* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 14 - Dr. Saadia McLeod
Depersonalization disorder wikipedia , lookup
Social anxiety disorder wikipedia , lookup
Impulsivity wikipedia , lookup
Conduct disorder wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Obsessive–compulsive personality disorder wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Personality disorder wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Anxiety disorder wikipedia , lookup
Anorexia nervosa wikipedia , lookup
Memory disorder wikipedia , lookup
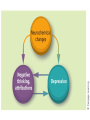
Learning disability wikipedia , lookup
Diagnosis of Asperger syndrome wikipedia , lookup
Asperger syndrome wikipedia , lookup
Autism spectrum wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Munchausen by Internet wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
Mental disorder wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Spectrum disorder wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Eating disorders and memory wikipedia , lookup
Eating disorder wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Child psychopathology wikipedia , lookup
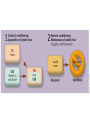
Chapter 14 Psychological Disorders ©2015 Cengage Learning. All Rights Reserved. Abnormal Behavior: Concepts and Controversies LEARNING OBJECTIVES • Describe and evaluate the medical model of abnormal behavior. • Identify the most commonly used criteria of abnormality. • Describe the five axes of the DSM-IV and controversies surrounding the DSM-IV system. • Summarize data on the prevalence of various psychological disorders. ©2015 Cengage Learning. All Rights Reserved. Abnormal Behavior, continued The medical model applied to abnormal behavior • The medical model “proposes that it is useful to think of abnormal behavior as a disease” and has become the main way of thinking about mental illness today. • This view is in stark contrast to how mental illness used to be perceived (see Figure 14.1). • Thus, the medical model has brought much needed improvement in patient care. ©2015 Cengage Learning. All Rights Reserved. Abnormal Behavior, continued The medical model, continued • Diagnosis – “involves distinguishing one illness from another." • Etiology – “refers to the apparent causation and developmental history of an illness." • Prognosis – “is a forecast about the probable course of an illness." ©2015 Cengage Learning. All Rights Reserved. Criteria of Abnormal Behavior 1. Deviance – the behavior must be significantly different from what society deems acceptable. 2. Maladaptive behavior – the behavior interferes with the person’s ability to function. 3. Personal distress – the behavior is troubling to the individual. ©2015 Cengage Learning. All Rights Reserved. Psychodiagnosis: The Classification of Disorders The American Psychological Association (A.P.A.) uses the Diagnostic and Statistical Manual. • It is now in its fifth revision and referred to as the DSM-5) to classify disorders. • It provides detailed information about various mental illnesses that allows clinicians to make more consistent diagnoses. ©2015 Cengage Learning. All Rights Reserved. Classification of Disorders, continued • Compared to the DSM IV, the DSM-5 no longer has a multiaxial system. • One major reason for the change is that individuals often qualify for the diagnosis of two or more conditions called “comorbity." • Rather, the DSM-5 utilizes a dimensional approach, which describes disorders in terms of how people score on a limited number of continuous dimensions (e.g. the degree to which they exhibit anxiety). ©2015 Cengage Learning. All Rights Reserved. Prevalence of Psychological Disorders • Epidemiology is “the study of the distribution of mental or physical disorders in a population." • Prevalence “refers to the percentage of the population that exhibits a disorder during a specified time period." • Research suggests that there has been a real increase in the prevalence in disorder (see Figure 14.3). • The most common classes are substance use, anxiety, and mood disorders. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders and Obsessive-Compulsive Disorder LEARNING OBJECTIVES • Describe three types of anxiety disorders, and discuss obsessive-compulsive disorder. • Discuss how biology, conditioning, cognition, and stress contribute to the etiology of these disorders. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders and OCD, continued • Anxiety disorders “are a class of disorders marked by feelings of excessive apprehension and anxiety." • Generalized anxiety disorder “is marked by a chronic, high level of anxiety that is not tied to any specific threat." • Phobic disorder “is marked by a persistent and irrational fear of an object of situation that presents no realistic danger." ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders and OCD, continued Panic Disorder and Agoraphobia • Panic disorder “is characterized by recurrent attacks of overwhelming anxiety that usually occur suddenly and unexpectedly” (see following animation sequence). • Agoraphobia “is a fear of going out to public places." – Agoraphobia may result from severe panic disorder, in which people “hide” in their homes out of fear of the outside world. – In DSM-5 it is listed as a separate disorder. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders and OCD, continued Obsessive-compulsive disorder (OCD) “is marked by persistent, uncontrollable intrusions of unwanted thoughts (obsessions) and urges to engage in senseless rituals (compulsions)." • Common obsessions include fear of contamination, harming others, suicide, or sexual acts. • Compulsions are highly ritualistic acts that temporarily reduce anxiety brought on by obsessions. • While 17% of people without a disorder report significant obsession or compulsion, • True OCD disorders only occur in approximately 2%3% of the population. • Most cases of OCD emerge before the age of 30. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders and OCD, continued Etiology of anxiety disorders • Biological factors – Inherited temperament may be a risk factor for anxiety disorders. – “Anxiety sensitivity” theory posits that some people are more sensitive to internal physiological symptoms of anxiety and overreact with fear when they occur. – The brain’s neurotransmitters, or “chemicals that carry signals from one neuron to another,” may underlie anxiety. – In particular, drugs that affect the neurotransmitter GABA (e.g., Valium) suggest that these chemical circuits may be involved in anxiety disorders. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders, continued Etiology of anxiety disorders, continued • Conditioning and learning – Classical conditioning may cause one to fear a particular object or scenario. – Then, avoiding the fear stimulus is negatively reinforced, through operant conditioning, by making the person feel less anxious (See Figure 14.5). – Seligman (1971) adds we are “biologically prepared” to fear some things more than others, however. ©2015 Cengage Learning. All Rights Reserved. Anxiety Disorders, continued Etiology of anxiety disorders, continued • Cognitive factors – Some people are more likely to experience anxiety disorders because they: o Misinterpret harmless situations as threatening o Focus excess attention on perceived threats o Selectively recall information that seems threatening ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders LEARNING OBJECTIVES • Distinguish among the three types of somatoform disorders. • Summarize what is known about the causes of somatoform disorders. ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders, continued • Somatoform disorders “are physical ailments that cannot be fully explained by organic conditions and are largely due to psychological factors." • Somatization disorder “is marked by a history of diverse physical complaints that appear to be psychological in origin." – It occurs mostly in women. – Symptoms seem to be linked to stress. ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders, continued • Conversion disorder – “is characterized by a significant loss of physical function with no apparent organic basis, usually in a single organ system." – Common symptoms include: o Partial or total loss of vision or hearing o Partial paralysis o Laryngitis or “mutism” (inability to speak) o Seizures or vomiting o Loss of function in limbs ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders, continued • Hypochondriasis (or hypochondria) “is characterized by excessive preoccupation with health concerns and incessant worry about developing physical illnesses." – People with hypochondria are convinced their symptoms are real and often become frustrated with the medical establishment. – Hypochondria often occurs along with anxiety disorders and depression. ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders, continued Etiology of somatoform disorders • Personality factors – Somatoform disorders are more common in people with “histrionic” personalities (those who thrive on the attention that illness brings). – Neuroticism also seems to elevate one’s predisposition to somatoform disorders. ©2015 Cengage Learning. All Rights Reserved. Somatoform Disorders, continued • Cognitive factors – Some people focus excessive attention on bodily sensations and amplify them into perceived symptoms of distress. – They also have unrealistically high standards of “good health." Thus, any deviation from perfect health is seen as a sign of illness. • The sick role – Some people learn to “like” being sick because: • It allows one to avoid challenging tasks. • Demands aren’t placed on sick people. • It provides