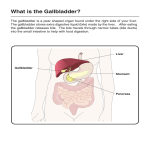
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Liver: Histology
Liver support systems wikipedia , lookup
Hepatocellular carcinoma wikipedia , lookup
Glycogen storage disease type I wikipedia , lookup
Intestine transplantation wikipedia , lookup
Wilson's disease wikipedia , lookup
Cholangiocarcinoma wikipedia , lookup
Hepatic encephalopathy wikipedia , lookup
Ingegneria delle tecnologie per la salute Fondamenti di anatomia e istologia aa. 2016-17 Digestive System (b) Salivary Glands = many small salivary glands housed within mucous membranes of mouth and tongue, constantly secreting saliva, either directly into oral cavity or indirectly through ducts (1-1.5 lts/day): usually just enough saliva is present to moisten mouth and teeth, but increases when eating, because it is essential to moisten food and initiate chemical digestion of carbohydrates Major Salivary Glands =outside oral mucosa 3 pairs of glands, secreting majority of saliva into ducts opening into mouth: • submandibular glands = in floor of mouth, secreting through submandibular ducts. • sublingual glands = below tongue, using lesser sublingual ducts to secrete into oral cavity. • parotid glands = between skin and masseter muscle (near ears), secreting through parotid duct (located near second upper molar tooth). Salivary Glands Salivary Glands Salivary Glands Salivary Glands Salivary Glands Salivary Glands Salivary Glands Saliva = essentially (95.5 %) water + 4.5 % [=complex mixture of ions, glycoproteins, enzymes, growth factors, and waste products] salivary amylase = perhaps most important ingredient in saliva initiating breakdown of carbohydrates (not enough time in mouth to allow all carbohydrates break down, but salivary amylase continues acting until inactivated by stomach acids) Bicarbonate + phosphate ions = chemical buffers, maintaining saliva at a pH 6.35-6.85. Salivary mucus = lubricate food, facilitating movement in mouth, bolus formation, and swallowing. immunoglobulin A + lysozyme = antimicrobial Regulation of Salivation • autonomic nervous system regulates salivation (secretion of saliva): parasympathetic stimulate - sympathetic reduce salivation • chemicals stimulating taste receptors on tongue impulses to sup and inf salivatory nuclei in brain stem parasympathetic impulses through fibers in glossopharyngeal and facial nerves, stimulating salivation Teeth = organs similar to bones used to tear, grind, and otherwise mechanically break down food. Types of Teeth 2 sets of teeth (= dentition): 20 deciduous teeth, or baby teeth, first appearing at about 6 mos of age; between approximately age 6 and 12, replaced by 32 permanent teeth, moving from center of mouth toward side: • 8 incisors, 4 top + 4 bottom • 4 canines • 8 premolars (or bicuspids) • 12 molars Teeth: Anatomy of a Tooth = secured in alveolar processes (sockets) of maxilla and mandible by connective tissue called periodontal ligament gingivae (gums) = soft tissues that line alveolar processes and surround necks of teeth. 2 main parts of a tooth: 1. crown (= portion projecting above gum line, 2. root (embedded in maxilla+mandible), both containing inner pulp cavity with loose connective tissue inside through which run nerves and blood vessels [root canal = pulp cavity that runs through root of tooth]; surrounding pulp cavity is dentin (=bone-like tissue) covered in root by an even harder bone-like layer called cementum and in crown by an outer layer of enamel (hardest substance in body) Teeth Pharynx = (involved in both digestion and respiration, when food enters pharynx, involuntary muscle contractions close off air passageways) short tube of skeletal muscle lined with mucous membrane, running from posterior oral and nasal cavities to opening of esophagus and larynx; 3 subdivisions: sup, nasopharynx, involved only in breathing and speech, other 2 subdivisions, oropharynx and laryngopharynx, used for both breathing and digestion: oropharynx begins inf to nasopharynx and continue below with laryngopharynx, connecting to esophagus, whereas ant portion connects to larynx, allowing air to flow into bronchial tree; histologically, wall of oropharynx is similar to that of oral cavity, with mucosa of stratified squamous epithelium endowing with mucus-producing glands. During swallowing, elevator skeletal muscles of pharynx contract, raising and expanding pharynx to receive bolus of food, then relax and constrictor muscles of pharynx contract, forcing bolus into esophagus and initiating peristalsis, meanwhile soft palate and uvula rise reflexively to close off entrance to nasopharynx and larynx is pulled superiorly with cartilaginous epiglottis folding inferiorly to cover glottis Esophagus = muscular tube connecting pharynx to stomach (running a mainly straight route through mediastinum of thorax, but to enter abdomen penetrates diaphragm through an opening = esophageal hiatus), approximately 25 cm in length, located post to trachea, and remaining collapsed when not engaged in swallowing Esophagus Passage of Food through Esophagus upper esophageal sphincter (continuous with inferior pharyngeal constrictor) = controls movement of food from pharynx into esophagus. upper two-thirds of esophagus = both smooth and skeletal muscle fibers, with the latter fading out in the bottom third of esophagus rhythmic waves of peristalsis, which begin in upper esophagus, propel bolus of food toward