* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pathogenicity
Germ theory of disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Immune system wikipedia , lookup
Infection control wikipedia , lookup
Adaptive immune system wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Gastroenteritis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
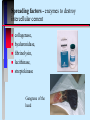
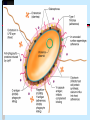
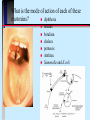
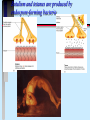
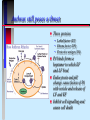
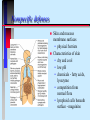
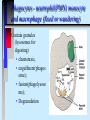
Pathogenicity What makes some bacteria dangerous? Disease Process Infection Virulence factors Pathogenicity No virulence factors Silent infection Environment Disease Symptoms Pathogenicity Ability to cause disease - this is qualitative yes or no Virulence - degree of pathogenicity Requires that organism survive host defenses cause damage Have virulence factors Bacterial virulence factors for adherence, colonization, and invasiveness Virulence • varies with infectivity and severity of damage Infectivity is often the single most important feature; the microbe must be able to "stick" around • Attachment molecules for bacteria are termed adhesins such as….. Microbes often enter cells to establish as intracellular parasites Some microbes move around the body from site of infection - invasiveness Within cells that circulate Through cells- in and out Through junctions that they weaken Cell entry of bacteria is typically by phagocytosis • Professional phagocytes • Non phagocytic cells are induced to local phagocytosis (Type III secretion) Salmonella entering gut cells Spreading factors - enzymes to destroy intercellular cement collagenase, hyaluronidase, fibrinolysin, lecithinase, streptokinase Gangrene of the hand Need to avoid host defenses to survive Antiphagocytic factors • Capsules, cell wall proteins • leukocidin • coagulase (walls off) • survival in WBC - intracellular parasites (mycobacteria, Listeria) IgA protease - Neisseria Opportunistic pathogens need compromised host N. meningitidis crosses blood-brain barrier Need for iron to survive How do bacteria damage the host? ENDOTOXIN vs EXOTOXIN • Composition LPS (lipidA) vs protein(immunogenic) • Toxic response fever and shock vs specific affect • Typically produced by gram negatives vs gram positives and negatives What is the mode of action of each of these exotoxins? diphtheria tetanus botulism cholera pertussis Anthrax Samonella and E.coli Botulism and tetanus are produced by endospore-forming bacteria Cholera deaths are preventable (iii) Salmonella Salmonella typhimurium - rod prokaryote (dividing); note the flagella. Causes salmonellosis (food poisoning). (x 20,800) © Dr Dennis Kunkel, University of Hawaii. Used with permission Based on genetic studies there is a single species of Salmonella (Salmonella enterica). Using appropriate antibodies more than 2000 antigenic "types" have been recognized. Only a few types that are commonly associated with characteristic human diseases 1. S. enteritidis 2. S. cholerae-suis 3. S. typhi 1. Salmonellosis, the common salmonella infection, is caused by a variety of serotypes (most commonly S. enteritidis) and is transmitted from contaminated food (such as poultry and eggs). 2. It does not have a human reservoir. 3. It usually presents as a gastroenteritis • nausea • vomiting • non-bloody stool 4. The disease is usually self-limiting (2 - 5 days). Like Shigella, salmonella invade the epithelium and do not produce systemic infection. In uncomplicated cases of salmonellosis, which are the vast majority, antibiotic therapy is not useful. S. cholerae-suis (seen much less commonly) causes septicemia after invasion. In this case, antibiotic therapy is required. The severest form of salmonella infections is called "typhoid" or enteric fever. Typhoid is caused by Salmonella typhi. This disease is rarely seen in the Australia. Typhoid is one of the historical causes of widespread epidemics and still causes epidemics in the third world. Salmonella typhi • The organism is transmitted from: 1. a human reservoir 2. in the water supply (if sanitary conditions are poor) 3. in contaminated food • It initially invades the intestinal epithelium and during this acute phase, gastrointestinal symptoms are noted. • The organisms penetrates (usually within the first week) and passes into the bloodstream where it is disseminated in macrophages. • Typical features of a systemic bacterial infection are noted. • The septicemia usually is temporary with the organism finally lodging in the gall bladder. • Organisms are shed into the intestine for some weeks. • At this time the gastroenteritis (including diarrhea) is noted again. • The Vi (capsular) antigen plays a role in the pathogenesis of typhoid. • A carrier state is common; thus one person e.g. a food handler can cause a lot of spread. • Antibiotic therapy is essential. • Vaccines are not widely effective and not generally used. Pertussis toxin helps bacteria bind to cilia and to kill cells Pentameric B subunit delivers A subunit ADP-ribosylates protein that is part of signal transduction mechanism at cell surface Kills cells in respiratory tract Anthrax still poses a threat Three proteins • Lethal factor (LF) • Edema factor (EF) • Protective antigen (PA) PA binds forms a heptamer to which EF and LF bind Endocytosis and pH change cause fusion of PA with vesicle and release of LF and EF Inhibit cell signalling and cause cell death Damage is often caused by the host Cytokine release Antibody cross reactions Immune complex deposition What about viruses? Adherence - access to cell with receptor Maintenance - ability to replicate Spread - no destruction in or out of cell Damage - lysis of cells, cytokine release, cross reactions of immune response Host Defenses Innate Resistance - genetic Nonspecific - present at all times but varies with portal of entry; directed against most bacteria Specific immunity - induced only after exposure; specific to the agent Nonspecific defenses Skin and mucous membrane surfaces • physical barriers Characteristics of skin • dry and cool • low pH • chemicals - fatty acids, lysozyme • competition from normal flora • lymphoid cells beneath surface - magainins How does mucous membrane differ? Moist Warm Living Defended by • • • • • • Mucus Sloughing Chemicals Peristalsis/cilia Normal flora Immune cells/molecules - -magainins Other chemical defenses Complement Phagocytes - neutrophil(PMN) monocyte and macrophage (fixed or wandering) Contain granules (lysosomes for digesting) • chemotaxis, • engulfment(phagos ome); • fusion(phagolysoso me); • Degranulation Activation of Compliment by Antgens “Classical pathway” Inflammation Localizes infection and prevents spread. Redness, swelling, pain and heat are due to vascular permeability which allows for phagocytic chemotaxis.