* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download WHITE BLOOD CELLS Formation Function ~ TEST YOURSELF
Adaptive immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Atherosclerosis wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
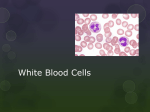
Chapter 9 WHITE BLOOD CELLS Any nucleated cell normally found in blood is a white blood cell. White blood cells are also known as WBCs or leukocytes. When white blood cells accumulate in one place, they grossly appear white or cream-colored. For example, pus is an accumulation of white blood cells. Mature white blood cells are larger than mature red blood cells. There are five types of white blood cells. They are neutrophils, eosinophils, basophils, monocytes and lymphocytes (Table 9-2). White blood cells can be classified in three different ways: 1. Type of defense function • Phagocytosis: neutrophils, eosinophils, basophils, monocytes • Antibody production and cellular immunity: lymphocytes 2. Shape of nucleus • Polymorphonuclear (multilobed, segmented nucleus): neutrophils, eosinophils, basophils (Figure 9-4) • Mononuclear (single, rounded nucleus): lymphocytes • Pleomorphic (varying shapes, nonsegmented nucleus): monocytes 3. Presence or absence of specific staining cytoplasmic granules Granulocytes (presence of granules): neutrophils, eosinophils, basophils • Agranuloctyes (absence of granules): lymphocytes, monocytes Blood, Lymph, and Immunity 231 All white blood cells develop in the bone marrow except for some lymphocytes (they start out in bone marrow but develop elsewhere). At the beginning of leukopoiesis all the immature white blood cells look alike even though they're already committed to a specific cell line. It's not until the cells start developing some of their unique characteristics that we can tell them apart. Function The function of all white blood cells is to provide a defense for the body against foreign invaders. Each type of white blood cell has its own unique role in this defense. If all the white blood cells are functioning properly, an animal has a good chance of remaining healthy. Individual white blood cell functions will be discussed with each cell type (see Table 9-2). In providing defense against foreign invaders, the white blood cells do their jobs primarily out in the tissues. The white blood cells use the peripheral blood to travel from their site of production (bone marrow) to their site of activity (tissue). There is a constant flow of white blood cells out of marrow and into tissues in an attempt to control the millions of foreign invaders that attack a body every day. It's happening in us too. And as long as they do their job, we don't even realize what's going on and we remain healthy. Formation The general term for the formation of white blood cells is . leukopoiesis. All white blood cell production starts out in the red bone marrow from the same pluripotent stem cell (PPSC) population that produced red blood cells and megakaryocytes. It is the stimuli that act upon the PPSCs that determine which cell type will be produced. Each type of white blood cell has its own stimulus for production. TABLE 9-2 ~ TEST YOURSELF 1. List the five white blood cells and indicate if each one is a granulocyte or an agranulocyte. 2. What is the common function of all white blood cells? 3. Which cell is the only white blood cell not capable of phagocytosis? White Blood Cells Name Cytoplasmic Granules Nuclear Shape Function Site of Action Neutrophil Polymorphonuclear Phagocytosis Body tissues Eosinophil Don't stain (usually invisible) Stain red Polymorphonuclear Body tissues Basophil Stain blue Polymorphonuclear Allergic reactions, anaphylaxis, phagocytosis Initiation of immune and allergic Body tissues None Pleomorphic reactions Phagocytosis and process antigens Body tissues or blood None Mononuclear None Mononuclear Monocyte (macrophage) B cell (lymphocyte) T cell (lymphocyte) Antibody production and humoral immunity Cytokine production and cell-mediated immunity Lymphoid tissue Lymphoid tissue and other body tissues 232 Chapter 9 Blood, Lymph, and Immunity Nucleus :~"':'-;':' • r:;; • •...' ::::.::::.. ~ • • ..'..:::~~.~. ~ ' •••..~.. ~:o.:::: ' ~. -, ~:'::..":'~ :::". ;"::'@-:':':'. ;..··tI:: ~.:.. :" Vi l?o0.,'. • " ,,\\. " " ~ " ~" .. ", : .. .. Figure 9-4 • ::.