stomach, meanwhile, secretions from esophageal mucosa lubricate esophagus and food, that passes from esophagus into stomach at lower esophageal sphincter (also called gastroesophageal or cardiac sphincter), relaxing to let food pass into stomach, then contracting to prevent stomach acids from backing up into esophagus. Esophagus Histology of the Esophagus mucosa with non-keratinized, stratified squamous epithelium, with a layer of basal and parabasal cells, protecting against erosion from food particles + lamina propria containing mucussecreting glands + muscularis layer changing according to location: in upper third muscularis = skeletal muscle, in middle third = skeletal and smooth muscle and in lower third = smooth muscle + adventitia, most superficial layer of esophagus not covered by a fold of visceral peritoneum. Esophagus Esophagus Esophagus Esophagus Esophagus Esophagus Esophagus Digestive functions Stomach [FUNCTION] = temporary holding chamber = meal can be ingested far more quickly than it can be digested and absorbed by small intestine: stomach holds food and parses only small amounts into small intestine at a time; foods not processed in order are eaten, but mixed together with digestive juices in stomach (= chyme), released into small intestine. plays several important roles in chemical digestion, including continued digestion of carbohydrates and initial digestion of proteins and triglycerides little if any nutrient absorption occurs in stomach, with exception of negligible amount of nutrients in alcohol Stomach: structure 4 main regions in stomach: 1. cardia (or cardiac region) = point where esophagus connects to stomach and through which food passes into stomach 2. Fundus = dome-shaped and located inf to diaphragm, above and left of cardia 3. Body = below fundus, main part of stomach 4. Pylorus = funnel-shaped, connecting stomach (pyloric antrum) to duodenum (=narrower end, called pyloric canal, with smooth muscle pyloric sphincter located at latter point of connection and controls stomach emptying) Stomach: structure In absence of food, stomach deflates inward, and mucosa and submucosa fall into a large fold (=ruga). greater curvature = convex lateral surface lesser curvature = concave medial border held in place by lesser omentum (extending from liver to lesser curvature) and greater omentum (running from greater curvature to posterior abdominal wall) Stomach: structure Stomach: histology wall made of same 4 layers as rest of alimentary canal, but with adaptations for unique functions of this organ to: a) Muscularis = in addition to typical circular and longitudinal smooth muscle layers, muscularis has an inner oblique (= in addition to moving food through canal, stomach can vigorously churn food, mechanically breaking it down into smaller particles) Stomach: histology b) mucosa Stomach: histology b) Mucosa = epithelial lining consists only of surface mucus cells, secreting a protective coat of alkaline mucus + vast number of gastric pits dot surface of epithelium, marking entry to each gastric gland, secreting complex digestive fluid referred to as gastric juice; Stomach: histology walls of gastric pits made up primarily of mucus cells, but gastric glands made up of different types of cells: glands of cardia and pylorus = primarily mucus-secreting cells pyloric antrum = mucus and a number of hormones, including majority of stimulatory hormone, gastrin fundus and body = (much larger glands) site of most chemical digestion, producing most of gastric secretions, due to a variety of secretory cells: Stomach: histology Stomach: histology 1. Parietal cells—located primarily in middle region of gastric glands (among the most highly differentiated of the body‘s epithelial cells) producing both hydrochloric acid (HCl, responsible for high acidity [pH 1.5 to 3.5] needed to activate protein-digesting enzyme, pepsin, and also killing much of bacteria ingested with food and helping to denature proteins, making them more available for enzymatic digestion) and intrinsic factor (glycoprotein necessary for absorption of vitamin B12 in small intestine). 2. Chief cells—located primarily in basal regions of gastric glands, secreting pepsinogen (inactive proenzyme form of pepsin, with HCl necessary for its conversion from pepsinogen) 3. Mucous neck cells— (gastric glands in upper part of stomach) secreting thin, acidic mucus that is much different from the mucus secreted by the goblet cells of the surface epithelium (role not currently known) 4. Enteroendocrine cells— secreting various hormones into interstitial fluid of lamina propria (including gastrin released mainly by enteroendocrine G cells) Stomach: histology Stomach: histology Stomach: histology Stomach: histology Stomach: histology Stomach: histology Stomach: histology Small Intestine: generality Chyme released from stomach enters small intestine = primary digestive organ in body. Not only where most digestion occurs, also where practically all absorption occurs. longest part of alimentary canal: about 3 mts long in a living person (twice as long in a cadaver due to loss of muscle tone). smaller diameter of only about 2.5 cm, compared with 7.5 cm for the large intestine. in addition to its length, folds and projections of lining of small intestine work to give it an enormous surface area, which is approximately 200 m2 , more than 100 times surface area of your skin: necessary for complex processes