* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Epidemiology of Psychoses
Major depressive disorder wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
Alcohol withdrawal syndrome wikipedia , lookup
Child psychopathology wikipedia , lookup
Rumination syndrome wikipedia , lookup
Substance dependence wikipedia , lookup
Autism spectrum wikipedia , lookup
Excoriation disorder wikipedia , lookup
Political abuse of psychiatry wikipedia , lookup
Panic disorder wikipedia , lookup
Abnormal psychology wikipedia , lookup
Dementia with Lewy bodies wikipedia , lookup
Bipolar II disorder wikipedia , lookup
History of psychiatry wikipedia , lookup
Mental disorder wikipedia , lookup
History of mental disorders wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Bipolar disorder wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Depersonalization disorder wikipedia , lookup
Dementia praecox wikipedia , lookup
Conduct disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Substance use disorder wikipedia , lookup
Asperger syndrome wikipedia , lookup
Factitious disorder imposed on another wikipedia , lookup
Spectrum disorder wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Conversion disorder wikipedia , lookup
Mental status examination wikipedia , lookup
Antipsychotic wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Sluggish schizophrenia wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Schizophrenia wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
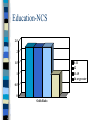
Psychosis and Schizophrenia: Differential Diagnosis William R. Yates, M.D. Professor of Research OU College of Medicine, Tulsa Laureate Research Center Brain Cortex in Schizophrenia QuickTime™ and a TIFF (Uncompressed) decompressor are needed to see this picture. Psychotic Disorders-Overview Common signs & symptoms Case vignettes Differential Diagnosis Medications and psychotic symptoms Management principles Psychopharmacologic overview Objectives Describe the common symptoms of psychosis List the key differential diagnoses for psychotic symptoms Describe the criteria for schizophrenia Outline a treatment plan for management of acute and chronic psychotic disorders Psychiatric exam-simplified Cognitive impairment? Psychotic symptoms/disorder? Mood disorder? Anxiety disorder? Substance use disorder? Differential Diagnosis: Psychosis Psychosis due to medical disorder? Psychosis due to medication? Psychosis due to drug/alcohol intoxication or withdrawal? Psychotic depression or mania? Psychosis of schizophrenia? Delusional disorder? Case Vignette #1 BT was recently admitted for fever, bloody diarrhea and following colonoscopy diagnosed with inflammatory bowel disease. He was admitted, placed on IV antibiotics and high dose corticosteroids. His medical condition improved and he was discharged. However, soon after returning home, his wife calls in the middle of the night. She found her husband up wandering around. He appears confused, agitated and reports he hears the voice of God telling him to prepare to become the next Messiah. His wife asks what she should do. Case Vignette #2 BF is a 72 year old women who lives alone. Her daughter brings her in for evaluation after she is noted to be more disorganized and agitated. She has told her daughter that her purse and money have been stolen. She also reports seeing small miniature men sneaking into her apartment and taking her things during the evening. Case Vignette #3 You are asked to evaluate a 40 year old man admitted to the hospital for fever and abdominal pain. He resides in a nursing home and has had several weeks of LLQ pain and a 20 pound weight loss. He has required residential care since age 22 due to a mental disorder. He refuses to have any blood drawn or other other diagnostic procedures. He states he feels his doctors are conspiring to kill him and inject him with the AIDS virus. A surgeon recommends surgical exploration for his clinical presentation and asks you to proceed with what is necessary to accomplish this. Common signs & symptoms Disturbances of perception & cognition – hallucinations: auditory, visual, tactile, olfactory, gustatory – delusions: paranoid, somatic, grandiose, religious, nihilisitic – First rank delusions: thought broadcasting, withdrawal, thought insertion, passivity – thought disorder: derailment, blocking, tangentiality, perseveration Common signs & symptoms II Disturbances of behavior and motor fx – psychomotor agitation or retardation – aggressive verbal or motor behavior – catatonia: immobility, mutism, waxy flexibility, posturing, sterotypy – bizarre behavior/social deterioration – avolition: lack of goal directed activity Disturbances of affect: flat/ anhedonia National Comorbidity Survey One or more psychosis screening questions endorsed by 28.4% (CIDI) Lifetime prevalence rates for narrowly defined psychotic illness 1.3% Lifetime prevalence rates for more broadly defined psychotic illness 2.2% National Comorbidity Survey Clinicians then reviewed the positive screened cases using CIDI interview and interviewed patients/reviewed records Lifetime prevalence rates for narrowly defined schizophrenia 0.2% Lifetime prevalence for more broadly defined schizophrenia was 0.7% Workup for new-onset psychosis History and physical Psychiatric evaluation General medical evaluation: chemistry panel, ABGs, CBC, thyroid function, HIV, Lumbar puncture, EEG Urine drug screen Brain imaging: CT/ MRI Medical Causes for Psychosis Delirium with psychotic features: – – – – – – – – – – – I nfectious W ithdrawal A cute metabolic T rauma C NS pathology H ypoxia D eficiencies E ndocrinopathy A cute Vascular T oxins H eavy metals encephalitis alcohol acidosis, hepatic failure head trauma stroke, vasculitis pulmonary embolus vitamin hypoglycemia hypertensive encephalopathy medications, pesticides, solvents lead, mercury Psychosis in Dementia Psychotic symptoms common in Alzheimers and other dementias May involve perceptual disturbances and interact with memory impairment Often accompanied by agitation, wandering, aggression Can significant contribute to functional deterioration Substance-induced psychosis Stimulants: Cocaine/Amphetamines – Often with paranoid delusions – Can also include auditory and tactile hallucinations Hallucinogens: LSD/PCP/Psilocybin Alcohol Withdrawl – Often includes visual hallucinations Medication-induced psychosis Paranoid and other delusions: – acyclovir, cephalosporins, cimetidine, corticosteroids, dopamine agonists (levodopa), theophylline Hallucinations – anticholinergics, calcium channel blockers, cimetidine, dopamine agonists, indomethacin, phenytoin Psychosis due to mood disorder Depression – may include hallucinations and delusions – delusions tend to match the mood state: I.e having committed terrible sin, being worthless and doomed to hell or death Mania – may include hallucinations and delusions – delusions tend to be grandiose, religious, and bizarre: I.e. becoming a famous person or religious person Primary psychotic disorders Schizophrenia: chronic hallucinations or delusions lasting 6 months, lifetime prevalence of about 1%, variable course but often progressive and disabling Schizophreniform disorder: like schizophrenia but less than 6 months Schizoaffective disorder: major mood disorder plus psychosis during periods of remission from mood symptoms Non-affective Psychoses: Definitions Schizophrenia Schizophreniform disorder Delusional disorder Atypical Psychosis Diagnosis: Schizophrenia A. Two or more of following x 1 month – delusions hallucination – disorganized speech negative sx – disorganized or catatonic behavior B. Social/Occupational Dysfunction C. Duration of A/B at least 6 months D. R/O schizoaffective, psychotic mood, substance abuse, gen medical cond. Prevalence Rates-Schizophrenia Article Criteria – Eaton pre-DSM – Eaton (2) pre-DSM – Levav SAD/RDC 6 mo – Kessler – 1. (NCS) SCID/DSM-IIIR – non-affective psychoses rate Rate/100 2.7 3.7 0.7 0.1 0.7 Prevalence Rates-Schizophrenia Environmental Catchment Area Study – Diagnostic Interview Schedule(DIS) – Lay interviewer measure – Only 20% agreement with psychiatric evaluation – ECA not a suitable source of information to estimate the prevalence of schizophrenia Prevalence Rates Schizophrenia Assuming most accurate survey in the NCS the in Tulsa SMA (750,000) Estimates of number of patients with schizophrenia would range from 750 to 5000 Community centers where services provided tend to increase prevalence rates Risk Factors-Schizophrenia Social Class Gender and Age Marital Status Season of Birth Pregnancy & Birth Complications Substance Abuse Genetic Factors Social Class Low social class increases risk Hypotheses – Environmental factors associated with low SES cause schizophrenia – Selection-drift hypothesis-failure to attain social rank or downward drift Several studies support selection-drift hypothesis Social Class-ECA 9 8 7 6 5 High 2 3 Low 4 3 2 1 0 Odds Ratio Education-NCS 2.5 2 0-11 12 13-15 16 or greater 1.5 1 0.5 0 Odds Ratio Gender and Age Very similar gender rates Some evidence male predominance – males may have higher severity – seek admission and