* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download By Sasha Darwazeh FY1
Remote ischemic conditioning wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Rheumatic fever wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Jatene procedure wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Electrocardiography wikipedia , lookup
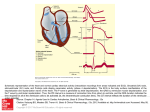
Arrhythmias By Sasha Darwazeh FY1 Types of arrhythmias Site of abnormality: Supraventricular ●Ventricular ● Abnormalities of heart rate: Tachyarrhythmias ●Bradyarrhythmias ● Tachyarrhythmias Supraventricular Tachycardias: Atrial Fibrillation 0.4% of population 2.4-4% >60 year olds, 4% >80 years olds. 50% of paroxysmal & 15-20% of chronic AF are idiopathic. 2º AF caused by dilatation, ↑ muscle mass, inflammation, infiltration & fibrosis. Generally associated with LA hypertrophy. Ineffective contractions = blood stasis in atria → thrombus formation. If from LA, can cause CVA; in RA can cause PE's. 3 types of AF: Acute AF - associated with systemic disease, precipated by electrolyte disturbance or hypoxia, resolves with treatment of underlying pathology Paroxysmal AF - recurrent episodes of AF lasting <48 hours which can progress to: Risk factors HTN Heart disease Lung disease Binge drinking Hyperthyroidism Carbon monoxide poisoning Clinical Features Early signs vague - fatigue & dyspnoea. Chronic phase- Irregular pulse (some impulses from atrial walls reach the ventricle, throwing it out of sinus rhythm). Force of contraction irregular Deteriorates with exercise Absent 'a' waves in JVP Thromboembolic events - CVA & PE. Investigations ECG Chronic AF- ECG Paroxsysmal- 24h ECG. Bloods FBC U+Es TFTs Imaging CXR Echo - size of LA, LV function. Transoesophageal echo for assessment of thrombus formation . Management Aim: return to SR. If not possible, control ventricular rate & thromboembolism risk Conservative Avoid alcohol & caffeine. Correct underlying pathologies - electrolyte disturbance, hypoxia. Medical Acute onset: If haemodynamicaly unstable → emergency cardioversion if lifethreatening. IV amiodarone if not. Paroxysmal - treat only if symptomatic: Beta-blockers 1st-line BISOPROLOL Class Ic antiarrhythmics 2nd-line FLECAINIDE or SOTALOL Chronic Rate-control <65; symptomatic; presenting 1st time; lone AF; or congestive heart failure. Digoxin + rate-limiting calcium-channel blocker i.e verapamil/diltiazem or digoxin + beta blocker. If fails pacemaker + ablation. Rhythm-control >65; coronary heart disease; contraindications to antiarrhythmics or elctrical cardioversion; no congestive heart failure. 1st line chemical cardioversion- amiodarone. 2nd-line: flecainide/sotalol, amiodarone in structural heart disease. Thromboprophylaxis- CHADS-VASc. Warfarin - ↓ incidence of stroke by 70%. INR 2-3. Surgery Percutaneous radiofrequency ablation: catheter up femoral vein to heart with radiological guidance. Ablate abnormal tissue. Never use verapamil & beta blocker together as can cause heart block & asystole Popular question in pharm exams! Atrial flutter Atrial contraction rate >250-300 bpm. Re-entrant circuit of excitation- it goes straight back into the atria instead of impulses only travelling to ventricles. Causes: IHD, hyperthyroidism, cardiomyopathy & rheumatic heart, idiopathic. Clinical Features: Palpitations Chest pain SOB O/E: Regular, fast pulse 'A' waves in JVP exceeds pulse rate Carotid compression may slow rate Signs of heart failure Investigations ECG: 3:1 block (3 atrial contractions: 1 ventricular contraction) → saw-tooth 2:1 block, P waves difficult to see. Carotid sinus pressure can uncouple atria & ventricles, revealing P waves. Consider in patients with a regular rate of 150 bpm. Blood: U+Es TFTs Imaging: Echo Management Drugs- antiarrhythmics: Class Ia - Disopyramide Class Ic - Flecanide, Propafenone Class III - Sotalol DC Cardioversion Pacing Re entry SVT's Caused by 2nd connection between atria & ventricles, in addition to normal conduction system. 2 types: nd ●AVRNT (Atrio-Ventricular Node Re-entry Tachycardia) - 2 connection closely related to AV node. nd connection not ●AVRT (Atrio-Ventricular Re-entry Tachycardia) - 2 related to AV node. Clinical Features: Palpitations Syncope/presyncope Chest pain & polyuria (release of ANP due to ↑ atrial pressures from contraction of atria against closed AV valve.) Symptoms often associated with exertion Investigation: ECG Rate 130-250. Narrow QRS complex P waves are inverted & one P wave per QRS complex. - masked by QRS complex (AVNRT) - or occur halfway between complexes (AVRT) Management Vagal - carotid sinus massage, valsalva manoeuvre, apply ice to face Drugs- adenosine/verapamil.