of digestion and absorption Small Intestine: structure coiled tube of small intestine is subdivided into 3 regions: duodenum, jejunum, and ileum Small Intestine: structure Duodenum = shortest region ( 25cm), beginning at pyloric sphincter, bends posteriorly behind peritoneum, becoming retroperitoneal, and then makes a C-shaped curve around the head of pancreas before ascending anteriorly again to return to peritoneal cavity and join jejunum, therefore being subdivided into 4 segments: sup, descending, horizontal, ascending hepatopancreatic ampulla (ampulla of Vater) = located in duodenal wall, marks transition from ant portion of alimentary canal to mid-region, where bile duct (through which bile passes from liver) and main pancreatic duct (through which pancreatic juice passes from pancreas) join, opening into duodenum at a tiny volcanoshaped structure called the major duodenal papilla (where hepatopancreatic sphincter, sphincter of Oddi, regulates flow of bilepancreatic juice from ampulla into duodenum). Small Intestine: structure Small Intestine: structure jejunum = about 1 mt long (in life), [means ―empty‖ in Latin], without clear demarcation between it and ileum. ileum = longest part of small intestine, measuring about 2 mts: thicker, more vascular, more developed mucosal folds than jejunum, joins cecum, at ileocecal sphincter (or valve); both tethered to post abd wall by mesentery; large intestine frames these 3 parts of SI. Parasympathetic nerve fibers from vagus nerve and sympathetic nerve fibers from thoracic splanchnic nerve = extrinsic innervation to small intestine sup mesenteric artery = main arterial supply veins running parallel to arteries, drain into sup mesenteric vein = nutrient-rich blood from small intestine is then carried to liver via hepatic portal vein. Small Intestine: Histology wall composed of same 4 layers typically present in alimentary system, but 3 features of mucosa and submucosa are unique, increasing absorptive surface area more than 600-fold, include circular folds, villi, and microvilli (these adaptations most abundant in proximal 2/3 of SI, where majority of absorption occurs) (a) The absorptive surface of the small intestine is vastly enlarged by the presence of circular folds, villi, and microvilli. (b) Micrograph of the circular folds. (c) Micrograph of the villi. (d) Electron micrograph of the microvilli. Small Intestine: Histology Circular folds = (also called plica circulare), deep ridge in mucosa and submucosa, beginning near proximal part of duodenum and ending near middle of ileum, facilitating absorption, because their shape causes chyme to spiral, rather than move in a straight line, through SI, slowing movement of chyme and providing time needed for nutrients to be fully absorbed. Villi = within circular folds, small (0.5–1 mm long) hairlike vascularized projections called villi (singular = villus), giving mucosa a furry texture, being about 20 to 40 villi mm2, increasing surface area tremendously; mucosal epithelium, primarily composed of absorptive cells, covering villi, that (in addition to muscle and connective tissue to support its structure) contains a capillary bed composed of 1 arteriole and 1 venule, as well as a lymphatic capillary called lacteal: breakdown products of carbohydrates and proteins (sugars and amino acids) enter bloodstream directly, but lipid breakdown products absorbed by lacteals and transported to bloodstream via lymphatic system. Microvilli = much smaller (1 µm) than villi, being cylindrical apical surface extensions of plasma membrane of mucosa‘s epithelial cells, supported by microfilaments, combined microscopic appearance suggests a mass of bristles (brush border), containing at surface enzymes that finish digesting carbohydrates and proteins, estimating 200 million microvilli per mm2, greatly expanding surface area of the plasma membrane and thus greatly enhancing absorption. Small Intestine: Histology Intestinal Glands = mucosa between villi is dotted with deep crevices that each lead into a tubular intestinal gland (crypt of Lieberkühn), formed by cells lining crevices, producing intestinal juice, a slightly alkaline (pH 7.4 to 7.8) mixture of water and mucus (daily about 1-2 lts secreted in response to distention of small intestine or irritating effects of chyme on intestinal mucosa). duodenal glands (Brunner’s glands) = submucosa of duodenum, only site of complex mucus-secreting, producing a bicarbonate-rich alkaline mucus buffering acidic chyme as it enters from stomach. roles of cells in small intestinal mucosa: Small Intestine: Histology Intestinal MALT = lamina propria of small intestine mucosa is studded with quite a bit of MALT: in addition to solitary lymphatic nodules, aggregations of intestinal MALT (= typically referred to as Peyer’s patches, concentrated in distal ileum, most prominent in young people and becoming less distinct in elders, coinciding with general activity of our immune system) serving to keep bacteria from entering bloodstream. Small Intestine (and Large Intestine…): Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Small Intestine: Histology Large Intestine = terminal part of alimentary canal, with function: finish absorption of nutrients and water, synthesize certain vitamins, form feces, eliminate feces running from appendix to anus, and framing small intestine on 3 sides small intestine (large = more than twice of small intestine, about 