~".: .' . . . . . . .. .. : 0.. : " he total white blood cell count and differential count are used to evaluate a patient for the diagnosis or prognosis of an abnormal condition. For example,. if an infection is' present in the body, there will be an increased need for neutrophils to killthe invading microorganisms. The bone marrow responds to this need by releasing more neutrophils into the bloodstream that willtravel to the infected tissue. The increased number of neutrophils in the blood will increase the total white blood cell count. The total white blood cell count is equal to the sum of each of the individual white blood cell counts. If one cell type increases or decreases, the total white blood cell count will increase or decrease accordingly. Sounds simple, doesn't it? Unfortunately, it's not always that simple. If one cell type increases and another cell type decreases, the net effect could be a normal total white blood cell count. That's the tricky part, so the total white blood cell count is only one of a series of tests performed to evaluate the white blood cells. To find out which white blood cells are affecting the total white blood cell count, we have to look at a stained smear of the blood. The usual method for evaluating the blood smear is to count the first 100 white blood cells and keep track of the number of each white blood cell type you see. This is called a ;..... ' .'.:' . .:W ." . .. ",," ..: 0:: .. Normal neutrophils showing polymorphonuclear T II • : •• ' •: " '...., "1': :. .:"• .: .. .. : 0,,":" :"" characteristics. differential count, commonly referred to as "the diff." Because you're counting 100 cells, the number of each cell type you see can be expressed as a percentage. For example, if you count 100 cells and find that 20 of the cells are neutrophils and 80 of the cells are lymphocytes, you would report you saw 20% neutrophils and 80% lymphocytes. There are automated hematology analyzers that will provide these numbers, but they won't pick up all cellular abnormalities. For this reason, you should always look at a stained blood smear even if you're using an automated analyzer. You don't have to complete a differential count; just look for physical abnormalities. For every species of common domestic animal, there is a value range that represents a normal white blood cell count. There is also a normal range for individual white blood cell types. For example, a dog willnormally have between 6 billion and 17 billion white blood cells per liter of blood, and 60% to 70% of these cells should be neutrophils. Cattle will have between 4 billion and 12 billion white blood cells per liter and only 15% to 45% of the cells should be neutrophils. Taken together, the total white blood cell count and the differential count can provide a lot of information about an animal's state of health. Granulocytes CLINICAL APPLICATION The granulocytes are the neutrophils, eosinophils, and basophils. They are named for the color of the granules in their cytoplasm when viewed on a stained blood smear (see an earlier discussion of stains in this chapter). Eosinophil granules pick up the acidic stain and appear red, basophil granules pick up the basic stain and appear blue, and neutrophils don't pick up either stain very well, so for the most part, the neutrophil granules appear colorless or faintly violet on a stained blood smear. :/.ld.r~~h!J!i!~~ti~2·;Z~'.!~;~.~i&z1~;i"~l0C~~;t~,.::.;;] he word leukemia means "white blood." It is caused by an abnormal proliferation of one of the white blood cell types. In response to some unknown stimulus, the stem cells in the bone marrow start producing abnormal cells in one cell line at an increased rate. These abnormal cells show up in peripheral blood in large numbers, many times before they are mature, and cause the total white blood cell numbers to increase dramatically aeukocytosis}. Leukemias are considered a form of malignancy or cancer and can be acute or chronic. They are classified by the type of cell involved (e.g., lymphocytic leukemia, monocytic leukemia, eosinophilic leukemia). T Formation. The production of all granulocytes is called granulopoiesis. In the bone marrow, early granulocytes are impossible to distinguish from one another. They are all large cells with lots of cytoplasm and large round nuclei. Initially there are no cytoplasmic granules. As the granulocytes mature, a first set of granules is formed. Chapter 9 These granules are the same in all three granulocytes and are called nonspecific granules. Gradually, the nonspecific granules are replaced by a new set of granules that is unique to each granulocyte type. These are called specific granules. The Golgi apparatus produces both nonspecific and specific granules. The substances found in its granules determine the function of a granuloctye. For example, neutrophil granules contain chemicals called lysosomal enzymes, which aid in killing microorganisms that have been engulfed by the neutrophil. Neutrophils have therefore become a major factor in preventing invading microorganisms from causing disease. An early granulocyte has blue cytoplasm indicating that it is a metabolically active cell. As it matures, the cytoplasm becomes less active and therefore doesn't stain as blue. Mature granulocytes in circulation contain almost colorless cytoplasm containing the specific granules. In fact, if it weren't for the granules, the limits of the cell membrane would be difficult