(Or flecanide, sotalol) Electrical - pacing & cardioversion Ablation - burn away extra conduction pathway. WPW aka pre-excitation syndrome Abnormal accessory pathway between atrium & ventricle. Rare → 0.1-0.3% of the population. Males> females, young people Predisposition to sudden death. Clinical Features: Mostly asymptomatic. Occasionally, palpitations/sudden death, general cardiac symptoms (SoB, dizziness or syncope) Investigations ECG: Delta wave PR interval <0.12s Management Ablation 1st line in symptomatics If unstable - cardioversion Amiodarone/procainamide Ventricular Tachyarrhythmias Ventricular Fibrillation Ventricular muscle fibres contract randomly causing complete failure of ventricular function. Occurs in those with pre-existing disease i.e CHD. Risk Factors: CAD & MI VT which often precedes to VF Antiarrhythmic drug adminsitration Hypoxia Ischaemia AF Rapid rates in pre-excitation syndromes (e.g. WPW) Shock during cardioversion Electric shock Pacing to terminate VT Clinical Features MI → Chest pain, fatigue, palpitations Investigations ECG: VF and If survive look for evidence of MI, WPW etc. Bloods ●Cardiac enzymes: troponin-T 12 hours after onset of symptoms ●U+Es: metabolic acidosis, hypokalaemia, hyperkalaemia, hypocalcaemia, hypomagnasaemia ●Drug levels of any antiarrhythmic, particularly digoxin ●Toxicology: cocaine can induce vasospasm ●TSH: hyperthyroidism CXR: signs of left heart failure, pulmonary hypertension Echo: check for structural deficiencies Angiography Management of VF Shockable rhythm Check for response Check for pulse/ breathing for up to 10 seconds 2222 Head tilt/chin lift Get help Chest compressions 30:2 Attach monitor Assess rhythm Stand back & shock Continue compressions for 2 mins Adrenaline IV every 2-3 mins VT Broad-complex tachycardia (QRS >120ms/3 small squares). Risk Factors: Structural heart disease/CHD Electrolyte disturbances: hypokalaemia, hypocalcaemia & hyponatraemia Clinical Features: Features of ischaemic heart disease or haemodynamic compromise. Chest pain, palpitations, dyspnoea, dizziness, syncope & symptoms of heart failure. Investigations ECG Bloods: U+Es: particularly calcium, potassium & magnesium. Levels of therapeutic drugs like digoxin Trop T for MI CXR -? heart failure Management of VT Pulseless VT: treat using ALS ● Unstable VT: synchronised cardioversion- can result in VF! Amiodarone 1st -line for haemodynamically unstable VT. Treat electrolyte disturbances. ● Stable VT: treat with IV lidocaine & cardioversion if lidocaine ineffective ● Refractory VT: amiodarone. ● Torsades de pointes (polymorphic VT) ●Acute(acquired) – Stop QT prolonging drugs ?examples ●IV magnesium, then beta 1-adrenergic agonist (isoprenaline), temporary pacing ●Long-term - beta-blockers (congenital), pacing ● Bradycardias Heart Block 1st degree heart block - PR interval > 0.2s; no dropped QRS complex 2nd -degree heart block Type 1 (Mobitz I/Wenkebach) - PR interval ↑ with each beat until you get a dropped QRS complex Type 2 (Mobitz II) - intermittent failure of P waves to conduct, not preceded by P wave elongation 2:1 & 3:1 type - regularly dropped QRS complexes with a 2:1 or 3:1 ratio 3rd -degree heart block (complete heart block) - P waves never conduct & are unrelated on ECG Causes: usually CAD, inferior or anterior wall MI. Management 1st degree - no treatment 2nd degree – pacemaker if consciousness is affected. 3rd -degree – pacemaker Atropine can be used if symptomatic If patient has heart block, they need to avoid: ●Anti-arrhythmics - amiodarone, flecainide. ●Beta blockers - such as atenolol, bisoprolol, propanolol. ●Calcium channel blockers - such as verapamil, diltiazem. Bundle branch block Delay of electrical conduction down either the left of right bundle branch. LBBB: aortic stenosis, dilated cardiomyopathy, MI, CAD. RBBB: atrial septal defect, PE, MI ECG Changes WiLLiaM & MaRRoW Wide QRS complexes. LBBB: there is a W shape in V1 and an M shape in V6. RBBB: there is an M shape in V1 and a W shape in V6 Management Generally nothing but if bundle branch block is severe, needs pacemaker