* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Obsessive Compulsive Disorder
Factitious disorder imposed on another wikipedia , lookup
Major depressive disorder wikipedia , lookup
Kleptomania wikipedia , lookup
Trichotillomania wikipedia , lookup
Antipsychotic wikipedia , lookup
Selective mutism wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Rumination syndrome wikipedia , lookup
Mental status examination wikipedia , lookup
Bipolar disorder wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Autism spectrum wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Mental disorder wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Excoriation disorder wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Depersonalization disorder wikipedia , lookup
History of psychiatry wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Obsessive–compulsive personality disorder wikipedia , lookup
Spectrum disorder wikipedia , lookup
Conduct disorder wikipedia , lookup
Asperger syndrome wikipedia , lookup
History of mental disorders wikipedia , lookup
Conversion disorder wikipedia , lookup
Panic disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Anxiety disorder wikipedia , lookup
Child psychopathology wikipedia , lookup
Abnormal psychology wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
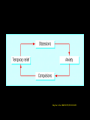
Obsessive Compulsive Disorder Dr Rebecca Jacob Consultant Psychiatrist Fulbourn Hospital Cambridge • Obsessive-Compulsive Disorder, OCD, is an anxiety disorder and is characterized by recurrent, unwanted thoughts (obsessions) and/or repetitive behaviors. • Excessive doubt, the need for completeness, shame, and abnormal assessment of risk in the mind of the patient are thought to underlie most obsessions. • Repetitive behaviors (compulsive acts) such as hand washing, counting, checking, or cleaning are often performed with the hope of preventing obsessive thoughts or making them go away. • Performing these so-called "rituals," however, provides only temporary relief, and not performing them markedly increases anxiety Most Common Symptoms Obsessions • Fear of causing harm to someone • Fear of harm coming to self • Fear of contamination • Need for symmetry or exactness • Sexual and religious obsessions • Fear of behaving unacceptably / making a mistake Compulsions • Cleaning • Hand-washing • Checking • Ordering and arranging • Hoarding • Asking for reassurance Mental acts • Counting • Repeating words silently • Ruminations • “Neutralising” thoughts The obsessive-compulsive disorder cycle. Heyman I et al. BMJ 2006;333:424-429 ©2006 by British Medical Journal Publishing Group Helpful Screening Questions • “Do you have repetitive thoughts that make you anxious and that you cannot get rid of regardless of how hard you try?” • “Do you keep things extremely clean or wash your hands frequently?” • “Do you check things to excess?” Jenike et al N Engl J Med 2004; 350:259-26 ICD 10 diagnosis • Symptoms present for >2 weeks, most days a) Obsessional symptoms recognized as individuals own thoughts. b) At least one thought that is still resisted unsuccessfully. c) Thought of carrying out acts not in itself pleasurable. d) Thoughts images or impulses repetitive. Epidemiology • Onset usually in childhood or early adult life. • M:F ratio 1:1 • Total prevalence 2.1% (pure form without comorbidity 1.2%) • Community samples 60-70% obsessions only, secondary care >70% suffer both obsessions and compulsions. Aetiology • Genetics: twin studies > concordance in monozygotic twins. Molecular studies, associations OCD gene coding/ 5HT ID. • Evidence of brain disorder: 1.Tourettes, Sydenham’s chorea, PANDAS • 2. Brain Imaging: no structural abnormalities but functional imaging (PET) activity orbitofrontal cortex, anterior cingulate gyrus, caudate nucleus and thalamus (altered with Rx). • Psychoanalytical- Freud suggested unconscious impulses (aggressive/ sexual) with attendance defence mechanism (repression, reaction formation). • Learning theory - abnormal learning with avoidance response • Cognitive Theory- deal with pts response rather than focusing on intrusive thoughts. • Abnormal Serotonergic function: Some studies measuring serotonin transport (PET/SPECT) suggestive but not conclusive. • Early Experience- nature AND nurture, weak link,stronger in non-specific neurosis. Differential Diagnoses • Anxiety Disorders • Depressive disorders • Schizophrenia-OCD thoughts may resemble delusions • Organic disorders: ecephalitis lethargica, Tourettes. Conditions that commonly occur with obsessive-compulsive disorder • • • • • • • • Condition Depression Specific phobia Social phobia Eating disorder Alcohol dependence Panic disorder Tourette's syndrome Schizophrenia Frequency (%) 50-60 22 18 17 14 12 7 14 Non-psychiatrists likely to see patients with obsessive-compulsive