to see, making it look like the nucleus was pretty much floating around alone. This sometimes is just how neutrophils appear because of their colorless or faintly stained granules. As a granulocyte matures, its nucleus transforms from a round structure to a segmented structure that takes on many shapes (polymorphonuclear). Thin filaments connect these segments. The chromatin pattern of the nucleus starts out quite loose. As the nucleus squeezes itself down into segments, the chromatin becomes more condensed. As the cell ages and approaches death, the segments break apart and lose all evidence of any chromatin pattern. This process is called pyknosis, and it is an indication of a dead cell. Neutrophils. Neutrophils are also known as polymorphonuclear cells (because their nuclei have many shapes), PMNs (PolyMorphoNuclear leukocytes), and segs (because their nuclei are segmented). Even though eosinophil, basophil, and monocyte nuclei can be polymorphonuclear, the neutrophil is the only cell that is commonly called a PMN. The neutrophil is the most numerous white blood cell in circulation in the dog, horse, and cat. Formation. Neutrophils are produced in the bone marrow and released into blood as needed, when neutrophils already in circulation leave the bloodstream and enter tissue to kill microorganisms or simply die of old age. It takes 3 to 6 days to produce a mature neutrophil under normal conditions, depending on the species of animal. If the body has a sudden need for more neutrophils, this time can be shortened. Blood, Lymph, and Immunity f a neutrophil nucleus in peripheral blood has more than segments, it is called a hypersegmented nucleus (see figure). This indicates that the neutrophil has stayed in peripheral blood longer than normal, because hypersegmenting usually takes place in tissue as part of the normal aging process. The presence of hypersegmented neutrophils on a stained blood smear can be indicative of a pathological condition that prevented neutrophils from leaving circulation, or it can mean the smear was made from old blood. Remember, blood is still living when it is removed from the animal, and it will continue the aging process as long as it can. So hypersegmented neutrophils may be just aging normally in the tube. Hypersegmented neutrophils are seen within a day after .dhe blood sample was drawn. For this reason, it is important that a smear be made as soon as possible after the blood sample is drawn. Ifive Nucleus Cytoplasm Hypersegmented nucleus. Can indicate an older cell than is normally found in peripheral blood. pieces of nucleus but are joined by a thin strand of chromatin. Sometimes this strand of chromatin is difficult to see, so it looks like the segments are separated. If the neutrophil is released from the bone marrow before it is mature, it will have a horseshoe nucleus without any segmentation. This is called a band neutrophil. When band neutrophils are seen in peripheral blood, it is an indication that there is an increased demand for neutrophils beyond what the bone marrow can supply in mature neutrophils. If the bone marrow runs out of band neutrophils and still hasn't met the body's demand, it will start releasing progressively more immature cells. function. Neutrophils Characteristics: Neutrophil granules don't stain with either the blue alkaline stain or the red acid stain, so they are said to be neutral. This means they are difficult to see on a stained smear; so identification of neutrophils is commonly based on nuclear morphology, rather than granule staining characteristics. A mature neutrophil in peripheral blood will have from two to five nuclear segments. The segments aren't separate 233 are phagocytes. That means they engulf (phagocytize) microorganisms and other microscopic debris in tissues. Neutrophils are part of the second line of defense, after the skin and/or mucous membranes, when invading microorganisms enter the body. Neutrophils can respond very quickly. Their granules contain digestive enzymes that are capable of destroying bacteria and viruses that have been engulfed. The neutrophil granules are organelles called lysosomes. ;------~ 234 . Chapter 9 Blood, Lymph, and Immunity Tissue Endothelial cells ® ® ® ® . ~ Microorganrsms ••• Capillary ~ ~ ?a.