an excuse for failure. • Being sick elicits attention from others. ©2015 Cengage Learning. All Rights Reserved. Dissociative Disorders LEARNING OBJECTIVES • Distinguish between two types of dissociative disorders. • Summarize what is known about the causes of dissociative disorders. ©2015 Cengage Learning. All Rights Reserved. Dissociative Disorders, continued Dissociative disorders “are a class of disorders in which people lose contact with portions of their consciousness or memory, resulting in disruptions in their sense of identity." • Dissociative amnesia “is a sudden loss of memory for important personal information that is too extensive to be due to normal forgetting." ©2015 Cengage Learning. All Rights Reserved. Dissociative Disorders, continued • Dissociative identity disorder (DID) “involves the coexistence in one person of two or more largely complete, and usually very different, personalities." – Also known as “multiple personality disorder”, in which each personality has its own name, memories, traits, and physical mannerisms. – Transitions between identities can be sudden and the differences between them can be extreme (e.g., different races or genders). ©2015 Cengage Learning. All Rights Reserved. Dissociative Disorders, continued • Etiology of dissociative disorders – Psychogenic amnesia and fugue are usually the result of extreme stress. – Dissociative identity disorder is a fascinating and bizarre disorder, and its causes are largely unknown. • However, many clinicians suspect that DID may result from severe emotional trauma that occurs in childhood. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders LEARNING OBJECTIVES • Describe depressive and bipolar disorders, discuss their prevalence, and explain their relation to suicide risk. • Explain how genetic, neurochemical, neuroanatomical, and hormonal factors contribute to the development of depressive and bipolar disorders. • Discuss how cognitive processes, interpersonal factors, and stress contribute to the development of depressive and bipolar disorders. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued • Major depressive disorder is one in which people “show persistent feelings of sadness and despair and a loss of interest in previous sources of pleasure.“ • - More than just feeling bad: -Mood/affect/apathy/anhedonia -Thoughts -Sleep/Fatigue – Suicidal ideation/risk high – Most will experience a repeat episode. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued Major depressive disorder, continued – Depression is one of the most common mental illnesses (the lifetime prevalence is 13% - 14%). – Women are twice as likely o This does not appear to be tied to biological differences between men and women and could result from greater stress and abuse that women experience. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued • Bipolar disorder “experience of both depressed and manic periods." – “Manic” periods are characterized by bouts of extreme exuberance and a feeling of invincibility. – However, this state of elation alternates, sometimes suddenly, with periods of depression (see Figure 14.8). ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued • Mood dysfunction and suicide – Ninety percent of suicide attempts linked to psychological disorder. o o o Lifetime risk for those with bipolar disorder is 15-20%; it is 10-15% in those who have had depression. Bipolar: highest risk of suicide Women are three times more likely to attempt suicide, but men “complete” four times as many suicides. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued Etiology of mood disorders • Genetic vulnerability – Concordance rates, or “the percentage of twin pairs or other pairs of relatives that exhibit the same disorder”, suggests there is a genetic basis for mood disorders. o Concordance rates for identical twins is 6572%, whereas it is only 14-19% for fraternal twins who share fewer genes but the same environment. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued Etiology of mood disorders, continued • Brain: Neurotransmitters (chemical messengers) 1. Norepinephrine 2. Serotonin 3. Antidepressants increase these neurotransmitters – Cause and effect problem ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued Etiology of mood disorders, continued • Neuroanatomical factors, continued – Depression is also correlated with • The hippocampus, is 8-10% smaller in depressed, than in normal, subjects (see Figure 14.11). • Development of new neurons stops in depressed patients (neurogenesis) • Causes depression or effect of depression? ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued • Hormonal factors – Stress Hormones higher in depressed patients : stress response on over-drive • Cognitive factors – Seligman (1974) “learned helplessness”, in which people become passive and “give up” in times of difficulty. o Depressed individuals grew up in a critical and punishing environment and have been shaped to be negative and passive. ©2015 Cengage Learning. All Rights Reserved. Mood Disorders, continued Etiology of mood disorders, continued • Social skills/social support – Depression has also been correlated with interpersonal factors, such as poor social skills. – It is unclear what the direction of cause and effect is, with regard to this correlation. • Precipitating stress – There is also a link between stress and the onset of mood disorders (See Figure 14.14). ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Schizophrenia literally means “split mind." • Schizophrenic disorders : Thought disorder • Rare: 1% of the population suffering from this class of disorders. • Schizophrenia is a severe disorder that usually has an early onset and a poor prognosis. (adolescence or early 20s) ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Symptoms 1. Irrational thought – Delusions : false beliefs disconnected from reality – Example: mind is being controlled by an external source. – Delusions of grandeur are irrational beliefs that one is “extremely important or famous.“ ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued 2. Deterioration of adaptive behavior – Feed self, care for self, hygiene, etc. 3. Distorted perception – Hallucinations – Hearing voices or seeing things that are not there (auditory and visual hallucinations). 4. Disturbed emotion (“flat” affect or inappropriate emotions for a situation). ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued • Schizophrenia was divided into four subtypes: 1. Paranoid type 2. Catatonic type 3. Disorganized type 4. Undifferentiated type • (DSM-5 has discarded this distinction.) ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Positive versus negative symptoms • Another way to classify: 1. Schizophrenias with negative symptoms (behavioral deficits, such as flat affect). 2. Schizophrenias with positive symptoms (hallucinations, delusions, & bizarre behavior). ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Course and outcome • Schizophrenia usually emerges during adolescence or early adulthood. • Its course is variable, with three likely outcomes: 1. Patients with milder versions who experience a full recovery. 2. Patients who experience a partial recovery and who are in and out of treatment facilities. 3. Patients whose symptoms are persistent and severe, and who require permanent hospitalization. ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued • Patients with a favorable prognosis: 1. Have a sudden onset of the disorder 2. Experience onset at a later age 3. Were well adjusted before the onset 4. Have a low proportion of negative symptoms 5. Have well preserved cognitive function 6. Show good adherence to treatment 7. Have a relatively healthy, supportive family environment to return to ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Etiology of schizophrenia • Genetic vulnerability – Concordance in identical twins is 48%, versus 17% in fraternal twins, suggesting a genetic basis for the disease (see Figure 14.15) • Brain: – Excess Dopamine link – Some studies have linked marijuana use in adolescence with the onset of schizophrenia. ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued Etiology of schizophrenia, continued – The neurodevelopmental hypothesis :disruptions in the normal maturational processes of the brain before or at birth." – may include: • Prenatal exposure to a viral infections • Malnutrition during prenatal development • Obstetrical complications during birth ©2015 Cengage Learning. All Rights Reserved. Schizophrenic Disorders, continued – Expressed emotion (EE) is “the degree to which a relative of a schizophrenic patient displays highly critical or emotionally overinvolved attitudes toward the patient." • A family’s EE is a good predictor of the course of a schizophrenic’s illness. • Patients who return to families high in EE are three to four times more likely to relapse because they add stress. – Precipitating stress itself may trigger the onset of schizophrenia in someone who is already vulnerable to the disease. ©2015 Cengage Learning. All Rights Reserved. Autism Spectrum Disorder, continued Autism, or autism spectrum disorder, – Social Deficits: Reciprocity – Verbal and Pragmatic Language – Restricted Interests – Self-Stimulation ©2015 Cengage Learning. All Rights Reserved. Autism Spectrum Disorder, continued Symptoms and prevalence • Symptoms may include: – Lack of interest in other people – Tendency to avoid eye contact – Failure to bond – Delayed, or inability to develop speech – Echolalia – rote repetition of others’ words – Inflexibility with changes in routine • Prevalence – About 1% of children are presently diagnosed with autism or an autism spectrum disorder. (some