* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Postpartum depression wikipedia , lookup
Anorexia nervosa wikipedia , lookup
Deinstitutionalisation wikipedia , lookup
Panic disorder wikipedia , lookup
Major depressive disorder wikipedia , lookup
Mental health professional wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Anxiety disorder wikipedia , lookup
Victor Skumin wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Spectrum disorder wikipedia , lookup
Mental status examination wikipedia , lookup
Emergency psychiatry wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Moral treatment wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Mental disorder wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Psychological evaluation wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Child psychopathology wikipedia , lookup
History of psychiatry wikipedia , lookup
Abnormal psychology wikipedia , lookup
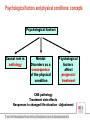
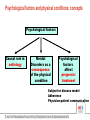
Psychological co-morbidity in Diabetes mellitus : assessment and therapy Prof. Dr. Claus Vögele Disability-adjusted life-years (DALY): sum of years lived with disability and years of life lost 20% Co-morbidity of mental disorders with Diabetes mellitus: a brief summary • Prevalence rates vary in relation to assessment techniques used. Typically higher prevalence rates (in particular depression and anxiety disorders) occur with the use of self-report scales as opposed to clinical interviews. • Nevertheless ... 12-months estimated prevalence in mood disorders 1.4 1.3 12-months estimated prevalence in anxiety disorders 1.6 1.5 12-months estimated prevalence in anxiety disorders 1.3 1.3 Co-morbidity of mental disorders with Diabetes mellitus: a brief summary Mental Disorder OR or observed prevalence Mood Disorders Major Depression Dysthymia 1.4 1.3 Anxiety Disorders GAD Agoraphobia/Panic Social Phobia PTSD 1.6 1.5 1.3 1.3 Schizophrenia 15% versus 2-3% (comm.) Psychological factors and physical conditions: concepts Psychological factors Causal role in aetiology Mental Disorders as a consequence of the physical condition Psychological factors affect prognosis/ treatment Health risk behaviours Neurobiological/psychophysiological processes Depression as a risk factor for Diabetes: neurobiological/psychoneuroendocrinological mechanisms • Depression is an independent risk factor for type 2 Diabetes (Eaton et al., 1996; Kawakami et al., 1999) Evidence for endocrinological mechanisms: • • • Depression is associated with increased serum glucocorticoids, catecholamines, and growth hormone (which counter the effects of insulin) and insulin resistance and secrection of inflammatory cytokines, which could facilitate development of diabetes (Musselmann et a., 2003). Psychological factors and physical conditions: concepts Psychological factors Causal role in aetiology Mental Disorders as a consequence of the physical condition Psychological factors affect prognosis/ treatment CNS pathology Treatment side effects Responses to changed life-situation - Adjustment Diabetes as a risk factor for Depression: Nouwen et al., 2010 Anxiety Disorders common amongst Diabetics • Hypoglycaemia anxiety – This can be associated with impaired perception of hypoglyaemic symptoms, which increases the probability of unexpected hypoglycaemic episodes and, therefore, the development of severe anxiety. • Specific type of blood-injection-injury phobia – Can lead to irregular insulin injections with all adverse consequences. • Panic Disorder (with or without Agoraphobia) – Panic attacks are often accompanied by very similar symptoms than hypoglycaemic episodes. Hypoglycaemic episodes can, therefore, contribute to the development of Panic Disorder. Eating Disorders common amongst Diabetics • The management of Diabetes requires patients to constantly be aware and check their food. The cognitive pattern (restrained eating) is typical for patients with Eating Disorders. • Anorexia nervosa and Bulimia nervosa are not more prevalent amongst Diabetics compared to community samples. However: • EDNOS (sub-clinical Eating Disorders syndromes) are more than twice as prevalent amongst young female Type-I diabetics. • Insulin-purging: deliberately reduced insulin intake in order to promote weight-reduction and fat-loss Psychological factors and physical conditions: concepts Psychological factors Causal role in aetiology Mental Disorders as a consequence of the physical condition Psychological factors affect prognosis/ treatment Subjective disease model Adherence Physician-patient communication Effects of severe mental illness on survival of people with diabetes Vinogradova et al., 2010 What needs to be done? 1.Psychological assessment • Interview (DSM), Questionnaires • Behavioural analysis: Analysis of individual conditions maintaining pathological processes Subjective Disease Models Illness Behaviour and Treatment Adherence Assessment of Individual Resources What needs to be done? 2.Psychological Treatment Treatment of Co-morbid Mental Disorders Depression: CBT and/or Pharamcotherapy Anxiety Disorders: CBT Blood glucose awareness training Discrimination training (learning to discriminate between symptoms of hypoglycaemia and panic reactions) Exposure based techniques Eating Disorders: CBT techniques in particular mirror image exposure What needs to be done? 2.Psychological Treatment • Health Promotion and Support in Illness Coping Stress Coping Patient Education Relaxation Training Biofeedback Who is / should be in charge? Appropriately qualified Psychologists e.g., Clinical Psychologists, Psychotherapists, Health Psychologists Literatur