~<3>~~ ® Cytoplasmic "'" granules ~~ """'(Iysosomes) • ® •• •• ~ ® 0) ®~ ®@~••• ® ®® ',. Neutrophils use blood as a transportation medium to take them to their site of action in tissue. Normally a neutrophil will spend an average of 10 hours in circulation before it enters the tissue. This circulation time is shorter when there is an increased demand for neutrophils in the tissue. Once a neutrophil enters tissue it doesn't return to blood, so all circulating neutrophils need to be replaced about two and a halftimes a day. Under normal conditions, they are replaced by mature neutrophils held in reservein the bone marrow. Neutrophils leave the blood vessel by squeezing between the cells of the endothelium in a process called diapedesis (Figure 9-5). Neutrophils are normally found in tissues that are constantly exposed to microorganism invasion (e.g., the lungs and intestinal tract). Other neutrophils wander through tissue to the sites where they are needed. Neutrophils stay in tissue until they die of old age or are destroyed by the microorganisms they are trying to destroy. Dead or abnormal neutrophils are picked up and destroyed by tissue macrophages. (See the discussion of tissue macrophages in the section on monocytes.) Think of neutrophils as garbage cans and tissue macrophages as garbage trucks. Neutrophils are attracted to a site of infection by chemotaxis, a process by which neutrophils and other cells are attracted by inflammatory chemicals produced by the interaction between microorganisms and the tissues they are invading. Having arrived at the site invaded by the microorganisms, the neutrophil must recognize what to ingest. Detecting some microorganisms is not a problem for the neutrophils. Other microorganisms try to "hide" inside capsules that make them difficult for neutrophils to recognize. To help make the microorganism more recognizable to the neutrophil, the encapsulated microorganism is coated with a plasma protein, usually a specific antibody. (See the discussion of antibody production in the immunity section.) These plasma proteins are called opsonins. Coating the microorganism enables the neutrophil to recognize it as foreign ® ® @® •• , Figure 9-5 Diapedesis. 1, Neutrophil lying against vessel wall begins to squeeze through the space between endothelial cells by flowing into pseudopod (false foot). 2, Pseudopod continues to push its way between cells. Rest of the cell cytoplasm flows along with it. 3, Pseudopod and the rest of the cell emerge on tissue side of blood vessel. 4, Neutrophil is off in search of foreign invaders to phagocytize. Neutrophil ® ~ 0~ ® Figure 9-6 Phagocytosis and destruction of microorganisms. 1, Neutrophil membrane engulfs microorganisms. 2, Phagocytic vacuole is formed. 3, Cytoplasmic granules (lysosomes) line up around phagocytic vacuole and empty their digestive enzymes into vacuole. 4, Microorganisms are destroyed. and to begin phagocytosis. The coating process is called opsonization. When the neutrophil recognizes a foreign microorganism, its outer membrane flows around the invader and encases it within a membrane-bound phagocytic vacuole (Figure 9-6). If you've seen the 1950s sci-fi movie The Blob, then you've seen how a neutrophil operates: it flows around anything in its way. (If you haven't seen the movie you should. It's a hoot.) The microorganism is surrounded by the neutrophil membrane, but isn't really inside the neutrophil. Think of it as a hug. When you put your arms around something, you're encasing it but not taking it inside your body. At this point, the neutrophil's cytoplasmic granules (lysosomes) move to the edge of the vacuole that contains the microorganism, fuse with the membrane, and secrete their digestive contents into the vacuole. Neutrophils increase their metabolism of oxygen during ingestion of microorganisms to produce substances that are toxic to ingested bacteria. Hydrogen peroxide is the product of oxygen metabolism that is the most important for the killing activity of neutrophils. Hydrogen peroxide is capable of killing bacteria (bactericidal effect) all by itself, but its action is enhanced by the enzyme myeloperoxidase, which is released from neutrophil granules. Lysozyme from the granules also enhances the bactericidal action of hydrogen peroxide and is capable of destroying the cell walls of microorganisms. Count in Peripheral Blood. The neutrophil count in peripheral blood is kept within a specific range in a healthy animal. This number is controlled by three factors: l. Release of mature neutrophils from the storage pool in the bone marrow into the peripheral blood. In the bone marrow storage pool, there is usually a 5-day supply of mature neutrophils. They are ready for immediate release if there Neutrophil Chapter 9 ~~~ Blood, Lymph, and Immunity 235 ~ fthere is an increased demand for neutrophils in tissue, bone marrow willrelease its reserve stores of mature-and, if necessary, immature-neutrophils into blood, so they can be transported to the site where neutrophils are needed. If a blood sample is drawn while these neutrophils are in transit, there will be a higher than normal number of neutrophils in the sample. This is called neutrophilia, and it is usually detected during a differential cell count. The increased number of neutrophils will also increase the total number of white blood cells in the sample. This is called leukocytosis and usually is detected using an automated blood analyzer or by looking at the thickness of the buffy coat in a