* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Drugs for Coagulation disorders - Suny-perfusion
Survey
Document related concepts
Polysubstance dependence wikipedia , lookup
Adherence (medicine) wikipedia , lookup
Psychedelic therapy wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Prescription costs wikipedia , lookup
Drug interaction wikipedia , lookup
Psychopharmacology wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Neuropharmacology wikipedia , lookup
Discovery and development of direct Xa inhibitors wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Discovery and development of direct thrombin inhibitors wikipedia , lookup
Transcript
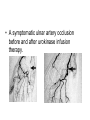
Drugs for Coagulation disorders • There are a number of different categories of drugs which modify the coagulation process: • I. Anticoagulants • II. Antiplatelet agents • III. Thrombolytics I. Anticoagulants A. The coagulation cascade • The coagulation cascade begins when injured cells release thromboplastin. • Thromboplastin converts the clotting factor prothrombin to thrombin. • Thrombin then converts the plasma protein fibrinogen to long strands of fibrin and activates several clotting factors (V, VIII, XIII, and protein C) • The fibrin strands form an insoluble web B. Types of anticoagulants • The mechanism of action of anticoagulant medications involves either the inactivation of various existing coagulation factors, or • preventing the synthesis of coagulation factors (the vitamin K antagonists) • Anticoagulant medications do NOT dissolve clots. 1. heparins • a. standard heparin • b. low molecular weight (LMW) heparins • Heparins are indicated for the treatment of: • deep vein thrombosis (DVT) • prophylaxis and treatment of venous thrombi, alone • prophylaxis and treatment of venous thrombi in conjunction with pulmonary emboli • Heparins are NOT direct thrombin inhibitors. • Instead, heparins prevent thrombin formation by binding to clotting factors in the circulation. • These clotting factors then bind to and inactivate thrombin, the major enzyme in the clotting pathway. • The main commercial sources of standard heparin are the lungs and intestines of cattle (bovine) and pigs (porcine). • LMW heparins are derived from porcine heparin. • They are smaller in size as they only contain the anticoagulant fraction of heparin, and not the additional saccharide chains that standard heparin has. a. Standard heparin • Standard heparin has an immediate onset of action if administered IV, it peaks within 5-10 minutes, and its duration is 2-6 hours. • Standard heparin has an onset of action of 20 minute – 1 hour if administered SC, it peaks within 2 hours, and its duration is 812 hours. • Standard heparin IV administration: bolus of 10,000 – 12,000 units followed by 5,000-10,000 units every 4-6 hours • Standard heparin SC administration: bolus of 10,000 – 12,000 units followed by 15,000-20,000 units every 12 hours b. Low molecular weight (LMW) heparins • LMW heparins are ONLY administered SC, have a rapid onset of action, generally peak within 3-6 hours, and have a duration of 12-24 hours depending on the agent. Specific LMW heparins include: • • i. dalteparin (Fragmin): • Indicated for prophylaxis of Deep Vein Thrombosis (DVT) in patients undergoing abdominal surgery or hip replacement surgery. • ii. enoxaprin (Lovenox): • Indicated for prophylaxis of DVT in patients undergoing abdominal, hip, or knee surgery. • iii. fondaparinux (Arixtra): • Indicated for both the treatment of and prophylaxis of DVT and pulmonary embolism (PE). • iv. tinzaparin (Innohep): • Indicated for both the treatment of and prophylaxis of DVT. • LMW heparins have certain advantages over standard heparin: • 90% bioavailability (standard heparin has 30%) • LMW heparin can be dosed based on body size without coagulation test monitoring (if patient has normal kidney function) • Adverse effects of heparins: • hemorrhage • anemia in elderly with Lovenox, due to decreased clearance • fever • hair loss • thrombocytopenia (↓ in no. of platelets) • Black box warning for LMW heparin use in patients concurrently receiving epidural or spinal anesthesia as it increases the risk for epidural or spinal hematomas 2. thrombin inhibitors • Unlike the heparins, these drugs bind directly to thrombin. They are all administered IV. • a. argatroban (Argatroban) • indicated for patients with, or at risk for thrombocytopenia who are undergoing percutaneous coronary intervention (PCI). • b. bivalirudin (Angiomax): used, along with aspirin, in patients with unstable angina who undergo PCI. This treatment is intended to reduce the risk of acute ischemic complications • c. lepirudin (Refludan): derives from the natural product hirudin, found in leech saliva. • Leeches have been used for bloodletting since the times of the ancient Greeks. 