* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 10 Endocrine System
Cryptorchidism wikipedia , lookup
History of catecholamine research wikipedia , lookup
Menstrual cycle wikipedia , lookup
Endocrine disruptor wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Neuroendocrine tumor wikipedia , lookup
Breast development wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Mammary gland wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Adrenal gland wikipedia , lookup
Hypothalamus wikipedia , lookup
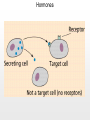
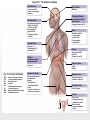
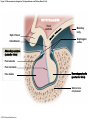
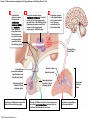
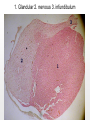
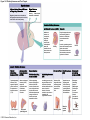
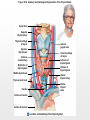
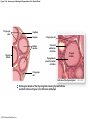
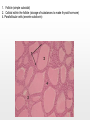
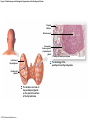
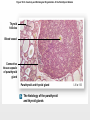
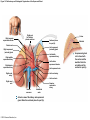
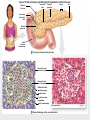
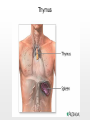
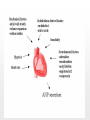
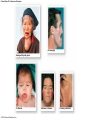
Chapter 19 Endocrine System Robert Pershing Wadlow Wadlow reached the height of 2.72 m (almost 9 ft) and a weight of 222 kg (488 lbs) before his death at the age of 22. His large size was attributed to a tumor in the pituitary. He was still in a growth phase when died of an infection. Hormones Figure 19.1 The Endocrine System Hypothalamus Pineal Gland Production of ADH, oxytocin, and regulatory hormones Melatonin Parathyroid Glands (on posterior surface of thyroid gland) Pituitary Gland Pars distalis (anterior lobe): ACTH, TSH, GH, PRL, FSH, LH, and MSH Neurohypophysis (posterior lobe): Release of oxytocin and ADH Parathyroid hormone (PTH) Heart Natriuretic peptides: Atrial natriuretic peptide (ANP) Brain natriuretic peptide (BNP) Thyroid Gland Thyroxine (T4) Triiodothyronine (T3) Calcitonin (CT) Kidney Erythropoietin (EPO) Calcitriol (Chapters 19 and 26) Thymus (Undergoes atrophy during adulthood) Adipose Tissue Thymosins KEY TO PITUITARY HORMONES Suprarenal Glands ACTH TSH GH PRL FSH LH MSH ADH Each suprarenal gland is subdivided into: Medulla: Epinephrine (E) Norepinephrine (NE) Cortex: Cortisol, corticosterone, aldosterone, androgens Adrenocorticotropic hormone Thyroid-stimulating hormone Growth hormone Prolactin Follicle-stimulating hormone Luteinizing hormone Melanocyte-stimulating hormone Antidiuretic hormone Leptin Resistin Digestive Tract Numerous hormones (detailed in Chapter 25) Pancreatic Islets Testis Insulin, glucagon Gonads Ovary Testes (male): Androgens (especially testosterone), inhibin Ovaries (female): Estrogens, progestins, inhibin Figure 19.2 Neuroendocrine Integration: The Hypothalamus and Pituitary Gland (5 of 6) HYPOTHALAMUS Third ventricle Mamillary body Optic chiasm Infundibulum Diaphragma sellae Adenohypophysis (anterior lobe) Pars tuberalis Pars intermedia Pars distalis Neurohypophysis (posterior lobe) Sella turcica of sphenoid © 2015 Pearson Education, Inc. Figure 19.2 Neuroendocrine Integration: The Hypothalamus and Pituitary Gland (3 of 6) 1 3 2 Hypothalamic neurons produce the hormones antidiuretic hormone (ADH) and oxytocin. After transport along their axons, these hormones are released at the neurohypophysis (posterior lobe of the pituitary gland). Integrative centers release regulatory hormones to control activity of the adenohypophysis (anterior lobe of the pituitary gland). Regulatory hormones reach their targets via the hypophyseal portal system, detailed below. Autonomic centers in the hypothalamus exert neural control over hormone secretion by the adrenal medullae. HYPOTHALAMUS Preganglionic motor fibers Infundibulum (connection between hypothalamus and the pituitary gland) Adenohypophysis (anterior lobe of pituitary gland) Secretion of multiple hormones that control other endocrine organs. © 2015 Pearson Education, Inc. Adrenal cortex Adrenal medulla Neurohypophysis (posterior lobe of pituitary gland) Release of ADH and oxytocin; these hormones are called neurosecretions because they are produced and released by neurons. Suprarenal (adrenal) gland Secretion of epinephrine and norepinephrine 1. Glandular 2. nervous 3. infundibulum Figure 19.3 Pituitary Hormones and Their Targets Hypothalamus Indirect Control through Release of Regulatory Hormones Regulatory hormones are released into the hypophyseal portal system for delivery to the enterior lobe of the pituitary Direct Release of Hormones Sensory Osmoreceptor stimulation stimulation Posterior Pituitary Hormones Antidiuretic hormone (ADH) Oxytocin Antidiuretic hormone, or vasopressin, targets the kidneys. It results in the reabsorption of water, and elevation of both blood volume and blood pressure. Oxytocin