hematocrit tube. Leukocytosis with accompanying neutrophilia can indicate an infection somewhere in the body. I fan infection is out of control, all the reserves of neutrophiIs can be used up faster than the bone marrow can replace them. If this happens, the number of neutrophils in circulation decreases, because the neutrophils are leaving the bloodstream and entering tissue, and there are no cells in the bone marrow to replace them. This condition is called neutropenia. The total white blood cell count will also decrease. This is leukocytopenia. The prognosis is poor for an animal that is clinicallyillwith accompanying neutropenia and leukocytopenia. It means the body is losing the war against the invading microorganisms. I is a sudden drop in circulating numbers of neutrophils caused by increased movement of neutrophils into tissue. 2. Rate of escape from peripheral blood into tissue. This rate depends on the need for neutrophils in the tissue. With a massive acute infection (e.g., coliform mastitis in cattle), the total neutrophil population of the peripheral blood can enter the tissue in a matter of hours. 3. The entrance of increased numbers of pluripotent stem cells into the neutrophil production line. This is a slow method of control because it takes 3 to 6 days for the neutrophils to mature and be ready to be released. Intravascular Pools of Neutrophils. In peripheral blood there are two pools of mature neutrophils: 1. The circulating pool is contained in the blood as it flows through the blood vessels. It is found toward the center of the lumen of the vessel. Blood samples obtained for laboratory analysis contain the neutro- eutrophils can move freely between the circulating and marginal pools. At any given time in dogs, cattle, and horses, there is about a 50:50 ratio between the number of neutrophils in the circulating pool and the marginal pool. In cats, the ratio is about a 30:70. Cells can detach from the marginal pool and enter the circulating pool when an animal is experiencing some sort of physical or mental stress. Trauma, fear, and exercise are a few of the stresses that may lead to a temporary transfer of neutrophils from the marginal pool to the circulating pool. This predictable neutrophil response is part of a larger physiological reaction called the stress response. Splenic contraction also plays an important role in this ,•. movement of cells out of the marginal pool. The temporary movement of neutrophils into the circulating pool can artificially elevate the total neutrophil count (neutrophilia) and the total white blood cell count (leukocytosis) because the normal values are based only on the number of cells normally found in the circulating pool. These artificiallyelevated results can lead to a possible misdiagnosis. Remember this when you have to chase a horse around a pasture or wrestle with a cat to get a blood sample. The administration of corticosteroid drugs, which are similar to glucocorticoid hormones (see Chapter 15) will cause the same response. This is one good reason for drawing a blood sample before medications are administered. N t phils from this pool. The normal range of neutrophil numbers in peripheral blood is based on the neutrophils contained in this pool. 2. The marginal pool is composed of neutrophils that line the walls of small blood vessels mainly in the spleen, lungs, and abdominal organs. These neutrophils are not circulating and are not contained in blood samples obtained for laboratory analysis. Eosinophils. Eosinophils are named for the red granules in the cytoplasm of mature cells. The granules stain with the red eosin component of the blood stain. They make up 0% to 5% of the total white blood cell count. fonnation and Characteristics. Eosinophils are produced in the bone marrow from the same pluripotent stem cells that give rise to all other blood cells. It takes 2 to 6 days to produce an eosinophil from a PPSc. The cytoplasmic granules take up the acidic stain eosin and appear red when seen on a blood smear. Frequently the segmented nucleus has only two lobes. The granules are shaped differently in various species: • Dogs: Granules are round. Their size varies from small to large within the same cell, and they stain very lightly. 