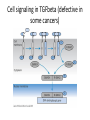
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cancer Genetics
History of genetic engineering wikipedia , lookup
Site-specific recombinase technology wikipedia , lookup
Designer baby wikipedia , lookup
Cancer epigenetics wikipedia , lookup
Genome (book) wikipedia , lookup
Point mutation wikipedia , lookup
Vectors in gene therapy wikipedia , lookup
Polycomb Group Proteins and Cancer wikipedia , lookup
Mir-92 microRNA precursor family wikipedia , lookup
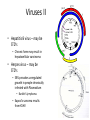
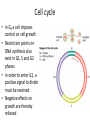
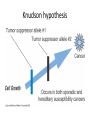
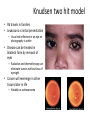
Cancer Genetics Cancer • Disease characterized by uncontrolled cell growth – This causes tumors • Tumors may be benign or malignant • Benign tumors grow in size but do not invade and destroy surrounding tissue – These may still be deadly – Laryngeal papillomas for example can occlude the airway and cause asphyxiation • Cancer usually means malignant – Malignancy means a cell is invasive – Invasion destroys • The internal cellular order of a tissue • Membranes and barriers that define organs Malignancy • Invasion is prerequisite to malignancy – Malignancy defined as the tendency to become worse, or to progress in virulence – Cells which are invasive tend to spread • This is metastasis • However an invasive tumor is not automatically metastatic – Metastatic cells may migrate to other sites within the same organ – Cells or groups of cells may travel through the vasculature or reticuloendothelial system to distant sites • Initial mutation (initiation) alters genes resulting in growth • Progressive growth (influenced by tumor promoters) creates more cells, each with a certain probability of mutating to more virulent state – Rapidly growing cells more prone to mutation than quiescent cells – Mutations may occur in DNA repair enzymes making other mutations more likely – Mutations may also lead to genomic instability, fragmenting the genome • Each break means another mutation • Mutant cells arise within the population of growing cells that are able to break through into surrounding tissues The steps in invasion Effects of mutations • Up regulation of positive signals for growth • Down regulation of negative signals that suppress growth • Elimination of signals that might stimulate immunological attack or apoptosis (programmed cell death) • Interference with the normal process of cell-cell binding • Production of proteins that result in degradation of surrounding tissues Tumor cell properties which may change during tumor progression • • • • • • antigenicity growth rate response to hormones response to cytotoxic drugs karyotypic abnormalities capacity for invasion and metastasis Germline versus somatic mutations that result in cancer • Germline – Mutations in certain genes • The mutation must not be so severe that it results in fetal death – Heritable • Variable penetrance depending on mutation • Somatic – Wider array of target genes • Mutations that wouldn’t be tolerated during development can occur in somatic cells – Sporadic appearance – Non-heritable Environmental factors • Experimentation and epidemiology indicate that cancer is caused by mutagens • Most mutagens are carcinogens and most carcinogens are mutagens – Exceptions include tumor promoters such as TPA – This stimulates cell division without mutagenizing • Identification of any particular agent is difficult Unidentified environmental influences • Japanese colon cancer rates rise and stomach cancer rates fall when Japanese move to America – Stomach cancer • Helicobacter pylori? • Stress? – Colon cancer? • Lifestyle – sedentary in US • Environmental exposures? • Overall risk dependent on both exposure and genetic predisposition Carcinogens • Mutagens = carcinogens generally • Works against specific genetic background • Two step experimental induction of cancer – Initiation = mutagenesis – Promotion = mitogenesis • Common carcinogens act as both initiators and promoters – Polycyclic aromatic hydrocarbons – cigarette smoke; soot; tobacco – Alkylating agents – mustard gas – Industrial agents – benzene; vinyl chloride; asbestos – Metals – arsenic – Drugs – cyclophosophamide; DES – Food additives – Nitrosamines – Natural substances – Aflatoxin B1 • Promoters – Are not mutagens but provoke cell division by activating positive growth signals – TPA (PMA) Carcinogens (and UV, ionizing radiation, …) • These are an uncommon cause of cancer – HTLV I and II – STD’s • Retroviruses found in patients leukemia – HTLV I Adult T-Cell leukemia/lymphoma – HTLV II Hairy Cell leukemia • Infection only rarely results in disease • Rare forms of leukemia • These are integrative viruses – It’s genome inserts into chromosomal DNA as a necessary step in viral replication – The integration site is therefore mutated – Promoters on the virus can up-regulate transcription from proximal host genes Human tumor viruses Viruses II • Hepatitis B virus – may be STD’s – Chronic form may result in hepatocellular carcinoma • Herpes virus – may be STD’s – EBV provokes unregulated growth in people chronically infected with Plasmodium • Burkitt’s lymphoma – Kaposi’s sarcoma results from KSHV • HPV 16 and 18 – STD’s – Cervical cancer • Unregulated expression of oncogenes E6 and E7 provoke tumors • De-regulation is a result of integration of the virus such that molecules that regulate expression of E6 and E7 are destroyed – Other HPV • Eg HPV-1 common warts; HPV-11 laryngeal warts • Exist as episomes – not integrated • Benign tumors (warts) that may regress or be recurrent • Almost never progress to malignancy Human papillomavirus Types of Cancer • Epithelial tissue – Carcinoma • Most common form of solid tumor in humans • Stem or basal cells are mutated • Not as common among animals • Connective tissue – Sarcoma • These are more common in animals and are often virally caused in them • Others named for the cell type of origin – Glial cells – glioma – Melanocytes – melanoma – Neuroblastoma (from sympathetic nervous tissue – most common in children), etc. Leukemia • Abnormal proliferation and development