stats show higher prevalence – 1/100) – This is a fourfold increase since the mid-1990s – Early Tx: 15% - 20% of autistic individuals can live independently. ©2015 Cengage Learning. All Rights Reserved. Autism Spectrum Disorder, continued Etiology • Given its appearance so early in life, most theorists believe autism has biological origins. • Familial studies suggest genetic factors may contribute. • The popular “mercury vaccine” hypothesis has been discredited. – The 1998 study that reported the link between the vaccinations and autism has been found to be fraudulent. – Recent attempts to replicate it have failed. ©2015 Cengage Learning. All Rights Reserved. Application: Understanding Eating Disorders LEARNING OBJECTIVES • Describe the subtypes, history, prevalence, and gender distribution of eating disorders. • Explain how genetic factors, personality, culture, family dynamics, and disturbed thinking contribute to the development of eating disorders. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Types of eating disorders • Eating disorders “are severe disturbances in eating behavior characterized by preoccupation with weight and unhealthy efforts to control weight." • There are three main types: – Anorexia nervosa – Bulimia nervosa – Binge-eating disorder ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Types of eating disorders, continued Anorexia nervosa “involves intense fear of gaining weight, disturbed body image, refusal to maintain normal weight, and dangerous measure to lose weight." • Two subtypes include 1. Restricting type anorexia nervosa 2. Binge-eating/purging type anorexia nervosa • Both entail distortions in body image. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Anorexia nervosa, continued • Medical complications from anorexia are serious and can include: – Amenorrhea (ceasing of menstrual cycles) – Gastrointestinal problems – Dental problems – Osteoporosis (loss of bone density) – Low blood pressure – Metabolic disturbances that can trigger cardiac arrest ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Types of eating disorders, continued Bulimia nervosa “involves habitually engaging in out-ofcontrol overeating followed by unhealthy compensatory efforts, such as self-induced vomiting, fasting, abuse of laxatives and diuretics, and excessive exercise." • Unlike with anorexia, patients with bulimia usually maintain a normal weight. • However, they do risk medical problems such as cardiac arrhythmias, dental problems, metabolic deficiencies, and gastrointestinal problems. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Types of eating disorders, continued Binge-eating disorder “involves distress-inducing eating binges that are not accompanied by the purging, fasting, and excessive exercise seen in bulimia." • Patients with this disorder are often overweight and disgusted with their bodies. • Excessive overeating is often triggered by stress. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued History and prevalence • Anorexia - more common in the middle of the 20th century. • Bulimia appears to be a more recent disorder (it did not become common until the 1970s). • Young women are much more likely to develop eating disorders (90% - 95% of cases) • Age of onset is early, and late adolescence for anorexia, and bulimia nervosa, respectively. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Etiology of eating disorders • Genetic vulnerability – Twin studies show higher concordance rates for identical twins than fraternal twins, suggesting a genetic predisposition for the disease. – However, many other factors influence the development of eating disorders. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Etiology of eating disorders, continued • Personality factors – Victims of anorexia tend to be perfectionistic, rigid, and anxious – In contrast, bulimia is associated with impulsiveness and low self-esteem. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Etiology of eating disorders, continued • Cultural values – In Western society, young women are socialized to believe they must be very thin in order to be attractive – “Desirable” weight, as seen in models and actresses, has decreased in recent decades. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Etiology of eating disorders, continued • The role of the family – Control over body as coping in chaotic family or over-involved family. – Some mothers even contribute to eating disorders by endorsing society’s obsession with being thin. ©2015 Cengage Learning. All Rights Reserved. Application: Eating Disorders, continued Etiology of eating disorders, continued • Cognitive factors – Beliefs: • “I must be thin to be accepted.” • “If I am not in complete control, I will lose all control.” • “If I gain one pound, I will become obese.” ©2015 Cengage Learning. All Rights Reserved.