3 inches) Subdivisions = 4 main regions: cecum, colon, rectum, anus (ileocecal valve = located at opening between ileum and large intestine, controling flow of chyme) CECUM = sac-like structure, suspended inferior to ileocecal valve, about 6 cm long, receiving contents of ileum, and continuing absorption of water and salts (VERMIFORM APPENDIX = winding tube attached to cecum, 8-cm long containing lymphoid tissue, suggesting an immunologic function, generally considered vestigial, but postulated a survival advantage in diarrheal illness, where may serve as bacterial reservoir to repopulate enteric bacteria for those surviving the initial phases of illness; mesoappendix = mesentery of appendix, tethering to mesentery of ileum) COLON = follows cecum: ascending colon, right colic flexure (hepatic flexure), transverse colon (with last third of this begins region defined as hindgut), left colic flexure (splenic flexure), descending colon, sigmoid colon (=entering pelvis inf, s-shaped, extending medially to midline ); ascending and descending colon, and rectum located retroperitoneally, meanwhile transverse and sigmoid colon tethered to post abd wall by mesocolon Large Intestine Large Intestine Foregut, midgut, hindgut… Large Intestine Rectum = in pelvis, near third sacral vertebra, final 20 cm of alimentary canal, extending ant to sacrum and coccyx, with 3 lateral bends creating a trio of internal transverse folds called rectal valves (helping separate feces from gas to prevent simultaneous passage of feces and gas). Anal Canal = located in perineum, completely outside of abdominopelvic cavity, 4–5 cm long, opening to exterior at anus (2 sphincters: internal anal sphincter made of smooth muscle, with involuntary contractions and external anal sphincter made of skeletal muscle, under voluntary control) Large Intestine 3 features unique to large intestine: 1. Teniae coli = three bands of smooth muscle that make up longitudinal muscle layer of muscularis of large intestine, except at its terminal end (tonic contractions bunch up colon into a succession of pouches = 2. Haustra (singular = hostrum) = responsible for wrinkled appearance of colon 3. epiploic appendages = small, fat-filled sacs of visceral peritoneum, attached to teniae coli, purpose unknown. Although rectum and anal canal have neither teniae coli nor haustra, they do have well-developed layers of muscularis that create the strong contractions needed for defecation. Large Intestine: Histology several notable differences between walls of large and small intestines: few enzyme-secreting cells found in large intestine, and no circular folds or villi. other than in anal canal, mucosa of colon is simple columnar epithelium made mostly of enterocytes (absorptive cells) and goblet cells. wall of large intestine far more intestinal glands, containing a vast population of enterocytes (absorbing water and salts as well as vitamins produced by intestinal bacteria) and goblet cells (secreting mucus, easing movement of feces, protecting intestine from effects of acids and gases produced by enteric bacteria). Large Intestine: Histology Large Intestine: Histology Large Intestine: Histology Large Intestine: Histology Large Intestine: Histology Large Intestine: Histology 2. Accessory Organs in Digestion Chemical digestion in small intestine relies on activities of 3 accessory digestive organs: 1. liver = to produce bile and export it to duodenum. 2. gallbladder = primarily stores, concentrates, and releases bile. 3. pancreas = produces pancreatic juice, which contains digestive enzymes and bicarbonate ions, and delivers it to duodenum. Liver = largest gland in body, weighing about 1,5 kg in an adult, also one of most important, being an accessory digestive organ and playing number of roles in metabolism and regulation. lies inf to diaphragm in right upper quadrant of abd cavity, receiving protection from surrounding ribs. divided in 2 primary lobes (large right + much smaller left), in right lobe, some anatomists also identify inf quadrate + post caudate lobe, defined by internal features connected to abd wall and diaphragm by 5 peritoneal folds referred to as ligaments: 1. falciform ligament, 2. ligamentum teres hepatis (both actually remnants of umbilical vein, separating right and left lobes anteriorly), 3-4. lateral ligaments, and 5 coronary ligament. + lesser omentum tethers liver to lesser curvature of stomach. Liver human liver is divided by the falciform ligament into an anatomical right lobe and left lobe. also has a functional right and left side, divided by Cantlie's line: a hypothetical line from the gallbladder fossa to the middle hepatic vein. Each functional hemi-liver is composed of 2 sections: on right, an ant section (segments 5 + 8) and a post section (segments 6 + 7) separated by right hepatic vein; and on left, a lat section (segments 2 + 3) and a medial section (segment 4) separated by left hepatic vein and the falciform ligament (not shown). Each segment can be individually resected. Black dashed lines show demarcations between sections. Liver Liver Liver Diaphragmatic surface 1 - coronary ligament of liver; 2 - aperture; 3 - triangular ligament of the liver; 4 - sickle ligament of the liver; 5 - the right lobe of the liver; 6 - Left lobe of the liver; 7 - Round ligament of liver; 8 - a sharp lower edge; 9 - gall bladder Liver Lower surface 1 - Left lobe of the liver; 2 - the triangular