fourth ventricles, which certainly contributed to or developed alongside her the absence of her posterior corpus callosum. The corpus callosum is a large band of nerve axons that not only separates the two hemispheres but also plays an important role in connecting the right and left side of the brain. It is the main white matter bundle in the brain (8). When a portion of this important structure does not form properly, it is termed agenesis of the corpus callosum. This maldevelopment can be complete or partial and results from multiple causes such as genetic, infectious, toxic, or vascular entities. Agenesis of the corpus callosum occurs in approximately 1 in 4000 births (10). The patient can often manifest “split brain” type symptoms, and show multiple developmental delays in infancy. Yet, the prognosis can be positive for patients with agenesis of the corpus callosum and if the condition is isolated, as many as 75% of patients can have normal intelligence levels (3). In our patient, she also developed hydrocephalus, and yet her intelligence level was clinically average without formal IQ testing. Both hydrocephalus and agenesis of the corpus callosum can manifest many ocular symptoms as demonstrated in this patient. To begin with hydrocephalus, in recent surveys, scientists have concluded that cognitive visual problems often present with this condition. Nearly, 61% of patients with hydrocephalus exhibited a strabismus, most of which were esotropic. In 39% some form of nystagmus was present, but most were in primary gaze; latent nystagmus was rarely documented (12). Our patient exhibited both of these findings. Most importantly, a visual field defect was present in only 16% and, of those defects, the most common were homonymous hemianopsias. The clinical finding of optic atrophy was found in 31% and correlated with the visual acuity of the patient (12). As discussed previously, the pathophysiology of this atrophy is retrograde in nature. This loss of nerve function resulted in her decrease in acuity, lack of color vision, and pallor of her optic disc. To complicate matters further, in addition to hydrocephalus, the posterior callosum has also been demonstrated to play a large role in visuomotor integration. According to one source the callosum, “helps to create a unified experience of the way we perceive the world” (9). Because the corpus callosum is necessary for the hemispheres of the brain to communicate, an inability to do so likely results in poor stereopsis and even hemispheric neglect. When studied, many people who have normal intelligence with agenesis of the corpus callosum have documented degradation in transfers between opposite hemispheres (11). Clearly, the missing portion of the corpus callosum might also play a role in her homonymous hemianopsia and her lack of stereopsis. It is widely known that more posterior defects cause congruous visual deficits that respect the midline of the field (13). Since hydrocephalus and agenesis of the corpus callosum both affect the posterior cortex, the cause of her homonymous visual field defect was attributed to each condition; still, research points more to her hydrocephalus. Her optic atrophy was secondary to loss of nerve axons and determined not to be glaucoma. The other ancillary findings were more likely caused from her hydrocephalus. Treatment and Management Since she showed compensated hydrocephalus, there was no need for immediate referral to neurology for shunt implantation; she simply needed to be monitored closely by her primary care physician for changes or worsening symptoms. Still, she was nearly 36 weeks pregnant, and so her obstetrician needed to be notified of our findings as well. Also, as in the genetic causes previously discussed, the baby had a small risk of developing similar neurological findings and need to be monitored (10). Records were obtained from the referring doctor which showed a longstanding decrease in vision of 20/50 OD and 20/30 OS. Importantly, she manifested extreme color blindness, missing all but one plate in both eyes on Isihara. She also consistently showed an esotropia with no ability to detect stereopsis, latent nystagmus, and a right homonymous hemianopsia on FDT testing. While an appointment was scheduled to follow-up with another Humphrey 24-2 visual field, the patient ended up delivering her baby early, and had to cancel her appointment. For now, her condition is stable and her ocular findings longstanding. Clearly, there is nothing that can be done to reverse her visual loss and treatment will be targeted at preserving her current visual status. Once available, we plan on following her visual field closely to monitor for progression along with other ocular signs of worsening hydrocephalus such as papilledema. Also, it would be interesting to do more sensory testing for possible visual agnosia, constructional apraxia, and central extinction phenomenon. This would help to determine if the patient has a clinical entity called callosal disconnection syndrome which commonly manifests in individuals missing all or part of the corpus callosum (14). A K-Bit intelligence test would also be interesting but not necessarily warranted. Conclusion While the list of differentials for optic atrophy and a homonymous hemianopsia is extensive, MRI imaging is one the physician’s most useful tools. In this case, it revealed a unique and undetected condition in a healthy, pregnant female. This case is evidence that many neurological conditions often cause ocular findings and therefore, as primary eye care physicians, we must be competent when ordering and diagnosing all such disorders. It is crucial that we play an active role the care of our patients and facilitate communication between multiple practitioners. References: 1. Sadun, A.A., Neuroophthalmology 6. “Neuroanatomy of the human visual system: Part I. Retinal projections to the LGN and pretectum as demonstrated with a new stain”. 1986. 353–361. 2. Van Stavern, G P . Ophthalmology clinics of North America. "Optic neuropathies. An overview". (03/2001)(0896-1549), 14 (1), p. 61. 3. Moutard ML, Kieffer V. Prenat Diagn. Isolated corpus callosum agenesis: a ten-year follow-up after prenatal diagnosis (how are the children without corpus callosum at 10 years of age?). 2012. 32:277-83. 4. Becker, M. European journal of radiology. "Imaging of the optic nerve". 05/2010. 74 (2), p. 299. 5. Lincoff, NS. Neuro-ophthalmology: The Practical Guide. “Arteritic anterior ischemic optic neuropathy.” Thieme Medical Publishers Inc. New York, NY. 2005: 187-93. 6. NINDS. NIH Publication. "Hydrocephalus Fact Sheet”. Publication date February 2008. No. 08-385. 7. Renier, D. Child's nervous system. "Prenatal hydrocephalus: outcome and prognosis". 08/1988. 0256-7040. 4 (4), p. 213. 8. The Journal of Neuroscience. JNEUROSCI. 13 February 2008, 28(7): 1535-1536. 9. Schulte, Tilman. Neuropsychology Review. "Contribution of callosal connections to the interhemispheric integration of visuomotor and cognitive processes". 2010. 1040-7308, 20 (2), p. 174. 10. Lynn K. Paul, Warren S. Brown, Ralph Adolphs, J. Neuroscience. “Agenesis of the corpus callosum: genetic, developmental and functional aspects of connectivity”. Volume 8, April 2007, 287-299. 11. Fischer M, Ryan SB, Dobyns WB. Arch of Neurology. “Mechanisms of interhemispheric transfer and patterns of cognitive function in acallosal patients of normal intelligence”. 1992. 49(3):271-7. 12. Houliston, M, Abdel H. Taguri. Developmental Medicine & Neurology. “Evidence of cognitive visual problems in children with hydrocephalus: a structured clinical history-taking strategy”. 1999. 41: 298-306. 13. Yanoff, M; Duker, J. Ophthalmology. “Neuro-Ophthalmology”. Elsevier Inc. 2009. 992-998. 14. Browndyke, J.N.. Neuropsychology Central. “Callosal Disconnection Syndrome”. 2002. 1-3.