3. anticoagulants which prevent the synthesis of coagulation factors • This category of anticoagulant is significantly different from the heparins in that it can be administered orally. • This type of anticoagulant has a longer onset because of the time required to clear the normal clotting factors from the circulation before an effect can be observed. • The only drug in this class is warfarin sodium (Coumadin): 2-10 mg • Its onset of activity is about 12-72 hours. • However, its duration of action is longer (2 to 10 days) even after drug administration has been discontinued. • Coumadin is indicated for the treatment of DVT and prevention of myocardial reinfarction • • • • • • Adverse effects include: GI disturbances hypotension hair loss headache hemorrhage (most serious) • A black box warning indicates that there is an ↑ risk of hemorrhage in: • patients over 65 • patients with a history of GI bleeding • INR > 4 • INR (international normalized ratio) is a test used to monitor coagulation status. • People not on anticoagulants have an INR of 1 • An INR of 2 – 3 is needed for a therapeutic effect with warfarin II. Antiplatelet agents • Antiplatelet agents exert an anticoagulant effect by interfering with various aspects of platelet function. • Antiplatelet agents are indicated for the treatment of : • thrombocytopenia • acute coronary syndrome • prevention of myocardial re-infarction • and reducing coronary events • The 2 subclasses of antiplatelet agents are: • A. nonselective COX inhibitors • B. adenosine diphosphate (ADP) receptor blockers A. nonselective COX inhibitors • Normally, the cyclooxygenase enzyme pathway in platelets results in the production of thromboxane A2, a potent platelet aggregator. • Aspirin, in doses from 81 mg (baby aspirin) to 325 mg (adult analgesic dose) irreversibly blocks a step in this pathway, preventing the synthesis of thromboxane A2. • Therefore, thromboxane will not be active until new platelets are formed. B. ADP receptor blockers • These drugs interfere with a receptor on the membrane of platelets, preventing them from aggregating. • Adenosine diphosphate (ADP) normally binds to these membrane receptors in platelets, resulting in the coagulation of the platelets. • The drugs in this class block the receptor so that ADP cannot bind. • All of the drugs in this class are administered orally. • • • • • 1. ticlopidine (Ticlid): 250 mg, bid 2. clopidogrel (Plavix): 75 mg 3. cilostazol (Pletal): 100 mg, bid 4. prasugrel (Effient): 5 – 10 mg with food 5. anagrelide (Agrylin): 1.0 mg, bid III. Thrombolytics • Thrombolytics are enzymes used to dissolve blood clots. • They convert plasminogen to plasmin, which is then able to degrade the fibrin present in clots. • Their primary functions are: to break apart pulmonary emboli and coronary artery thromboses during acute MI. • They need to be administered as soon as possible once it has been established that a clot or infarct has occurred. • Other disorders for which they may be indicated are: • DVT • stroke • occluded central venous access devices • For the treatment of acute MI: administer the drug within 1-6 hours of the onset of symptoms. • There is a longer window of opportunity for use of these drugs in treating a pulmonary embolism. Here the time for initiation of therapy may be up to a few days. • All drugs in this class are enzymes that must be administered IV. A. streptokinase • Streptokinase (Streptase, Kabbikinase): generally, 250,000 IU over 30 minutes, then 100,000 IU/hour for up to 72 hours • Larger doses may be used in the treatment of MI B. urokinase • urokinase (Abbokinase): IV 4400-6000 IU administered over several minutes to 12 hours • A symptomatic ulnar artery occlusion before and after urokinase infusion therapy. C. thrombolytics produced via recombinant DNA • alteplase (Activase, Cathflo), reteplase (Retavase) and tenecteplase (TNKase) are thrombolytic enzymes produced through recombinant DNA technology • alteplase: based on patient weight, not to exceed 100 mg. Generally, a 15 mg bolus, followed by 50 mg over next 30 minutes then 35 mg over the next 60 minutes • reteplase: 10 unit bolus over 2 minutes, wait 30 minutes, repeat • tenecteplase: a single bolus, over 5 seconds based on body weight, not to exceed 50 mg • Generally used in conjunction with aspirin and heparin therapy • • • • • • • Adverse effects of the thrombolytics: hemorrhage rash/itching headache nausea bronchospasm cardiogenic shock or arrhythmias with the recombinants