of hematopoietic cells in bone marrow and blood – This results in the expansion of cells that circulate in the vasculature – Often in the form of blast cells, or undifferentiated cells of hematopoietic origin – Classification • Acute or chronic • Lymphogenous or myelogenous – Suffixes -cytic verus -blastic refers to the maturity of the proliferating cell – A blast is a more immature form of a cell • Leukemic or aleukemic – Aleukemic means there is no abnormal increase of cells in the blood Lymphoma • Cancer of the lymphoid tissue – Usually malignant – Named according to the predominant cell type within the tumor or the discoverer • Burkitt’s lymphoma – A B-cell proliferation confined to the lymphoid tissues – Also properly described as a "B-Cell lymphoma" Types of cancer genes Cancer Gene type Transmission, effect How discovered Cell types involved Oncogenes Dominant, positive acting (gain of function) Retroviral Somatic, origins, sometimes transfection germline Tumor Dominant or Suppressor recessive, negative genes acting (loss of function) Pedigrees mainly Somatic and germline Cancer is a genetic disease • Cell division accomplishes replacement of dead or sloughed cells – Most cells are programmed to die as a result of normal terminal differentiation • Apoptosis • Sloughing • Genes affecting growth control may either turn cell division off or turn it on – Germline mutations may result in predisposition • Often are Tumor suppressor genes – These are negative controls on cell growth » Restrict cell division » Provoke apoptosis – Somatic mutations may result in uncontrolled growth • Oncogenes – These are positive signals to grow or inhibitory signals against apoptosis – Viral oncogenes interact with cellular cancer genes Cell cycle • In G0 a cell imposes control on cell growth • Restriction points on DNA synthesis also exist in G1, S and G2 phases • In order to enter G1, a positive signal to divide must be received • Negative effects on growth are thereby relieved Families • How positive signals changed? – Hormone – autocrine loop • Cell overproduces a signal that tells itself to grow – Sis – Platelet Derived Growth Factor beta subunit – Stomach cancer – HST – FGF – Glioma – Growth Factor Receptors • RET – Rearranged during Transfection – Multiple Endocrine Neoplasia (MEN) • Erb B – (First identified in avian erythroblastosis virus) – ERBB1 – EGFR homolog – glioblastoma – but viral oncogene – ERBB2 – (NEU) EGFR family – responsiveness to chemotherapy in breast cancer – amplified in 20-30% breast cancers - over expression confers taxol resistance in breast cancer – B3/B4 – no cancer connections Positive acting Cancer Genes – Growth factor receptors • Cells grow and differentiate under control of external signals • Why would a cell divide? – It receives an external signal – It responds to that signal with division • The signal is a growth factor – E.g. Epidermal Growth Factor • Must have a specific receptor to respond – Epidermal Growth Factor Receptor Nuclear • N-myc – related to v-myc and c-myc • Avian myelocytomatosis virus • DNA binding protein – amplification in neuroblastomas • Myb – related to v-myb • Avian myeloblastosis viral oncogene • DNA binding protein – malignant melanoma, lymphoma, leukemia • Fos – related to v-fos • Finkel murine osteosarcoma • transcription factor of AP-1 complex – Human osteosarcoma DNA repair enzymes • These are not oncogenes per se • They do not participate in cellular proliferative signals • Instead they act to enhance the mutability of the genome • This in turn increases the chances for mutagenesis of cancer genes Family History Flags of Hereditary Cancer • • • • • Cancer in 2 or more relatives Early age of diagnosis Multiple primary tumors Bilateral or multiple rare tumors Existing mutation predisposes to cancer Multistep evolution in cancer Proto-oncogenes • • • • Induce telomerase activity Block apoptosis Stimulate proliferation Increase blood supply Tumor Suppresor Genes • Gatekeepers: regulation of cell cycle; growth inhibition by cell-to-cell contact • Caretakers: Repair DNA damage • Maintain genome integrity Oncogene-caused cancer exemples - Amplification of the same gene as a cause of oncogene-caused cancer (can be diagnosed by FISH) - Chromosomal translocations as a cause of oncogene-caused cancer (Brc/Abl novel fusion gene that confers growth and survival advantage to Chronic Multiple Myeloma is a result of translocation) - Common idea – overexpression or gain-offunction of oncogenes in cancer Hereditary Syndromes of Oncogenes • MEN2 – predisposition to thyroid cancer, GOF germline mutations • Different mutations in RET gene (cell surface receptor tyrosine kinase) • Different outcomes so genetic testing is important Loss of second allele in cancer Knudson hypothesis Hereditary Syndromes of Tumor Suppresor Genes • Retinoblastoma – Rb1 (gate-keeper gene) • Familial Adenomatous Polyposis (FAP) • Hereditary Nonpolyposis Colorectal Cancer Syndrome • Hereditary Breast/Ovarian Cancer Syndrome Knudsen two hit model for Retinoblastoma • Model for heritable cancer • Rb-1 travels in families • Single hit in germline predisposes for Retinoblastoma – results in heterozygosity for all cells • Second hit in Rb necessary to lose cell cycle control – This results in a Loss of Heterozygosity – Specific mechanisms for the second hit Knudsen two hit model • Rb travels in families • Leukocoria is initial presentation – Usual red reflection in an eye on photography is white • Disease can be treated in bilateral form by removal of eyes – Radiation and chemotherapy can eliminate tumors without loss of eyesight • Cancer will reemerge in other tissues later in life – Notably as osteosarcoma Normal Colon and FAP colon Normal function of APC protein Specific FAP phenotypes associated with specific APC mutations • FAP is caused by germline LOF mutations in APC gene Colorectal tumor DNA sample gel electrophoresis with microsatellite instability Cell signaling in TGFbeta (defective in some cancers) Hereditary Breast/Ovarian Cancer • BRCA 1 / 2 genes • Associated with defective DNA repair complex that repairs breaks and cross-links in DNA