* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Acute management of myocardial infarction
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Jatene procedure wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
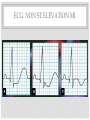
MYOCARDIAL INFARCTION CASE 1 • Mr. A: 38 years old • He smokes 1 pack of cigarettes per day • He has no other past medical history • 8 hours ago, he gets sharp central chest pain that is worse with inspiration. It has not yet resolved. • He feels short of breath CASE 2 • Mr. D: 50 years old • He also smokes 1 pack of cigarettes per day • His past medical history includes hypertension and diabetes • While he was working on the farm, he develops dull central chest pain that radiates to his neck • With rest, the pain went away after about 5 minutes • He also has shortness of breath WHICH PATIENT IS HAVING AN MI? WH Y ? HISTORY • Pain • Location • Exertional • Other symptoms: • Shortness of breath • Nausea • Sweaty • Risk Factors • • • • • • Family history Diabetes Hypertension Smoking Hyperlipidemia Previous MI or stroke PHYSICAL EXAM • Vital signs • BP • HR • O2 saturation • Cardiac exam • S3 or S4 may be present • Murmur of mitral regurgitation • May have heart failure on cardiac and respiratory exam ECG: ST ELEVATION MI ECG ECG: NON ST ELEVATION MI ECG STEMI VERSUS NSTEMI MANAGEMENT: CASE When you examine Mr. D, he can talk to you • BP 110/70 HR 100 O2 93% on room air • He has normal heart sounds, no murmur, but has S4 • Lungs are clear • ECG shows ST depression and T wave inversion in V2- V6. • What do you want to do next? MANAGEMENT • First, ABC’s! • If you have cardiac monitor, put him on it • IV access • Oxygen • What medications do you want to give him? • For his pain? • To prevent further thrombosis (antithrombotics)? • To prevent arrythmia? • To treat other cardiac risk factors? MEDICATIONS: PAIN • Nitrates • Vasodilation of coronary arteries • Decrease preload (venous vasodilation) • Decrease afterload (arterial vasodilation) • Be careful of hypotension (aortic stenosis, right ventricular MI) • Morphine • Avoid NSAIDS if you can MEDICATIONS: ANTITHROMBOTIC • Aspirin • 162-325mg Po chewed x 1 then 75mg-100mg daily • Patient needs to take indefinitely • Decreases mortality • Give as soon as you suspect an MI • Consider clopidogrel • 300mg PO x 1 then 75mg daily for 1-12 months • Small additional benefit MEDICATIONS: ANTICOAGULANTS • Heparin • Decreases risk of death and re-infarction • If using unfractionated heparin IV, monitor PTT • Duration is at least 48 hours MEDICATIONS: PREVENTING ARRYTHMIA • Beta blockers (eg. Atenolol, propranolol, metoprolol) • Decreases mortality and ventricular arrythmias • Start within 24 hours • Contraindications • Acute heart failure • Heart block • Asthma • Hypotension • No role for antiarrythmics such as lidocaine or digoxin • No role for calcium channel blockers MEDICATIONS • ACE inhibitors (ramipril, enalopril) • Especially beneficial in those with heart failure • Start within 24 hours • Prevents left ventricular remodelling REPERFUSION • 2 options • A) Fibrinolytics • If symptoms started less than 24 hours ago • Contraindications: Uncontrolled hypertension, stroke in last 3 months, previous intracranial hemorrhage • For STEMI patients only • B) Percutaneous coronary intervention (PCI) • If symptoms started less than 12 hours ago • If the “door to balloon” time can be less than 90 minutes • For STEMI patients. Can consider for NSTEMI patients REPERFUSION • Which NSTEMI patients should you think about sending for reperfusion? • Chest pain and ischemia not responding to medications • Unstable patients • Arrythmias • Heart failure COMPLICATIONS • Heart failure • Bradycardia from AV (conduction) block • Arrythmia • Non sustained ventricular tachycardia (VT) • Sustained VT and ventricular fibrillation • New mitral regurgitation • Ventricular wall rupture • Cardiogenic shock