* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Affective and Personality Disorders
Depersonalization disorder wikipedia , lookup
History of psychosurgery in the United Kingdom wikipedia , lookup
Asperger syndrome wikipedia , lookup
Major depressive disorder wikipedia , lookup
Mental disorder wikipedia , lookup
Conduct disorder wikipedia , lookup
Moral treatment wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Conversion disorder wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Personality disorder wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Child psychopathology wikipedia , lookup
Spectrum disorder wikipedia , lookup
Schizoid personality disorder wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Bipolar disorder wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
History of psychiatry wikipedia , lookup
History of mental disorders wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Abnormal psychology wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
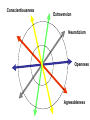
Mood and Personality Disorders Joe MacLellan PGY-3 July 28, 2011 Thank you • Dr. Colleen Carey • Colleen Weir Outline • Mood Disorders – Depressed mood – Elevated Mood • Personality Disorders – Cluster A, B, and C Mood Disorders MDE/MDD Dysthymia Bipolar disorder I Bipolar disorder II Cyclothymia Case 1 45 single F, presents to the ED c/o fatigue and abdominal pain. • Vitals Normal • Bloodwork is Normal • Abdominal exam is benign Next step? How do depressed patients present to the ED? 1) Suicidal Ideation 2) Depressed 3) Vague complaints 4) Anxiety Major Depressive Episode MDE Criteria • At least 5 of SIGECAPS* • Causes impairment, for >2 weeks • Not a mixed episode, not substanceinduced or caused by a GMC, not bereavement How do adolescents and elderly differ in their presentation? Adolescents Geriatrics – Cognitive changes (dementia) – Misdiagnosed as ADD – Boredom* – Substance use/criminal activity – Mood can be irritable Should we be prescribing anti-depressant medication in the ED? What disorders mimic Major Depression? Mimics • Medical Conditions • Medications • Substance Abuse/Withdrawal How does Dysthymia differ? Dysthymia • Chronic, low-grade depression • Responsive to anti-depressants • Increase risk of MDD Specifiers • Seasonal Affective • Postpartum • With other features: psychotic, atypical, melancholic Treatment Moderate-Severe: • Anti-depressants • Psychotherapy • ECT Mild: • Exercise, self-help books • Counseling Who needs to be admitted? Disposition • Who needs admission? – Risk of suicide/homicide – Lacks capacity to cooperate with treatment – Inadequate psychosocial support – Co-morbid condition requiring admission • Who can be discharged? Resources We will come back to this… All the kids are doing it… “I feel more alive. I feel more focused. I feel more energetic. My workouts are really intense.” “Every great movement begins with one man, and that’s me.” [Did you get out of control?] “Well yeah! I don’t have another gear!” How do manic patients typically present to the ED? Mania presents as • Dangerous activity • Trauma • Gambling • Binge Drinking Manic Episode • Elevated mood lasting 1 week • 3 or more of DIGFAST* • Not mixed, substance-induced, GMC • Causes impairment Mimics • Substance abuse/withdrawal • Medications • Delirium • Hyperthyroid How would you control an aggressive Manic patient • Initially: – Single room, offering medications • If necessary: – Haldol/lorazepam – restraints How does Hypomania differ? Hypomania • Elevated/irritable for 4+ days • 3 or more of DIGFAST • BUT… – Not signicant enough to cause marked impairment or to necessitate hospitalization Bipolar disorder • Bipolar I – Episode of mania, +/- MDE +/-, hypomania • Bipolar II – Hypomanic and MDE episodes – NO manic or mixed episodes Cyclothymia • 2 years of episodes of hypomania and depressive symptoms • Not meeting criteria for MDE, mania, or mixed episoder • Not substance-induced, GMC, schizophreniform Treatment • Acute depression: – SSRI’s • Acute mania: – Lithium – +/- antipsychotics, benzodiazepines • Maintenance: – lithium – Educational and psychosocial support Disposition • Who needs admission? • Who can be discharged? Resources We will come back to this… Personality Disorders “an enduring pattern of inner experience and behavior that deviates markedly from the expectations of the individual's culture, is pervasive and inflexible, has an onset in adolescence or early adulthood, is stable over time, and leads to distress or impairment” Is this a Personality Disorder? Is this? 2 people in this room have a PD • Cluster A = • Cluster B • Cluster C Conscientiousness Extraversion Neuroticism Openness Agreeableness Cluster A • Schizoid Personality Disorder • Schizotypal Personality Disorder • Paranoid Personality Disorder Cluster C • Dependant Personality Disorder • Avoidant Personality Disorder • Obsessive-compulsive Personality Disorder Personality Disorder Party Jason The Guest List Kim Skye Jason Amber Tyler Crystle Cheat Sheet • • • • • • Harold - Schizoid Kim - Paranoid Skye - Dependant Tyler - Schizotypal Amber - OCPD Crystle - Avoidant A • These patients rarely seek treatment. • Treatment largely psychotherapy • Use clear explanations, establish trust C • Typically present with another symptom* • Pharmacotherapy for symptom relief but mainstay is psychotherapy • Be supportive but set limits Cluster B Borderline PD How does Borderline PD present to the ED? BPD in the ED Biological 1. Sequelae of self-harm 2. Sequelae of reckless behaviour Psychological 1. “Depression” (mood instability) 2. Suicidal ideation 3. Intense anger, agitation in the community 4. Stress-related “psychosis” Social 1. Therapist is unavailable 2. Caregiver is unavailable 3. Housing crisis 4. Financial crisis (day before AISH cheque) 5. Seeking admission What is the approach to the Borderline patient in the ED? 1. Medical clearance – untold parasuicidal or suicidal gestures 2. Mental state clearance – look for new features to this presentation (is this “the same old same old”?) 3. Supportive interventions 1. Ask the patient what would be helpful 2. Nicorette, warm blanket, food 3. Recognize and reinforce healthy choices 4. Watch your own countertransference (helplessness; anger) 4. Take responsibility for the patient’s treatment, but not the patient’s behaviours. Tips for Working with BPD • Be truthful and keep it simple • Beware of splitting, communicate clearly with other staff • Elicit expectations from patient • Goal: have patient take ownership of solution Narcissistic PD • Be careful of overlap with manic grandiosity • Illness disrupts their selfimage • Appeal to their narcissism How does Antisocial PD present to the ED? ASPD in the ED • Facing charges and is now “suicidal” • Facing charges, now “acting bizarrely” • Assault • Intoxicated • Demanding abusable substances What is the approach to the Antisocial patient in the ED? 1. Medical clearance – untold parasuicidal or suicidal gestures 2. Mental state clearance – look for new features to this presentation (is this “the same old same old”?) 3. Supportive interventions 1. Ask the patient what would be helpful 2. Nicorette, warm blanket, food 3. Recognize and reinforce healthy choices 4. Watch your own countertransference (helplessness; anger) 4. Take responsibility for the patient’s treatment, but not the patient’s behaviours. Tips for working with ASPD • Be Objective • Provide a thorough, non-authoritarian approach to investigation • Set clear approach/plan with patient Histrionic PD • Vague/loosely connected sx. • Often under/over investigate • Sensitive to emotional concerns while avoiding closeness Cognitive Behavioural Therapy A psychotherapeutic treatment that helps patients understand the thoughts and feelings that influence behaviors Patients learn how to identify and change maladaptive thought patterns that have a negative influence on behaviour. Resources • Private (Fee): – Inner solutions – Bridging the gap – Calgary counseling Resources • Public Access: – Admission, short stay, day program – SCHC and SC • walk in counseling • Brief therapy – – – – – ERO DBT program Access Mental Health Crisis Line PAS