ligament of the liver; 3 - Rear (tailed) fraction of the liver; 4 - adrenal indentation; 5 - kidney indentation; 6 - proper hepatic artery; 7 - Vienna gate; 8 - the common bile duct; 9 - common hepatic duct; 10 - cystic duct; 11 - the right lobe of the liver; 12 - duodenal-intestinal indentation; 13 - Round ligament of liver; 14 - colon-intestinal indentation; 15 - Front (square) share; 16 - gall bladder Liver Liver: biliary tree Liver • • • porta hepatis = (―gate to the liver‖) where hepatic artery and hepatic portal vein enter liver (running along with common hepatic duct behind lateral border of lesser omentum on way to their destinations) hepatic artery delivers oxygenated blood from heart to liver, hepatic portal vein delivers partially deoxygenated blood containing nutrients (+ drugs and toxins) absorbed from the SI and actually supplies more oxygen to liver than do much smaller hepatic arteries; after processing bloodborne nutrients and toxins, liver releases nutrients needed by other cells back into the blood, which drains into central vein and then through hepatic vein to inferior vena cava. hepatic portal circulation = all blood from alimentary canal passes through liver (explaining liver most common site for alimentary canal cancers metastasis) Liver: Histology = 3 main components: 1. hepatocytes [liver‘s main cell type, accounting for around 80% of liver's volume, playing a role in a wide variety of secretory, metabolic, and endocrine functions; plates of hepatocytes called hepatic laminae radiate outward from portal vein in each hepatic lobule] = from their central position, hepatocytes process nutrients, toxins, and waste materials carried by blood: materials such as bilirubin processed and excreted into bile canaliculi, other materials including proteins, lipids, and carbohydrates processed and secreted into sinusoids or just stored in cells until needed 2. bile canaliculi [grooves in cell membranes between adjacent hepatocytes accumulating bile produced by hepatocytes: from here, bile flows first into bile ductules and then into bile ducts, uniting to form larger right and left hepatic ducts, which themselves merge and exit liver as common hepatic duct, that joins with cystic duct from gallbladder, forming common bile duct through which bile flows into small intestine] 3. hepatic sinusoids [open, porous blood space formed by fenestrated capillaries from nutrient-rich hepatic portal veins and oxygen-rich hepatic arteries, where hepatocytes are tightly packed around, giving them easy access to the blood] = combine and send blood to a central vein and then through hepatic vein into inf vena cava (this means that blood and bile flow in opposite directions); also contain star-shaped reticuloendothelial cells (Kupffer cells), phagocytes removing dead red and white blood cells, bacteria, and other foreign material that enter sinusoids Liver: Histology Liver: Histology Liver: Histology Liver: Histology portal triad = distinctive arrangement around perimeter of hepatic lobules, consisting of 3 basic structures: a bile duct, a hepatic artery branch, and a hepatic portal vein branch. Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Histology Liver: Bile • lipids are hydrophobic (= do not dissolve in water), before they can be digested in watery environment of SI, large lipid globules must be broken down into smaller lipid globules (= emulsification) • Bile = yellow-brown or yellow-green alkaline solution (pH 7.6 to 8.6) mixture of water, bile salts, bile pigments, phospholipids (such as lecithin), electrolytes, cholesterol, and triglycerides secreted (about lt/day) by liver to accomplish emulsification of lipids in SI. • bile salts and phospholipids = components most critical to emulsification having a nonpolar (hydrophobic) region as well as a polar (hydrophilic) region [hydrophobic region interacts with large lipid molecules, whereas hydrophilic region interacts with watery chyme in intestine: large lipid globules being pulled apart into many tiny lipid fragments of about 1 μm , dramatically increasing surface area available for lipid-digesting enzyme activity] Liver: Bile • • • While most constituents of bile are eliminated in feces, bile salts are reclaimed by enterohepatic circulation: once bile salts reach ileum, they are absorbed and returned to liver in hepatic portal blood; hepatocytes then excrete bile salts into newly formed bile. bilirubin = main bile pigment [waste product produced when spleen removes old or damaged red blood cells from circulation, including proteins, iron, and toxic bilirubin, transported to liver via splenic vein of hepatic portal system]: proteins and iron recycled, whereas bilirubin excreted in bile, accounting for green color of bile, and transformed by intestinal bacteria into stercobilin [=brown pigment giving stool its characteristic color: in some disease states, bile does not enter intestine, resulting in white (‗acholic‘) stool with a high fat content, since virtually no fats are broken down or absorbed] Hepatocytes work non-stop, but bile production increases when fatty chyme enters duodenum and stimulates secretion of gut hormone secretin. Between meals, bile is produced but conserved: valve-like hepatopancreatic ampulla closes, allowing bile to divert to gallbladder, where it is concentrated and stored until next meal. Liver & Pancreas PANCREAS ANATOMY = soft, oblong, glandular organ lying transversely