236 Chapter 9 Blood, Lymph, and Immunity Cats: Granules are small, rod-shaped, and numerous. They stain darker than canine eosinophil granules. • Horses: Granules are very large, round or oval, and stain very intensely. • Cattle, sheep, and pigs: Granules are round and much smaller than equine granules. They stain pink to red. There is a good bone marrow reserve of eosinophils. There are also circulating and marginal pools of eosinophils in peripheral blood, like the neutrophil pools. Eosinophils don't stay in peripheral blood very long but migrate into tissue in a few hours, where they spend the rest of their lives. In tissue they undergo the same aging process as neutrophils. function. The functions of eosinophils are not yet entirely understood, but like neutrophils, the functions are determined by the contents of their granules. Chemotaxis regulates their entry into tissue. They don't re-enter circulation once they leave blood vessels. Large numbers of eosinophils-, are normally found in certain tissues in the body (e.g., skin, lung, small intestines). Three key functions are most often associated with eosinophils: • Anti-inflammatory response. Eosinophils are attracted to and inhibit local allergic and anaphylactic reactions. Their granules contain anti-inflammatory substances that are released at the site of the allergic reaction. • Immunity. Eosinophils can ingest substances associated with the humoral immune response (e.g., antigenantibody reaction complexes). • Phagocytosis. Eosinophils have minimal phagocytotic and bactericidal functions, but they are especially effective in the phagocytosis of large, pathogenic organisms, such as protozoa and some parasitic worms but are not protective against most bacterial infections. Basophils. Basophils are named for the blue granules in the cytoplasm of mature cells. The granules stain with the basic component of the blood stain. They are the white blood cell least often seen in circulation, and for this reason they are also the least understood white blood cell. Formation. Basophils are produced in the bone marrow from the same pluripotent stem cell as the other blood cells. Not much is known about the production and function of basophils. Characteristics. The basophil granules are water soluble and are frequently washed out during the staining procedure, so they are not always readily visible on a stained smear. When they are seen, the basophil granules stain blue and fill the cytoplasm. A dog has fewer granules than the other common domestic species. Basophils most often have a two- to three-lobed nucleus. Basophils and Tissue Mast Cells. Basophils share some characteristics with tissue mast cells, but some controversy exists over the relationship between these two cells. Mast cells are normally found in tissue and don't migrate there from blood. Basophils are not commonly seen in tissue. Mast cells are larger than basophils and have more cytoplasmic granules that are not water-soluble. Mast cells have a round nucleus that doesn't segment. Two theories currently exist regarding this relationship: 1. Mast cells and basophils are two different cell types with similar characteristics. They are produced in two different areas of the body and don't give rise to one another. 2. Mast cells are tissue basophils. This theory is not as popular as the first theory. Eosinophilia and Leukocytosis. Increased numbers of eosinophils in peripheral blood (eosinophilia) can be seen during allergic reactions and certain parasitic infections. The increased numbers are a response to a demand created by a pathological condition in the animal. An accompanying leukocytosis may also occur, but because there are normally few eosinophils in circulation, the increased number may not be enough to elevate the white blood cell count beyond the normal range. Eosinophilia can result from any of the following: • Increased release of mature eosinophils from the storage pool in the bone marrow • Migration of eosinophils from the marginal pool to the circulating pool • Increased production in the bone marrow • Increased time spent in peripheral blood before entering the tissue Eosinopenia. Decreased numbers of eosinophils in peripheral blood (eosinopenia) are difficult to detect and evaluate, because their numbers are normally low. function. Not much is known about the function of basophils. They are the least phagocytic of the granulocytes. Basophil granules contain histamine and heparin, which are responsible for at least part of basophil function in the following ways: • Histamine helps initiate inflammation and acute allergic reactions. Eosinophils are attracted to the site of an allergic reaction by eosinophilic chemotactic factor released from the basophil granules. • Heparin acts as a localized anticoagulant to keep blood flowing to an injured or damaged area. Basophilia and Basopenia. Increased numbers of basophils in peripheral blood (basophilia) can be associated with an allergic or hypersensitivity reaction in tissue. Sometimes basophilia and eosinophilia are seen at the same time. Decreased numbers of basophils in peripheral blood (basopenia) are difficult to evaluate because basophils are so Chapter 9 Agranulocytes Agranulocytes are white blood cells that don't have specific staining granules in their cytoplasm. They include monocytes and lymphocytes. Monocytes. Monocytes make up 5% to 6% of the cirwhite blood cells in all common domestic Formation and Characteristics. Monocytes are formed in the bone marrow from pluripotent stem