treatment earlier Some support for higher rates of men in younger populations (under 35 years) and higher rates for women in older populations Marital Status Risk ratio for nonmarried vs married individuals ranges from 2.6 to 7.2 Women are more likely to be married than men (30 % vs 10%) Some of this may be due to later onset or milder forms of the illness in women compared to men ECA-Marital Status 3 2.5 2 Married Single Divorced Widowed 1.5 1 0.5 0 Odds ratio Risk Factors: Season of Birth A number of studies have reported that the proportion of patients with schizophrenia born during winter is 5 to 15 % greater than expected Higher proportion in those without a family history of schizophrnenia Has not been linked to specific viral infections Pregnancy & Birth Complication Studies inconsistent looking at a variety of PBCs (I.e. bleeding, low APGARs) PBCs are associated with abnormal brain structure by MRI PBCs may be potentiator of risk in those with genetic predispositon to schiz PBCs may be indicator of fetal viral inf PBCs occur more commonly in low SES ECA Substance Abuse Comorbidity 35 30 25 Alcohol Dep Alc Abuse/Dep Drug Dep Drug Abuse/Dep 20 15 10 5 0 Rate % Substance Abuse Large Swedish study showed cannabis use (more than 15 x) increased risk of schizophrenia 6 x Cannabis associated psychosis associated with FH schizophrenia Also some interest in LSD and other hallucinogens role in initiation Definition: Delusional Disorder A. Nonbizarre delusions of 1 month B. Criterion A for schizophrenia not met C. Function not markedly impaired D. No prominent mood disorder E. Not due to substance or GMC Subtypes: erotomanic, grandiose, jealous, persecutory, somatic, mixed Course & Prognosis Community sample groups often have better prognosis than those collected in hospital samples Still overall high rates of chronicity Worse than affective psychoses Poor Prognosis Male Unmarried Family history of schizophrenia Long duration of symptoms before RX Few positive sx/Many negative sx Noncompliance Substance abuse comorbidity Case Vignette #1 BT was recently admitted for fever, bloody diarrhea and following colonoscopy diagnosed with inflammatory bowel disease. He was admitted, placed on IV antibiotics and high dose corticosteroids. His medical condition improved and he was discharged. However, soon after returning home, his wife calls in the middle of the night. She found her husband up wandering around. He appears confused, agitated and reports he hears the voice of God telling him to prepare to become the next Messiah. His wife asks what she should do. Case Vignette #2 BF is a 72 year old women who lives alone. Her daughter brings her in for evaluation after she is noted to be more disorganized and agitated. She has told her daughter that her purse and money have been stolen. She also reports seeing small miniature men sneaking into her apartment and taking her things during the evening. Case Vignette #3 You are asked to evaluate a 40 year old man admitted to the hospital for fever and abdominal pain. He resides in a nursing home and has had several weeks of LLQ pain and a 20 pound weight loss. He has required residential care since age 22 due to a mental disorder. He refuses to have any blood drawn or other other diagnostic procedures. He states he feels his doctors are conspiring to kill him and inject him with the AIDS virus. A surgeon recommends surgical exploration for his clinical presentation and asks you to proceed with what is necessary to accomplish this. Typical Antipsychotics Phenothiazines (aliphatic) – chlorpromazine (Thorazine) Phenothiazines (piperidine) – thioridizine (Mellaril) Phenothiazines (piperazine) – fluphenazine (Prolixin) Butyrophenone-haloperidol (Haldol) Thioxanthene-thiothixene (Navane) Atypical Antipsychotics Clozapine (Clozaril) Olanzapine (Zyprexa) Risperidone (Risperdal) Quetiapine (Seroquel) Ziprasidone (Geodon) Aripiprazole (Abilify) Paliperidone (Invega) Psychosis: Acute Management Haloperidol 2 to 5 mg IM q 30 minutes until agitation/psychosis is controlled Can alternate with lorazepam 1 to 2 mg IM or IV for a synergistic sedative effect Haloperidol has been administered IV for rapid control, however this is not approved by FDA and probably best done with cardiac monitoring Psychosis: Chronic management Typical antipsychotics: chlorpromazine, fluphenazine, haloperidol--all have significant rates of dystonic reactions, Parkinsonian symptoms & tardive dyskinesia Haloperidol/Prolixin decanoate forms Atypical agents: Clozapine, olanzapine, risperidone, quetiapine & ziprasidone, palliperidone