targets the uterus and mammary glands in females. It causes labor contractions and milk ejection. Kidney In males, oxytocin targets the ductus deferens and prostate gland, and results in contractions of the ductus deferens and prostate, and ejection of secretions. Uterus Prostate Anterior Pituitary Hormones Thyroidstimulating hormone (TSH) Adrenocorticotropic hormone (ACTH) Gonadotropins: Follicle-stimulating hormone (FSH) Luteinizing hormone (LH) Thyroid-stimulating hormone (TSH) targets the thyroid gland. It results in the production of thyroid hormones (T3, T4). Adrenocorticotropic hormone (ACTH) targets the suprarenal cortex. It stimulates glucocorticoid secretion. Follicle-stimulating hormone (FSH) targets follicular cells in the ovaries of females, and nurse cells in the testes of males. FSH causes follicle development and estrogen secretion in females, and sperm maturation in males. Luteinizing hormone (LH) targets follicular cells in the ovaries of females and interstitial cells in the testes of males. In females, LH causes ovulation, corpus luteum formation, and progesterone secretion. Thyroid gland © 2015 Pearson Education, Inc. Suprarenal (adrenal) gland Ovary Prolactin (PRL) Testis Prolactin (PRL) targets the female mammary glands and causes the production of milk. Mammary gland Growth hormone (GH) Growth hormone (GH) targets all cells in the body. It causes growth, protein synthesis, lipid mobilization and catabolism. Musculoskeletal system Melanocytestimulating hormone (MSH) Melanocytestimulating hormone (MSH) targets melanocytes. It results in increased melanin production in the epidermis. Melanocyte Figure 19.6a Anatomy and Histological Organization of the Thyroid Gland Hyoid bone Superior thyroid artery Thyroid cartilage of larynx Superior thyroid vein Common carotid artery Right lobe of thyroid gland Middle thyroid vein Internal jugular vein Cricoid cartilage of larynx Left lobe of thyroid gland Isthmus of thyroid gland Inferior thyroid artery Thyrocervical trunk Trachea Inferior thyroid veins Outline of clavicle Outline of sternum Location and anatomy of the thyroid gland Figure 19.4c Anatomy and Histological Organization of the Thyroid Gland T thyrocyte cells Capillary Capsule C thyrocyte cell Follicle cavities Cuboidal epithelium of follicle Thyroid follicle Thyroid follicle Thyroglobulin stored in colloid of follicle C thyrocyte cell Follicles of the thyroid gland c Histological details of the thyroid gland showing thyroid follicles and both of the cell types in the follicular epithelium © 2015 Pearson Education, Inc. LM x 260 1. Follicle (simple cuboidal) 2. Colloid within the follicle (storage of substances to make thyroid hormone) 4. Parafollicular cells (secrete calcitonin) Figure 19.6ab Anatomy and Histological Organization of the Parathyroid Glands Thyroid follicles Blood vessel Connective tissue capsule of parathyroid gland Parathyroid and thyroid gland Left lobe of thyroid gland b The histology of the parathyroid and thyroid glands Parathyroid glands a The location and size of the parathyroid glands on the posterior surface of the thyroid lobes © 2015 Pearson Education, Inc. LM x 100 Figure 19.8b Anatomy and Histological Organization of the Parathyroid Glands Thyroid follicles Blood vessel Connective tissue capsule of parathyroid gland Parathyroid and thyroid gland The histology of the parathyroid and thyroid glands LM 100 Figure 19.7ab Anatomy and Histological Organization of the Suprarenal Gland Right and left inferior phrenic arteries Right superior suprarenal arteries Cortex Sectional plane for part (b) Medulla Celiac trunk Left suprarenal (adrenal) gland Right suprarenal (adrenal) gland Left middle suprerenal artery Right middle suprarenal artery Left inferior suprarenal arteries Right inferior suprarenal artery Left suprarenal vein Right renal artery Left renal artery Left renal vein Right renal vein Inferior vena cava Abdominal aorta a Anterior view of the kidney and suprarenal gland. Note the sectional plane for part (b). © 2015 Pearson Education, Inc. Superior mesenteric artery b A suprarenal gland cut to show both the cortex and the medulla. Note the orientation of the section for part (c). Figure 19.10ab Anatomy and Histological Organization of the Pancreas Common bile duct Pancreatic duct Body of pancreas Lobule Tail Accessory pancreatic duct Head of pancreas Small intestine (duodenum) The gross anatomy of the pancreas Pancreatic acini (exocrine cells) Pancreatic islet (islet of Langerhans) Endocrine cells: cells (glucagon) cells (insulin) F cells (pancreatic polypeptide) cells (somatostatin) Pancreatic islet General histology of the pancreatic islets LM 400 Thymus Clinical Note 19.1 Endocrine Disorders Acromegaly Enlarged thyroid gland Cretinism © 2015 Pearson Education, Inc. Addison’s disease Cushing’s disease