cells. They mature much faster than neutrophils (total monocyte development time is 24 to 36 hours) and stay in the blood longer (24 to 36 hours) than neutrophils. From peripheral blood, monocytes enter the tissue, where they do their work. Monocytes are the largest white blood cells in circulation. They have abundant cytoplasm that stains gray-blue and may contain vacuoles of varying sizes. Sometimes the cytoplasm takes on a fine granular appearance that is commonly referred to as a "ground glass" appearance. The nucleus can be round or any number of shapes (pleomorphic), but it doesn't split up into distinct segments like a mature granulocyte nucleus. function. Monocytes are major phagocytic cells. When they enter tissue, they become known as tissue macrophages. Monocytes in the bloodstream are less effective phagocytes than tissue macrophages. In fact, monocytes are considered immature tissue macrophages. Tissue macrophages are larger than monocytes and can be found in any tissue, but are most prevalent in "filter" organs such as the liver, spleen, lung, and lymph nodes. These filter organs are responsible for removing or containing foreign invaders, damaged and old blood cells, and cellular debris. Some tissue macrophages wander through tissue freely, while others become fixed in specific tissues and remain there for the rest of their life span. Collectively the tissue macro phages and monocytes are known as the mononuclear phagocyte system (MPS). Monocytes and tissue macrophages perform several specific functions: They clean up cellular debris that remains after an inflammation or infection clears up. • They process certain antigens, making them more antigenic. Monocytes and tissue macrophages can ingest antigens and present them on their cell membranes to the lymphocytes that will then destroy them. This important role in the immune response will be discussed in the immune system section of this chapter 237 • They ingest foreign substances. They have the same phagocytic capabilities as neutrophils and then some. They are larger than neutrophils, so they can engulf structures beyond the phagocytic capacity of neutrophils (e.g., fungi, protozoa, viruses, and dead neutrophils). Monocytes follow neutrophils into tissue by the process of chemotaxis in response to tissue damage caused by trauma or invading microorganisms. Neutrophils respond more quickly to the tissue damage, but monocytes stay around longer once they get to the damaged site and become tissue macrophages. Tissue macrophages have a longer life span than neutrophils, so they are often associated with chronic infections. Monocytes can also function in circulating blood to phagocytize damaged blood cells or microorganisms found in the blood, such as in the case of septicemia. rarely seen in peripheral blood. In all of the common domestic species, basophils make up less than one percent of all white blood cells in peripheral blood. They are not seen at all on many blood smears. culating species. Blood, Lymph, and Immunity Monocytosis. An increased number of monocytes in .,~peripheral blood is called monocytosis. It is often associated with a chronic inflammatory condition, such as an infection. Monocytopenia. A decreased number of monocytes in peripheral blood is called monocytopenia. It can be difficult to evaluate because of the low numbers of monocytes normally found in circulation. - Lymphocytes. Lymphocytes are normally the predominant white blood cell in circulation in ruminants and pigs. They are the only white blood cell that has no phagocytic capabilities. Most of the lymphocytes in the body actually live in what are called lymphoid tissues and constantly recirculate between these tissues and blood. Formation and function. Some controversy still exists as to the origin and development of lymphocytes. It is most popularly believed that they arise from the same pluripotent stem cells in the bone marrow as other blood cells. Before they begin to mature, some of the cells leave the bone marrow to develop in other central lymphoid organs located throughout the body before settling in their permanent home in peripheral lymphoid tissue. Types of Lymphocytes. There are three different types of lymphocytes: T lymphocytes, B lymphocytes, and natural killer cells. T lymphocytes (T cells). T lymphocytes are processed in the thymus before going to peripheral lymphoid tissue. The preT cells in the thymus are thymocytes. Thymocytes multiply rapidly, leave the thymus, and travel to specific T -dependent zones in lymph nodes and the spleen. After they leave the thymus, thymocytes are known as T cells or T lymphocytes. T cells are responsible for cell-mediated immunity and for activating B cells. Most of the lymphocytes in peripheral blood are T cells. 