in retroperitoneum behind stomach: head nestled into “c-shaped” curvature of duodenum with body extending to left about 15 cm and ending as a tapering tail in hilum of spleen [curious mix of exocrine (secreting digestive enzymes) and endocrine (releasing hormones into blood) functions] esophagus stomach ductus choledocus pancreas duodenum duct of Santorini duct of Wirsung Pancreas • exocrine part = arises as little grape-like cell clusters, each called an acinus (plural = acini), located at terminal ends of pancreatic ducts, secreting enzyme-rich pancreatic juice into tiny merging ducts that form 2 dominant ducts [larger duct, Wirsung, fuses with common bile duct (carrying bile from liver and gallbladder) just before entering the duodenum via a common opening (hepatopancreatic ampulla)]; smooth muscle sphincter of hepatopancreatic ampulla controls release of pancreatic juice and bile into small intestine; second and smaller pancreatic duct, the accessory duct (duct of Santorini), runs from pancreas directly into duodenum, approximately 1 inch above hepatopancreatic ampulla. Pancreas • Scattered through sea of exocrine acini are small islands of endocrine cells, islets of Langerhans, producing hormones pancreatic polypeptide, insulin, glucagon, and somatostatin PANCREATIC SECRETIONS 1. PROTEASES (70%) Endopeptidases (trypsin, chymotrypsin, elastases) Exopeptidases (carboxypeptidases) trypsinogen trypsin activates all other precursors enterokinase (duct walls) 2. NUCLEASES (DNAase, RNAase) 3. PANCREATIC AMYLASE (hydrolyse starch and glycogen) 4. PANCREATIC LIPASE (triglycerides fatty acids and glycerol) REGULATION OF SECRETION 1. SECRETIN food in stomach release of stomach acid into duodenum release of secretin into blood by duodenal cells secretion of bicarbonate by duct cells alkaline pH (ideal for pancreatic enzymes) 2. PANCREOZYMIN (cholecystokinen) amino acids and fats in intestine release of pancreozymin by intestinal mucosa into blood relase of pancreatic enzymes into the intestine 3. GASTRIN food in stomach gastrin secretion by stomach mucosa 4. AUTONOMIC INNERVATION (vagus nerve) release of pancreatic enzymes into the intestine Pancreas: Histology Pancreas: Histology islet of Langerhans pancreatic acini islet of Langerhans pancreatic lobe BV Pancreas: Histology LARGE SECRETORY DUCT INTERLOBULAR DUCT PANCREATIC SECRETORY DUCTS simple cuboidal epithelium acinus simple columnar epithelium Exocrine Pancreas: Histology pyramidal secretory basal basophilia cell (rough ER) acinus merocrine secretion (exocytosis) zymogen granules centroacinar cells blood vessel condensing vacuoles golgi vesicles intercalated duct rough endoplasmic reticulum nerve interlobular duct zymogen granules golgi apparatus Pancreas: Histology INTERCALARY DUCTS AND CENTROACINAR CELLS intercalary duct centroacinar cell intercalary duct PANCREATIC EXOCRINE SECRETORY CELL zymogen granules centroacinar cell CELL BIOLOGY OF PANCREATIC SECRETION 1. SYNTHESIS 2. SEGREGATION 14 C -leucine + tRNA mRNA for chymotrysinogen 14 C-amino-acyl tRNA ribosomes mRNA ribosomes polypeptide chymotrysinogen RER cisterna 6. DISCHARGE 3. INTRACELLULAR TRANSPORT exocytosis RER transitional elements 5. INTRACELLULAR STORAGE zymogen granules 4. CONCENTRATION golgi apparatus H2O H2O condensing vacuoles golgi vesicles ISLET OF LANGERHANS alpha cell (glucagon) vascular pole (secretion by exocytosis) acinus beta cell beta cell (insulin) fenestrated capillary blood capillary INSULIN- increases membrane permeability to glucose GLUCAGON - promotes glycogenolysis promotes glycogenesis decrease blood glucose levels increases blood glucose levels “ ANTAGONISTIC HORMONES” alpha cell Pancreas: Histology Pancreas: Histology ISLET OF LANGERHANS Pancreas: Histology ISLET OF LANGERHANS - TEM STAINED ALPHA AND BETA CELLS ALPHA CELLS BETA CELLS Pancreas: Histology INTERCALARY DUCTS AND CENTROACINAR CELLS intercalary duct centroacinar cell intercalary duct Pancreas: Histology Gallbladder = 8–10 cm (~3–4 in) long, nested in a shallow area on posterior aspect of right liver lobe , muscular sac storing, concentrating, and, when stimulated, propelling bile into duodenum via common bile duct, divided into 3 regions: 1.fundus = widest portion, tapering medially into 2.body, which in turn narrows to become 3.neck, angling slightly superiorly as it approaches hepatic duct; cystic duct = 1–2 cm (less than 1 in) long, turning inferiorly as it bridges neck and hepatic duct. simple columnar epithelium organized in rugae, similar to those of stomach, absorbing water and ions from bile and concentrating it by up to 10-fold: no submucosa in gallbladder wall and wall‘s middle, muscular coat is made of smooth muscle fibers [when contracting, gallbladder‘s contents ejected through cystic duct and into bile duct] visceral peritoneum reflected from liver capsule holds gallbladder against liver and forms outer coat of the gallbladder. Gallbladder: Histology Liver, Pancreas, and Gallbladder Anatomy-Histology Correlate • The liver and gallbladder play important roles in digestion via the production and storage of bile. The liver is also the major organ for metabolism and detoxification. The pancreas also produces digestive enzymes to break down proteins, sugars, and fats. • The processes described above are the exocrine functions of the liver and gallbladder. But they also have endocrine roles, secreting compounds into the bloodstream. The hepatocytes