disorder (OCD) • • • • • • • • Professional General practitioner Dermatologist Cosmetic surgeon disorder) Oncologist GU specialist Neurologist Obstetrician Gynaecologist Reason for consultation Depression, anxiety Chapped hands, eczema, trichotillomania Concerns about appearance (body dysmorphic Fear of cancer Fear of HIV OCD associated with Tourette's syndrome OCD during pregnancy or puerperium Vaginal discomfort from douching Heyman et al BMJ 2006; 333 : 424 Management • Psycho-eduction • Investigation • Treatments (Assessments of severity and treatment response with rating scales- best validated Yale-Brown (Y-BOCS) scale.) Treatment • Medication- SSRI’s, Clomipramine SSRI’s plus augmentation strategies (antipsychotics /anixiolytics) • Cognitive Therapy-remedying faulty reasoning that may have developed with the disorder. • CBT • Neurosurgery Cognitive Behavioural Therapy • The patient generates a hierarchy of feared situations and then practices facing the fear (exposure), • During the exposure to the event he/she will monitor the anxiety and note that it lessens without the need to carry out a ritual (response prevention). Neurosurgery (limited RCT evidence) • Anterior cingulotomy, anterior capsulotomy, subcaudate tractotomy, and limbic leucotomy. ( Blocks connections between dorsolateral and the orbitomedial areas of the frontal lobes and limbic and thalamic structures). • Deep brain stimulation, surgically implanted electrodes that can be turned on and off to stimulate or inhibit activity in surrounding brain tissue, has been used for the treatment of Parkinson's disease and intractable pain; • Transcranial magnetic stimulation, whereby pulses of magnetic energy are intermittently administered to surface regions of the brain through the skull, appeared to be effective in one preliminary study.54 Treatment options for adults with obsessive-compulsive disorder (OCD). Obsessive-compulsive disorder: core interventions in the treatment of obsessive-compulsive disorder and body dysmorphic disorder. London: NICE, 2005. (Clinical guideline 31.)06;333:424-429 ©2006 by British Medical Journal Publishing Group Unanswered Research Questions in obsessivecompulsive disorder (OCD) Nosological status of OCD Should OCD be classified as an anxiety disorder? Do subtypes exist, each with different causes (for example, early onset OCD, OCD with co-morbid tics, compulsive hoarding)? Are hypochondriasis, body dysmorphic disorder, and other “spectrum” disorders variants or completely separate disorders? Causative Factors What are the precise genetics of OCD? Might environmental factors such as family environment or streptococcal infection be risk factors? Management Questions What is the most effective cognitive behaviour therapy package in terms of intensity and length of treatment and training of therapist? For how long should drugs be used? What makes some cases treatment resistant? How might treatments be best modified for these cases? Lecture session 2 Clinical Encounter • A 30 year old lady is referred to you by her GP with symptoms of anxiety, breathlessness and increasing social isolation. • How would you manage this case? Anxiety Disorders • Phobias (Specific/Social) • Panic Disorder • Generalized Anxiety Disorder • OCD • PTSD/ Acute stress, Adjustment disorders) Generalized Anxiety Disorder • Essential feature is anxiety, generalized and not persistent but not restricted to any particular environment ‘free floating’. • In addition to cognitive anxiety, autonomic symptoms must be evident. ICD 10 Diagnosis • Primary symptoms of anxiety for weeks and usually several month: a)Apprehension, worries, feeling on edge b)Motor tension, fidgeting, headaches c)Autonomic overactivity,sweating, dizziness etc Co-morbidities • Major depression most common coexisting psychiatric illness , occurring in almost two thirds of such patients. • Panic disorder occurs in a quarter of patients with generalized anxiety disorder, and alcohol abuse in more than a third. • In prospective studies, anxiety almost always appears to be the primary disorder and to increase the risk of depression. Treatment Non-pharmacological`: • Counseling: absence of well conducted controlled trials in other therapies • Relaxation Training • CBT Pharmacological Medication- : Short term (2-3 weeks) anxiolytics e.g. long acting benzodiazepines • Diazepam • Alprazolam • Clonazepam (BEWARE DEPENDANCE) Longer term: • other Anxiolytics- Buspirone • Antidepressants SSRI’s • Antipsychotics fluanxiol • Beta-adrenoceptor anatogonists, propranolol References • ICD 10 • NICE Guidelines Obsessive Compulsive and Body Dysmorphic Disorders. • Nice Guidelines Anxiety Disorders (GAD and Panic Disorders) in Primary and Secondary Care • Oxford Textbook of Psychiatry • Hineman et al BMJ 2006; 333 : 424 • Jenike et al N Engl J Med 2004; 350:259-265