238 Chapter 9 Blood, Lymph, and Immunity found in any tissue in the body, but are most numerous in tissues engaged in antibody formation (e.g., lymph nodes, spleen). Plasma cells are rarely found in peripheral blood. ~D\) VWV o Antigen o Epitope o Antibody Figure 9-7 Antigens and antibodies. Every antigen has a uniquely shaped epitope on its cell membrane that will fit into a combining shape on an antibody. (Modified from the National Cancer Institute, NIH Publication No, 03-5423, September 2003.) Natural killer cells. Natural killer (NK) lymphocytes are neither T cells nor B cells. They don't have to be activated by a specific antigen, and they have the ability to kill some types of tumor cells and cells infected with various viruses. NK cells must come in direct contact with these cells before they can destroy them. Every lymphocyte has surface markers that differentiate B cells from T cells and subsets of each type of lymphocyte. These markers are not visible under light microscopy. We'll discuss the function of lymphocytes in more detail in the immunity section of this chapter. Characteristics. The lymphocytes we see in circulation are '(., classified as either large or small. Large lymphocytes have more cytoplasm and are thought to be younger than small lymphocytes, They gradually develop into small lymphocytes that have very little cytoplasm. B lymphocytes (B cells). The B means "bursa equivalent" Lymphocytes contain no granules in their cytoplasm. The and refers to bone marrow and other lymphoid tissue nucleus is round or oval and does not segment. Large lymthought to be the equivalent of a bird organ called the bursa phocytes have abundant sky-blue cytoplasm. Small lymphoof Fabricius. Inactive B cells travel through lymph nodes, the cytes have such a scant amount of cytoplasm that it is spleen, and other lymphoid structures but rarely circulate , sometimes difficult to see. Small lymphocytes frequently in peripheral blood. B cells are ultimately responsible for look like nuclei without cytoplasm. Or there may be just a antibody production. small amount of sky-blue cytoplasm visible on one side of Each B cell is preprogrammed to produce only one spe-the nucleus. cific antibody type against one specific antigen (foreign protein). On its cell surface, it has thousands of receptors Memory Cells. Both T cells and B cells can become shaped to fit only one antigen shape. Every antigen has a memory cells. These cells are clones of an originallymphounique shape on its cell surface made up of amino acids. This cyte. They don't participate in an initial immune response area is called the epitope. The sequence of amino acids to a specific antigen but survive in lymphoid tissue waiting determines the shape of the epitope. And there is a B cell for a second exposure to that same antigen. When the animal that has a complementary combining site or receptor that is exposed to the antigen for a second time, the memory fits the shape of the epitope (Figure 9-7). cells are ready to respond. This response is much quicker When the B cell and antigen are joined, an antigenantibody complex is formed. For example, there are certain and mounts a greater response than the initial immune B cells that are preprogrammed to receive only the canine response. distemper virus. If a dog is exposed to the distemper virus, Lymphocytosis and Leukocytosis. Lymphocytosis is an only the B cells that are preprogrammed to recognize the virus will respond by eventually making antibodies against increased number oflymphocytes in peripheral blood. It can the virus. All the other B cells will be unaffected. The amazing be the result of leukemia (a form of cancer of the lymphocytes), chronic infections, or epinephrine release (as part of thing is that the B cells are preprogrammed to produce antibodies against antigens to which they have never been the fight-or-flight response). Lymphocytosis can be signifiexposed. When B cells recognize an antigen, they transform cant enough to cause leukocytosis. into plasma cells that release antibodies. The human body can produce over 100 trillion (102°) antibodies, and there is Lymphopenia and Leukopenia. Lymphopenia is a no reason to think an animal can't do the same. This is called decreased number oflymphocytes in peripheral blood. It can humoral immunity. be the result of many factors, including decreased producPlasma cells are derived from B cells in response to an tion of lymphocytes, the presence of corticosteroids (drugs antigenic stimulus. The B cells that are activated by their similar to glucocorticoid hormones from the adrenal cortex), antigen multiply by mitosis in a process called blastic transimmune deficiency diseases, and acute viral diseases. In formation to become plasma cells. some animals, especially ruminants, in which lymphocytes Plasma cells produce, store, and release antibodies that are the primary white blood cell in circulation, lymphocytoare also known as immunoglobins. Plasma cells can be penia can result in leukocytopenia.