produce albumin, fibrinogen, and thrombin, for example. The pancreatic islets produce insulin, glucagon, and somatostatin. Liver, Pancreas, and Gallbladder Anatomy-Histology Correlate The liver, gallbladder, and pancreas receive blood supply from the celiac trunk. One main branch is the common hepatic artery, leading to the hepatic artery proper that branches into left and right hepatic arteries to supply the liver. The right hepatic artery gives off the cystic artery to supply the gallbladder. The pancreas is supplied by multiple vessels. The body and tail are supplied by the dorsal, inferior, and great pancreatic arteries, which all branch off the splenic artery (another main branch of the celiac trunk). The head, neck, and uncinate process are supplied by anastomoses of arteries branching off the celiac trunk and sup mesenteric artery. The gastroduodenal artery, from the common hepatic artery, divides into the anterior and posterior superior pancreaticoduodenal arteries. They anastomose with inferior branches of the inferior pancreatico-duodenal artery from the superior mesenteric artery. The same arteries supply the duodenum. Liver, Pancreas, and Gallbladder AnatomyHistology Correlate -The liver has diaphragmatic and visceral surfaces which contact the diaphragm and abdominal viscera, respectively. Note the right triangular, left triangular, and coronary ligaments that attach to the diaphragm. Note also the bare area not covered by peritoneum. Anteriorly, there is a fold of peritoneum connecting the liver to the umbilicus called the falciform ligament, which contains the round ligament or ligamentum teres. It is the remnant of the umbilical vein that brought oxygenated blood from the placenta to the fetus heart. The ligamentum venosum is the remnant of the fetal ductus venosus that shunted blood from the umbilical vein to the inferior vena cava to bypass the liver. In the adult liver, the porta hepatis includes the hepatic arteries from the hepatic artery proper, the hepatic portal vein, and the hepatic and cystic ducts joining to form the common bile duct. - The portal vein brings nutrients and other compounds absorbed by the GI tract to be stored and/or processed. - Anatomical lobes: Note how the inferior vena cava, gallbladder, ligamentum teres, ligamentum venosum, and porta hepatis form an ―H‖ shape on the visceral surface. It divides the liver into 4 anatomical lobes based on outer appearance – the right, left, caudate, and quadrate lobes. - Functional lobes: These are based on the distribution of the hepatic arteries, portal vein, and hepatic bile duct. The inferior vena cava and the gallbladder serve as the dividing line between the functional right and left lobes. Liver, Pancreas, and Gallbladder Anatomy-Histology Correlate - The liver is divided into many hepatic lobules. Inflow to the liver involves hepatic arteries, which bring oxygenated blood to hepatic tissue, and portal veins, which bring nutrients and other compounds absorbed by the GI tract to be processed and/or stored in the liver. Outflow also involves two routes – hepatic veins which drain into the inferior vena cava and the common hepatic duct which joins the cystic duct and empties bile into the duodenum. - Major characteristics of the liver are portal triads (labeled ―portal‖ in bottom left and shown in the middle) and central veins (labeled in bottom left and shown in the right). Red arrows indicate direction of blood flow within blood sinusoids flanking cords of liver cells. - Note the portal triad contains 1) the portal vein, 2) the hepatic artery, and 3) the bile duct. Each has its typical appearance. The central vein is lined with endothelial cells, with perforations into which the sinusoids empty. Liver, Pancreas, and Gallbladder Anatomy-Histology Correlate • The central veins lead to sublobular veins, which reach collecting veins, hepatic veins, and finally the inferior vena cava. The venous outflow of the liver has no regard to the organization of the lobules. • The liver sinusoids are shown in higher magnification in the bottom left. They are dilated, capillary-like vessels lined by fenestrated, discontinuous epithelium (labeled ―e‖). Interspersed among the endothelial cells are Kupffer cells (labeled ―k‖), which are fixed macrophages within the hepatic tissue. They have distinct cytoplasm that may enter the sinusoidal lumen and function like other macrophages within the body. They also break down damaged red blood cell hemoglobin. • In the bottom middle panel, there are many spaces between the hepatocytes and sinusoidal epithelial cells marked by arrowheads. They are referred to the space of Disse where exchange between hepatocytes and blood flow takes place. • Once again, in the bottom right, we review the Kupffer cell, endothelial cell of the liver sinusoid, and the space of Disse. - The liver lobules can be defined in 3 ways: - 1) Classic lobule – centered around the central vein with the portal triads at each corner. Shown below on the left, the classic lobule may not always be hexagonal in shape. - 2) Portal lobule (not shown) – centered on the portal triad, based on bile secretion, and approximately triangular in shape. - As mentioned earlier, the liver has both endocrine and exocrine functions. The various proteins that hepatocytes secrete enter the bloodstream via the liver sinusoids. The liver also secretes bile in the conventional exocrine fashion. - The hepatocytes secrete bile into sealed extracellular spaces called bile canaliculi. The typical ―chicken-wire‖ appearance is more easily visualized with silver stain. - 3) Liver acinus of Rappaport – this is the most functionally important classification. Shown below on the right, the acinus is roughly oval in shape with 2 central veins and 2 portal triads on opposite ends. Based on the blood flow within hepatic tissue, the acinus is divided into 3 zones. Cells in different zones are specialized for different activity. Zone 1 cells, being closest to the portal triads and hence most oxygenated blood, have the most drug-metabolizing enzymatic activity. Following that same reasoning, zone 3 hepatocytes near the central veins are most susceptible to ischemia. - Once again, inflow to the liver involves oxygenated blood via hepatic arteries and absorbed nutrients and compounds from the GI tract via the hepatic portal veins. - All venous drainage from the GI tract and abdominal visceral organs enters the portal system back to the liver. The overall order is as following: arteries → capillaries → veins → portal vein → hepatic sinusoids → veins → vena cava → heart. - In contrast, the caval system is as following: arteries → capillaries → veins → vena cava → heart. Obviously, this is the circulatory system within the rest of the body. - The portal and caval system are not exclusive from each other. There are 4 sites of portocaval anastomoses: - 1) esophageal veins - 2) paraumbilical veins - 3) rectal veins - 4) retroperitoneal veins - If there is liver damage or cirrhosis – accumulation of fibrous tissue that constricts the sinusoids – there may be portal hypertension. This may lead to varicose veins at the 4 sites of anastomoses. - The gallbladder is found under the right lobe of the liver. Its function is to store bile produced by the liver, which leaves via the cystic duct. It also enters the gallbladder in the cystic duct, traveling retrograde when the bile is not needed for digestion. Note the fundus, body, neck, and infundibulum of the gallbladder. - Note the right and left hepatic ducts coming together as the common hepatic duct, joining the cystic duct to form the common bile duct. This descends to the 2nd part of the duodenum, is joined by the pancreatic duct, and empties its contents into the duodenal lumen via the major duodenal papilla. - The gallbladder is supplied by the cystic artery, which is extremely important to find during a cholecystectomy. In most people it branches off the right hepatic artery, but could also come off the left hepatic, proper hepatic, or gastroduodenal arteries. - Note the extensive folds of mucosa extending into the lumen, consisting of tall, simple columnar epithelium. The underlying connective tissue is comprised of lamina propria, with no distinctly defined submucosa. There are scattered bundles of smooth muscle in the muscularis. The adventitia has rather dense connective tissue connecting the gallbladder to the liver. - Finally, we will look at the pancreas. To review: The head of the pancreas and duodenum are supplied from both the celiac trunk and the superior mesenteric artery. - The body and tail of the pancreas are mostly supplied by branches of the splenic artery, namely the dorsal, greater, and inferior pancreatic arteries. - Piece of advice: It can be very confusing when identifying these arteries. First orient yourself, note whether the duodenum is in anatomical position or reflected (as it is on the bottom left), and identify where the arteries branch from and where they lead. - The pancreas contains multiple ducts, but the main pancreatic duct runs from the tail to the head of the pancreas. There may be a smaller accessory pancreatic duct. They join the common bile duct to empty into the duodenum. The pancreas is retroperitoneal. - Histologically, we can see the septa (S) between pancreatic lobules with interlobular ducts (D). As mentioned above, the pancreas also has both exocrine and endocrine functions. Most of the bottom left panel is filled with exocrine pancreatic tissue. Secretory portions are called acini. The scattered endocrine islets of Langerhans (I) are paler staining. - An islet is magnified in the bottom right. It is a compact mass of epithelial cells that receive rich vascular supply (arrows). It is typically very difficult to identify the different cell types in the islets. Briefly, the alpha cells secrete glucagon, the beta cells secrete insulin, and the delta cells secrete somatostatin. -Once again, most of the pancreas contains exocrine acini. Pancreatic enzymes are very diverse, including extremely efficient proteases, lipases, and amylases. - Separate acini are shown in the left. The pancreatic acinar or secretory cells are polarized, meaning the basal portions are filled with basophilic rough ER. The apical regions are filled with zymogen granules that contain many stored pro-enzymes. - Centroacinar cells, with paler staining, can be seen in the middle of some acini and mark the beginning of the duct system (marked ―A‖ in the middle panel). They converge at ―B‖ to form intercalated ducts, marked as ―C‖. The intercalated duct cells may be hard to identify, but they actively pump water and bicarbonate into the duct lumen. Intercalated ducts empty into interlobular ducts, marked as ―small duct‖ in the bottom right, which lead to the main pancreatic duct. [email protected] [email protected]